Improving screening and treatment for depression in primary care will require better mental health care integration. Depression is common in primary care, yet screening for the condition remains low. Enhanced, coordinated financial support for the integration of mental health care into primary care could improve identification and treatment of depression.
Most people with poor mental health will be diagnosed and treated in the primary care setting.1,2 Depression and anxiety disorders are the most common mental health conditions in primary care, often complicating other medical conditions and making them more expensive.3 Offering treatment for depression after screening can improve outcomes,4 but the U.S. Preventive Services Task Force recommends against screening for depression in primary care unless there are staff-assisted care supports in place to assure accurate diagnosis, effective treatment, and follow-up.5 This is in part a response to evidence that screening alone does not lead to improved outcomes in depression care.4 Staff-assisted supports such as on-site mental health providers and care managers can improve depression identification and treatment. Current health care policy makes it difficult for most primary care practices to integrate mental health staff because of insufficient reimbursement, mental health insurance carve-outs, and difficulty of supporting colocated mental health professionals, to name a few.6
Analysis of National Ambulatory Medical Care Surveys from 2003 to 2006 reveals that despite the high prevalence of depression in primary care (10 to 12 percent), screening is extremely low at 2 to 4 percent (see accompanying figure).7 Primary care physicians can generally tell which patients do not have depression, but often miss those who do.8 Current patterns of screening for depression may be evidence-based given that primary care typically lacks on-site mental health providers, but they are not consistent with making health care more patient-centered, efficient, or effective. Improving identification and treatment of depression in primary care is unlikely to change without better integration of mental health services. Payment and other policies that separate mental health from physical health should be changed to better accommodate care for depression in primary care.
Figure. Percentage of visits with depression diagnosis and screening
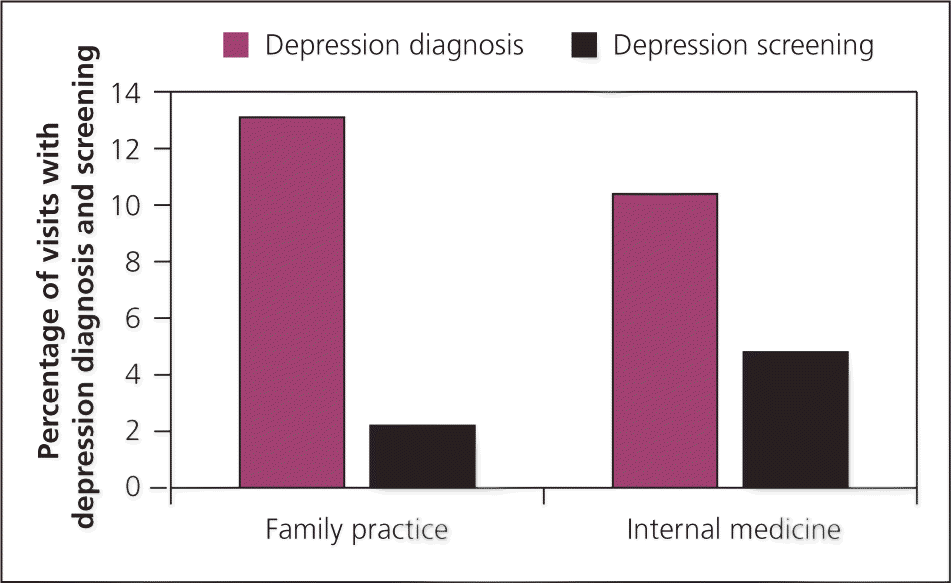
Incidence of depression screening and diagnosis during primary care visits in the United States.
Information from reference 7.

