The diagnosis of depression in older patients is often complicated by comorbid conditions, such as cerebrovascular disease or dementia. Tools specific for this age group, such as the Geriatric Depression Scale or the Cornell Scale for Depression in Dementia, may assist in making the diagnosis. Treatment decisions should consider risks associated with medications, such as serotonin syndrome, hyponatremia, falls, fractures, and gastrointestinal bleeding. Older white men with depression are at high risk of suicide. Depression is common after stroke or myocardial infarction, and response to antidepressant treatment has been linked to vascular outcomes. Depression care management is an important adjunct to the use of antidepressant medications. Structured psychotherapy and exercise programs are useful treatments for select patients.
The epidemiology of geriatric major depression is similar to that of younger adults, affecting 5 to 10 percent of older patients in primary care outpatient settings and occurring more often in women.1 Depression in older persons may represent a relapse of depression from earlier in life rather than a new depressive disorder presenting late in life. Persons with late-onset depressive symptoms are more likely to have underlying cerebrovascular disease or incipient dementia. This may explain why response to psychological and pharmacologic treatment approaches is lower in older populations. Psychotic depression, which causes delusions or hallucinations, is more common in late-life depression.1 The following illustrative cases highlight challenges presented by older patients with depression.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| The Geriatric Depression Scale and the Cornell Scale for Depression in Dementia are validated tools for screening for depression in older patients with dementia. | C | 7, 8 | — |
| Patients with ST-segment elevation myocardial infarction should be assessed for depression during hospitalization, one month after discharge, and annually thereafter. Cognitive behavior therapy and selective serotonin reuptake inhibitors are useful for treating depression in this population. | C | 28 | American College of Cardiology/American Heart Association recommendation |
| Routine screening for depression in older patients is recommended only if depression care management is available. | A | 35 | U.S. Preventive Services Task Force recommendation |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Case 1. An 85-year-old nursing home patient with dementia has been withdrawn and eating poorly. The staff thinks that she may be depressed and asks you about prescribing an antidepressant.
Major depression in older patients is diagnosed using the same criteria as in younger adults. It is based on the persistence of the core symptoms of anhedonia or depressed mood for two weeks, with four or more of the following: feelings of worthlessness or guilt, decreased ability to concentrate or make decisions, fatigue, psychomotor agitation or retardation, insomnia or hypersomnia, significant changes in weight or appetite, and recurrent thoughts of suicide or death.2
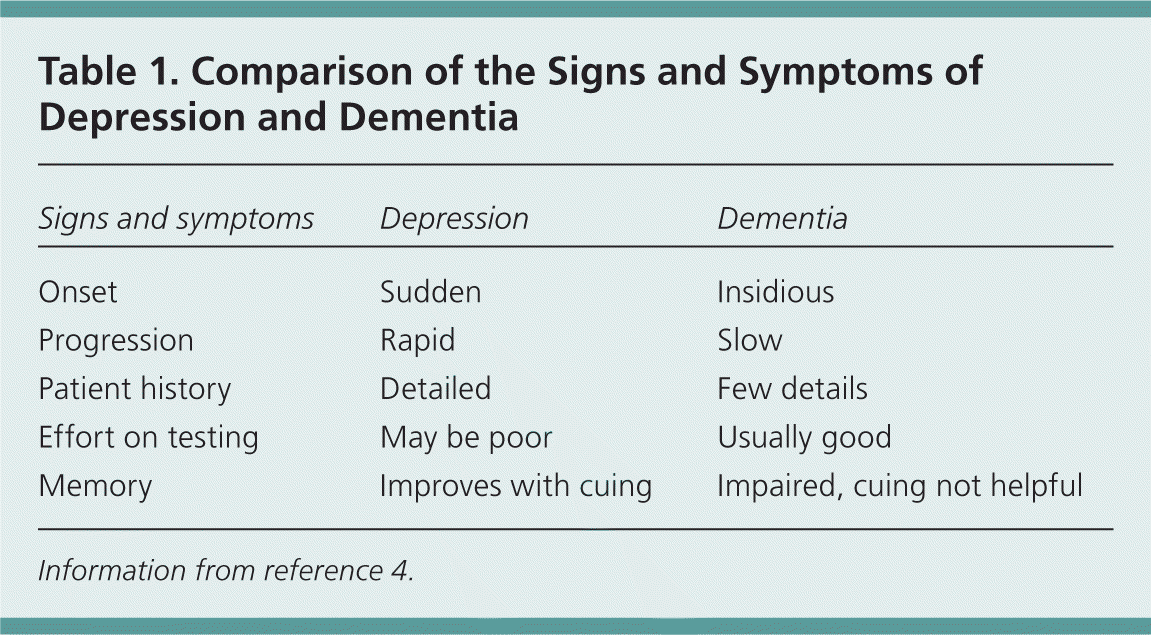
The diagnosis can be more difficult in older persons, because they may have somatic symptoms related to comorbid illnesses and are less likely to report certain symptoms, such as guilt. Depressive symptoms such as fatigue and hypersomnia may be a consequence of illness.3 The diagnosis may be further obscured by dementia, limiting the patient's ability to provide a thorough history. Table 1 shows a comparison of the symptoms and signs of depression and dementia.4 Depression is more common in patients in nursing homes and is often manifested by weight loss.5
Table 1. Comparison of the Signs and Symptoms of Depression and Dementia
| Signs and symptoms | Depression | Dementia |
|---|---|---|
| Onset | Sudden | Insidious |
| Progression | Rapid | Slow |
| Patient history | Detailed | Few details |
| Effort on testing | May be poor | Usually good |
| Memory | Improves with cuing | Impaired, cuing not helpful |
Information from reference 4.
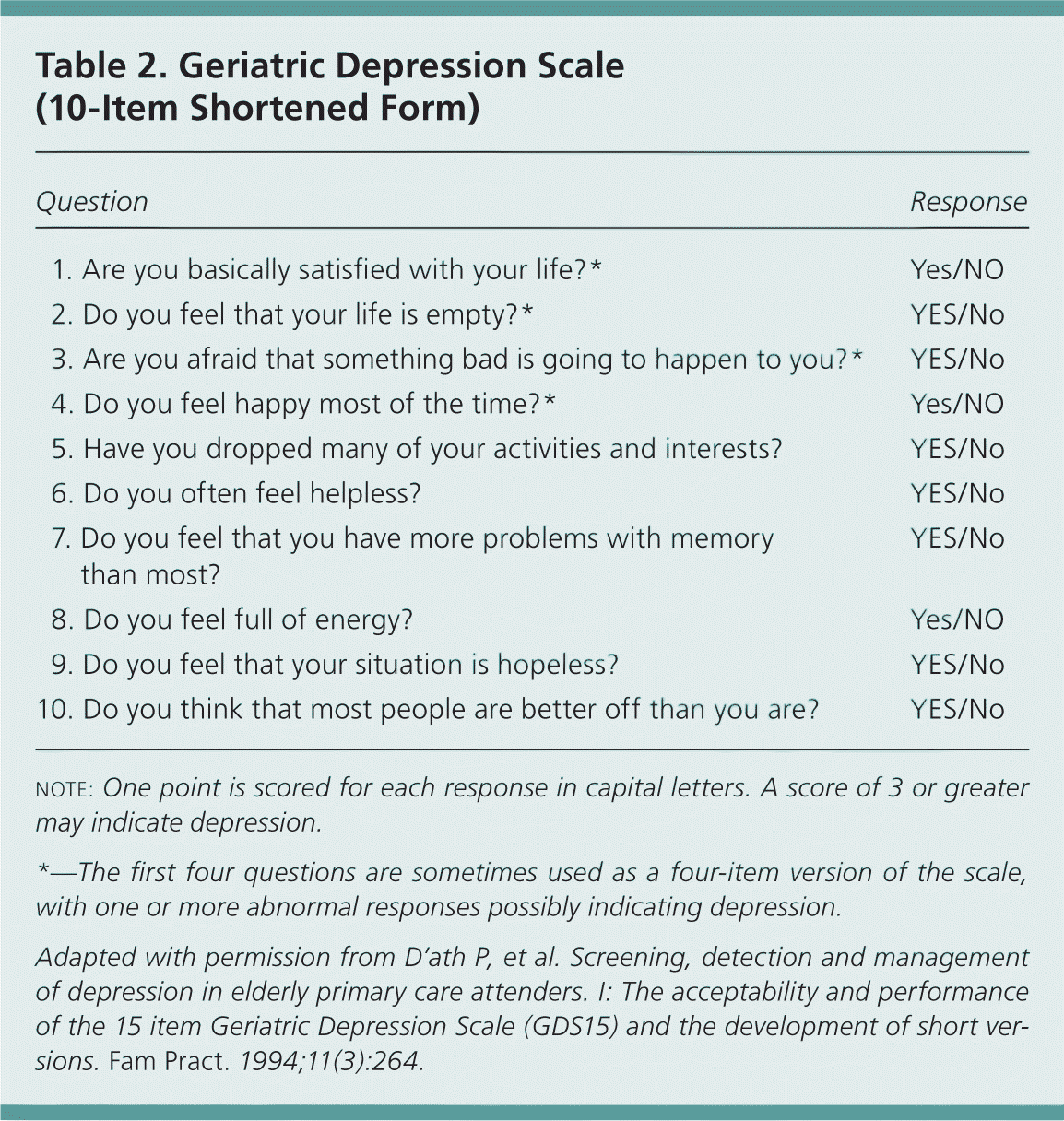
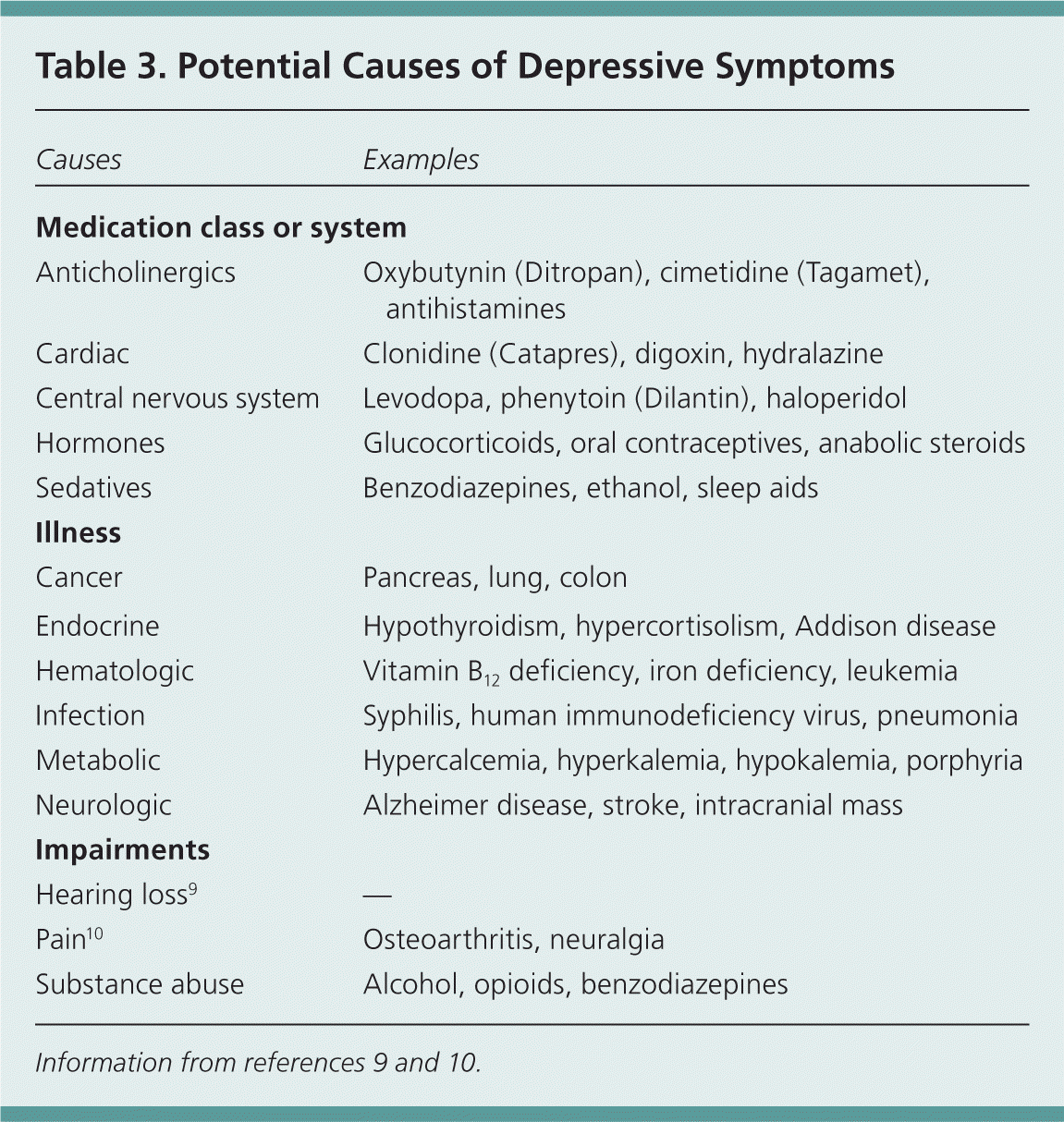
The Geriatric Depression Scale is a useful screening tool that has been validated for use in patients with dementia who have Mini-Mental State Examination scores as low as 15 (Table 26 ).7 The Cornell Scale for Depression in Dementia is a caregiver-based evaluation tool that can be used to diagnose depression that accompanies more severe dementia.8 It can be accessed at http://www.amda.com/resources/2005_updates_ltc_teaching_kits/dementia.pdf. Other causes of depressive symptoms should be considered, such as delirium, adverse effects from medication, or metabolic disorders (Table 39,10 ).
Table 2. Geriatric Depression Scale (10-Item Shortened Form)
| Question | Response |
|---|---|
| 1. Are you basically satisfied with your life?* | Yes/NO |
| 2. Do you feel that your life is empty?* | YES/No |
| 3. Are you afraid that something bad is going to happen to you?* | YES/No |
| 4. Do you feel happy most of the time?* | Yes/NO |
| 5. Have you dropped many of your activities and interests? | YES/No |
| 6. Do you often feel helpless? | YES/No |
| 7. Do you feel that you have more problems with memory than most? | YES/No |
| 8. Do you feel full of energy? | Yes/NO |
| 9. Do you feel that your situation is hopeless? | YES/No |
| 10. Do you think that most people are better off than you are? | YES/No |
note: One point is scored for each response in capital letters. A score of 3 or greater may indicate depression.
*—The first four questions are sometimes used as a four-item version of the scale, with one or more abnormal responses possibly indicating depression.
Adapted with permission from D'ath P, et al. Screening, detection and management of depression in elderly primary care attenders. I: The acceptability and performance of the 15 item Geriatric Depression Scale (GDS15) and the development of short versions. Fam Pract. 1994;11(3):264.
Table 3. Potential Causes of Depressive Symptoms
| Causes | Examples |
|---|---|
| Medication class or system | |
| Anticholinergics | Oxybutynin (Ditropan), cimetidine (Tagamet), antihistamines |
| Cardiac | Clonidine (Catapres), digoxin, hydralazine |
| Central nervous system | Levodopa, phenytoin (Dilantin), haloperidol |
| Hormones | Glucocorticoids, oral contraceptives, anabolic steroids |
| Sedatives | Benzodiazepines, ethanol, sleep aids |
| Illness | |
| Cancer | Pancreas, lung, colon |
| Endocrine | Hypothyroidism, hypercortisolism, Addison disease |
| Hematologic | Vitamin B12 deficiency, iron deficiency, leukemia |
| Infection | Syphilis, human immunodeficiency virus, pneumonia |
| Metabolic | Hypercalcemia, hyperkalemia, hypokalemia, porphyria |
| Neurologic | Alzheimer disease, stroke, intracranial mass |
| Impairments | |
| Hearing loss9 | — |
| Pain10 | Osteoarthritis, neuralgia |
| Substance abuse | Alcohol, opioids, benzodiazepines |
Treating depression in patients living in a nursing home may be problematic because polypharmacy makes medication interactions and adverse effects more likely. Compromised renal or hepatic function also may contribute to adverse reactions. Tricyclic antidepressants, selective serotonin reuptake inhibitors (SSRIs), serotonin-norepinephrine reuptake inhibitors, and other second-generation antidepressants have similar effectiveness. Based on their adverse effect profiles, SSRIs are the preferred medications for treating depression in older adults. Based on expert opinion, citalopram (Celexa), escitalopram (Lexapro), and sertraline (Zoloft) may be preferred because of fewer drug interactions or cognitive risks.11
Frail older patients are more likely to be taking other medications with serotonergic properties (Table 412 ). Therefore, care should be taken to avoid serotonin syndrome, which is manifested as autonomic (e.g., hyperthermia, hypertension, tachycardia), neuromotor (e.g., hyperreflexia, myoclonus, tremors) or cognitive/behavioral (e.g., confusion, anxiety, hallucinations) symptoms.12
Table 4. Drugs That May Cause Serotonin Syndrome

| Category | Examples |
|---|---|
| Amphetamines | Methylphenidate (Ritalin) |
| Analgesics | Meperidine (Demerol), tramadol (Ultram) |
| Antispasmodics | Cyclobenzaprine (Flexeril) |
| Cough and cold | Dextromethorphan |
| Herbals | St. John's wort (Hypericum perforatum) |
| Migraine (triptans) | Sumatriptan (Imitrex) |
| Monoamine oxidase inhibitors | Phenelzine (Nardil) |
| Selective serotonin reuptake inhibitors | Sertraline (Zoloft) |
| Serotonin-norepinephrine reuptake inhibitors | Venlafaxine (Effexor), duloxetine (Cymbalta) |
| Other serotonergic medications | Lithium, trazodone |
note: The risk of serotonin syndrome increases when agents are used in combination.
Information from reference 12.
Because hyponatremia has been linked to the use of SSRIs, serum sodium levels should be checked if a patient exhibits lethargy or delirium after starting therapy.13 SSRI use also increases the risk of falls, fractures, gastrointestinal bleeding, and sleep disturbances.14–17 The duration of therapy required to maintain remission is uncertain.18,19 Based on principles of geriatric pharmacotherapy, patients should have periodic assessments for continuing medication or tapering to a minimal effective dose.
Case 2. Three weeks ago, a 75-year-old man presented with a viral-sounding illness. The patient seemed apathetic, but commented that he needed to recover in time for hunting season. He later died of a self-inflicted gunshot wound.
White men older than 65 years account for a disproportionate number of completed suicides.1 Depression is a major risk factor for suicidal ideation (Table 5).20 Suicidal patients may present to their physician with seemingly unrelated symptoms shortly before making an attempt. A mood change, especially when means for self-harm (e.g., firearms) are readily available, should prompt a careful evaluation for suicidal ideation. Suicidal intent, the presence of a plan, and the means available to carry out the plan should be addressed directly in the interview.
Table 5. Risk Factors for Suicide

| Bereavement |
| Depression |
| Living alone, social isolation |
| Male sex |
| Poor health status, development of disability |
| Poor sleep quality |
| Substance abuse (e.g., alcohol, sedatives, pain medications) |
| White race |
Information from reference 20.
Management of suicidal ideation in older patients requires hospitalization, unless there is a reliable source of psychosocial support, and good follow-up is assured. Although SSRI therapy has been shown to reduce suicidal ideation, it has been difficult to demonstrate that it reduces the rate of suicide attempts.21,22 Medications more likely to be lethal in overdose (e.g., tricyclic antidepressants) should be avoided. Persisting suicidal ideation is one of the indications for electroconvulsive therapy, which may be safely administered to older patients. Other indications for electroconvulsive therapy are lack of response to medication, psychosis, and previous good response to this modality.23
Case 3. A 72-year-old woman had a myocardial infarction and underwent coronary artery bypass grafting four weeks ago. She has been participating in an outpatient cardiac rehabilitation program. Her therapist is concerned about her lack of progress and apparent apathy. The patient's son comments that she seems uninterested in participating in family activities and looks depressed.
About 20 percent of patients who have a stroke or myocardial infarction develop major depression.24,25 Depression persisting after an acute coronary event increases the risk of future cardiovascular events and death.26 In one study, response to treatment for depression was associated with a 7.4 percent risk of recurrent cardiac events, compared with a 25.6 percent risk in those whose depression did not respond to treatment.27
The American College of Cardiology and the American Heart Association recommend screening for and treating depression for secondary prevention in patients with ST-segment elevation myocardial infarction. Assessment is recommended during hospitalization, one month after discharge, and annually thereafter.28 Cognitive behavior therapy (CBT) or antidepressant medication is recommended for treatment. SSRIs are generally well tolerated by patients with cardiac conditions. Whether treatment of depression prevents future cardiovascular events is uncertain. A study of patients with acute coronary syndrome showed treatment of depression to be associated with greater patient satisfaction and a reduction of depressive symptoms, with a trend toward improved cardiac prognosis.29
Case 4. An 82-year-old woman comes to the office for a checkup three months after the death of her husband. The patient says her daughter asked her to make the appointment because she had not seemed like herself lately. The patient expresses anhedonia, and her 10-item Geriatric Depression Scale score is 7 out of 10. Her physical examination and laboratory tests are otherwise unremarkable. You prescribe a 30-day supply of an SSRI with three refills. Six weeks later, she says she discontinued the medication after the 30-day supply ran out and did not understand that she needed to get a refill. She is uncertain whether the medication was helpful.
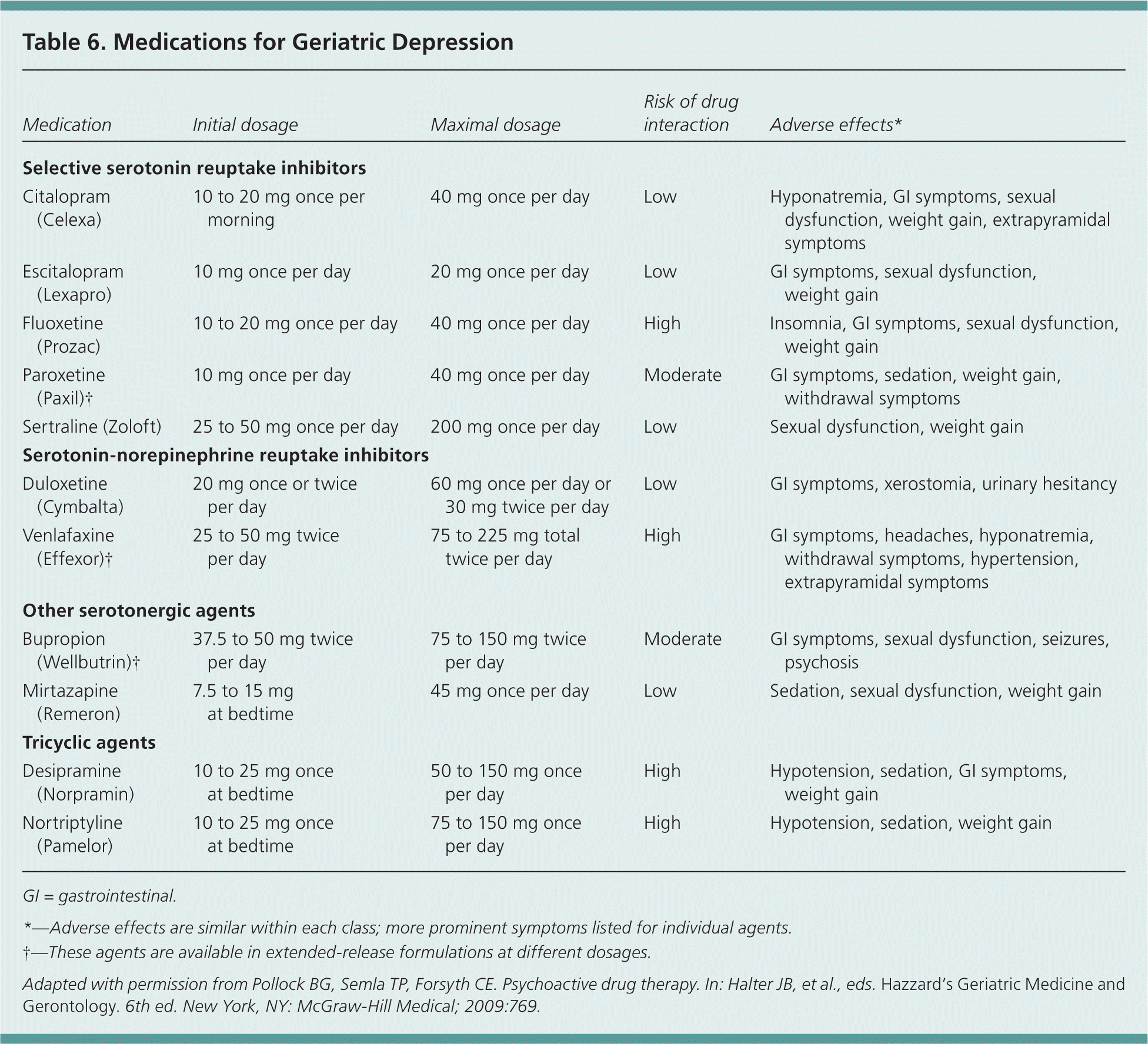
Depressive symptoms may be a normal part of bereavement. Symptoms causing functional impairment and persisting without improvement for more than two months after the loss of a loved one should result in consideration for treatment.30 After a diagnosis of depression is established, pharmacotherapy is one of several treatment options (Table 6).11
Table 6. Medications for Geriatric Depression
| Medication | Initial dosage | Maximal dosage | Risk of drug interaction | Adverse effects* |
|---|---|---|---|---|
| Selective serotonin reuptake inhibitors | ||||
| Citalopram (Celexa) | 10 to 20 mg once per morning | 40 mg once per day | Low | Hyponatremia, GI symptoms, sexual dysfunction, weight gain, extrapyramidal symptoms |
| Escitalopram (Lexapro) | 10 mg once per day | 20 mg once per day | Low | GI symptoms, sexual dysfunction, weight gain |
| Fluoxetine (Prozac) | 10 to 20 mg once per day | 40 mg once per day | High | Insomnia, GI symptoms, sexual dysfunction, weight gain |
| Paroxetine (Paxil) | 10 mg once per day | 40 mg once per day | Moderate | GI symptoms, sedation, weight gain, withdrawal symptoms |
| Sertraline (Zoloft) | 25 to 50 mg once per day | 200 mg once per day | Low | Sexual dysfunction, weight gain |
| Serotonin-norepinephrine reuptake inhibitors | ||||
| Duloxetine (Cymbalta) | 20 mg once or twice per day | 60 mg once per day or 30 mg twice per day | Low | GI symptoms, xerostomia, urinary hesitancy |
| Venlafaxine (Effexor) | 25 to 50 mg twice per day | 75 to 225 mg total twice per day | High | GI symptoms, headaches, hyponatremia, withdrawal symptoms, hypertension, extrapyramidal symptoms |
| Other serotonergic agents | ||||
| Bupropion (Wellbutrin)† | 37.5 to 50 mg twice per day | 75 to 150 mg twice per day | Moderate | GI symptoms, sexual dysfunction, seizures, psychosis |
| Mirtazapine (Remeron) | 7.5 to 15 mg at bedtime | 45 mg once per day | Low | Sedation, sexual dysfunction, weight gain |
| Tricyclic agents | ||||
| Desipramine (Norpramin) | 10 to 25 mg once at bedtime | 50 to 150 mg once per day | High | Hypotension, sedation, GI symptoms, weight gain |
| Nortriptyline (Pamelor) | 10 to 25 mg once at bedtime | 75 to 150 mg once per day | High | Hypotension, sedation, weight gain |
GI = gastrointestinal.
*—Adverse effects are similar within each class; more prominent symptoms listed for individual agents.
†—These agents are available in extended-release formulations at different dosages.
Adapted with permission from Pollock BG, Semla TP, Forsyth CE. Psychoactive drug therapy. In: Halter JB, et al., eds. Hazzard's Geriatric Medicine and Gerontology. 6th ed. New York, NY: McGraw-Hill Medical; 2009:769.
If medication is chosen, there is increasing evidence that a prescription with office-based follow-up is inferior to an organized program of depression care management or collaborative care.31,32 Depression care management involves the designation of an allied health professional to assist treatment by providing education and close follow-up, and monitoring response to treatment.33 A randomized study compared usual care with pharmacotherapy augmented by depression care management. It found improved remission rates and medication adherence over the 12-month intervention (number needed to treat = 4), and the results were sustained for another 12 months after intervention had ended (number needed to treat = 9).34 The evidence in favor of depression care management is strong enough that the U.S. Preventive Services Task Force (USPSTF) recommends screening for depression in adults (including older adults) only when staff-assisted depression care supports are in place to assure accurate diagnosis, effective treatment, and follow-up. The USPSTF notes that the evidence demonstrating a benefit of screening in the absence of depression care support is small.35
Structured psychotherapy yields depression remission rates similar to medication, and may be preferred in patients at higher risk of adverse drug reactions.36 CBT is the most widely studied form of psychotherapy and has been shown to be effective in geriatric depression, particularly in mild to moderately severe cases. CBT involves replacing negative distortions of events and situations with more positive and rational cognitive responses.37,38 There is some evidence that the effects of CBT may be longer lasting than drug therapy following discontinuation of treatment. Older persons do well with CBT, but need special attention because of memory impairment and sensory deficits, primarily hearing loss.39
There is some evidence that aerobic and anaerobic exercise programs are helpful for treating depression. A meta-analysis specific to older patients found evidence of benefit for major depression but the effects were not sustained unless the exercise program continued.40 A Cochrane review on exercise for adult depression found evidence of benefit comparable to cognitive therapy.41 Both reviews noted inconsistencies in the quality of the studies and the need for further research.

