
Am Fam Physician. 2011;84(12):1335-1336
Author disclosure: No relevant financial affiliations to disclose.
Several organizations have called for obstetric care professionals to decrease the number of elective (non-medically indicated) deliveries before an estimated gestational age of 39 weeks to prevent iatrogenic neonatal harm.1 More than 30 years ago, the American College of Obstetricians and Gynecologists made a similar recommendation against elective inductions,2 but approximately one out of every three births in the United States occurs between 34 and 38 6/7 weeks' gestation.3 Decreasing the number of deliveries before 39 weeks will decrease neonatal morbidity and associated costs.
A comparison of U.S. deliveries from 1990 and 2006 revealed an increase in late preterm deliveries (34 to 36 weeks) from 10 to 25 percent, whereas early term deliveries (37 to 38 6/7 weeks) increased by close to 50 percent.4 In an analysis of more than 13,000 elective cesarean deliveries, almost 36 percent were before 39 weeks.5 The cause of this rise in deliveries before 39 weeks is likely multifaceted, involving the health care professional,6 the patient, and her family.7 For example, a survey of pregnant women found that more than 90 percent believed that it was safe to deliver their baby before 39 weeks without medical indications, and more than 75 percent believed that full-term was 34 to 38 weeks.7 Common reasons given for elective delivery of early term pregnancies include intolerable maternal discomfort, a poor previous pregnancy outcome, suspected fetal macrosomia, history of shoulder dystocia, previous precipitous delivery, the patient lives remotely from the delivering hospital, convenience for family or physician schedule, and patient preference for a specific health care professional.
When there is no medical indication for early delivery, infants delivered before 39 weeks are exposed to numerous unnecessary risks. One group of investigators reviewed the morbidity of newborns by gestational weeks for term (377,638) and late preterm (26,170) deliveries.8 The baseline neonatal intensive care unit (NICU) admission rate at 39 weeks was 2.6 percent, but this rate nearly doubled for each week before 38 weeks.8 Another group analyzed 13,258 elective cesarean deliveries, of which 35.8 percent were performed before 39 weeks, and found that infants born before 39 weeks had a significantly increased risk of adverse outcomes (Table 1).5 Notably, this was also true for the neonates born at 38 weeks. A retrospective review of almost 180,000 births showed that the risk of severe respiratory distress syndrome was 22.5-fold higher for neonates born at 37 weeks and 7.5-fold higher for infants born at 38 weeks compared with those born at or after 39 weeks.9 The risk of an early term neonate being admitted to the NICU is approximately one in 20 deliveries, compared with about one in 50 for neonates born between 39 and 40 weeks.10 Deliveries before 39 weeks are expensive, with an average daily cost for a NICU admission of approximately $3,000.11
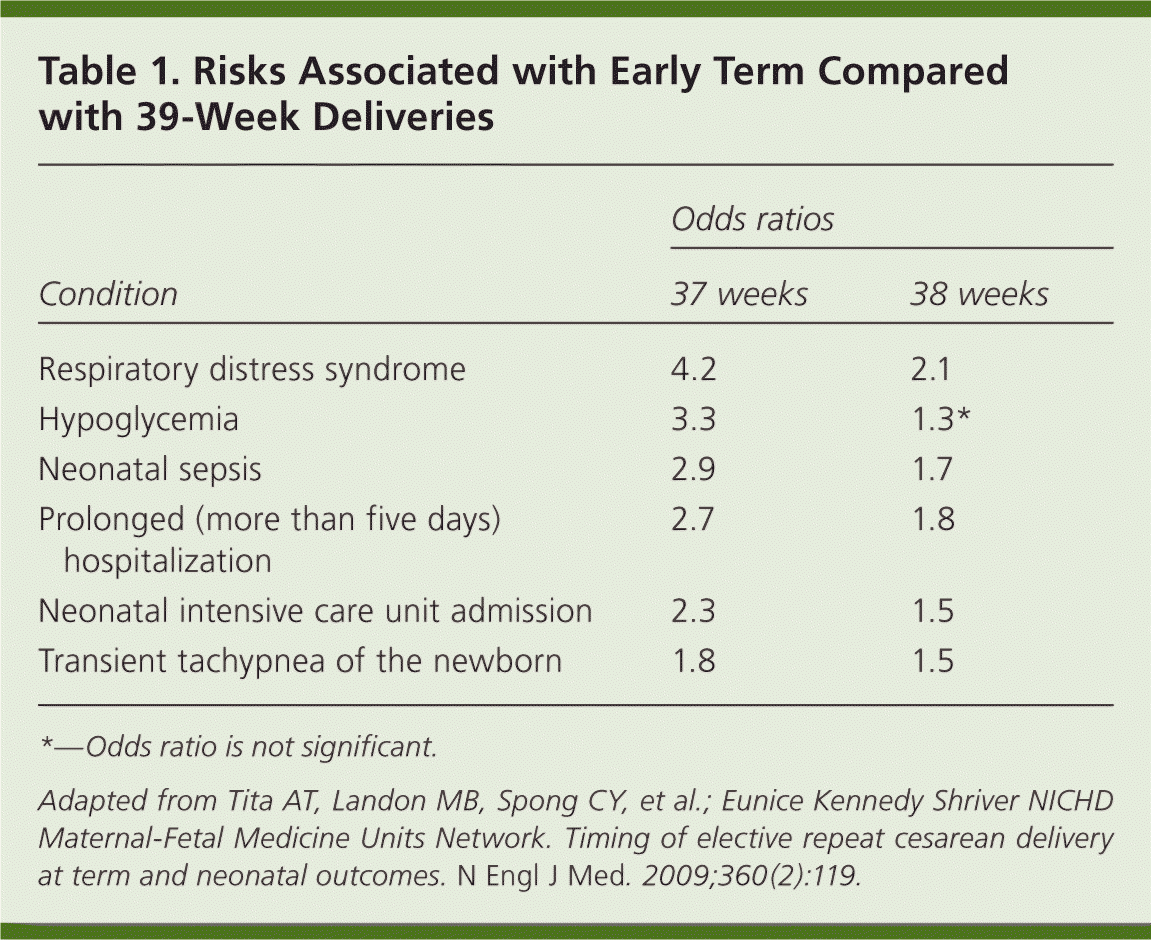
| Condition | Odds ratios | |
|---|---|---|
| 37 weeks | 38 weeks | |
| Respiratory distress syndrome | 4.2 | 2.1 |
| Hypoglycemia | 3.3 | 1.3* |
| Neonatal sepsis | 2.9 | 1.7 |
| Prolonged (more than five days) hospitalization | 2.7 | 1.8 |
| Neonatal intensive care unit admission | 2.3 | 1.5 |
| Transient tachypnea of the newborn | 1.8 | 1.5 |
Several hospital systems have implemented successful strategies that have reduced the number of elective deliveries before 39 weeks with improvement in outcomes and no increased risk of stillbirth.9,12,13 We have implemented a successful strategy using a multidisciplinary team that includes medical and nursing leadership. A critical step in this process is to confirm term gestation, using one of the following criteria: fetal heart tones have been documented for 30 or more weeks by Doppler ultrasonography; ultrasonography performed before 20 weeks' gestation supports an estimated gestational age of 39 or more weeks; or 36 weeks or more have passed since a positive urine or serum human chorionic gonadotropin pregnancy test result.14 Educating patients, obstetrics professionals, and nurses about the importance of preventing deliveries before 39 weeks' gestation; using a mandatory scheduling process and dating criteria form; and reviewing all scheduled inductions and cesarean deliveries before patient arrival are key components of a successful strategy (Table 2). Cases that do not meet criteria are discussed with the scheduling obstetric professional and, when necessary, mediated by the obstetrics department leadership. Copies of the forms we use for scheduling deliveries and auditing charts are available for download.15 In addition, a toolkit developed by the March of Dimes is available online.1

| Empower administrative, physician, and nursing champions |
| Establish a mandatory scheduling process |
| Educate patients, physicians, nurses, and schedulers about rationale for the process |
| Use a mandatory scheduling form that uses strict dating and delivery criteria15 |
| Review all scheduled deliveries before patient arrival |
| Use chain of command to mediate disagreements about dating or indications |
| Audit process regularly and discuss at peer-review or multidisciplinary committee meetings |
Having a 39-week elective delivery policy will help reduce NICU admissions, newborn morbidity, and medical costs. A policy mandating health care professionals to schedule elective deliveries after 39 weeks supports a key tenet of the Hippocratic teaching—to first, do no harm.
