A 31-year-old black man presented with a cough that began about four months before, when he was a smoker. Although he had quit smoking, his cough worsened. The cough was productive with scant yellow sputum and did not improve with a course of azithromycin (Zithromax). The patient did not have fever, weight loss, shortness of breath, or fatigue. He had not been exposed to occupational dust or chemicals; however, he was a firefighter. He had a history of allergic rhinitis for which he was taking fexofenadine/pseudoephedrine (Allegra-D). He had a family history of lung cancer and asthma.
On physical examination the patient appeared well and was afebrile. His nasal mucosa was swollen, and he had an injected pharynx. Findings on lung examination were normal. His lungs were clear to auscultation with normal inspiratory effort. There was no wheezing, rhonchi, or rales. Chest radiography was performed (see accompanying figure).
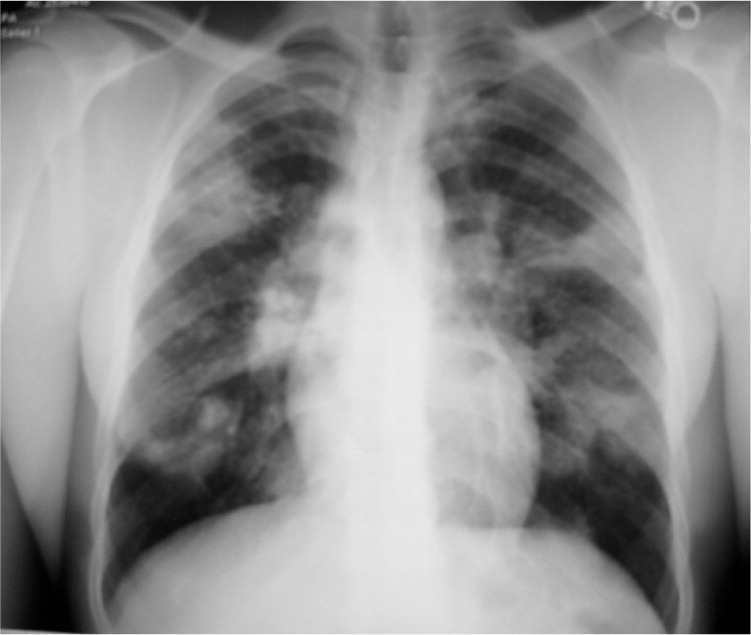
Question
Based on the patient’s history, physical examination, and radiologic findings, which one of the following is the most likely diagnosis?
A. Bronchogenic carcinoma.
B. Histoplasmosis.
C. Pneumocystis jiroveci pneumonia.
D. Sarcoidosis.
E. Tuberculosis.
Discussion
The answer is D: sarcoidosis. Sarcoidosis is a chronic multisystem granulomatous disease of unknown etiology. It typically affects young and middle-aged adults and is three to four times more common in blacks than in whites.1 Common presenting symptoms include cough, dyspnea, and chest pain. Chest radiography classically reveals bilateral hilar adenopathy with or without parenchymal opacities.2 In more advanced cases, hilar nodes may be smaller, and there may be evidence of pulmonary fibrosis and volume loss. Pleural involvement is rare.
The diagnosis of sarcoidosis requires suggestive clinical and radiologic findings, a histologic demonstration of noncaseating granulomas in involved organs, and the exclusion of alternative explanations.3 The first-line treatment of sarcoidosis is oral corticosteroids.3 Alternative agents include methotrexate, cyclophosphamide, azathioprine (Imuran), chloroquine (Aralen), and tumor necrosis factor antagonists. Patients may have spontaneous remission, or the clinical course may be chronic with progressive loss of lung function. The age-adjusted mortality rate is 4.32 per 1 million persons.4
Bronchogenic carcinoma is an unlikely cause of chronic cough; however, it should be considered in current and former smokers with a new cough or hemoptysis.5 Radiologic findings may vary from pleural thickening to nodules, lobar collapse, consolidation, unilateral hilar enlargement, or pleural effusion.
Histoplasmosis is endemic in fertile river valleys, such as those of the Mississippi, Missouri, Ohio, Saint Lawrence, and Rio Grande rivers.6 Infections in patients who are immunocompetent are generally asymptomatic but may cause fever, chills, dry or productive cough, arthralgias, and rash. The diagnosis relies on high or rising serum antibody complement fixation titers.7 Radiographs may show ill-defined opacities, areas of consolidation, hilar adenopathy, pulmonary nodules, parenchymal infiltrates, cavitation, and mediastinal fibrosis. Granulomas are typically caseating.
Pneumocystis jiroveci (formerly Pneumocystis carinii) is an opportunistic pathogen that commonly infects immunocompromised patients, such as those with AIDS. Characteristic symptoms are fever, nonproductive cough, disproportionate breathlessness, and failure to respond to standard antibiotics. Common radiologic findings are bilateral, diffuse interstitial infiltrates without hilar adenopathy. Pneumatoceles or pneumothorax may be present, but pleural effusions are absent. Findings on chest radiography are normal in about 5 to 10 percent of patients with P. jiroveci infection.8 The diagnosis is confirmed if the organism is identified in sputum using specific stains.8 Adequate specimens can be obtained through induced sputum or bronchoalveolar lavage.
Patients with tuberculosis typically present with the slowly progressive constitutional symptoms of malaise, fever, night sweats, weight loss, and chronic cough. Radiographic abnormalities include hilar and paratracheal lymph node enlargement, infiltrates, atelectasis, pleural effusion, and cavitation.7 A tuberculin skin test identifies Mycobacterium tuberculosis infection, but does not distinguish between latent and active disease. The diagnosis can be confirmed if M. tuberculosis is identified with cultures or with DNA or RNA amplification techniques.7
Summary Table

| Condition | Radiographic findings |
|---|---|
| Bronchogenic carcinoma | Findings vary and may include unilateral hilar enlargement; peripheral pulmonary opacity; lung, lobar, or segmental collapse; nodules; consolidation; pleural thickening; pleural effusion; broadening of mediastinum; enlarged cardiac shadow; elevation of hemidiaphragm; rib destruction |
| Histoplasmosis | Ill-defined opacities; areas of consolidation; parenchymal infiltrates; pulmonary nodules; hilar adenopathy; cavitation; mediastinal fibrosis |
| Pneumocystis jiroveci pneumonia | Bilateral, diffuse interstitial infiltrates without hilar adenopathy; pneumatoceles or pneumothorax may be present; pleural effusions are absent; chest radiographs may appear normal |
| Sarcoidosis | Stage I: Bilateral hilar enlargement, usually symmetric; paratracheal nodes often enlarged; spontaneous resolution within one year in most cases |
| Stage II: Combination of hilar glandular enlargement and pulmonary opacities that are often diffuse | |
| Stage III: Diffuse pulmonary shadows without evidence of hilar adenopathy | |
| Stage IV: Pulmonary fibrosis; volume loss; pleural involvement rare | |
| Tuberculosis | Small homogenous infiltrates; hilar and paratracheal lymph node enlargement; atelectasis from airway compression; cavitation; pleural effusion |

