Febrile seizures are common in the first five years of life, and many factors that increase seizure risk have been identified. Initial evaluation should determine whether features of a complex seizure are present and identify the source of fever. Routine blood tests, neuroimaging, and electroencephalography are not recommended, and lumbar puncture is no longer recommended in patients with uncomplicated febrile seizures. In the unusual case of febrile status epilepticus, intravenous lorazepam and buccal midazolam are first-line agents. After an initial febrile seizure, physicians should reassure parents about the low risk of long-term effects, including neurologic sequelae, epilepsy, and death. However, there is a 15 to 70 percent risk of recurrence in the first two years after an initial febrile seizure. This risk is increased in patients younger than 18 months and those with a lower fever, short duration of fever before seizure onset, or a family history of febrile seizures. Continuous or intermittent antiepileptic or antipyretic medication is not recommended for the prevention of recurrent febrile seizures.
Febrile seizures are the most common seizures of childhood, occurring in 2 to 5 percent of children six months to five years of age.1 As defined by the American Academy of Pediatrics (AAP), febrile seizures occur in the absence of intracranial infection, metabolic disturbance, or history of afebrile seizures, and are classified as simple or complex1,2 (Table 11,3 ). Simple febrile seizures represent 65 to 90 percent of febrile seizures2 and require all of the following features: a duration of less than 15 minutes, generalized in nature, a single occurrence in a 24-hour period, and no previous neurologic problems.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
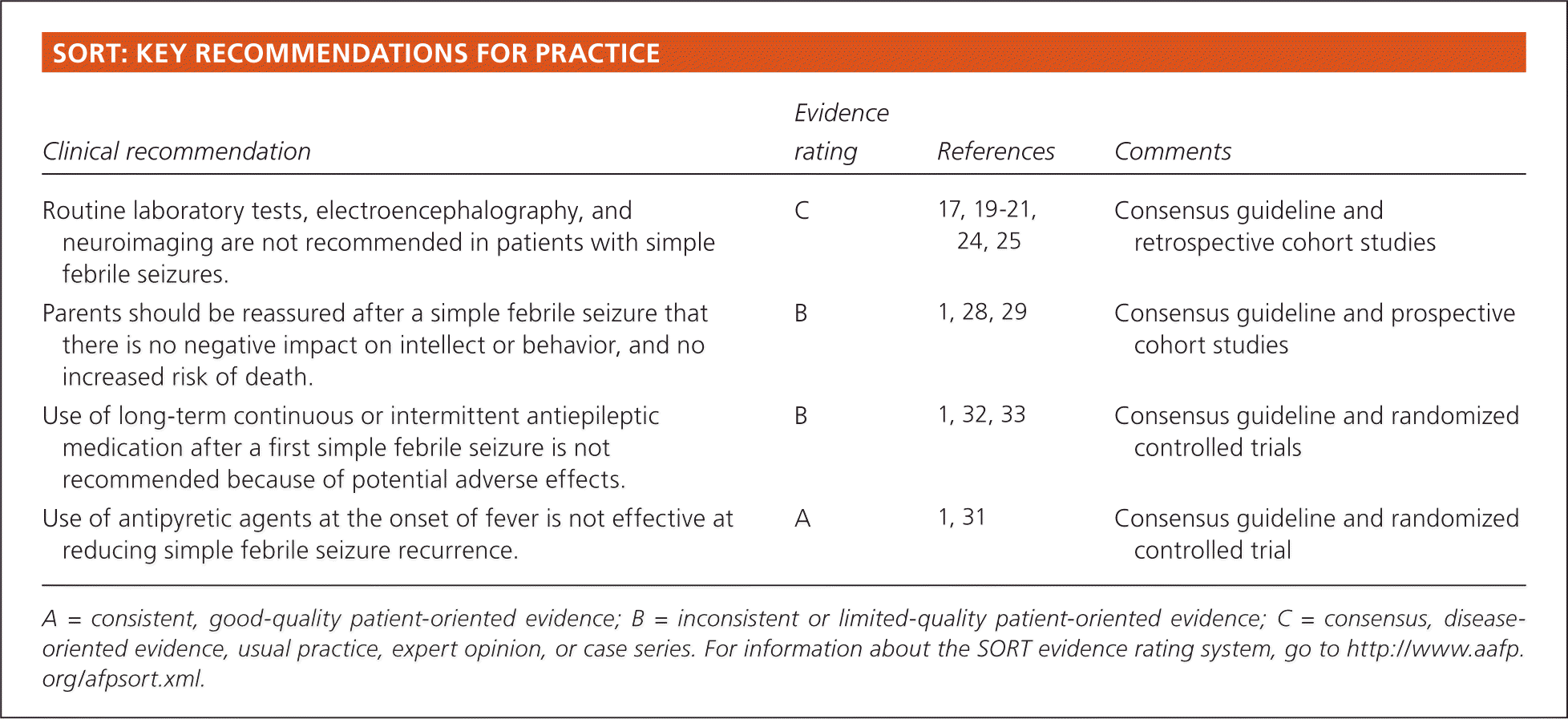
| Routine laboratory tests, electroencephalography, and neuroimaging are not recommended in patients with simple febrile seizures. | C | 17, 19–21, 24, 25 | Consensus guideline and retrospective cohort studies |
| Parents should be reassured after a simple febrile seizure that there is no negative impact on intellect or behavior, and no increased risk of death. | B | 1, 28, 29 | Consensus guideline and prospective cohort studies |
| Use of long-term continuous or intermittent antiepileptic medication after a first simple febrile seizure is not recommended because of potential adverse effects. | B | 1, 32, 33 | Consensus guideline and randomized controlled trials |
| Use of antipyretic agents at the onset of fever is not effective at reducing simple febrile seizure recurrence. | A | 1, 31 | Consensus guideline and randomized controlled trial |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Table 1. Classification of Febrile Seizures

| Simple (all of the following) |
| Duration of less than 15 minutes |
| Generalized |
| No previous neurologic problems |
| Occur once in 24 hours |
| Complex (any of the following) |
| Duration of more than 15 minutes |
| Focal |
| Recurs within 24 hours |
Adapted with permission from Millar JS. Evaluation and treatment of the child with febrile seizure. Am Fam Physician. 2006;73(10):1761, with additional information from reference 1.
Risk Factors
Risk factors for febrile seizures include developmental delay, discharge from a neonatal unit after 28 days, day care attendance, viral infections, a family history of febrile seizures, certain vaccinations, and possibly iron and zinc deficiencies.4–13 Febrile seizures may occur before or soon after the onset of fever, with the likelihood of seizure increasing with the child's temperature and not with the rate of temperature rise.4
Vaccinations associated with increased risk include 2010 Southern Hemisphere seasonal influenza trivalent inactivated vaccine (Fluvax Junior and Fluvax); diphtheria and tetanus toxoids and whole-cell pertussis (DTP); and measles, mumps, and rubella (MMR).13–15 A Cochrane review and a review of 530,000 children receiving the MMR vaccine showed that the risk of febrile seizures increased only during the first two weeks after vaccination, was small (an additional one or two febrile seizures per 1,000 vaccinations), and was likely related to fever from the vaccine.6,9
A genetic predisposition for febrile seizures has been postulated, although no susceptibility gene has been identified. Genetic abnormalities have been reported in persons with febrile epilepsy syndromes, such as severe myoclonic epilepsy in infancy and generalized epilepsy with febrile seizures plus (GEFS+).14 Most causes of febrile seizures are multifactorial, with two or more genetic and contributing environmental factors.
Case-control studies suggest that iron and zinc deficiencies may also be risk factors for febrile seizures. One study of febrile seizures in Indian children three months to five years of age showed lower serum zinc levels in patients with seizures compared with age-matched febrile patients without seizures.7 In another study, children with febrile seizures had nearly two times the incidence of iron deficiency compared with febrile children who did not have seizures.8
Viral infections are a common cause of fever that triggers febrile seizures. A particular risk for febrile seizure is associated with primary human herpesvirus 6 infection, which is typically acquired during the first two years of life. In a case-control study, polymerase chain reaction testing and antibody titers suggested that 10 of 55 children (18 percent) who experienced a first febrile seizure had acute herpesvirus 6 infection, whereas none of the 85 children with fever but no seizure had evidence of such infection.12 Other common viral infections, such as influenza, adenovirus, and parainfluenza, are associated with simple and complex febrile seizures.11
Evaluation
Children should be promptly evaluated after an initial seizure. Most patients with febrile seizures present for medical care after resolution of the seizure and return to full alertness within an hour of the seizure.16 The initial evaluation should focus on determining the source of the fever.3,17 Parents should be questioned about a family history of febrile seizures or epilepsy, immunizations, recent antibiotic use, duration of the seizure, a prolonged postictal phase, and any focal symptoms. During the examination, attention should be given to the presence of meningeal signs and to the child's level of consciousness. In a 20-year retrospective review of 526 cases of bacterial meningitis, 93 percent of patients presented with altered consciousness.18
Routine laboratory studies in patients with simple febrile seizures are discouraged because electrolyte abnormalities and serious bacterial illnesses are rare.16,19,20 In a retrospective review of 379 children with simple febrile seizures, only eight were found to have bacteremia.21 Streptococcus pneumoniae was isolated in seven of the eight children, in an era before routine pneumococcal vaccination.
The AAP recently updated its 1996 guideline regarding the use of lumbar puncture in children with simple febrile seizures.17 A lumbar puncture is now an option when evaluating children six to 12 months of age whose immunization status for Haemophilus influenzae type b and S. pneumoniae is incomplete or unknown, and in those pretreated with antibiotics.17 This differs from the previous recommendation that lumbar puncture be performed in all children younger than 12 months and strongly considered in those 12 to 18 months of age. Currently, as in the previous guideline, a lumbar puncture is strongly recommended in those with meningeal signs and in those with any other findings from the history or physical examination that are concerning for intracranial infection.17,19
The AAP's updated recommendations are supported by evidence from observational studies, as well as two reviews.16 In the 20-year retrospective review mentioned previously, no patients with bacterial meningitis presented with only fever and seizure.18 In a more recent review of 704 patients with simple febrile seizures and no other findings concerning for bacterial meningitis, no cases of meningitis were identified.22 A second study reviewed 526 cases of complex febrile seizures and found only three cases of bacterial meningitis.23 Of these, one patient was unresponsive at presentation, and another had clear indications for lumbar puncture based on physical findings. The third was treated for bacterial meningitis after she had a negative lumbar puncture in the presence of S. pneumoniae bacteremia.
Electroencephalography has not been shown to predict recurrence of febrile seizures or future epilepsy in patients with simple febrile seizures.17,19 Routine neuroimaging after simple febrile seizures is discouraged; it also has no additional diagnostic or prognostic value, and in the case of computed tomography, carries a small increased risk of cancer.16,19,24 Even after first complex febrile seizures, neuroimaging is not likely to be helpful in well-appearing children. In a review of 71 patients with first complex seizures, none had intracranial findings necessitating acute medical or surgical intervention.25 Electroencephalography and neuroimaging may be considered in children with neurologic abnormalities on examination and in those with recurrent febrile seizures.26
Acute Treatment
Although most febrile seizures have resolved by the time of presentation, physicians should be prepared to treat patients with febrile status epilepticus. In the acute setting, intravenous lorazepam (Ativan) in a dose of 0.1 mg per kg is the treatment of choice for acute tonicclonic pediatric seizures. A Cochrane review found lorazepam to be as effective as diazepam (Valium), with fewer adverse effects and less need for additional antiepileptic agents.27 The same study found buccal midazolam to be superior to rectal diazepam (Diastat) when intravenous administration is not possible.
Prognosis and Long-term Management
Physicians can play a vital role in reassuring families about the good prognosis after a febrile seizure. Key concerns to be addressed include the risks of neurologic morbidity (including epilepsy), mortality, and seizure recurrence.
Parents should be reassured that children without underlying developmental problems do not seem to have lasting neurologic effects from febrile seizures. A population-based study in the United Kingdom that included 381 children with febrile seizures reported that those with febrile seizures perform as well as others academically, intellectually, and behaviorally when assessed at 10 years of age.28 Parents should be told that mortality from febrile seizures is very rare—so rare that it is difficult to assess accurately. A large cohort study in Denmark examined mortality rates in 1.6 million children.29 There was a slight increase in mortality (adjusted mortality rate ratio of 1.99) during the two years after a complex febrile seizure, but no significant increase among those with simple febrile seizures.
Parents should be warned that febrile seizures reoccur frequently. One cohort study found that 32 percent of children presenting with an initial febrile seizure later had additional febrile seizures, 75 percent of which occurred within one year.30 Risk factors and risk of recurrence after an initial febrile seizure are provided in Table 2.30 The risk of recurrence is similar between simple and complex febrile seizures.
Table 2. Risk of Recurrence After an Initial Febrile Seizure

| Risk factors | |
| Age < 18 months | |
| Duration of fever < 1 hour before seizure onset | |
| First-degree relative with febrile seizure | |
| Temperature < 104°F (40°C) | |
| Number of risk factors | 2-year risk of recurrence (%) |
| 0 | 14 |
| 1 | > 20 |
| 2 | > 30 |
| 3 | > 60 |
| 4 | > 70 |
Information from reference 30.
Multiple agents have been evaluated in the prevention of recurrent simple febrile seizures. Continuous use of phenobarbital, primidone (Mysoline), and valproic acid (Depakene) has proved effective in reducing recurrence of simple febrile seizures.1 However, these agents are not recommended because of associated adverse effects, the burden of long-term compliance, and a lack of data showing a reduced risk of future epilepsy with prevention of recurrent simple febrile seizures.1
Intermittent use of antipyretics or anticonvulsants at the onset of fever is not recommended. No studies have shown a reduction in recurrent simple febrile seizures when antipyretics are given at the onset of fever. In a randomized, placebo-controlled, double-blind trial, no decrease in febrile seizure recurrence was observed with scheduled administration of maximal doses of acetaminophen or ibuprofen.31 Although intermittent use of oral diazepam at the onset of fever is effective at reducing recurrence of simple febrile seizures, the AAP does not recommend it because of potential adverse effects and because many recurrent febrile seizures occur before recognition of fever.1,32,33 If parental anxiety is high, oral diazepam given at the onset of a child's fever may be considered. Additionally, rectal administration of diazepam for abortive use at home may be considered in those with an initial prolonged febrile seizure and in those at highest risk of recurrence.
Some population cohort studies have indicated that children with a history of febrile seizures have an increased but still low rate of epilepsy.34 A Danish cohort study of 1.54 million persons found that the long-term risk of epilepsy is increased 5.43-fold after febrile seizures, but did not distinguish between simple and complex febrile seizures.34 Risk factors included a family history of epilepsy, cerebral palsy, and Apgar score less than 7 at five minutes. Parents can be reassured that the risk of epilepsy after an initial simple febrile seizure is approximately 2 percent.35,36 This risk increases in children with complex febrile seizures. In one study, children with one complex seizure feature had a risk of 6 to 8 percent.36 In those with two or three complex features, the risk was 17 to 22 percent and 49 percent, respectively. Risk factors for the development of future epilepsy are included in Table 3.37
Table 3. Risk Factors for Future Epilepsy After a Febrile Seizure

| Complex febrile seizure* |
| Family history of epilepsy |
| Fever duration < 1 hour before seizure onset |
| Neurodevelopmental abnormality (e.g., cerebral palsy, hydrocephalus) |
*—Febrile seizures with multiple complex features are a possible risk factor.
Adapted with permission from Shinnar S, Glauser TA. Febrile seizures. J Child Neurol. 2002;17(suppl 1):S46.
Data Sources: We used the term febrile seizures to search PubMed for all articles from 2004 to the present for children younger than 18 years. Another search was performed with no date limits using the term febrile convulsion. The same terms and limitations were used to search PubMed Clinical Inquiries in the diagnosis and therapy categories. The National Guideline Clearinghouse, Cochrane Database of Systematic Reviews, UpToDate, Dynamed, Agency for Healthcare Research and Quality, Institute for Clinical Systems Improvement, U.S. Preventive Services Task Force, Ovid Evidence-Based Medicine Reviews (including systematic reviews from Cochrane, DARE, and ACP Journal Club), and Bandolier were also searched using the term febrile seizure. Search date: October 2010.

