Herpes simplex virus infection and syphilis are the most common causes of genital ulcers in the United States. Other infectious causes include chancroid, lymphogranuloma venereum, granuloma inguinale (donovanosis), secondary bacterial infections, and fungi. Noninfectious etiologies, including sexual trauma, psoriasis, Behçet syndrome, and fixed drug eruptions, can also lead to genital ulcers. Although initial treatment of genital ulcers is generally based on clinical presentation, the following tests should be considered in all patients: serologic tests for syphilis and darkfield microscopy or direct fluorescent antibody testing for Treponema pallidum, culture or polymerase chain reaction test for herpes simplex virus, and culture for Haemophilus ducreyi in settings with a high prevalence of chancroid. No pathogen is identified in up to 25 percent of patients with genital ulcers. The first episode of herpes simplex virus infection is usually treated with seven to 10 days of oral acyclovir (five days for recurrent episodes). Famciclovir and valacyclovir are alternative therapies. One dose of intramuscular penicillin G benzathine is recommended to treat genital ulcers caused by primary syphilis. Treatment options for chancroid include a single dose of intramuscular ceftriaxone or oral azithromycin, ciprofloxacin, or erythromycin. Lymphogranuloma venereum and donovanosis are treated with 21 days of oral doxycycline. Treatment of noninfectious causes of genital ulcers varies by etiology, and ranges from topical wound care for ulcers caused by sexual trauma to consideration of subcutaneous pegylated interferon alfa-2a for ulcers caused by Behçet syndrome.
Genital ulcers may be caused by infectious or noninfectious etiologies (Table 1).1–3 Sexually transmitted infections (STIs) characterized by genital ulcers include genital herpes simplex virus (HSV) infection, syphilis (Treponema pallidum), chancroid (Haemophilus ducreyi), granuloma inguinale (donovanosis; Calymmatobacterium granulomatis), and lymphogranuloma venereum (Chlamydia trachomatis serotypes L1, L2, and L3). Secondary bacterial infections or fungi can also cause genital ulcers. Noninfectious etiologies include psoriasis, sexual trauma, Behçet syndrome, Wegener granulomatosis, and fixed drug eruptions.1,4 In the United States, most young, sexually active patients who present with genital ulcers have HSV infection or syphilis.1,4 Lymphogranuloma venereum, donovanosis, secondary bacterial infections, fungi, and noninfectious etiologies are rare.
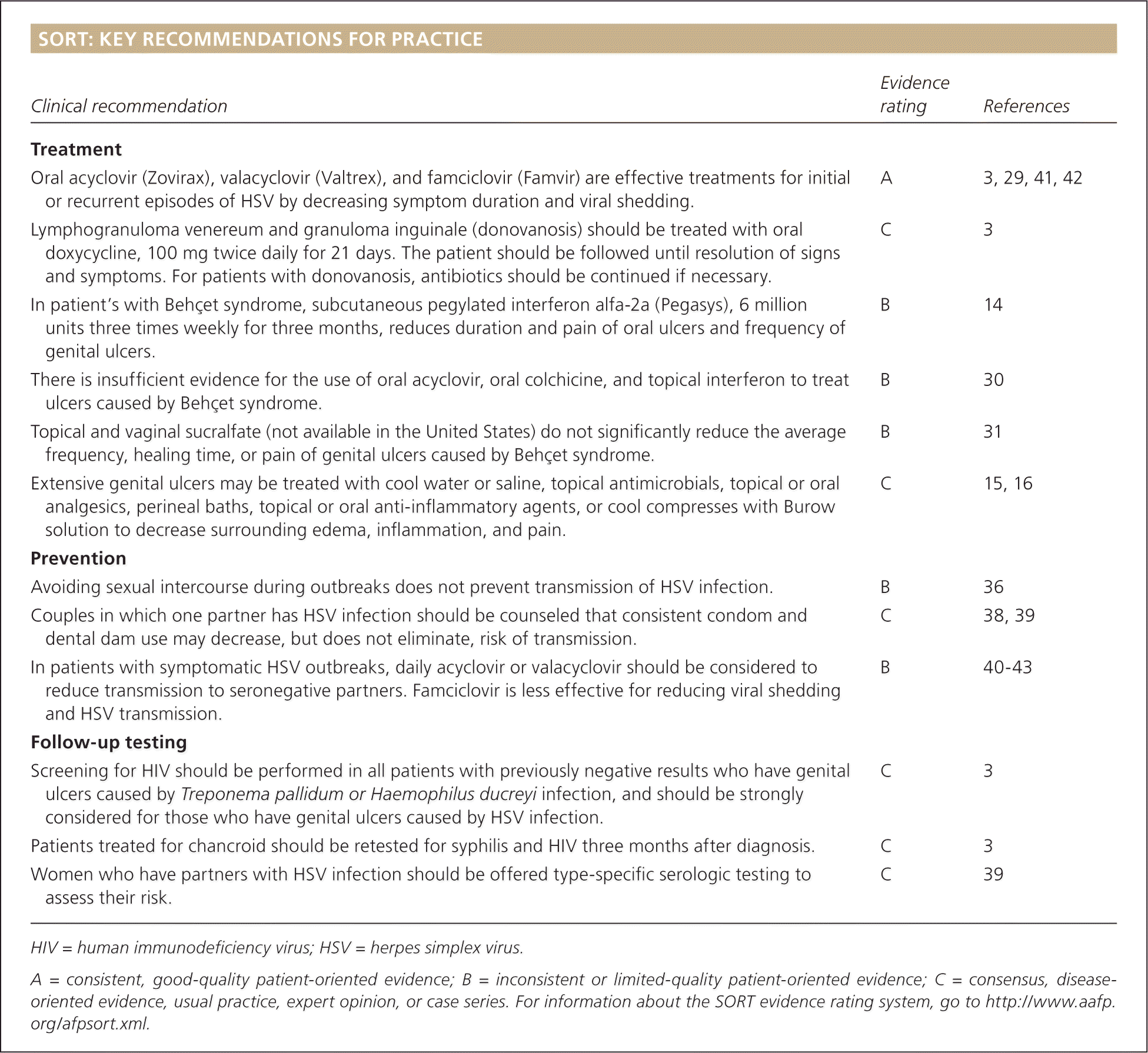
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Treatment | ||
| Oral acyclovir (Zovirax), valacyclovir (Valtrex), and famciclovir (Famvir) are effective treatments for initial or recurrent episodes of HSV by decreasing symptom duration and viral shedding. | A | 3, 29, 41, 42 |
| Lymphogranuloma venereum and granuloma inguinale (donovanosis) should be treated with oral doxycycline, 100 mg twice daily for 21 days. The patient should be followed until resolution of signs and symptoms. For patients with donovanosis, antibiotics should be continued if necessary. | C | 3 |
| In patient's with Behçet syndrome, subcutaneous pegylated interferon alfa-2a (Pegasys), 6 million units three times weekly for three months, reduces duration and pain of oral ulcers and frequency of genital ulcers. | B | 14 |
| There is insufficient evidence for the use of oral acyclovir, oral colchicine, and topical interferon to treat ulcers caused by Behçet syndrome. | B | 30 |
| Topical and vaginal sucralfate (not available in the United States) do not significantly reduce the average frequency, healing time, or pain of genital ulcers caused by Behçet syndrome. | B | 31 |
| Extensive genital ulcers may be treated with cool water or saline, topical antimicrobials, topical or oral analgesics, perineal baths, topical or oral anti-inflammatory agents, or cool compresses with Burow solution to decrease surrounding edema, inflammation, and pain. | C | 15, 16 |
| Prevention | ||
| Avoiding sexual intercourse during outbreaks does not prevent transmission of HSV infection. | B | 36 |
| Couples in which one partner has HSV infection should be counseled that consistent condom and dental dam use may decrease, but does not eliminate, risk of transmission. | C | 38, 39 |
| In patients with symptomatic HSV outbreaks, daily acyclovir or valacyclovir should be considered to reduce transmission to seronegative partners. Famciclovir is less effective for reducing viral shedding and HSV transmission. | B | 40–43 |
| Follow-up testing | ||
| Screening for HIV should be performed in all patients with previously negative results who have genital ulcers caused by Treponema pallidum or Haemophilus ducreyi infection, and should be strongly considered for those who have genital ulcers caused by HSV infection. | C | 3 |
| Patients treated for chancroid should be retested for syphilis and HIV three months after diagnosis. | C | 3 |
| Women who have partners with HSV infection should be offered type-specific serologic testing to assess their risk. | C | 39 |
HIV = human immunodeficiency virus; HSV = herpes simplex virus.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Table 1. Differential Diagnosis of Genital Ulcers

| Infectious (most common)* |
| Genital herpes simplex virus |
| Syphilis |
| Chancroid |
| Lymphogranuloma venereum |
| Granuloma inguinale (donovanosis) |
| Fungal infection (e.g., Candida) |
| Secondary bacterial infection |
| Noninfectious (less common) |
| Behçet syndrome |
| Fixed drug eruption |
| Psoriasis |
| Sexual trauma |
| Wegener granulomatosis |
*—Listed in order of frequency.
Epidemiology
The global incidence of genital ulcer disease is estimated to be more than 20 million cases annually.4 HSV types 1 and 2 are the most common causes of genital ulcers in the United States, followed by syphilis and chancroid.5 One in five women and one in nine men 14 to 49 years of age has genital HSV type 2 infection.6
In 2009, the rate of syphilis was highest in men and women 20 to 24 years of age (20.7 and 5.6 cases per 100,000 persons, respectively). However, syphilis rates increased in persons 15 to 19 years of age between 2002 and 2009 (1.3 versus 6.0 cases per 100,000 males and 1.5 versus 3.3 cases per 100,000 females).7,8 In 2006, most cases of primary and secondary syphilis occurred in men who have sex with men.7,8
Chancroid usually occurs in discrete outbreaks, but the disease may be endemic in some regions. The incidence of chancroid has been declining in the United States, with only 28 cases reported to state health departments in 2009.9 However, H. ducreyi infection is challenging to confirm, likely leading to underreporting.9 Approximately 10 percent of patients with chancroid are coinfected with syphilis or HSV; these are even more common coinfections for patients who acquired chancroid outside the United States.5
Lymphogranuloma venereum primarily occurs in men who have sex with men.10 Behçet syndrome is most common in young adults in the Eastern Mediterranean and in men in the Far East, whereas women are predominantly affected in the United States.2
Diagnostic Evaluation
The diagnosis of genital ulcer disease is based on the presence of one or more mucocutaneous ulcers involving the genitalia, perineum, or anus.5 Diagnosing the specific cause of genital ulcers is based on history, physical examination, and laboratory findings.
HISTORY AND PHYSICAL EXAMINATION
Risk factors for infectious causes of genital ulcers are similar to those for STIs, whereas risk factors for noninfectious causes vary (Table 21–3,5,6 ). For instance, patients with psoriasis are at greater risk of genital ulcers after exposure to trauma or medications such as nonsteroidal anti-inflammatory drugs, antimalarials, angiotensin-converting enzyme inhibitors, beta blockers, lithium, salicylates, or corticosteroids.1 Behçet syndrome is associated with the human leukocyte antigen-B51/B5 allele (57.2 percent of patients with the allele have the condition).11 History and physical examination findings associated with genital ulcers are summarized in Table 3.1,3,5,12–16
Table 2. Risk Factors for Genital Ulcers

| History of inflammatory disease (e.g., psoriasis) and exposure to trauma or medications such as nonsteroidal anti-inflammatory drugs, antimalarials, angiotensin-converting enzyme inhibitors, beta blockers, lithium, salicylates, or corticosteroids |
| Lack of male circumcision |
| Multiple sex partners, lifetime or current |
| Nonrecognition of ulcers in prodrome stage |
| Serodiscordant sex partners (i.e., one partner with herpes simplex virus and one without) |
| Unprotected sexual contact |
| Unprotected skin-to-skin contact with ulcers |
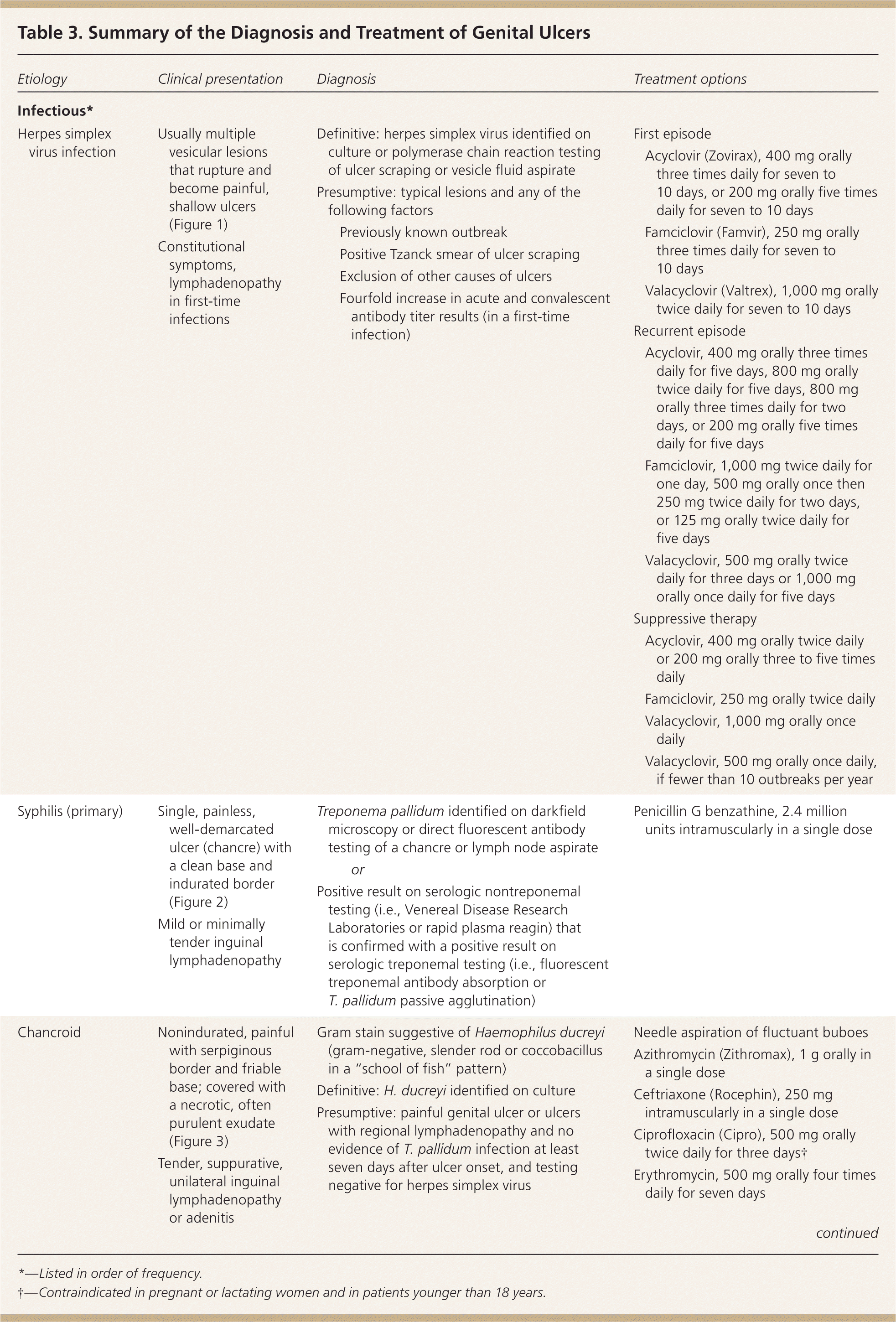
Table 3. Summary of the Diagnosis and Treatment of Genital Ulcers
| Etiology | Clinical presentation | Diagnosis | Treatment options | |||
|---|---|---|---|---|---|---|
| Infectious* | ||||||
| Herpes simplex virus infection |
|
|
| |||
| Syphilis (primary) |
|
|
| |||
| Chancroid |
|
|
| |||
| Lymphogranuloma venereum |
|
|
| |||
| Granuloma inguinale (donovanosis) |
|
|
| |||
| Noninfectious | ||||||
| Behçet syndrome |
|
|
| |||
| Fixed drug eruptions |
|
|
| |||
*—Listed in order of frequency.
†—Contraindicated in pregnant or lactating women and in patients younger than 18 years.
Genital HSV infection usually begins as multiple vesicular lesions, sometimes painless, that are located inside the foreskin, labia, vagina, or rectum. Vesicles may rupture spontaneously, becoming painful, shallow ulcers (Figure 1).17 Prodromal symptoms may occur in 20 percent of HSV cases before ulceration. The prodrome may include a mild tingling sensation up to 48 hours before ulceration, or shooting pain in the buttocks, legs, or hips up to five days before.12 Asymptomatic viral shedding may occur in more than 60 percent of patients with HSV infection.18 First-time infections may also feature constitutional symptoms and regional lymphadenopathy.3
Figure 1.
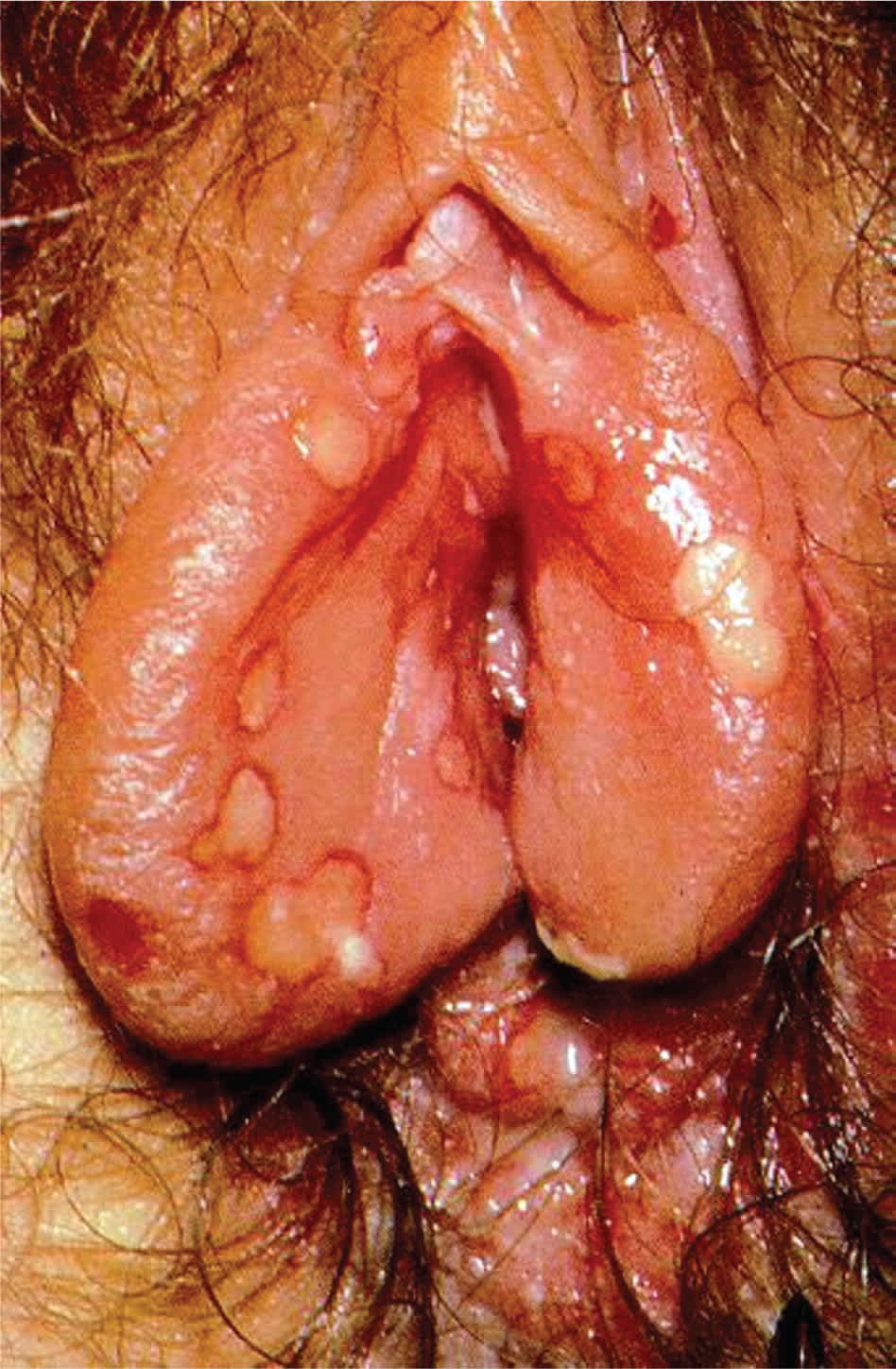
Genital herpes simplex virus. Painful, shallow ulcers may manifest from ruptured vesicular lesions.
Reprinted with permission from Sharma R, Dronen SC. Herpes simplex in emergency medicine. Medscape Reference. http://emedicine.medscape.com/article/783113-overview. Accessed September 13, 2011.
Primary syphilis usually begins with a single, painless, well-demarcated ulcer (chancre) with a clean base and indurated border19 (Figure 2). When the patient seeks treatment for signs or symptoms, the solitary chancre of primary infection may still be visible, or it may have progressed to secondary infection (e.g., rash, lymphadenopathy) or tertiary infection (e.g., gummatous lesions).
Figure 2.
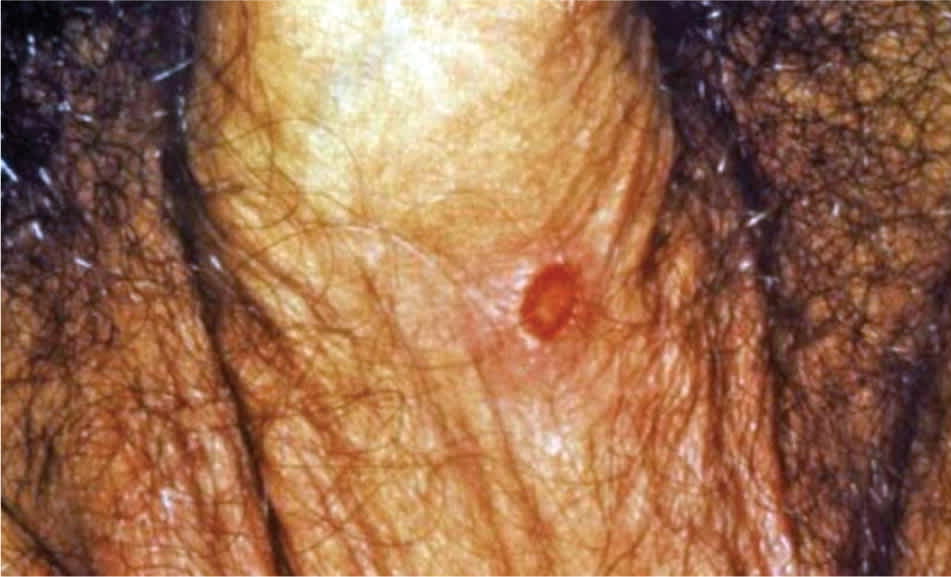
Primary syphilis begins as a single, well-demarcated ulcer (chancre) with a clean base and indurated border.
Photo courtesy of N.J. Fiumara, Gavin Hart; Centers for Disease Control and Prevention.
Chancroid ulcers are usually nonindurated and painful with a serpiginous border and friable base (Figure 3). The ulcers occur on the prepuce and frenulum of the penis in men or on the vulva or cervix in women. Perineal lesions are common in women or in men who have sex with men. Painful, unilateral, inguinal adenitis occurs in one-half of patients with chancroid and may develop into buboes.19,20 Fluctuant buboes may rupture spontaneously if not aspirated or incised and drained. Complications of chancroid include phimosis in men and further ulceration caused by secondary bacterial infection.20 Extragenital lesions on the inner thighs and fingers have been reported but are relatively rare.20
Figure 3.
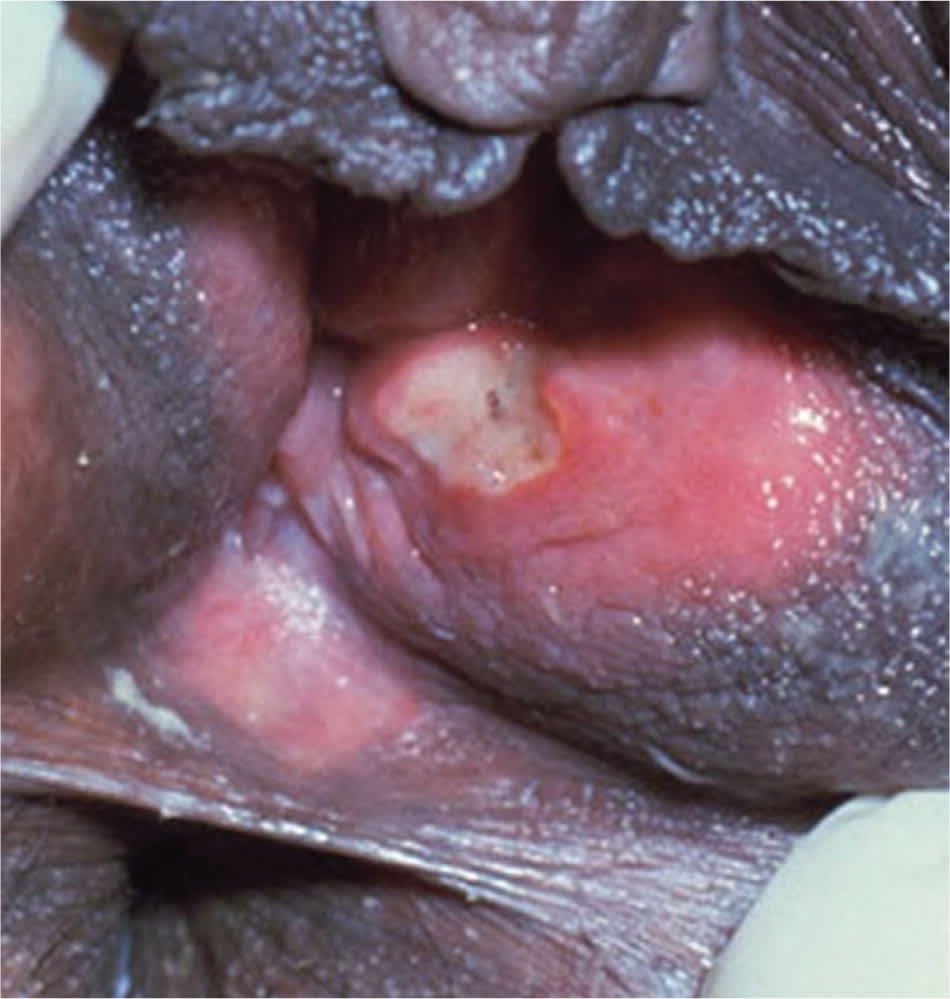
Chancroid ulcers are usually nonindurated with serpiginous borders and friable base, often covered with purulent exudate.
Photo courtesy of Connie Celum, Walter Stamm; Seattle STD/HIV Prevention Training Center, University of Washington.
Lymphogranuloma venereum infection is characterized by a small, shallow, painless genital or rectal papule that may ulcerate at the site of infection after an incubation period of three to 30 days. These ulcers may be self-limited and remain primarily undetected within the urethra, vagina, or rectum. However, if left untreated, the condition may be complicated by secondary bacterial infections or lymphatic obstruction, which may progress to genital elephantiasis.10 In persons who have receptive anal intercourse, lymphogranuloma venereum may result in tenesmus; constipation; rectal bleeding; pain or discharge; proctitis; anogenital ulcerations; and unilateral, tender inguinal or femoral lymphadenopathy.13,20,21
Granuloma inguinale, or donovanosis, is characterized by persistent, painless, beefy-red papules or ulcers, which may be hypertrophic, necrotic, or sclerotic with an incubation period of eight to 12 weeks (Figure 4).22 Patients with Behçet syndrome usually have intermittent arthritis, recurrent oral and genital ulcers, and possibly a family history of inflammatory disorders.23 Up to 60 percent of genital ulcers associated with Behçet syndrome lead to significant scarring.24
Figure 4.
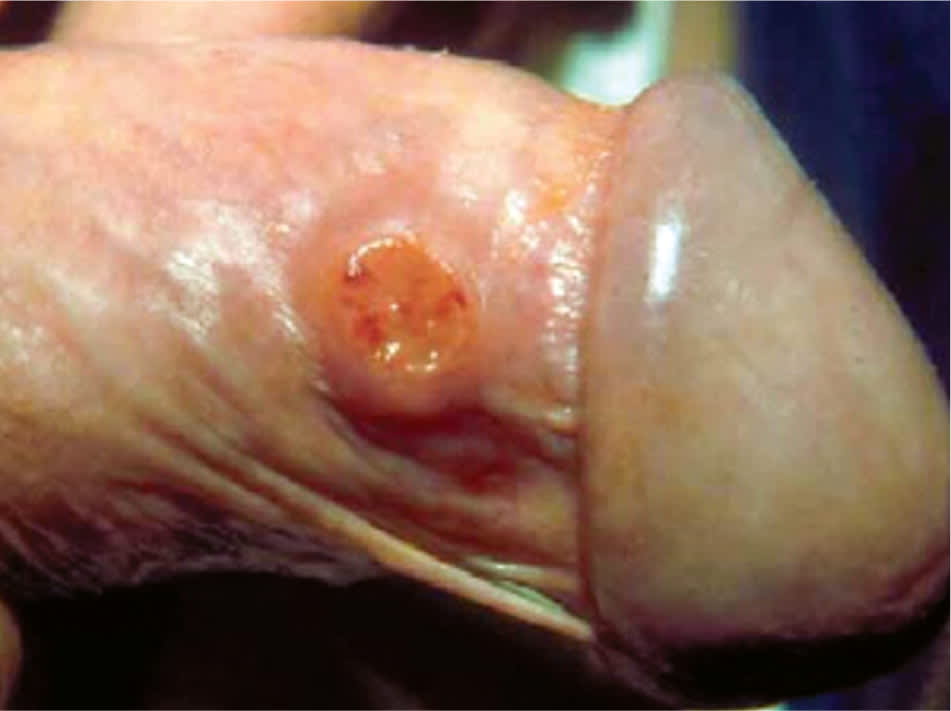
Genital ulcer with hypertrophic borders, caused by donovanosis.
Reprinted with permission from Velho PE, Souza EM, Belda Junior W. Donovanosis. Braz J Infect Dis . 2008;12(6):523.
LABORATORY EVALUATION
Laboratory evaluation of an initial genital ulcer outbreak should include culture or polymerase chain reaction testing for HSV infection, HSV type-specific serology, serologic testing for syphilis, and culture for H. ducreyi in settings with a high prevalence of chancroid. For the diagnosis of HSV infection, polymerase chain reaction testing is 96 to 100 percent sensitive and 97 to 98 percent specific (positive likelihood ratio = 49, negative likelihood ratio = 0.02), much more sensitive than culture.25,26 Among adults who report that they have never had genital herpes, the seroprevalence of HSV type 2 antibodies is 21.6 percent, suggesting the disease is underdiagnosed.27
Darkfield microscopy and direct fluorescent antibody tests of exudate or tissue material are the definitive methods for diagnosing primary syphilis.3,4,28 However, in patients presenting with genital ulcers, a presumptive diagnosis of syphilis can be made with a serologic nontreponemal test (i.e., Venereal Disease Research Laboratories or rapid plasma reagin). But, because of possible false-positive results, positive nontreponemal test results should be confirmed with serologic treponemal testing (i.e., fluorescent treponemal antibody absorption or T. pallidum passive agglutination).3,4,28 Nontreponemal titers typically decline and may become nonreactive after treatment, but most positive treponemal test results tend to remain persistently active. If primary syphilis is treated, up to 25 percent of patients may have nonreactive treponemal results in two to three years; however, treponemal titers are not recommended to evaluate response to treatment.3
Although a definitive diagnosis of chancroid requires identification of H. ducreyi, testing with special culture media is less than 80 percent sensitive and polymerase chain reaction testing for H. ducreyi is not available in the United States.4 A presumptive diagnosis is possible with a painful genital ulcer, regional lymphadenopathy, no evidence of T. pallidum infection, and negative HSV test results.3
To diagnose lymphogranuloma venereum, genital swabs or bubo aspirate may be tested for C. trachomatis serotypes L1, L2, and L3 by culture, direct immunofluorescence, or nucleic acid amplification.3 Nucleic acid amplification tests for lymphogranuloma venereum are not approved by the U.S. Food and Drug Administration for rectal specimens. Health care professionals may collect and send rectal specimens to state health departments for referral to the Centers for Disease Control and Prevention for testing and validating diagnostic methods for lymphogranuloma venereum.3
Even with appropriate laboratory testing, no pathogen is identified in up to 25 percent of patients with genital ulcers.4 Biopsy is rarely needed to diagnose the cause of genital ulcers, but it may be considered if an ulcer persists after treatment.3
Treatment
The 2010 Centers for Disease Control and Prevention guidelines for managing STIs provide treatment options for patients with genital ulcer disease.3 Treatment of HSV infection should be initiated before test results are available because early treatment decreases transmission and duration of ulcers. Patients should be instructed to abstain from sexual activity during the prodrome stage, while lesions are present, and for the duration of treatment. Treatments for common causes of genital ulcers are outlined in Table 3.1,3,5,12–16
The first episode of genital HSV infection may be treated with acyclovir (Zovirax), 400 mg orally three times daily for seven to 10 days (five days for recurrent episodes). Alternative therapies include famciclovir (Famvir) or valacyclovir (Valtrex).3,29 Topical antivirals are of limited benefit in the treatment of HSV infection and are not recommended.3
Primary syphilis may be treated with intramuscular penicillin G benzathine, 2.4 million units in a single dose. The Centers for Disease Control and Prevention guidelines recommend that patients allergic to penicillin undergo desensitization.3
Treatment options for chancroid include intramuscular ceftriaxone (Rocephin), 250 mg in a single dose, or oral azithromycin (Zithromax), ciprofloxacin (Cipro), or erythromycin. Treatment is less effective for uncircumcised males and patients coinfected with human immunodeficiency virus (HIV). Sex partners should be treated for chancroid, regardless of symptoms, if they have had sexual contact with the patient within the previous 10 days.3
Patients with lymphogranuloma venereum or donovanosis are treated with oral doxycycline, 100 mg twice daily for 21 days, and followed clinically. Donovanosis may require continued antibiotics until resolution of symptoms. Erythromycin is an alternative therapy for lymphogranuloma venereum.3
Treatment of mucocutaneous ulcers in Behçet syndrome is based on associated symptoms because ulcerations may regress spontaneously. In a randomized trial, subcutaneous pegylated interferon alfa-2a (Pegasys), 6 million units three times weekly for three months, improved duration and pain of oral ulcers and frequency of genital ulcers.14 A Cochrane review of randomized controlled trials found insufficient evidence for the use of oral acyclovir, oral colchicine, or topical interferon to treat ulcers caused by Behçet syndrome.30 In patients with Behçet syndrome, topical or vaginal sucralfate (not available in the United States) decreases the pain of oral ulcers, but does not significantly decrease the average frequency, healing time, or pain of genital ulcers.31
Treatment of extensive genital ulcers, regardless of etiology, has traditionally included wound cleansing and dressing. Although clinical trials are lacking, local treatment may include topical or oral analgesics, perineal baths, topical or oral anti-inflammatory agents, or cool compresses with Burow solution.15 Topical antimicrobials, such as benzoyl peroxide, dimethyl sulfoxide, gentamicin, oxyquinoline (not available in the United States), and silver sulfadiazine (Silvadene), may be beneficial for extragenital ulcers, but evidence of effectiveness is limited.16
Promptly treating genital ulcers is particularly important for patients with HIV to reduce HIV shedding and transmission. Genital ulcers increase HIV viral load in semen, increasing the likelihood of transmission to sex partners. Conversely, a patient with genital ulcers is more likely to acquire HIV infection with unprotected sexual contact.28,32,33
Prevention and Screening
The U.S. Preventive Services Task Force recommends screening for syphilis in persons at increased risk,34 and recommends against routinely screening for HSV in asymptomatic patients.35 There are no current screening recommendations for chancroid, lymphogranuloma venereum, or donovanosis.
Patients with genital ulcers should be counseled on reducing risk factors for STIs, including limiting the number of sex partners, using a condom with each sexual encounter, and regularly being screened for STIs if recommended by evidence-based guidelines. HIV testing should be performed in all patients with previously negative HIV test results who have genital ulcers caused by T. pallidum or H. ducreyi infection, and should be strongly considered for those who have genital ulcers caused by HSV infection.3
Avoiding sexual intercourse during outbreaks does not prevent HSV transmission.36 Although condom use can effectively prevent transmission, the infection can be spread through skin-to-skin contact in genital areas unprotected by a condom.37,38 The American College of Obstetricians and Gynecologists recommends that women who have partners with HSV infection be offered type-specific serologic testing to assess their risk, and these couples should be advised on condom and dental dam use, including a warning about incomplete protection.39
Chemoprophylaxis is available for severe or recurrent outbreaks of genital HSV infection in the form of daily suppressive medication. Suppressive therapy reduces the frequency and severity of outbreaks, reduces asymptomatic viral shedding by 90 percent, and reduces the risk of transmission to a seronegative partner.40 Options for suppressive therapy include acyclovir, 400 mg twice daily; famciclovir, 250 mg twice daily; or valacyclovir, 1,000 mg daily.29,41,42 If a patient has fewer than 10 outbreaks per year, 500 mg of oral valacyclovir daily is an appropriate option.3 Famciclovir is equally effective for suppression but less effective for the prevention of viral shedding and transmission to sex partners.43
The American College of Obstetricians and Gynecologists recommends that pregnant patients with HSV infection begin suppressive therapy at 34 to 36 weeks' gestation to reduce the likelihood of lesions during labor.44 Suppressive therapy reduces the risk of recurrence by 75 percent and the rate of cesarean delivery because of HSV lesions by 40 percent.45
Data Sources: A PubMed search was conducted for genital ulcer topics including clinical reviews, randomized controlled trials, and meta-analyses. Search terms were genital ulcer disease, ulcers, herpes, syphilis, chancroid, lymphogranuloma venereum, granuloma inguinale, Behçet, psoriasis, and sexually transmitted infections. Also reviewed were relevant publications from the Cochrane Database, Essential Evidence, National Guideline Clearinghouse, U.S. Preventive Services Task Force, Centers for Disease Control and Prevention, and Dynamed. Search date: August 2010.

