Am Fam Physician. 2012;85(3):271-272
Author disclosure: No relevant financial affiliations to disclose.
A 50-year-old woman presented to the emergency department with a diffuse rash that appeared four months earlier. The rash began on the upper extremities and gradually spread to her entire body. It was pruritic and associated with subjective fever and chills. Some of the lesions were pustular and crusting. She did not have a history of skin problems, and she had not been exposed to any new body creams, medications, detergents, or foods. The patient also noted a lump in her right breast at the same time the rash appeared. She had not seen a physician previously for the lump. She had a significant history of tobacco use and a family history of breast cancer in an aunt.
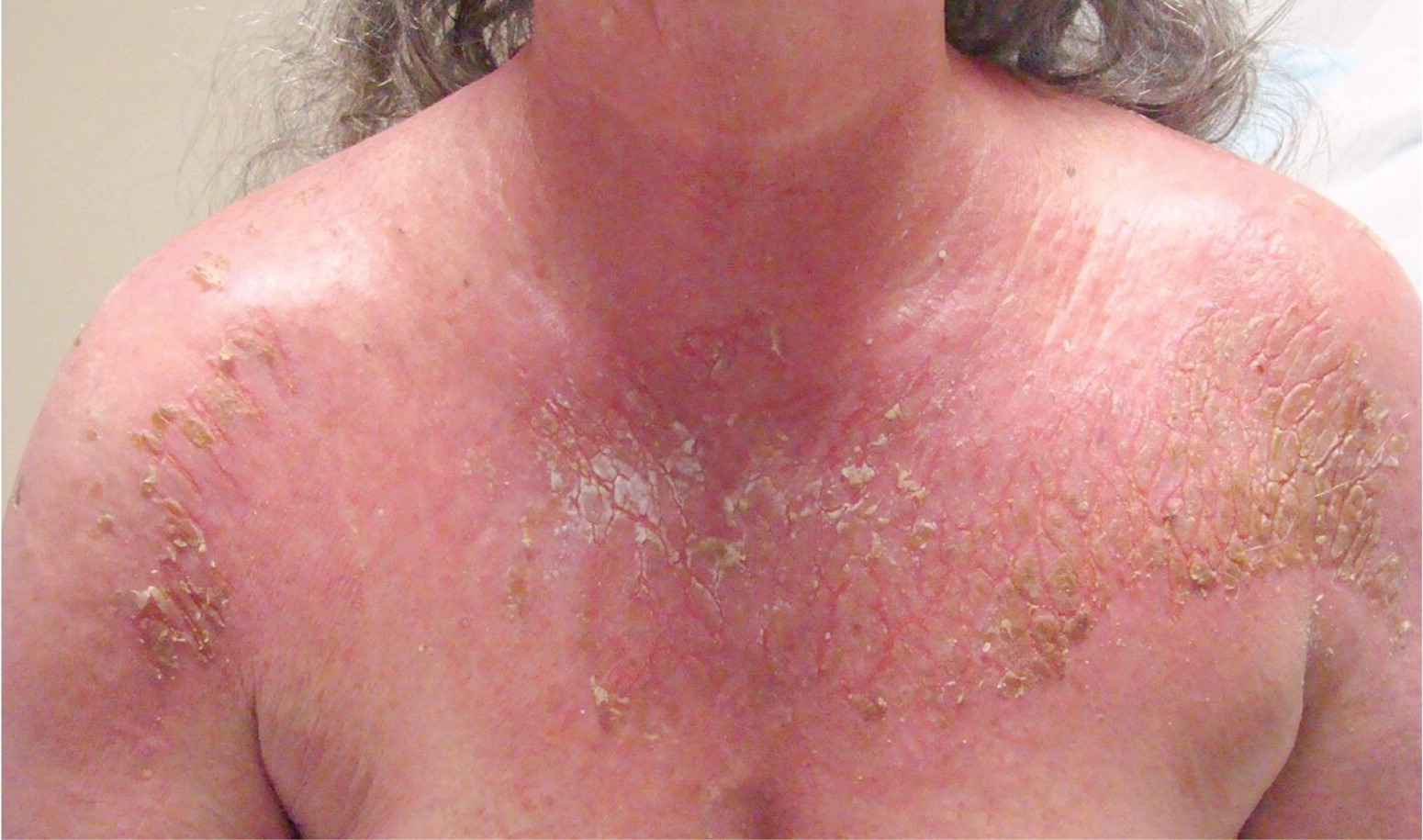
On examination, her blood pressure was 176/84 mm Hg, and her pulse was 113 beats per minute. The breast examination revealed a 3-cm, firm mass in the right outer quadrant that was fixed to underlying structures. There were peau d'orange changes surrounding the areola and a single palpable right axillary lymph node. She had generalized erythema and desquamation of the scalp, face, chest, back, and extremities with crusting and weeping of the skin surface (see accompanying figure). No lesions were noted on the palms or soles.
Question
Discussion
The answer is A: Erythroderma (exfoliative dermatitis). Exfoliative dermatitis is a diffuse erythema and scaling of the skin involving more than 90 percent of the total body skin surface. Common underlying etiologies include drug hypersensitivity reactions, psoriasis, atopic dermatitis, and malignancy. Drug hypersensitivity reactions account for approximately 15 percent of exfoliative dermatitis cases.1 The most commonly implicated drugs are calcium channel blockers, antiepileptics (phenytoin [Dilantin], carbamazepine [Tegretol], lamotrigine [Lamictal]), antibiotics (vancomycin, sulfonamides, penicillins), cimetidine (Tagamet), dapsone, and allopurinol (Zyloprim). Cutaneous T-cell lymphoma is the most common malignancy associated with exfoliative dermatitis.2 This patient had a more unusual presentation associated with a solid organ tumor (breast cancer).
Patients with exfoliative dermatitis initially present with pruritic, erythematous patches that progress to generalized erythema, possibly with fever and chills. Physical examination may reveal lymphadenopathy, pretibial edema, and alopecia. Laboratory findings are generally nonspecific.3 Because of the diffuse skin involvement, the condition may be complicated by fluid and electrolyte imbalances, hypothermia, staphylococcal infection, and high-output heart failure.
Treatment is supportive and includes wound care with emollients, and low-dose topical steroids plus oral antihistamines and antibiotics for superinfections. A dermatology consultation may be helpful if there is inadequate response to initial therapy. Second-line treatment includes oral corticosteroids and immunosuppressive agents, such as cyclophosphamide and methotrexate.
Pemphigus foliaceus is an autoimmune disorder characterized by acantholysis and superficial blistering.4 Autoantibodies against desmoglein 1 lead to the formation of blisters. Patients with typical pemphigus may present with scaly, crusted lesions on a red base without mucosal involvement. The lesions are confined to the face, scalp, and upper trunk. Initial treatment involves topical antibiotics and corticosteroids.
Staphylococcal scalded skin syndrome is a toxin-mediated form of exfoliative dermatitis that usually occurs in children.5 Patients present with fever, malaise, and skin tenderness. The condition begins as a burning, erythematous, sandpaper-like rash that is worse in flexor creases. The rash progresses to wrinkled, desquamative, bullous lesions.5 Treatment involves supportive care with antipyretics, intravenous fluids, and parenteral antibiotics.
Toxic epidermal necrolysis is a clinical syndrome related to Stevens-Johnson syndrome and involves greater than 30 percent epidermal skin detachment.6 Like erythroderma, toxic epidermal necrolysis is often related to medication use; 80 percent of cases occur one to three weeks after initiation of the medication.7 Medications associated with toxic epidermal necrolysis include allopurinol, anticonvulsants, nonsteroidal anti-inflammatory drugs, and sulfonamide antibiotics. Patients often present following an influenza-like illness with fever, sore throat, and myalgias. Skin examination reveals desquamative, atypical, purpuric, targetoid lesions that coalesce into dusky, poorly demarcated, confluent patches.7 Treatment involves immediate discontinuation of the offending medication, as well as supportive therapy and aggressive wound care.
| Condition | Characteristics |
|---|---|
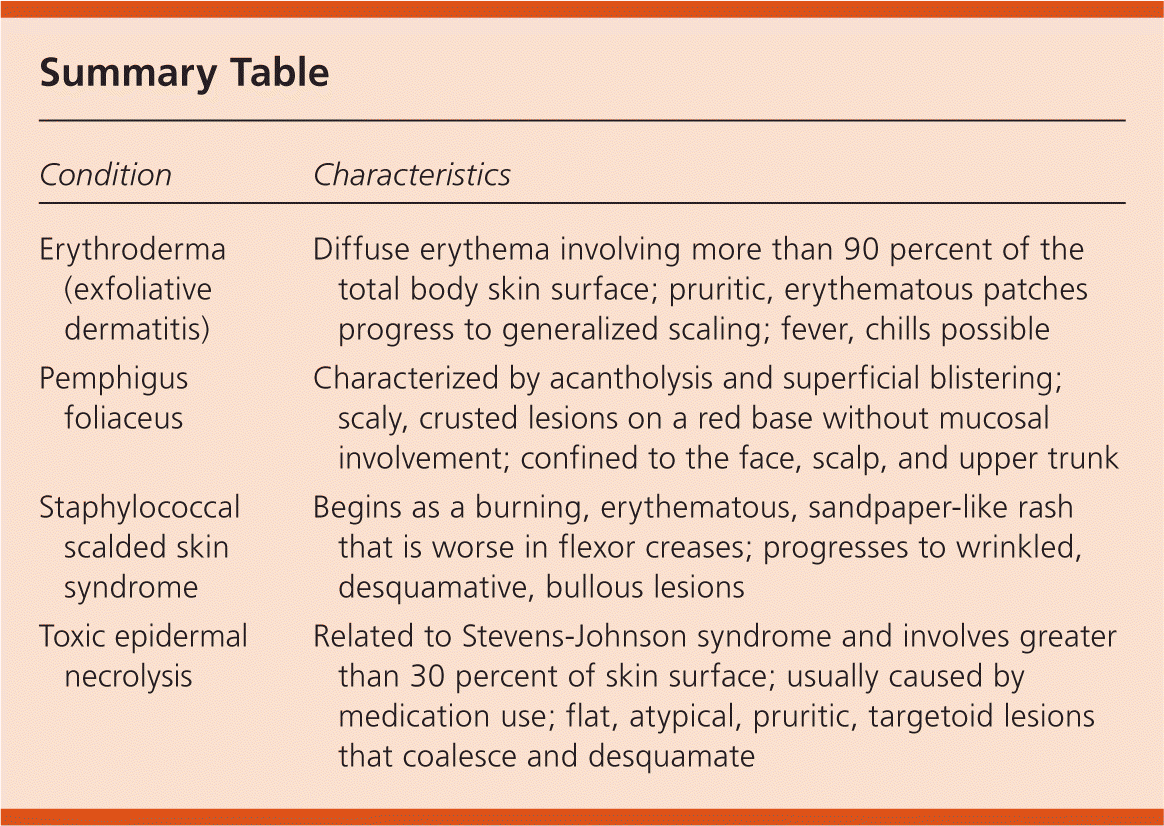
| Erythroderma (exfoliative dermatitis) | Diffuse erythema involving more than 90 percent of the total body skin surface; pruritic, erythematous patches progress to generalized scaling; fever, chills possible |
| Pemphigus foliaceus | Characterized by acantholysis and superficial blistering; scaly, crusted lesions on a red base without mucosal involvement; confined to the face, scalp, and upper trunk |
| Staphylococcal scalded skin syndrome | Begins as a burning, erythematous, sandpaper-like rash that is worse in flexor creases; progresses to wrinkled, desquamative, bullous lesions |
| Toxic epidermal necrolysis | Related to Stevens-Johnson syndrome and involves greater than 30 percent of skin surface; usually caused by medication use; flat, atypical, pruritic, targetoid lesions that coalesce and desquamate |