Acute low back pain is one of the most common reasons for adults to see a family physician. Although most patients recover quickly with minimal treatment, proper evaluation is imperative to identify rare cases of serious underlying pathology. Certain red flags should prompt aggressive treatment or referral to a spine specialist, whereas others are less concerning. Serious red flags include significant trauma related to age (i.e., injury related to a fall from a height or motor vehicle crash in a young patient, or from a minor fall or heavy lifting in a patient with osteoporosis or possible osteoporosis), major or progressive motor or sensory deficit, new-onset bowel or bladder incontinence or urinary retention, loss of anal sphincter tone, saddle anesthesia, history of cancer metastatic to bone, and suspected spinal infection. Without clinical signs of serious pathology, diagnostic imaging and laboratory testing often are not required. Although there are numerous treatments for nonspecific acute low back pain, most have little evidence of benefit. Patient education and medications such as nonsteroidal anti-inflammatory drugs, acetaminophen, and muscle relaxants are beneficial. Bed rest should be avoided if possible. Exercises directed by a physical therapist, such as the McKenzie method and spine stabilization exercises, may decrease recurrent pain and need for health care services. Spinal manipulation and chiropractic techniques are no more effective than established medical treatments, and adding them to established treatments does not improve outcomes. No substantial benefit has been shown with oral steroids, acupuncture, massage, traction, lumbar supports, or regular exercise programs.
Most persons will experience acute low back pain during their lifetime. The first episode usually occurs between 20 and 40 years of age. For many, acute low back pain is the first reason to seek medical care as an adult. Pain can be moderate to severe and debilitating, causing anxiety. Many cases are self-limited and resolve with little intervention. However, 31 percent of persons with low back pain will not fully recover within six months,1 although most will improve. Recurrent back pain occurs in 25 to 62 percent of patients within one to two years, with up to 33 percent having moderate pain and 15 percent having severe pain.2–4
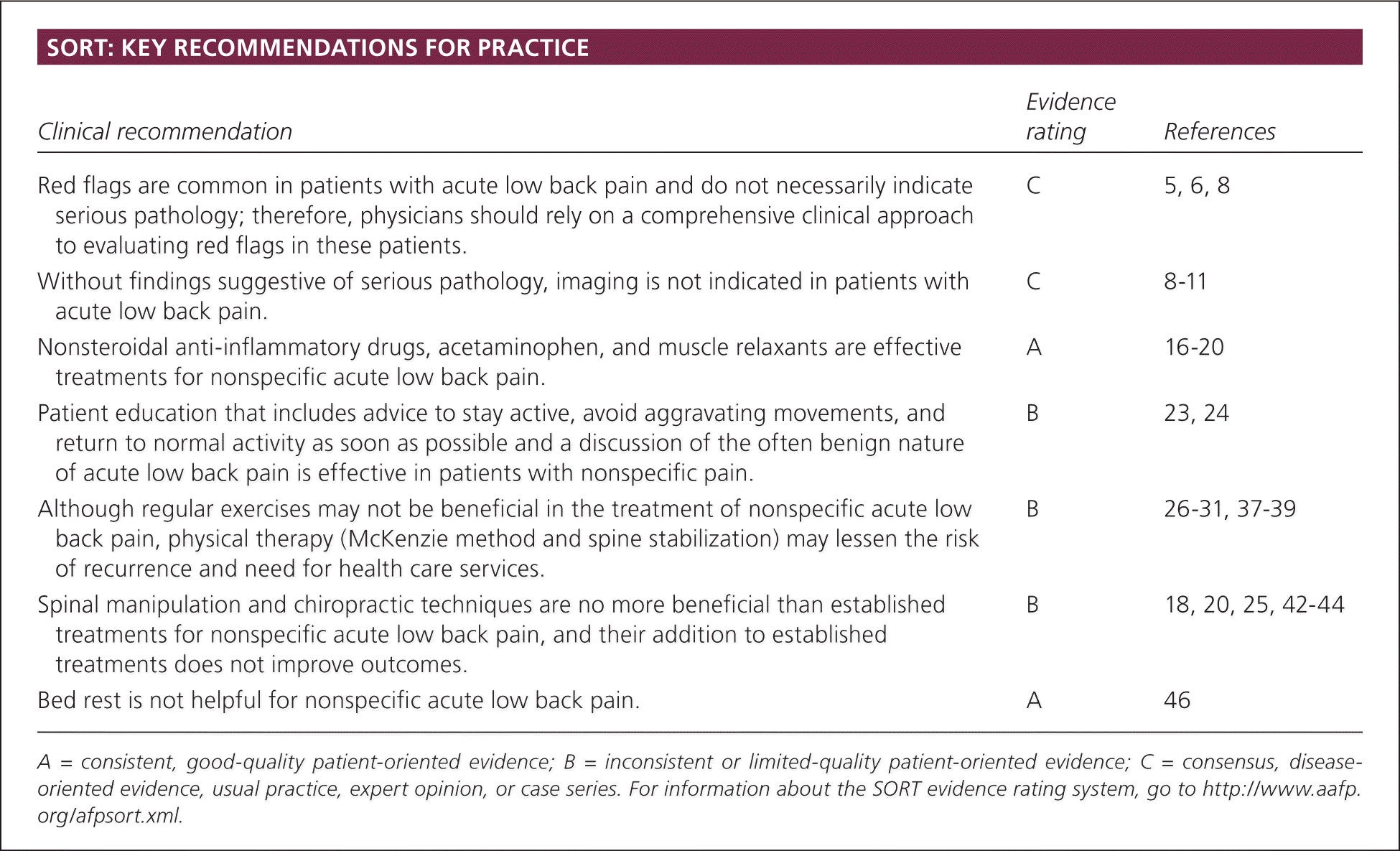
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Red flags are common in patients with acute low back pain and do not necessarily indicate serious pathology; therefore, physicians should rely on a comprehensive clinical approach to evaluating red flags in these patients. | C | 5, 6, 8 |
| Without findings suggestive of serious pathology, imaging is not indicated in patients with acute low back pain. | C | 8–11 |
| Nonsteroidal anti-inflammatory drugs, acetaminophen, and muscle relaxants are effective treatments for nonspecific acute low back pain. | A | 16–20 |
| Patient education that includes advice to stay active, avoid aggravating movements, and return to normal activity as soon as possible and a discussion of the often benign nature of acute low back pain is effective in patients with nonspecific pain. | B | 23, 24 |
| Although regular exercises may not be beneficial in the treatment of nonspecific acute low back pain, physical therapy (McKenzie method and spine stabilization) may lessen the risk of recurrence and need for health care services. | B | 26–31, 37–39 |
| Spinal manipulation and chiropractic techniques are no more beneficial than established treatments for nonspecific acute low back pain, and their addition to established treatments does not improve outcomes. | B | 18, 20, 25, 42–44 |
| Bed rest is not helpful for nonspecific acute low back pain. | A | 46 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
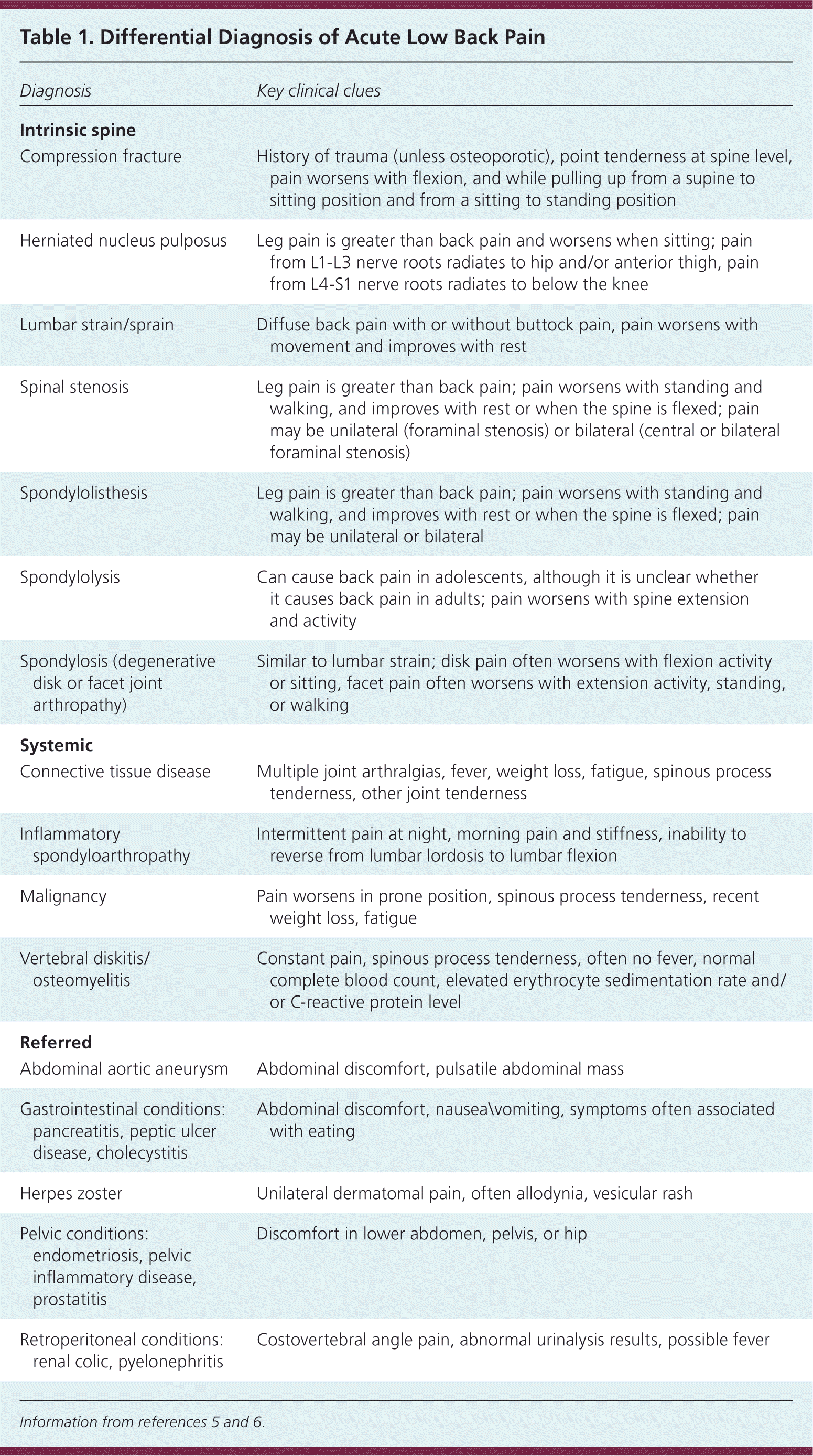
Acute low back pain can be defined as six to 12 weeks of pain between the costal angles and gluteal folds that may radiate down one or both legs (sciatica). Acute low back pain is often nonspecific and therefore cannot be attributed to a definite cause. However, possible causes of acute low back pain (e.g., infection, tumor, osteoporosis, fracture, inflammatory arthritis) need to be considered based on the patient's history and physical examination. Table 1 presents the differential diagnosis of acute low back pain.5,6
Table 1. Differential Diagnosis of Acute Low Back Pain
| Diagnosis | Key clinical clues |
|---|---|
| Intrinsic spine | |
| Compression fracture | History of trauma (unless osteoporotic), point tenderness at spine level, pain worsens with flexion, and while pulling up from a supine to sitting position and from a sitting to standing position |
| Herniated nucleus pulposus | Leg pain is greater than back pain and worsens when sitting; pain from L1-L3 nerve roots radiates to hip and/or anterior thigh, pain from L4-S1 nerve roots radiates to below the knee |
| Lumbar strain/sprain | Diffuse back pain with or without buttock pain, pain worsens with movement and improves with rest |
| Spinal stenosis | Leg pain is greater than back pain; pain worsens with standing and walking, and improves with rest or when the spine is flexed; pain may be unilateral (foraminal stenosis) or bilateral (central or bilateral foraminal stenosis) |
| Spondylolisthesis | Leg pain is greater than back pain; pain worsens with standing and walking, and improves with rest or when the spine is flexed; pain may be unilateral or bilateral |
| Spondylolysis | Can cause back pain in adolescents, although it is unclear whether it causes back pain in adults; pain worsens with spine extension and activity |
| Spondylosis (degenerative disk or facet joint arthropathy) | Similar to lumbar strain; disk pain often worsens with flexion activity or sitting, facet pain often worsens with extension activity, standing, or walking |
| Systemic | |
| Connective tissue disease | Multiple joint arthralgias, fever, weight loss, fatigue, spinous process tenderness, other joint tenderness |
| Inflammatory spondyloarthropathy | Intermittent pain at night, morning pain and stiffness, inability to reverse from lumbar lordosis to lumbar flexion |
| Malignancy | Pain worsens in prone position, spinous process tenderness, recent weight loss, fatigue |
| Vertebral diskitis/ osteomyelitis | Constant pain, spinous process tenderness, often no fever, normal complete blood count, elevated erythrocyte sedimentation rate and/ or C-reactive protein level |
| Referred | |
| Abdominal aortic aneurysm | Abdominal discomfort, pulsatile abdominal mass |
| Gastrointestinal conditions: pancreatitis, peptic ulcer disease, cholecystitis | Abdominal discomfort, nausea\vomiting, symptoms often associated with eating |
| Herpes zoster | Unilateral dermatomal pain, often allodynia, vesicular rash |
| Pelvic conditions: endometriosis, pelvic inflammatory disease, prostatitis | Discomfort in lower abdomen, pelvis, or hip |
| Retroperitoneal conditions: renal colic, pyelonephritis | Costovertebral angle pain, abnormal urinalysis results, possible fever |
The goals of treatment for acute low back pain are to relieve pain, improve function, reduce time away from work, and develop coping strategies through education. Optimizing treatment may minimize the development of chronic pain, which accounts for most of the health care costs related to low back pain.7
History and Physical Examination
An accurate history and physical examination are essential for evaluating acute low back pain. Often, patients awaken with morning pain or develop pain after minor forward bending, twisting, or lifting. It is also important to note whether it is a first episode or a recurrent episode. Recurrent episodes usually are more painful with increased symptoms. Red flags are often used to distinguish a common, benign episode from a more significant problem that requires urgent workup and treatment (Table 2).5,6,8 A recent study shows that some red flags are more important than others, and that red flags overall are poor at ruling in more serious causes of low back pain.8 Patients with back pain in the primary care setting (80 percent) tend to have one or more red flags, but rarely have a serious condition.8 However, physicians should be aware of the signs and symptoms of cauda equina syndrome, major intra-abdominal pathology, infections, malignancy, and fractures (Tables 15,6 and 25,6,8 ). Cauda equina syndrome and infections require immediate referral. Family physicians should rely on a comprehensive clinical approach rather than solely on a checklist of red flags.
Table 2. Red Flags for Serious Etiologies of Acute Low Back Pain

| Possible etiology | History findings | Physical examination findings |
|---|---|---|
| Cancer | Strong: Cancer metastatic to bone Intermediate: Unexplained weight loss | Weak: Vertebral tenderness, limited spine range of motion |
| Weak: Cancer, pain increased or unrelieved by rest | ||
| Cauda equina syndrome | Strong: Bladder or bowel incontinence, urinary retention, progressive motor or sensory loss | Strong: Major motor weakness or sensory deficit, loss of anal sphincter tone, saddle anesthesia |
| Weak: Limited spine range of motion | ||
| Fracture | Strong: Significant trauma related to age* | Weak: Vertebral tenderness, limited spine range of motion |
| Intermediate: Prolonged use of steroids | ||
| Weak: Age older than 70 years, history of osteoporosis | ||
| Infection | Strong: Severe pain and lumbar spine surgery within the past year | Strong: Fever, urinary tract infection, wound in spine region |
| Intermediate: Intravenous drug use, immunosuppression, severe pain and distant lumbar spine surgery | Weak: Vertebral tenderness, limited spine range of motion | |
| Weak: Pain increased or unrelieved by rest |
note: Presence of one or two weak or intermediate red flags may warrant observation because few patients will be significantly harmed if diagnosis of a serious cause is delayed for four to six weeks. Presence of any strong red flag warrants more urgent workup and probable referral to a spine subspecialist.
*—Fall from a height or motor vehicle crash in a young patient, minor fall or heavy lifting in a patient with osteoporosis or possible osteoporosis.
Pain from spine structures, such as musculature, ligaments, facet joints, and disks, can refer to the thigh region, but rarely to areas below the knee. Pain related to the sacroiliac joint often refers to the thigh, but can also radiate below the knee. Irritation, impingement, or compression of the lumbar root often results in more leg pain than back pain. Pain from the L1-L3 nerve roots will radiate to the hip and/or thigh, whereas pain from the L4-S1 nerve roots will radiate below the knee.
Neurologic examination of the lower extremities includes strength, sensation, and reflex testing (Table 3), even in the absence of significant sciatica. A straight leg raise test is positive for L4-S1 nerve root pain if it radiates below the knee. A reverse straight leg raise test (extending hip and flexing knee while in the prone position) is positive for L3 nerve root pain if it radiates into the anterior thigh. A central, paracentral, or lateral disk herniation may affect different nerve roots at the same level. Examination of the lumbosacral, pelvic, and abdominal regions may provide clues to underlying abnormalities relating to back pain (Table 15,6 and 25,6,8 ).
Table 3. Neurologic Examination Findings in Patients with Acute Low Back Pain

| Disk herniation | ||||||
|---|---|---|---|---|---|---|
| Affected nerve root | Motor deficit | Sensory deficit | Reflex | Central | Paracentral | Lateral |
| L3 | Hip flexion | Anterior/medial thigh | Patella | Above L2-L3 | L2-L3 | L3-L4 |
| L4 | Knee extension | Anterior leg/medial foot | Patella | Above L3-L4 | L3-L4 | L4-L5 |
| L5 | Dorsiflexion\great toe | Lateral leg/dorsal foot | Medial hamstring | Above L4-L5 | L4-L5 | L5-S1 |
| S1 | Plantar flexion | Posterior leg/lateral foot | Achilles tendon | Above L5-S1 | L5-S1 | None |
Diagnostic Workup
Imaging is not warranted for most patients with acute low back pain. Without signs and symptoms indicating a serious underlying condition, imaging does not improve clinical outcomes in these patients.9–11 Even with a few weaker red flags, four to six weeks of treatment is appropriate before consideration of imaging studies.8–10 If a serious condition is suspected, magnetic resonance imaging (MRI) is usually most appropriate. Computed tomography is an alternative if MRI is contraindicated or unavailable.10 Clinical correlation of MRI or computed tomography findings is essential because the likelihood of false-positive results increases with age.12–14 Radiography may be helpful to screen for serious conditions, but usually has little diagnostic value because of its low sensitivity and specificity.10
Laboratory tests such as complete blood count with differential, erythrocyte sedimentation rate, and C-reactive protein level may be beneficial if infection or bone marrow neoplasm is suspected. These tests may be most sensitive in cases of spinal infection because lack of fever and a normal complete blood count are common in patients with spinal infection.15 Because laboratory testing lacks specificity, MRI with and without contrast media and, in many cases, biopsy are essential for accurate diagnosis.15
Treatment of Nonspecific Pain
Many treatments are available for acute low back pain, but strong evidence for their benefit is lacking. Based on the evidence, a reasonable approach to treatment is described in Table 4.
Table 4. Approach to the Treatment of Nonspecific Acute Low Back Pain

| First visit | |
| Patient education | |
| Reassure the patient that the prognosis is often good, with most cases resolving with little intervention | |
| Advise the patient to stay active, avoiding bed rest as much as possible, and to return to normal activities as soon as possible | |
| Advise the patient to avoid twisting and bending | |
| Initiate trial of a nonsteroidal anti-inflammatory drug or acetaminophen | |
| Consider a muscle relaxant based on pain severity | |
| Consider a short course of opioid therapy if pain is severe | |
| Consider referral for physical therapy (McKenzie method and/or spine stabilization) if it is not the first episode | |
| Second visit* | |
| Consider changing to a different nonsteroidal anti-inflammatory drug | |
| Consider referral for physical therapy (McKenzie method and/or spine stabilization) if not done at initial visit | |
| Consider referral to a spine subspecialist if pain is severe or limits function | |
*—Two to four weeks after the initial visit, if the patient has not significantly improved.
RECOMMENDED
Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs) are often first-line therapy for low back pain. Low-quality evidence suggests that they are effective for short-term symptom relief, compared with placebo.16 No patient characteristics at baseline can predict the success of NSAID therapy.17 Moderate evidence suggests that no one NSAID is superior, and switching to a different NSAID may be considered if the first is ineffective. Whether NSAIDs are more effective than acetaminophen is unknown, but the addition of an NSAID to acetaminophen therapy is no more beneficial than acetaminophen alone.16,18
Moderate-quality evidence shows that non-benzodiazepine muscle relaxants (e.g., cyclobenzaprine [Flexeril], tizanidine [Zanaflex], metaxalone [Skelaxin]) are beneficial in the treatment of acute low back pain. Most pain reduction from these medications occurs in the first seven to 14 days, but the benefit may continue for up to four weeks.19,20 However, nonbenzodiazepine muscle relaxants do not affect disability status.19,20 Very low-quality evidence shows that a short course (up to five days) of oral diazepam (Valium) may also be beneficial for pain relief.19 Because all muscle relaxants have adverse effects, such as drowsiness, dizziness, and nausea, they should be used cautiously. Diazepam and carisoprodol (Soma) use should be brief to decrease the risk of abuse and dependence. There is also moderate-quality evidence that muscle relaxants combined with NSAIDs may have additive benefit for reducing pain.19
Opioids are commonly prescribed for patients with severe acute low back pain; however, there is little evidence of benefit. Three studies showed no difference in pain relief or time to return to work between oral opioids and NSAIDs or acetaminophen, and there is risk of harmful dose escalation over time with opioids, especially with purer formulations.16,21 Although epidural steroid injections are not beneficial for isolated acute low back pain, they may be helpful for radicular pain that does not respond to two to six weeks of noninvasive treatment. Transforaminal injections appear to have more favorable short- and long-term benefit than traditional interlaminar injections.22
Patient Education. Patient education involves a discussion of the often benign nature of acute back pain and reassurance that most patients need little intervention for significant improvement. Patients should be advised to stay as active as possible, within pain limits; to avoid twisting and bending, particularly when lifting; and to return to normal activities as soon as possible. The goal is to reduce worry about back pain and to teach ways to avoid worsening of pain or pain recurrence.
High-quality evidence shows that individual patient education of greater than two hours is more effective than no education or less-intense education for pain that persists for four weeks or more.23 Moderate-quality evidence shows that less-intense individual education and advice to stay active have small benefits and are at least as effective as other back pain interventions.23,24 It is unclear whether patient education and advice for patients with acute low back pain are cost-effective.25
ACCEPTABLE
Physical Therapy. Physical therapists often recommend the McKenzie method or spine stabilization exercises for the treatment of low back pain. The McKenzie method is described at http://www.mckenziemdt.org/approach.cfm, and a video demonstration is available at http://www.youtube.com/watch?v=wBOp-ugJbTQ. The McKenzie method has been shown to be slightly more effective than other common low back pain treatments; however, the difference is not clinically significant,26,27 and evidence on its effect on disability is conflicting.26,27 There also do not appear to be good long-term benefits with the McKenzie method, other than decreased need for health care services.27 Spine stabilization exercises have been shown to decrease pain, disability, and risk of recurrence after a first episode of back pain.28
According to moderate-quality evidence, physical therapist–directed home exercise programs for acute back pain can reduce the rate of recurrence, increase the time between episodes of back pain, and decrease the need for health care services. Therefore, most of these exercise programs are cost-effective treatments for acute low back pain.29–31
Application of Ice or Heat. Low-quality evidence shows that in the first five days of acute low back pain, the use of heat treatments may be more effective for reducing pain and disability than nonheat wraps, NSAIDs, or acetaminophen, but shows no difference between heat application and McKenzie therapy at seven days.32 A low-quality study found that heat therapy in conjunction with education or NSAIDs is more effective than education or NSAIDs alone at 14 days.33 Ice and heat therapy have similar analgesic effects.32
UNSUPPORTED
Oral Steroids. A short course of oral corticosteroids has questionable benefit for patients with acute radicular leg pain.34 However, there are no studies to support the use of oral steroids for isolated acute low back pain.
Acupuncture. Several low-quality trials show that acupuncture has minimal or no benefit over sham treatment, naproxen (Naprosyn), or the Chinese herbal therapy moxibustion.35,36 Although evidence to support its effectiveness is limited, acupuncture may be cost-effective in patients with pain lasting longer than four weeks.25
Exercise. Aerobic conditioning, strengthening exercises, flexibility exercises, or a combination of these exercises is no more effective than other treatments in patients with acute low back pain.37–39
Lumbar Support. It is unclear whether lumbar support is more effective than no intervention or other treatments for acute low back pain.40
Massage. There is insufficient evidence to recommend for or against massage therapy for acute low back pain.41,26 It is unlikely to be cost-effective.25
Spinal Manipulation and Chiropractic Techniques. Low-quality evidence shows that spinal manipulation may be more effective than sham treatments in the short-term reduction of pain (less than six weeks), but no more effective in reducing disability.18,20,42,43 There is little evidence that manipulation is cost-effective for treating acute low back pain.25
Although chiropractic techniques are considered safe if performed by a well-trained chiropractor, a systematic review found that these techniques (e.g., manipulation, temperature modalities, exercises, mechanical devices, patient education) provide no clinically relevant improvement in pain or disability compared with other treatments.44
Traction. High-quality trials show no evidence of benefit with traction, as a single treatment or in combination with other treatments, in patients with acute or chronic back pain.45 There are no studies on acute low back pain alone.
INADVISABLE
Bed Rest. Bed rest should not be recommended for patients with nonspecific acute low back pain. Moderate-quality evidence suggests that bed rest is less effective at reducing pain and improving function at three to 12 weeks than advice to stay active.46 Prolonged bed rest can also cause adverse effects such as joint stiffness, muscle wasting, loss of bone mineral density, pressure ulcers, and venous thromboembolism.37
Data Sources: We searched PubMed for the key term acute low back pain; this term was also searched with the following key terms: medications, nonsteroidals, muscle relaxants, opioids, red flags, differential diagnosis, exercise, McKenzie, spine stabilization, traction, acupuncture, heat, ice, advice, cost, manipulation, chiropractic care, brace, bed rest, massage. In addition, we searched the Cochrane Database of Systematic Reviews, Clinical Evidence, Essential Evidence Plus, and the National Guideline Clearinghouse. Search dates: April 2011 and May 2, 2011.
Editor's note: This review of acute low back pain presents evidence against the substantial benefit of spinal manipulation. Because there are differing viewpoints on this, we ran a series of pro/con editorials to address this question. They will link back to this article, and round out the discussion of this topic.

