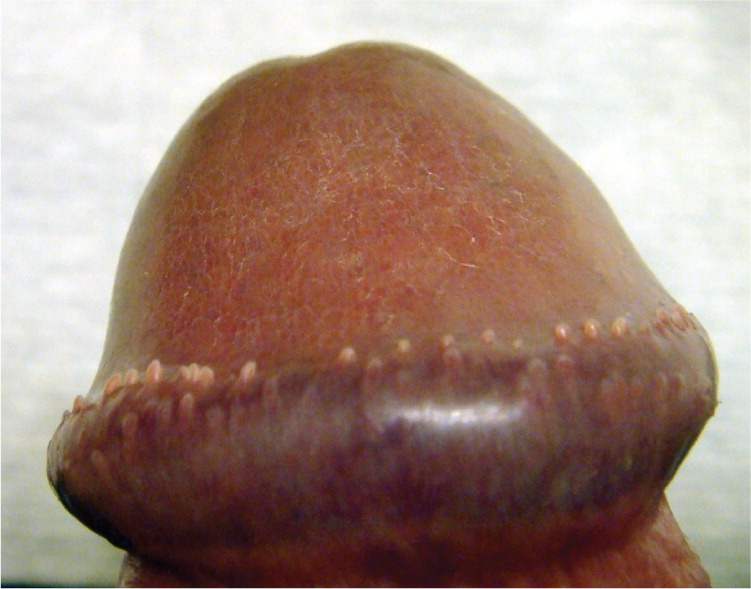
A 16-year-old boy presented to his family physician with concerns about bumps on the end of his penis that he had never seen before. He was not circumcised. He did not have penile discharge or burning, frequent urination, or a history of ulcers on his penis. He was sexually active with more than two partners. Examination revealed multiple 1- to 2-mm, flesh-colored papules on the head of his penis (see accompanying figure). No ulcers or inguinal lymphadenopathy was noted.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Genital warts.
B. Lichen nitidus.
C. Molluscum contagiosum.
D. Pearly penile papules.
E. Scabies.
Discussion
The answer is D: pearly penile papules. Pearly penile papules usually develop after puberty, but may occur in children.1,2 The papules are 1 to 4 mm, smooth, and asymptomatic. They commonly occur in a double row on the corona of the glans penis. The etiology is unknown, but does not appear to be related to the human papillomavirus.3 The papules have been found in many animals and may represent genetic residua from our animal ancestry.4
Reassurance is the primary treatment for pearly penile papules. Modalities such as silver nitrate and cryotherapy have had limited success. In extreme cases, removal with a carbon-dioxide laser may be effective.5
Genital warts commonly appear on the penile shaft and scrotum after sexual contact. They can be hyperkeratotic or soft, moist, pink or flesh-colored papules. They also may have a cauliflower appearance. There are many options for treatment, including cryotherapy, laser therapy, podophyllum, podofilox (Condylox), trichloroacetic acid, bichloracetic acid (not available in the United States), fluorouracil, interferon alfa-n3, and imiquimod (Aldara).
Lichen nitidus causes tiny, discrete, flesh-colored papules that are commonly located on the genitalia, trunk, and extremities.6 They usually begin in childhood or early adulthood, and the etiology is unknown. Biopsy shows a classic “claw clutching a ball” pattern. Lesions are self-limited and typically resolve spontaneously within one year. If they are associated with significant pruritus, topical steroids usually are the first-line treatment.
Molluscum contagiosum is caused by a poxvirus and presents as 1- to 5-mm, pearly, flesh-colored, dome-shaped papules. Penile lesions are uncommon, but can occur through self-inoculation or sexual transmission. Diagnosis usually can be made by examining material from the central plug under the microscope, using potassium hydroxide or Giemsa staining. Microscopy characteristically reveals a cup-shaped mass of homogeneous cells. Rarely, biopsy is needed to confirm the diagnosis. The lesions are self-limited, typically lasting six to nine months. Treatments are generally destructive, topical, and immunomodulatory.
Scabies is caused by Sarcoptes scabiei mites and usually presents as 1- to 3-mm, erythematous papules and vesicles. Papules are common on the shaft of the penis. Transmission is through direct, prolonged contact with an infected person. The mites cause burrows in the skin by secreting a protease that degrades the stratum corneum. Intense pruritus from delayed type IV hypersensitivity is characteristic. Microscopy of the scraping that identifies mites usually confirms the diagnosis. Permethrin cream is the standard treatment.
Summary Table
| Condition | Characteristics |
|---|---|
| Genital warts | Soft, moist, pink or flesh-colored papules; may have cauliflower appearance |
| Lichen nitidus | Tiny, discrete, flesh-colored papules; classic “claw clutching a ball” pattern on biopsy |
| Molluscum contagiosum | 1- to 5-mm, pearly, flesh-colored, dome-shaped papules; cup-shaped mass of homogeneous cells is a characteristic finding on microscopy |
| Pearly penile papules | 1- to 4-mm, smooth, asymptomatic papules; commonly occur in a double row on the corona of the glans penis |
| Scabies | Pruritic, 1- to 3-mm, erythematous papules and vesicles; microscopy usually confirms the presence of mites |

