Attention-deficit/hyperactivity disorder in childhood can persist into adulthood in at least 30 percent of patients, with 3 to 4 percent of adults meeting the Diagnostic and Statistical Manual of Mental Disorders, 4th ed., diagnostic criteria. A number of conditions, such as thyroid disease, mood disorders, and substance use disorders, have symptoms similar to those of attention-deficit/hyperactivity disorder and should be considered in the differential diagnosis. Steroids, antihistamines, anticonvulsants, caffeine, and nicotine also can have adverse effects that mimic attention-deficit/hyperactivity disorder symptoms. Proper diagnosis and treatment can improve daily functioning. Diagnosis relies on a thorough clinical history, supported by a number of rating scales that take five to 20 minutes to complete, depending on the scale. Clinical guidelines recommend stimulants and the nonstimulant atomoxetine as first-line treatments, followed by antidepressants. Cognitive behavior therapy has also been shown to be helpful as adjunctive treatment with medication. For adults with coexisting depression, the combination of an antidepressant and stimulants has been shown to be safe and effective. To monitor for misuse or diversion of stimulants, family physicians should consider using a controlled substances agreement and random urine drug screening in addition to regular follow-up visits.
Attention-deficit/hyperactivity disorder (ADHD) has long been recognized and treated in children. Over the past few decades, more attention has been placed on the persistence of ADHD into adulthood, with significant sequelae.1 It is now believed that ADHD can continue into adulthood in at least 30 percent of patients diagnosed with this disorder as a child.2
Current estimates indicate that approximately 3 to 4 percent of adults meet the Diagnostic and Statistical Manual of Mental Disorders, 4th ed. (DSM-IV), diagnostic criteria for ADHD, whereas approximately 16 percent of adults meet some of these criteria, but not enough for diagnosis.3,4 Of those who meet the diagnostic criteria, approximately two-fifths are categorized as having severe ADHD.5 Sixty-five to 85 percent of initial ADHD diagnoses in children and adolescents occur in the primary care setting6; therefore, it is reasonable to conclude that many adults will present to their primary care physician for evaluation of ADHD as well.
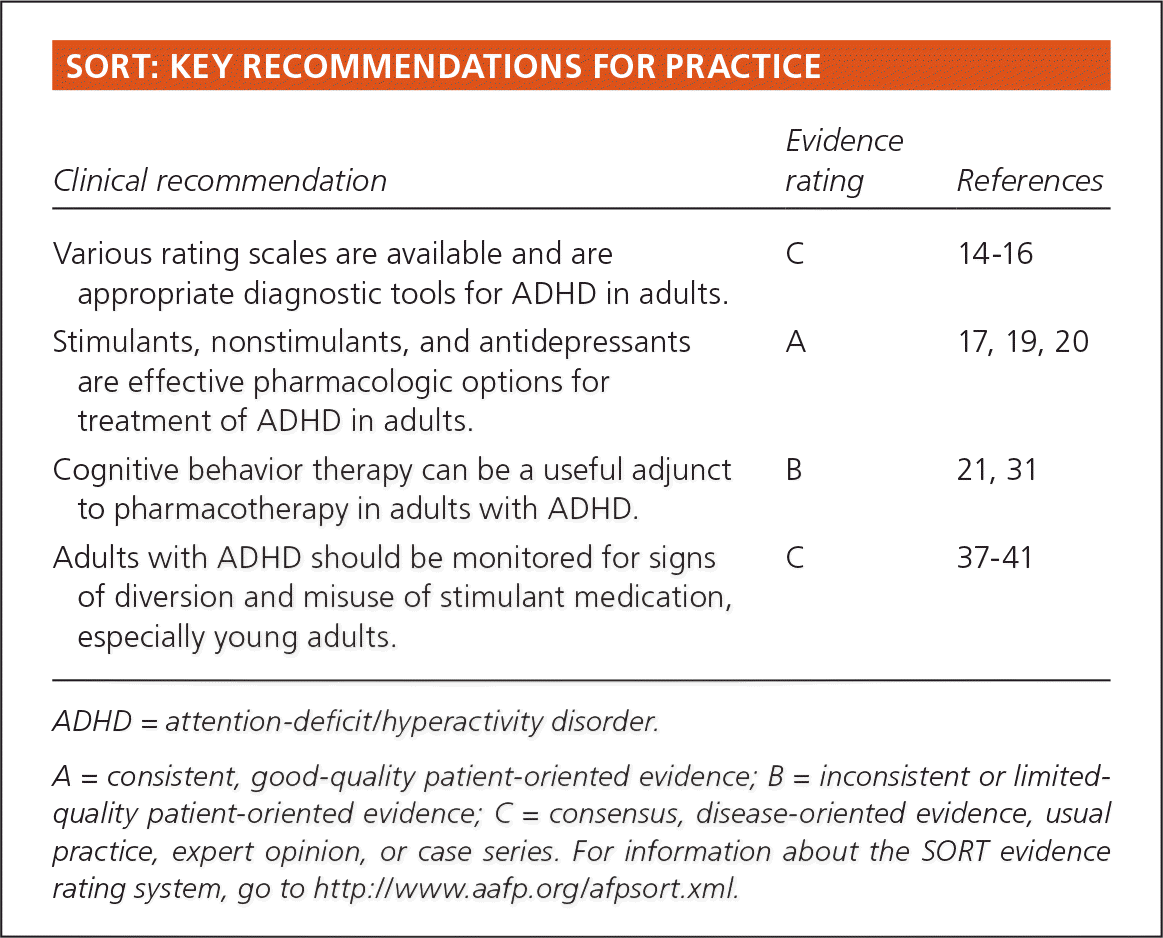
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Various rating scales are available and are appropriate diagnostic tools for ADHD in adults. | C | 14–16 |
| Stimulants, nonstimulants, and antidepressants are effective pharmacologic options for treatment of ADHD in adults. | A | 17, 19, 20 |
| Cognitive behavior therapy can be a useful adjunct to pharmacotherapy in adults with ADHD. | B | 21, 31 |
| Adults with ADHD should be monitored for signs of diversion and misuse of stimulant medication, especially young adults. | C | 37–41 |
ADHD = attention-deficit/hyperactivity disorder.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Differential Diagnosis
A number of conditions have symptoms similar to those of ADHD and should be considered in the differential diagnosis. Medical conditions include hearing impairment, thyroid disease, lead toxicity, hepatic disease, sleep apnea, and drug interactions.7,8 Psychiatric conditions include anxiety, mood, obsessive-compulsive, substance use, antisocial personality, borderline personality, and learning disorders, and intellectual disability.7,8 Certain substances, such as steroids, antihistamines, anticonvulsants, caffeine, and nicotine, may have adverse effects that impact attentiveness.7 Patients with major depressive, anxiety, or bipolar disorder, or any of the previously mentioned personality disorders may show signs of inattention or hyperactivity, but many other cardinal signs of those disorders are also usually present. Adults with ADHD may present with these psychiatric conditions as comorbidities8; therefore, timing of the onset of symptoms is essential in making an accurate diagnosis. For example, inattentiveness that begins after a depressive episode is not likely to be caused by ADHD; however, depression that begins after significant inattentiveness likely represents comorbid depression and ADHD.
Diagnosis
Diagnosis is based primarily on a detailed patient history and an assessment of current behavior and level of functioning. DSM-IV criteria (Table 19 ) for ADHD in adults are the same as for children. Although the criteria stipulate that symptoms must be present before seven years of age, many adults do not recall early symptoms. Furthermore, it has been shown that if no diagnosis of ADHD was made in childhood, primary care physicians do not even consider making a diagnosis of ADHD in adults.10
Table 1. DSM-IV Diagnostic Criteria for Attention-Deficit/Hyperactivity Disorder

| A. Either 1 or 2: | ||
| 1. Six (or more) of the following symptoms of inattention have persisted for at least six months to a degree that is maladaptive and inconsistent with developmental level: | ||
| Inattention | ||
| a. Often fails to give close attention to details or makes careless mistakes in schoolwork, work, or other activities | ||
| b. Often has difficulty sustaining attention in tasks or play activities | ||
| c. Often does not seem to listen when spoken to directly | ||
| d. Often does not follow through on instructions and fails to finish schoolwork, chores, or duties in the workplace (not due to oppositional behavior or failure to understand instructions) | ||
| e. Often has difficulty organizing tasks and activities | ||
| f. Often avoids, dislikes, or is reluctant to engage in tasks that require sustained mental effort (such as schoolwork or homework) | ||
| g. Often loses things necessary for tasks or activities (e.g., toys, school assignments, pencils, books, or tools) | ||
| h. Is often easily distracted by extraneous stimuli | ||
| i. Is often forgetful in daily activities | ||
| 2. Six (or more) of the following symptoms of hyperactivity-impulsivity have persisted for at least six months to a degree that is maladaptive and inconsistent with developmental level: | ||
| Hyperactivity | ||
| a. Often fidgets with hands or feet or squirms in seat | ||
| b. Often leaves seat in classroom or in other situations in which remaining seated is expected | ||
| c. Often runs about or climbs excessively in situations in which it is inappropriate (in adolescents or adults, may be limited to subjective feelings of restlessness) | ||
| d. Often has difficulty playing or engaging in leisure activities quietly | ||
| e. Is often “on the go” or often acts as if “driven by a motor” | ||
| f. Often talks excessively | ||
| Impulsivity | ||
| g. Often blurts out answers before questions have been completed | ||
| h. Often has difficulty awaiting turn | ||
| i. Often interrupts or intrudes on others (e.g., butts into conversations or games) | ||
| B. Some hyperactive-impulsive or inattentive symptoms that caused impairment were present before age seven years. | ||
| C. Some impairment from the symptoms is present in two or more settings (e.g., at school [or work] and at home). | ||
| D. There must be clear evidence of clinically significant impairment in social, academic, or occupational functioning. | ||
| E. The symptoms do not occur exclusively during the course of a pervasive developmental disorder, schizophrenia, or other psychotic disorder and are not better accounted for by another mental disorder (e.g., mood disorder, anxiety disorder, dissociative disorder, or a personality disorder). | ||
DSM-IV = Diagnostic and Statistical Manual of Mental Disorders, 4th ed.
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. Washington, DC: American Psychiatric Association; 1994:83–84.
There have been many criticisms of the DSM-IV criteria, mainly regarding the low age cutoff for diagnosis and the fact that adult manifestation of the disorder is different from childhood presentation.11 In anticipation of DSM-V, the American Psychiatric Association has listed a number of proposed changes to the current DSM-IV. These include increasing the age at which impairment must first have been observed from before seven years of age to before 12 years of age, and suggesting that for inattention and hyperactivity/impulsivity symptoms, those 17 years and older need only meet four criteria instead of six.12
The clinical diagnosis of ADHD in adults should take a stepwise approach, including13:
- Evaluating current (in the past six months) ADHD symptoms using rating scales with adult norms (Table 214–16 ).
- Establishing a childhood history (before seven years of age) of ADHD (this is one of the DSM-IV criteria for diagnosis [Table 19 ]). It may be helpful to try to obtain school records or report cards, and to speak with the patient's parents or other family members who interacted with the patient when he or she was a child.14 Using corroborating information can be useful in helping to determine whether the patient is malingering or attempting to obtain psychostimulant medication for illicit use or sale.
- Evaluating functional impairment at home, work, and school, and in relationships.
- Obtaining a developmental history, which helps establish symptoms that occurred in childhood.
- Obtaining a psychiatric history to rule out other psychiatric disorders or to establish the presence of comorbid disorders, including substance abuse, depression, and anxiety.
- Obtaining a family history for ADHD, tics, drug use, and criminal behavior.
- Performing a physical examination to eliminate medical causes. The examination should focus on thyroid and neurologic examination to rule out thyroid abnormalities and neurologic disorders (e.g., head injury, seizure disorder), and on possible contraindications of stimulant therapy (e.g., hypertension). Baseline weight should be recorded for comparison in future monitoring.
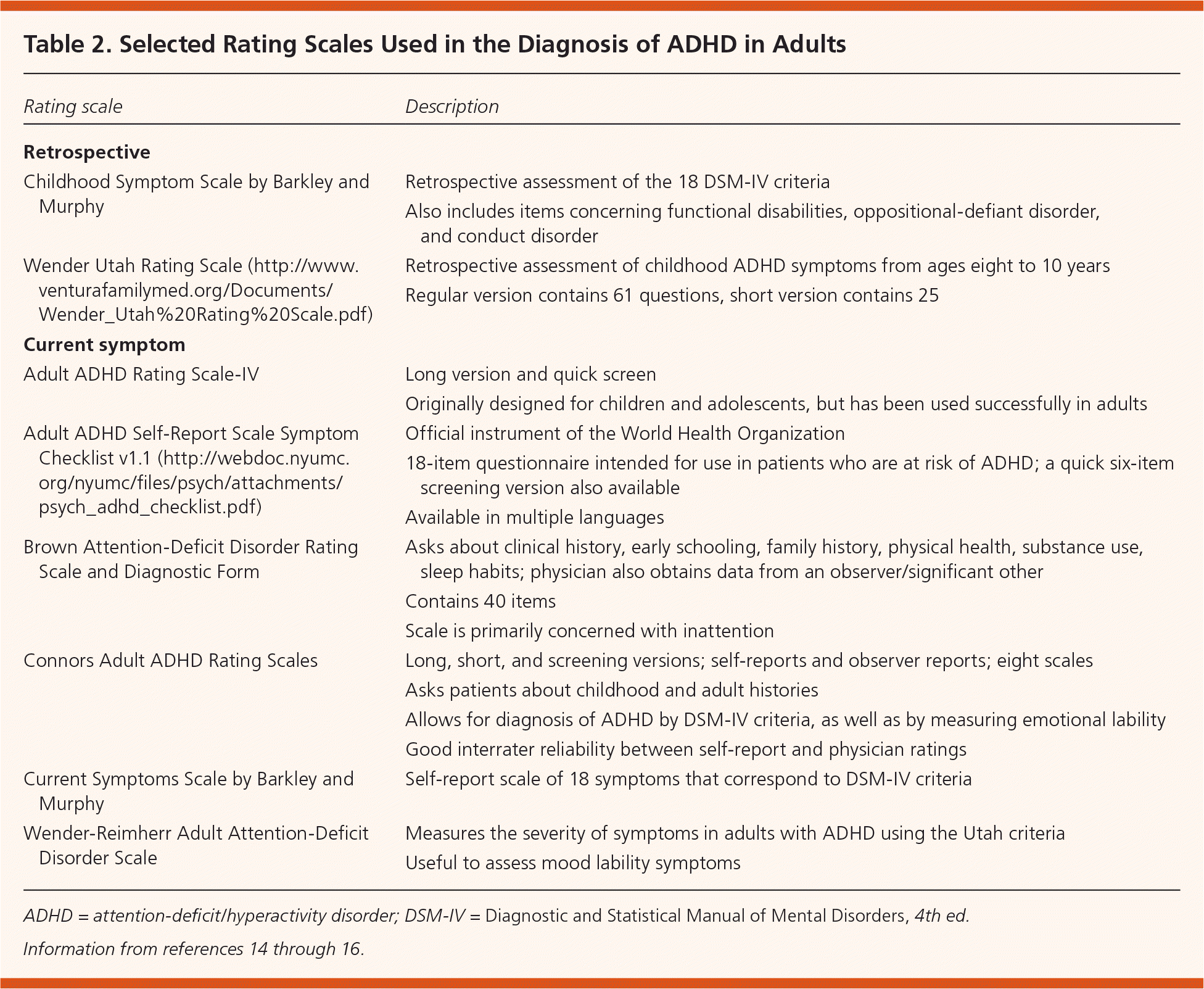
Table 2. Selected Rating Scales Used in the Diagnosis of ADHD in Adults
| Rating scale | Description |
|---|---|
| Retrospective | |
| Childhood Symptom Scale by Barkley and Murphy | Retrospective assessment of the 18 DSM-IV criteria |
| Also includes items concerning functional disabilities, oppositional-defiant disorder, and conduct disorder | |
| Wender Utah Rating Scale (http://www.venturafamilymed.org/Documents/Wender_Utah%20Rating%20Scale.pdf) | Retrospective assessment of childhood ADHD symptoms from ages eight to 10 years |
| Regular version contains 61 questions, short version contains 25 | |
| Current symptom | |
| Adult ADHD Rating Scale-IV | Long version and quick screen |
| Originally designed for children and adolescents, but has been used successfully in adults | |
| Adult ADHD Self-Report Scale Symptom Checklist v1.1 (http://webdoc.nyumc.org/nyumc/files/psych/attachments/psych_adhd_checklist.pdf) | Official instrument of the World Health Organization |
| 18-item questionnaire intended for use in patients who are at risk of ADHD; a quick six-item screening version also available | |
| Available in multiple languages | |
| Brown Attention-Deficit Disorder Rating Scale and Diagnostic Form | Asks about clinical history, early schooling, family history, physical health, substance use, sleep habits; physician also obtains data from an observer/significant other |
| Contains 40 items | |
| Scale is primarily concerned with inattention | |
| Connors Adult ADHD Rating Scales | Long, short, and screening versions; self-reports and observer reports; eight scales |
| Asks patients about childhood and adult histories | |
| Allows for diagnosis of ADHD by DSM-IV criteria, as well as by measuring emotional lability | |
| Good interrater reliability between self-report and physician ratings | |
| Current Symptoms Scale by Barkley and Murphy | Self-report scale of 18 symptoms that correspond to DSM-IV criteria |
| Wender-Reimherr Adult Attention-Deficit Disorder Scale | Measures the severity of symptoms in adults with ADHD using the Utah criteria |
| Useful to assess mood lability symptoms | |
ADHD = attention-deficit/hyperactivity disorder; DSM-IV = Diagnostic and Statistical Manual of Mental Disorders, 4th ed.
A number of structured diagnostic instruments/rating scales are available to help diagnose ADHD in adults (Table 2).14–16 These scales are useful because they provide structure in the diagnostic process and can help aid those who are less experienced with adult ADHD.14 In general, the instruments assess the diagnostic criteria for ADHD consistent with DSM-IV and take five to 20 minutes to complete, depending on the scale.15 However, there are scant data regarding the sensitivity and specificity of these scales.
There are no specific laboratory or ancillary tests for confirmation of diagnosis, but some tests, such as thyroid studies, liver function tests, and lead levels, may be helpful for ruling out comorbid or mimicking conditions.7
Treatment
PHARMACOTHERAPY
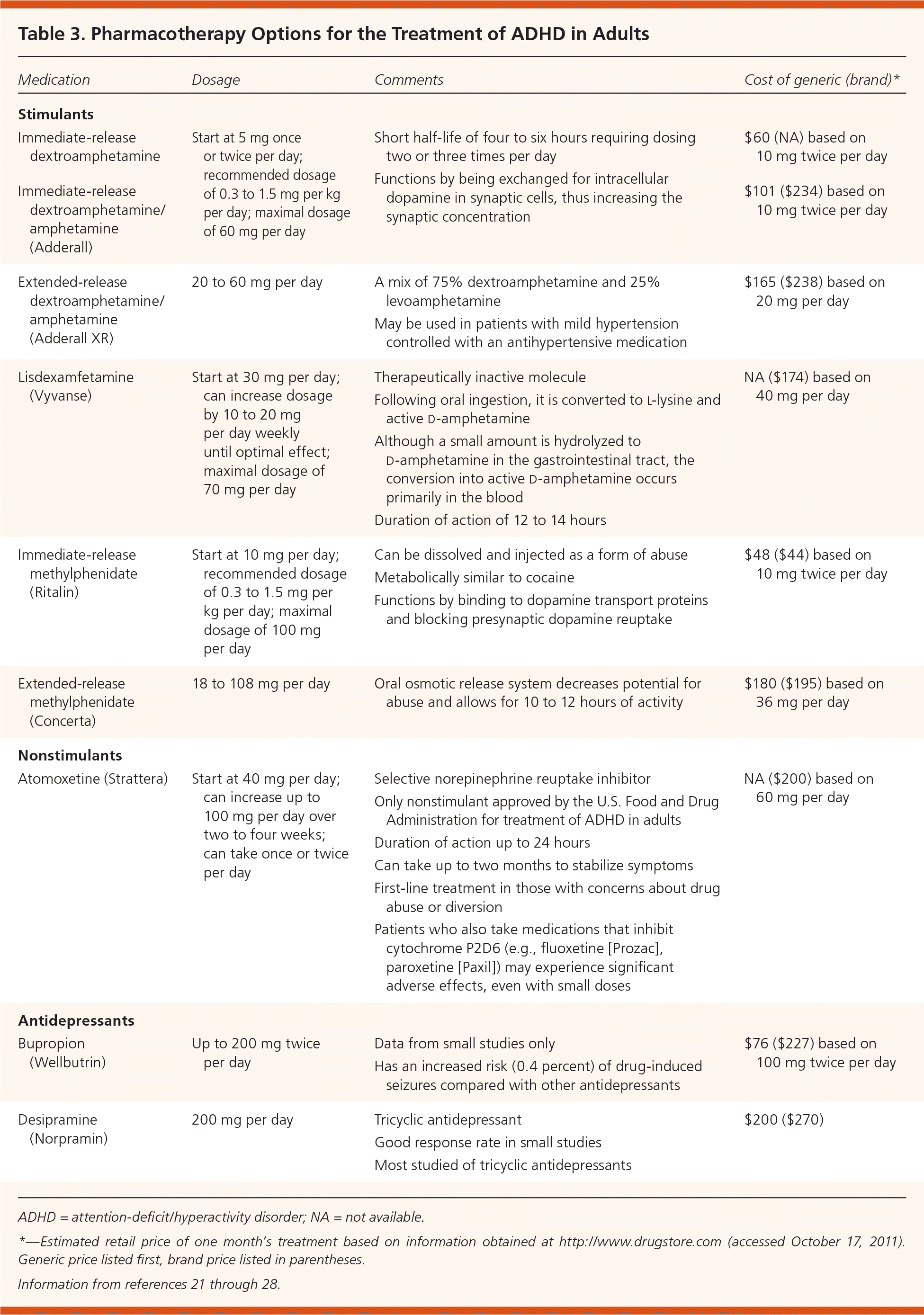
The mainstay of ADHD treatment is pharmacotherapy. Most studies focus on medications in children, yet these medications have been shown to be safe and effective in adults as well.17,18 Stimulants and antidepressants (e.g., bupropion [Wellbutrin], desipramine [Norpramin]) have similar effectiveness, although no direct comparison trials have been conducted.19 In a recent meta-analysis, stimulant and nonstimulant medications showed clinically significant improvements compared with placebo.20 Clinical guidelines recommend stimulants and atomoxetine (Strattera) as first-line treatments, followed by antidepressants.20 These medications are reviewed in Table 3.21–28
Table 3. Pharmacotherapy Options for the Treatment of ADHD in Adults
| Medication | Dosage | Comments | Cost of generic (brand)* |
|---|---|---|---|
| Stimulants | |||
| Immediate-release dextroamphetamine | Start at 5 mg once or twice per day; recommended dosage of 0.3 to 1.5 mg per kg per day; maximal dosage of 60 mg per day | Short half-life of four to six hours requiring dosing two or three times per day Functions by being exchanged for intracellular dopamine in synaptic cells, thus increasing the synaptic concentration | $60 (NA) based on 10 mg twice per day |
| Immediate-release dextroamphetamine/amphetamine (Adderall) | $101 ($234) based on 10 mg twice per day | ||
| Extended-release dextroamphetamine/amphetamine (Adderall XR) | 20 to 60 mg per day | A mix of 75% dextroamphetamine and 25% levoamphetamine | $165 ($238) based on 20 mg per day |
| May be used in patients with mild hypertension controlled with an antihypertensive medication | |||
| Lisdexamfetamine (Vyvanse) | Start at 30 mg per day; can increase dosage by 10 to 20 mg per day weekly until optimal effect; maximal dosage of 70 mg per day | Therapeutically inactive molecule | NA ($174) based on 40 mg per day |
| Following oral ingestion, it is converted to | |||
| Although a small amount is hydrolyzed to | |||
| Duration of action of 12 to 14 hours | |||
| Immediate-release methylphenidate (Ritalin) | Start at 10 mg per day; recommended dosage of 0.3 to 1.5 mg per kg per day; maximal dosage of 100 mg per day | Can be dissolved and injected as a form of abuse | $48 ($44) based on 10 mg twice per day |
| Metabolically similar to cocaine | |||
| Functions by binding to dopamine transport proteins and blocking presynaptic dopamine reuptake | |||
| Extended-release methylphenidate (Concerta) | 18 to 108 mg per day | Oral osmotic release system decreases potential for abuse and allows for 10 to 12 hours of activity | $180 ($195) based on 36 mg per day |
| Nonstimulants | |||
| Atomoxetine (Strattera) | Start at 40 mg per day; can increase up to 100 mg per day over two to four weeks; can take once or twice per day | Selective norepinephrine reuptake inhibitor | NA ($200) based on 60 mg per day |
| Only nonstimulant approved by the U.S. Food and Drug Administration for treatment of ADHD in adults | |||
| Duration of action up to 24 hours | |||
| Can take up to two months to stabilize symptoms | |||
| First-line treatment in those with concerns about drug abuse or diversion | |||
| Patients who also take medications that inhibit cytochrome P2D6 (e.g., fluoxetine [Prozac], paroxetine [Paxil]) may experience significant adverse effects, even with small doses | |||
| Antidepressants | |||
| Bupropion (Wellbutrin) | Up to 200 mg twice per day | Data from small studies only | $76 ($227) based on 100 mg twice per day |
| Has an increased risk (0.4 percent) of drug-induced seizures compared with other antidepressants | |||
| Desipramine (Norpramin) | 200 mg per day | Tricyclic antidepressant | $200 ($270) |
| Good response rate in small studies | |||
| Most studied of tricyclic antidepressants | |||
ADHD = attention-deficit/hyperactivity disorder; NA = not available.
*—Estimated retail price of one month's treatment based on information obtained at http://www.drugstore.com (accessed October 17, 2011). Generic price listed first, brand price listed in parentheses.
Medications should be started at a low dose and titrated slowly until maximal benefit is achieved or adverse effects become intolerable. A trial of four to six weeks should be allowed for each dosing change.22 Long-acting stimulants are preferred, because 70 percent of patients reported satisfaction with these versus 40 to 50 percent with immediate-release medications.23
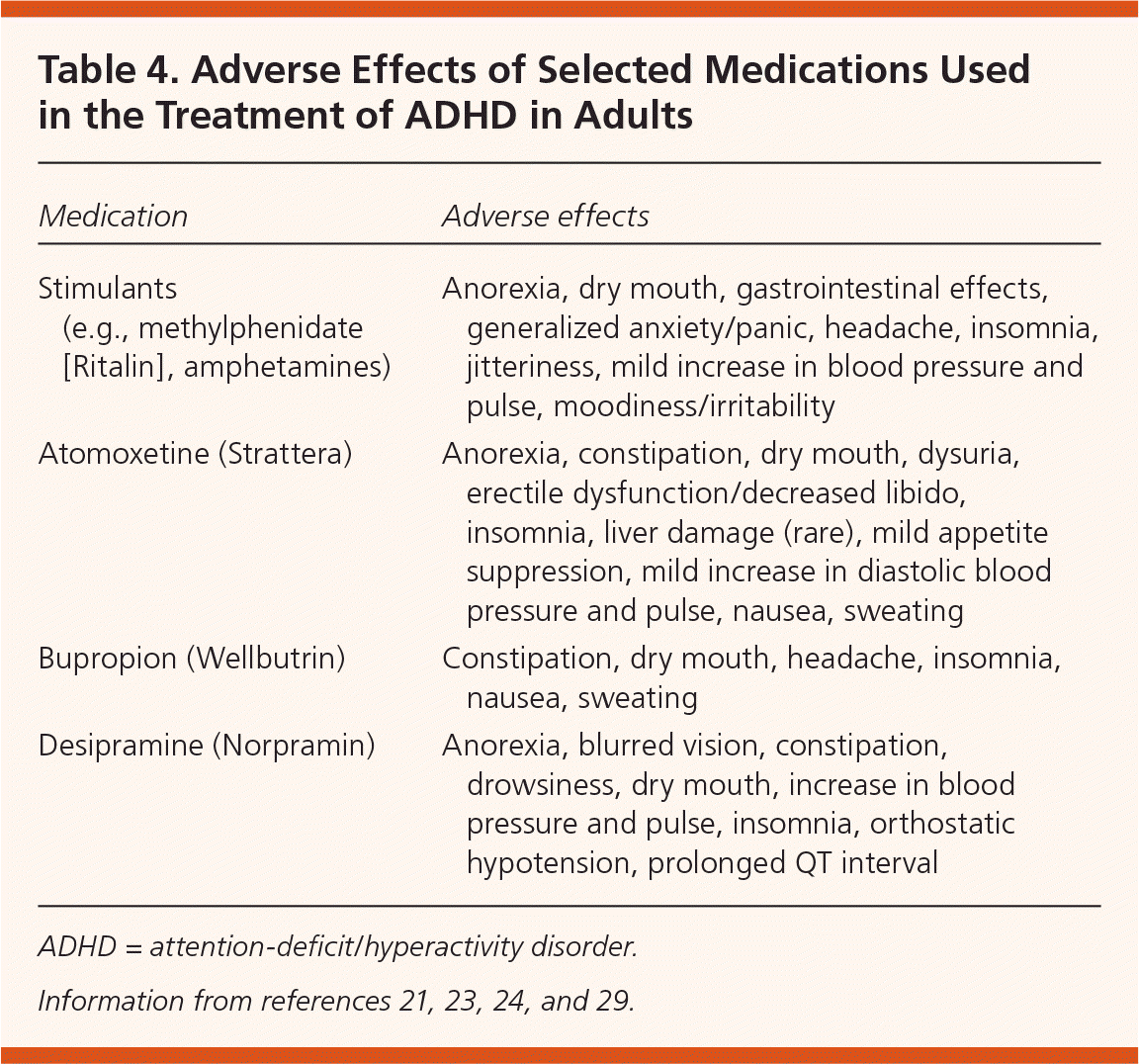
Up to 30 percent of patients discontinue stimulants because of uncontrolled symptoms or intolerance of adverse effects24 (Table 421,23,24,29 ). Contraindications for stimulant use include hypertension, tachycardia, arrhythmia, psychosis, bipolar disorder, severe anorexia, and Tourette syndrome.23 Also, a U.S. Food and Drug Administration review reported incidents of sudden death in patients with underlying serious heart problems who were taking standard stimulant doses.25 However, a recent study of more than 150,000 U.S. adults found that current or new use of stimulant medications for ADHD did not increase the risk of serious cardiovascular events, including myocardial infarction, sudden cardiac death, or stroke.30
Table 4. Adverse Effects of Selected Medications Used in the Treatment of ADHD in Adults
| Medication | Adverse effects |
|---|---|
| Stimulants (e.g., methylphenidate [Ritalin], amphetamines) | Anorexia, dry mouth, gastrointestinal effects, generalized anxiety/panic, headache, insomnia, jitteriness, mild increase in blood pressure and pulse, moodiness/irritability |
| Atomoxetine (Strattera) | Anorexia, constipation, dry mouth, dysuria, erectile dysfunction/decreased libido, insomnia, liver damage (rare), mild appetite suppression, mild increase in diastolic blood pressure and pulse, nausea, sweating |
| Bupropion (Wellbutrin) | Constipation, dry mouth, headache, insomnia, nausea, sweating |
| Desipramine (Norpramin) | Anorexia, blurred vision, constipation, drowsiness, dry mouth, increase in blood pressure and pulse, insomnia, orthostatic hypotension, prolonged QT interval |
ADHD = attention-deficit/hyperactivity disorder.
Of note, other medications used in children with ADHD, such as modafinil (Provigil) and the alpha agonists clonidine (Catapres) and guanfacine (Tenex), do not have enough evidence in adults to be recommended at this time.
OTHER THERAPIES
Small studies have found that cognitive behavior therapy is helpful as an adjunct to medication in the treatment of ADHD in adults.21,31 The mechanism of how cognitive behavior therapy helps treat ADHD is uncertain, but it may help improve daily life skills affected by ADHD.
Meditation and St. John's wort have also been suggested as potential therapies, but at this time, there is no evidence to recommend either treatment.32,33
Comorbid Conditions
DEPRESSION
In general, depression should be treated before ADHD is treated. Also, the combination of an antidepressant and stimulants has been shown to be safe and effective. Of note, atomoxetine and selective serotonin reuptake inhibitors should not be combined because both medications are metabolized by the cytochrome P450 pathway.
BIPOLAR DISORDER
Stimulants should be avoided in patients with bipolar disorder, and mood stabilizers or atypical antipsychotics should be used instead.
ANXIETY DISORDERS
For patients with comorbid anxiety disorders, stimulants are a first-line treatment, followed by selective serotonin reuptake inhibitors and cognitive behavior therapy.23,34
INTELLECTUAL DISABILITIES
In those with intellectual disabilities, there is not enough evidence to recommend the use of stimulants for the treatment of ADHD.35 There have also been studies involving the use of risperidone (Risperdal) in this population, but there is insufficient evidence for effectiveness of this medication as well.36
REFERRAL
Because there is no compelling evidence regarding the specific point at which the family physician should refer patients to behavioral health services, that decision may best be based on other comorbidities for which the family physician would generally refer, including significant depression or anxiety; symptoms that are often a function of ADHD (e.g., issues with organization and planning, marital problems); and other major disabilities affecting daily function.
Stimulant Misuse and Diversion
One survey of almost 4,300 adults found a nonmedical use rate of stimulants of 2 percent.37 Young adults 18 to 25 years of age report a misuse rate of about 4 to 6 percent.37,38 Multiple studies regarding diversion of stimulants in college students have shown that this is a significant problem, with about 8 percent of students in one study reporting illicit stimulant use by the oral route and by intranasal use of crushed tablets.39 White men and persons with a history of alcohol or illicit drug use are more likely to misuse prescription stimulants.38 The World Health Organization has estimated a threefold increase in stimulant consumption versus a twofold increase in stimulant prescriptions written in the United States from 1995 to 2006.40
Accordingly, family physicians should consider several strategies to prevent misuse or diversion of stimulants prescribed for adults with ADHD. These include signing a controlled substances agreement; performing random urine drug screening to verify that the patient is taking the prescribed medication and to screen for nonprescribed or illicit drugs; and scheduling periodic follow-up visits to assess medication effectiveness and potential violation of the agreement.41
Data Sources: A PubMed search was completed using the key term adult ADHD combined in separate searches with diagnosis, management, and treatment. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence-based practice database, the Cochrane Database of Systematic Reviews, the National Guideline Clearinghouse database, and Essential Evidence Plus. Search date: January 10, 2011.

