
Am Fam Physician. 2012;85(10):987-988
Author disclosure: No relevant financial affiliations to disclose.
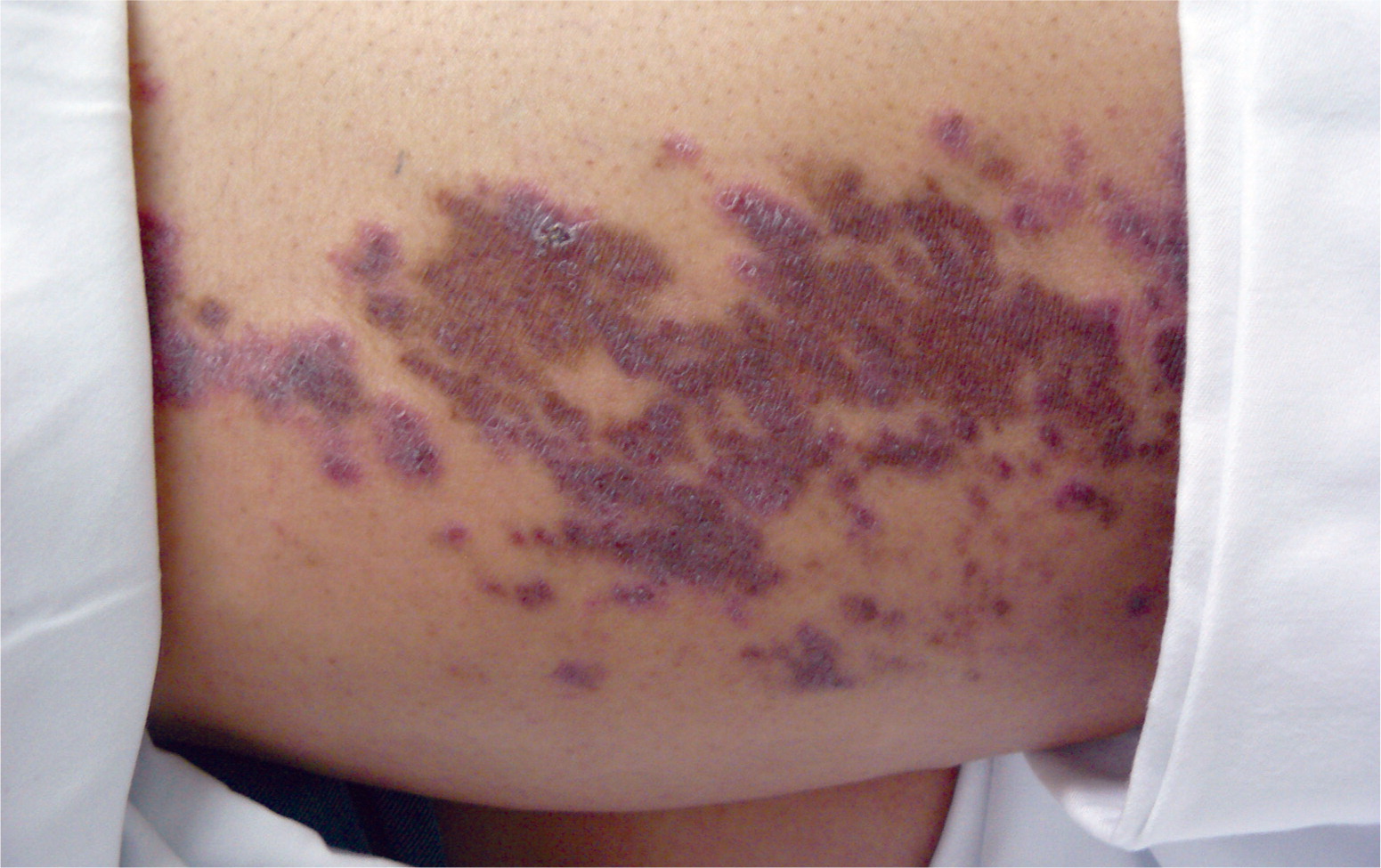
A 53-year-old woman presented with a pruritic rash on the back of her left thigh that had persisted for six months. She had no new contacts and had not taken any new medications. The rash had partially responded to a moderate-potency topical steroid cream, but never fully resolved. She had a history of uncontrolled type 2 diabetes mellitus, diabetic retinopathy, chronic foot ulcer, hypertension, hyperlipidemia, and obesity. Physical examination revealed multiple dark plaques that extended from the left buttock to the back of the left knee. The lesions were scaly, with an erythematous rim (see accompanying figure).
Question
Discussion
The answer is B: lichen planus. Lichen planus is a disorder of the skin and mucous membranes that affects middle-aged adults. It can be recurring or chronic.¹ The mechanism is unknown but is thought to be autoimmune. An association with hepatitis C or medication use has also been described.¹ The skin is most often involved, although the nails, oral mucosa, and genital mucosa also may be affected. The classic lesions occur on the flexor areas of the extremities and are pruritic, flat, violaceous papules and plaques.2
The subtypes of lichen planus include hypertrophic, linear, vesiculobullous, planopilaris, and sclerosus. Diagnosis is clinical but may be aided by biopsy. Lichen planus is treated with topical or intralesional steroids. Severe or generalized cases may be treated with systemic steroids, oral retinoids, phototherapy, cyclosporine (Sandimmune), and hydroxychloroquine (Plaquenil).2,3
In this patient, the final diagnosis was reached only after multiple biopsies. Prior to the diagnosis, the rash did not fully respond to topical therapy because the potency and length of treatment were not sufficient. When treating a chronic or extensive rash, it is helpful to perform a biopsy if the clinical diagnosis is unclear or if the biopsy results may change treatment options. Inconclusive results may require additional biopsies.
Kaposi sarcoma is an angioproliferative skin disorder caused by human herpesvirus 8 infection. It is characterized by dark purplish macules, papules, or plaques on the lower extremities.4 The lesions are most common in patients with untreated AIDS or in older men. Biopsy can confirm the diagnosis.
Although rare, mycosis fungoides is the most common type of cutaneous T-cell lymphoma. It usually occurs in men around 60 years of age. The lesions start as flat, erythematous macules that may be pruritic, and evolve into palpable, well-demarcated, asymmetrical plaques. Diagnosis is challenging because early stages of the disease may resemble psoriasis or eczema, and several biopsies may be necessary.5
Psoriasis is a common chronic, autoimmune, inflammatory disorder that is characterized by round or oval erythematous plaques distributed over extensor body surfaces and the scalp.6 Psoriatic plaques have dry, thin, silvery-white scaling and tend to be symmetrically distributed over the body. Diagnosis usually is reached clinically, with or without a skin biopsy.
| Condition | Characteristics |
|---|---|
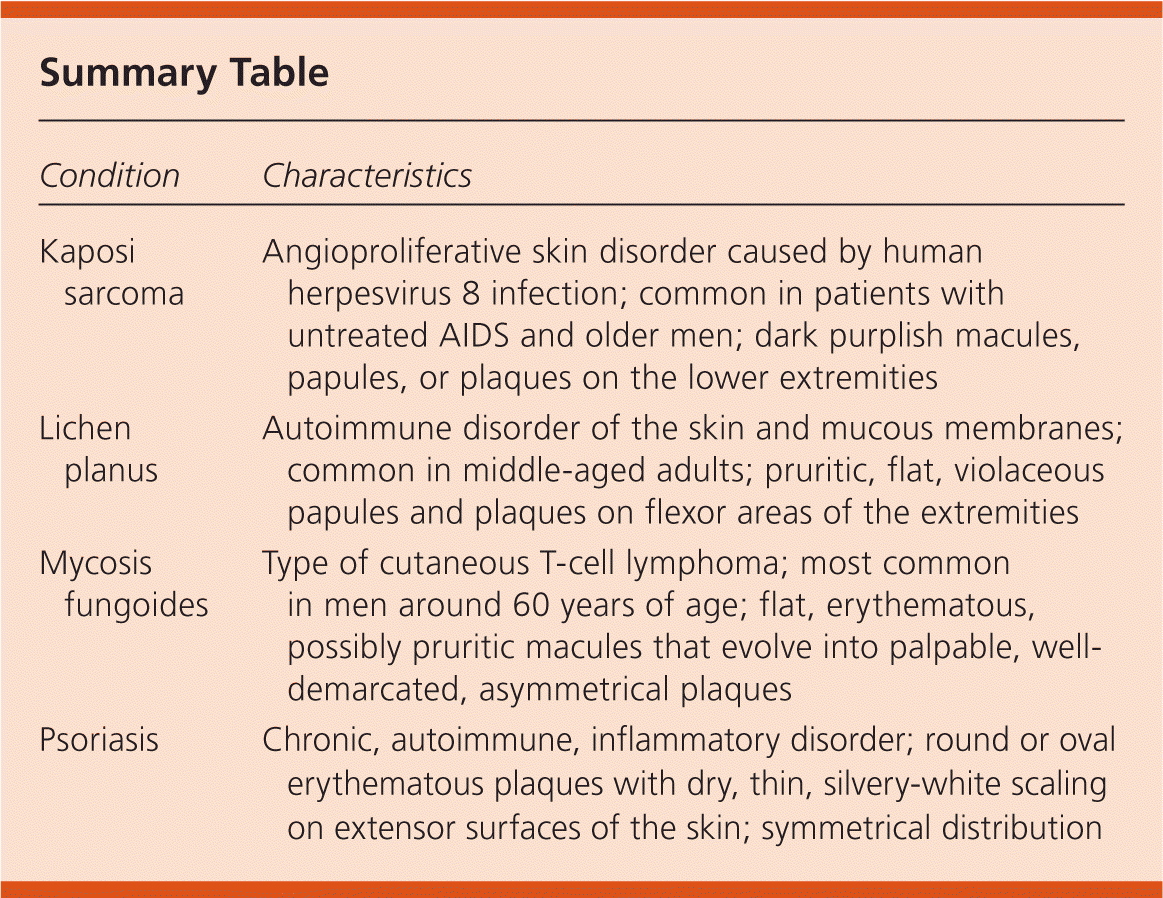
| Kaposi sarcoma | Angioproliferative skin disorder caused by human herpesvirus 8 infection; common in patients with untreated AIDS and older men; dark purplish macules, papules, or plaques on the lower extremities |
| Lichen planus | Autoimmune disorder of the skin and mucous membranes; common in middle-aged adults; pruritic, flat, violaceous papules and plaques on flexor areas of the extremities |
| Mycosis fungoides | Type of cutaneous T-cell lymphoma; most common in men around 60 years of age; flat, erythematous, possibly pruritic macules that evolve into palpable, well-demarcated, asymmetrical plaques |
| Psoriasis | Chronic, autoimmune, inflammatory disorder; round or oval erythematous plaques with dry, thin, silvery-white scaling on extensor surfaces of the skin; symmetrical distribution |
