Clinical Question
What is the likelihood of a serious outcome or death in patients presenting with syncope?
Evidence Summary
A previous Point-of-Care Guide addressed risk stratification in patients with syncope and described two validated clinical decision rules.1 Shared variables between the two rules included abnormal findings on electrocardiography (ECG) and a history of congestive heart failure; other variables included decreased systolic blood pressure, shortness of breath, anemia, age older than 45 years, and history of arrhythmia.2,3
Subsequently, seven further validation studies of one of these rules, the San Francisco Syncope Rule (SFSR), found some variation in its accuracy.4 In part, this may be attributed to different definitions used in the validation studies than in the original study, retrospective rather than prospective data collection, and ECG interpretation by someone other than the admitting emergency physician. Validation studies that avoided these issues had approximately 90 percent sensitivity and 60 percent specificity, which are not much lower than the original study.
Since the 2006 Point-of-Care Guide, two other clinical rules have been proposed and validated: the Risk Stratification of Syncope in the Emergency Department (ROSE) score5 and the Osservatorio Epidemiologico sulla Sincope nel Lazio (OESIL) score.6 This article summarizes these updated data (Table 1).3,5,6
Table 1. Scores for Stratifying Risk After an Episode of Syncope
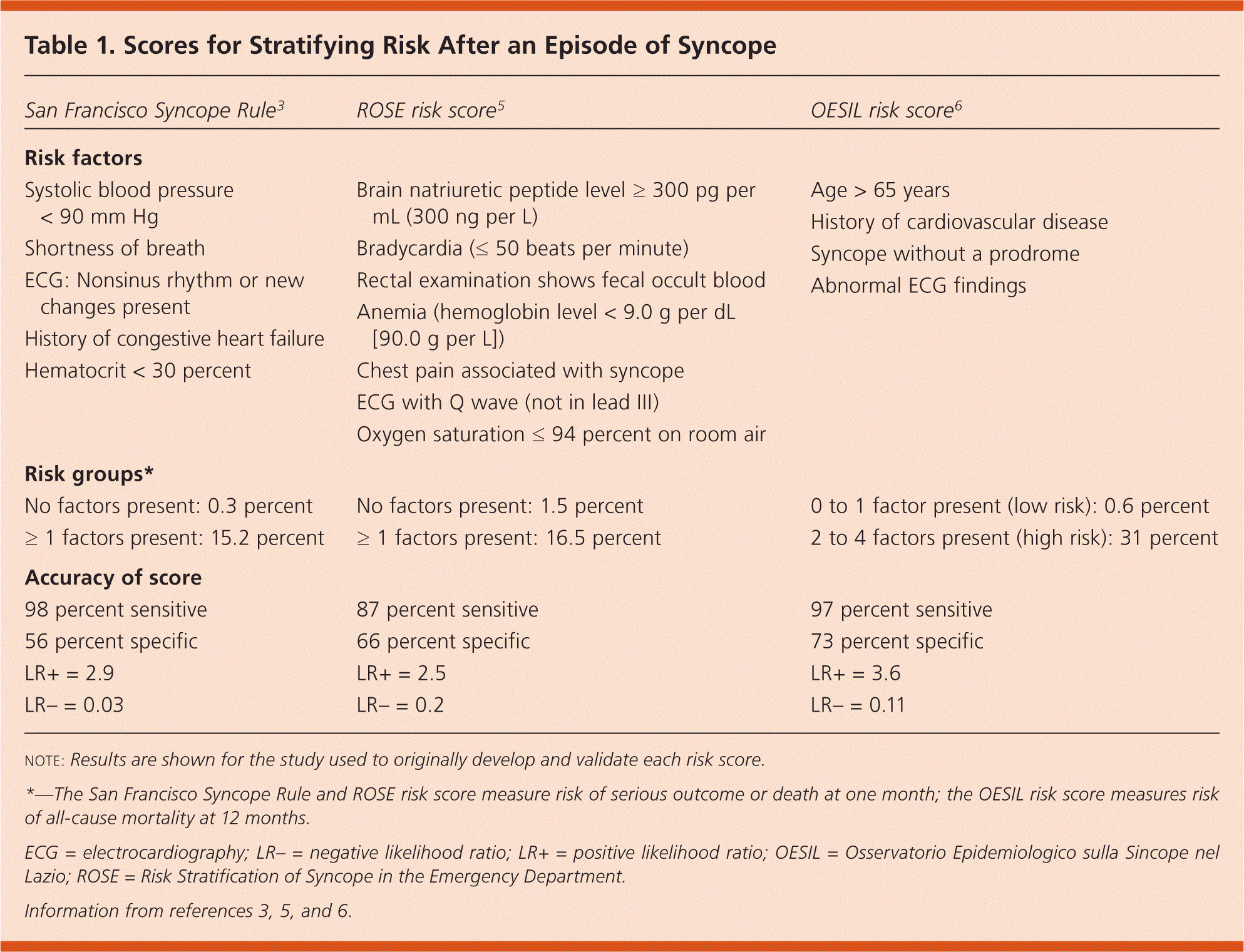
| San Francisco Syncope Rule3 | ROSE risk score5 | OESIL risk score6 |
|---|---|---|
| Risk factors | ||
|
|
|
| Risk groups* | ||
| No factors present: 0.3 percent | No factors present: 1.5 percent | 0 to 1 factor present (low risk): 0.6 percent |
| ≥ 1 factors present: 15.2 percent | ≥ 1 factors present: 16.5 percent | 2 to 4 factors present (high risk): 31 percent |
| Accuracy of score | ||
| 98 percent sensitive | 87 percent sensitive | 97 percent sensitive |
| 56 percent specific | 66 percent specific | 73 percent specific |
| LR+ = 2.9 | LR+ = 2.5 | LR+ = 3.6 |
| LR– = 0.03 | LR– = 0.2 | LR– = 0.11 |
note: Results are shown for the study used to originally develop and validate each risk score.
*—The San Francisco Syncope Rule and ROSE risk score measure risk of serious outcome or death at one month; the OESIL risk score measures risk of all-cause mortality at 12 months.
ECG = electrocardiography; LR– = negative likelihood ratio; LR+ = positive likelihood ratio; OESIL = Osservatorio Epidemiologico sulla Sincope nel Lazio; ROSE = Risk Stratification of Syncope in the Emergency Department.
The ROSE score was developed in a group of 529 patients 16 years and older presenting to a British emergency department with syncope; of these patients, 7.6 percent had a serious outcome (i.e., acute myocardial infarction, life-threatening arrhythmia, pacemaker or defibrillator placement, pulmonary embolus, serious hemorrhage, stroke, or need for surgery) or died within one month. It was validated in the next 538 syncopal patients presenting to the same institution. The average age of participants was 63 years; 45 percent were men; and 41 percent had a history of syncope. The score recommends admission for further evaluation if the patient has any of the risk factors shown in Table 1.3,5,6 Because the ROSE score requires measurement of brain natriuretic peptide levels, it is suitable only for use in hospital or emergency department settings. In the validation cohort, a serious outcome occurred in 16.5 percent of patients for whom admission was recommended, compared with 1.5 percent for whom it was not (positive likelihood ratio = 2.5, negative likelihood ratio = 0.2).5 There have been no further validation studies of the ROSE score.
The OESIL score was developed in a group of 270 patients older than 12 years presenting with syncope to one of six Italian hospitals; of these patients, 11.5 percent died within 12 months. The score was validated in a similar group of 328 consecutive patients from the same institutions. The mean age was 58 years; 46 percent were men; and 32 percent had experienced previous syncopal episodes. The score was 97 percent sensitive and 73 percent specific in the derivation group, and performed similarly in the validation group.6 A recent systematic review identified two additional validation studies for the OESIL score, which showed a sensitivity of 88 to 95 percent and a specificity of 11 to 59 percent.4
The clinical variables used by these decision rules highlight the most important elements of the history and physical examination to guide the assessment of patients with syncope. SFSR and ROSE scores will identify about 90 percent of persons who will have a serious outcome in the month after presentation, and the OESIL score will identify more than 95 percent of those who will die in the year following presentation. However, good clinical judgment is still needed to guide the final decision regarding hospital admission.
Applying the Evidence
A 67-year-old man presents with an episode of syncope accompanied by a prodrome of nausea. His ECG results are normal. He has no known history of cardiovascular disease, such as arrhythmia or heart failure, or of anemia. His hematocrit level is 43 percent, but he reports recent onset of increasing shortness of breath with activity. His oxygen saturation level is 93 percent on room air. Should he be admitted for further evaluation?


