Am Fam Physician. 2012;86(1):21-23
Author disclosure: No relevant financial affiliations to disclose.
Key Clinical Issue
Are there clinical advantages to augmenting standard therapy for stable ischemic heart disease with an angiotensin-converting enzyme (ACE) inhibitor or angiotensin receptor blocker (ARB)?
Evidence-Based Answer
Adding an ACE inhibitor to standard therapy reduces total mortality and cardiovascular events. Adding an ARB also reduces cardiovascular events. Overall effects are modest. Current evidence does not support the use of ACE inhibitor and ARB combinations over ACE inhibitors alone, because the risk of adverse events increases without additional benefit. Evidence suggests that adding ACE inhibitors or ARBs close to revascularization increases the risk of subsequent revascularization and hypotension. There were insufficient data to determine differences in effectiveness among specific ACE inhibitors and ARBs. (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
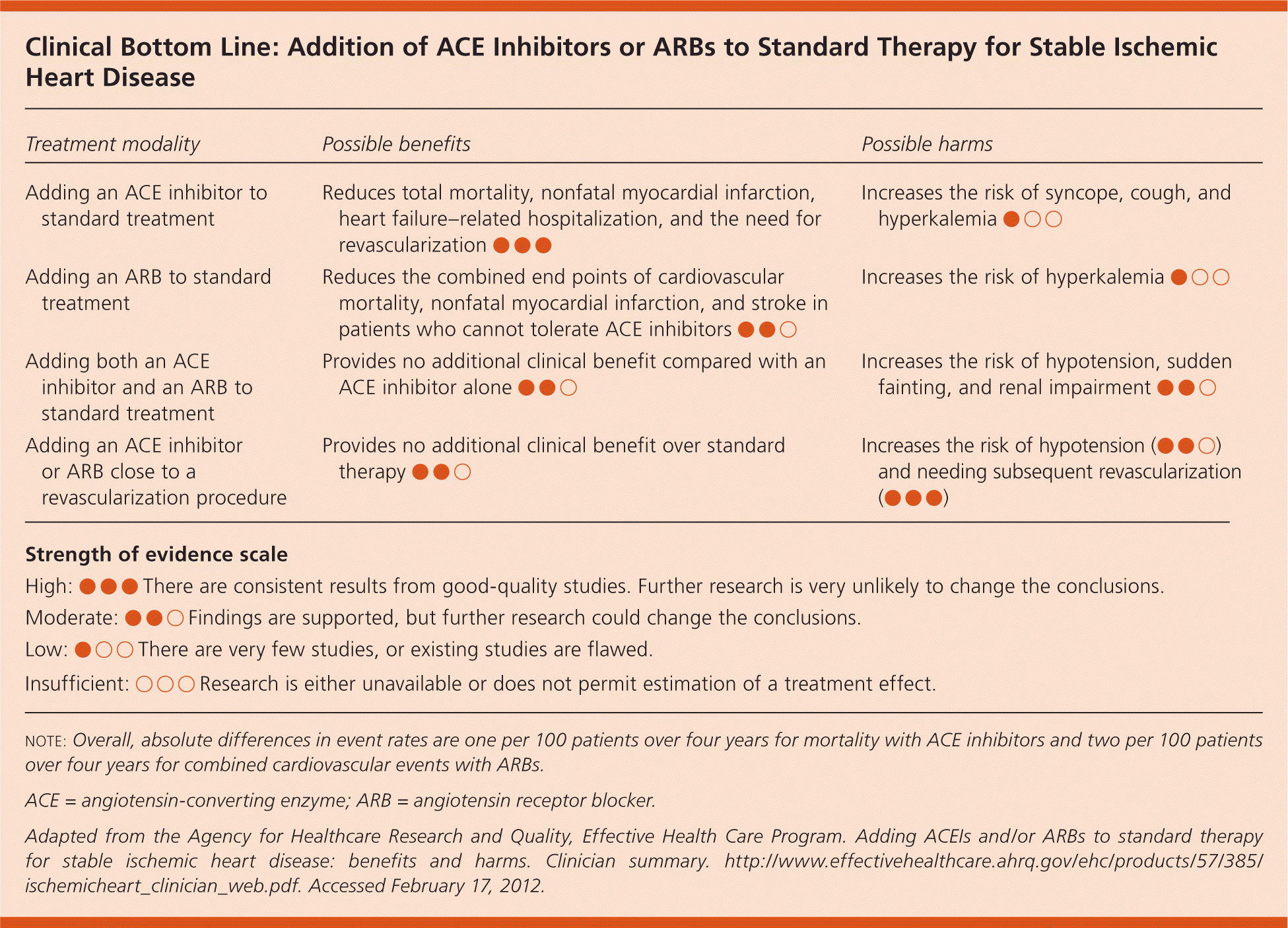
| Treatment modality | Possible benefits | Possible harms |
|---|---|---|
| Adding an ACE inhibitor to standard treatment | Reduces total mortality, nonfatal myocardial infarction, heart failure–related hospitalization, and the need for revascularization ● ● ● | Increases the risk of syncope, cough, and hyperkalemia ● ○ ○ |
| Adding an ARB to standard treatment | Reduces the combined end points of cardiovascular mortality, nonfatal myocardial infarction, and stroke in patients who cannot tolerate ACE inhibitors ● ● ○ | Increases the risk of hyperkalemia ● ○ ○ |
| Adding both an ACE inhibitor and an ARB to standard treatment | Provides no additional clinical benefit compared with an ACE inhibitor alone ● ● ○ | Increases the risk of hypotension, sudden fainting, and renal impairment ● ● ○ |
| Adding an ACE inhibitor or ARB close to a revascularization procedure | Provides no additional clinical benefit over standard therapy ● ● ○ | Increases the risk of hypotension (● ● ○) and needing subsequent revascularization (● ● ●) |
| Strength of evidence scale | ||
| High: ● ● ● There are consistent results from good-quality studies. Further research is very unlikely to change the conclusions. | ||
| Moderate: ● ● ○ Findings are supported, but further research could change the conclusions. | ||
| Low: ● ○ ○ There are very few studies, or existing studies are flawed. | ||
| Insufficient: ○ ○ ○ Research is either unavailable or does not permit estimation of a treatment effect. | ||
Practice Pointers
Medical management, which includes aspirin, statins, beta blockers, dual antiplatelet therapy, or combinations of these options, improves mortality in patients with chronic stable angina or stable ischemic heart disease, with or without comorbid heart failure.1 For patients with chronic stable angina and comorbid heart failure, the addition of ACE inhibitors or ARBs to standard medical therapy reduces myocardial infarction, hospital readmissions, and mortality.1
The Agency for Healthcare Research and Quality report examined whether the benefit of ACE inhibitors or ARBs in those with heart failure also applies to patients with chronic stable angina and normal systolic function.2 This meta-analysis of several randomized controlled trials demonstrated that ACE inhibitors or ARBs added to standard medical therapy in patients with ischemic heart disease and normal systolic function reduce total mortality (relative risk [RR] = 0.91; 95% confidence interval [CI], 0.84 to 0.98), nonfatal myocardial infarction (RR = 0.83; 95% CI, 0.73 to 0.94), stroke (RR = 0.79; 95% CI, 0.67 to 0.93), heart failure–related hospitalization (RR = 0.83; 95% CI, 0.70 to 0.98), and the need for revascularization (RR = 0.90; 95% CI, 0.85 to 0.96) compared with standard medical therapy alone at two to four years of follow-up.2 Most study patients were men (51 to 89 percent) with an average age of 59 to 67 years. Drugs used in these studies included ramipril (Altace), enalapril (Vasotec), perindopril (Aceon), trandolapril (Mavik), and telmisartan (Micardis). Benefits were consistent across the studies.
For patients who cannot tolerate ACE inhibitors, the addition of telmisartan, 80 mg daily, to standard therapy compared with standard therapy alone may modestly reduce the composite end points of cardiovascular mortality, nonfatal myocardial infarction, and stroke at 56 months of follow-up, based on a single randomized controlled trial of 5,926 patients.3 However, there was no statistically significant difference in the study’s primary composite outcomes of cardiovascular death, myocardial infarction, stroke, or hospitalization for heart failure.
One large, international, multicenter, randomized controlled trial (n = 25,620 patients from 733 centers) with a 56-month follow-up found that combination treatment with an ACE inhibitor and an ARB is no better than treatment with an ACE inhibitor alone in reducing cardiovascular and total mortality, myocardial infarction, and stroke.4 In addition, the combination increases the risk of hypotensive symptoms (4.8 versus 1.7 percent), syncope (0.3 versus 0.2 percent), and renal dysfunction (13.5 versus 10.2 percent).
ACE inhibitor and ARB therapy in patients with stable ischemic heart disease significantly increases the risk of discontinuation of therapy because of adverse events, and the risk of syncope, cough, and hyperkalemia compared with placebo. Angioedema, a rare but potentially serious reaction, has been reported in several studies and is more common with ACE inhibitors compared with ARBs when evaluated for all hypertensive indications.5 Rates of dizziness and headache are the same for ACE inhibitors and ARBs. Cough is more common with ACE inhibitors compared with ARBs (mean rate of 8.7 percent with ACE inhibitors versus 2.2 percent with ARBs).5
In summary, in addition to those with ischemic heart disease and comorbid heart failure, patients with ischemic heart disease and normal systolic function benefit from ACE inhibitors and ARBs. Initiating ACE inhibitors first, and reserving ARBs for those who cannot tolerate ACE inhibitors, makes sense based on the results of a meta-analysis and a systematic review.2,5 This benefit for ACE inhibitors and ARBs probably can be generalized to older populations and those with ischemic heart disease, but may not be generalized to younger populations or those with ischemic heart disease risk equivalents, such as diabetes mellitus or peripheral vascular disease. Combination treatment with an ACE inhibitor and an ARB in patients with ischemic heart disease, but without heart failure, should be discouraged because it is associated with more harm and no added effectiveness.