
Am Fam Physician. 2012;86(2):128-133
Author disclosure: No relevant financial affiliations to disclose.
Sometimes, the hardest thing for a physician to do is nothing: not ordering magnetic resonance imaging for a patient with acute, uncomplicated back pain; not prescribing antibiotics for a simple upper respiratory tract infection; not reaching for the prescription pad when patients—exhorted by a television advertisement—ask if some new medicine is “right for them.” And although patients are sometimes a source of excess utilization, physicians, responding to conventional practices, current fads, and the rituals of medicine, often order tests or treatments that don't stand up to clinical scrutiny. How do we do better? How do we know not only what to do, but also what not to do?
For years, we've had the benefit of practice guidelines, although these tend to focus mainly on what to do. A new program, the Choosing Wisely campaign, now prompts physicians and patients to avoid unnecessary testing and treatment, things that not only don't help, but that also may lead to harm.
Initially sponsored by nine medical specialty societies, the campaign consists of specialty-specific top-five lists of common tests and procedures that are often performed unnecessarily, when they are not likely to improve a patient's health. The primary focus of the campaign is to improve health care quality and reduce harm by avoiding unnecessary interventions, with the added benefit of lowering costs. Even seemingly innocuous interventions, such as magnetic resonance imaging or a simple blood test, can be harmful, even fatal, if they lead to additional testing, invasive procedures, and a small but predictable rate of complications.
More information about the Choosing Wisely campaign is available at http://choosingwisely.org. In addition, Consumer Reports Health is helping get the word out to consumers (http://consumerhealthchoices.org/campaigns/choosing-wisely). The campaign's lead paper was recently published as part of the “Less Is More” series in Archives of Internal Medicine, and contains the top-five lists from family medicine, internal medicine, and pediatrics.1 However, given family medicine's broad scope, segregating various items into specialty-specific lists is somewhat artificial. To avoid unnecessarily limiting these lists to just five areas in which quality of care could be improved, I've compiled all the relevant items from the three primary care specialties (see accompanying table).
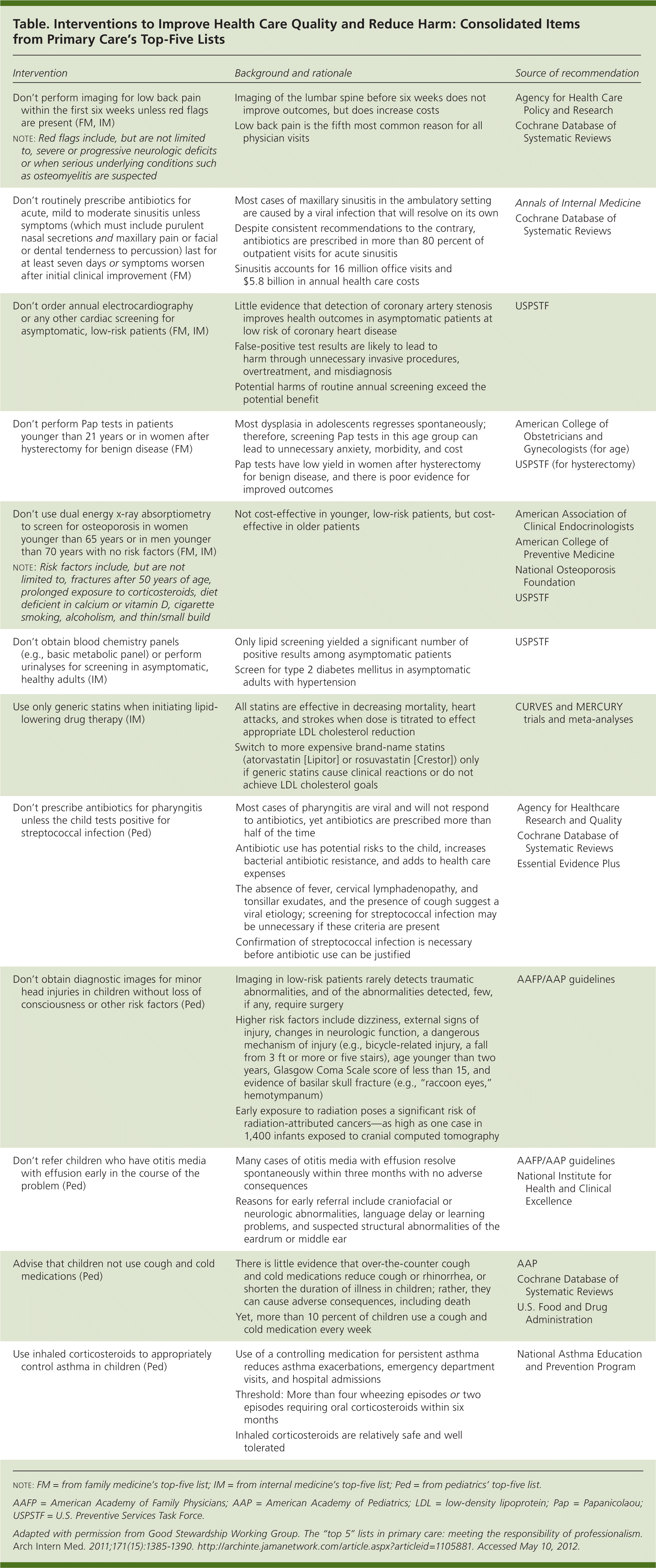
| Intervention | Background and rationale | Source of recommendation |
|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Other medical specialties have already joined the campaign and will contribute their top-five lists in the coming months. To help our readers, American Family Physician will maintain a running catalog of items relevant to family medicine on our Web site (see “Choosing Wisely: Top Interventions to Improve Health Care Quality and Reduce Harm” at https://www.aafp.org/online/en/home/publications/journals/afp/ebmtoolkit/choosingwisely.html).
editor's note: Dr. Siwek is editor of American Family Physician.
