The common cold, or upper respiratory tract infection, is one of the leading reasons for physician visits. Generally caused by viruses, the common cold is treated symptomatically. Antibiotics are not effective in children or adults. In children, there is a potential for harm and no benefits with over-the-counter cough and cold medications; therefore, they should not be used in children younger than four years. Other commonly used medications, such as inhaled corticosteroids, oral prednisolone, and Echinacea, also are ineffective in children. Products that improve symptoms in children include vapor rub, zinc sulfate, Pelargonium sidoides (geranium) extract, and buckwheat honey. Prophylactic probiotics, zinc sulfate, nasal saline irrigation, and the herbal preparation Chizukit reduce the incidence of colds in children. For adults, antihistamines, intranasal corticosteroids, codeine, nasal saline irrigation, Echinacea angustifolia preparations, and steam inhalation are ineffective at relieving cold symptoms. Pseudoephedrine, phenylephrine, inhaled ipratropium, and zinc (acetate or gluconate) modestly reduce the severity and duration of symptoms for adults. Nonsteroidal anti-inflammatory drugs and some herbal preparations, including Echinacea purpurea, improve symptoms in adults. Prophylactic use of garlic may decrease the frequency of colds in adults, but has no effect on duration of symptoms. Hand hygiene reduces the spread of viruses that cause cold illnesses. Prophylactic vitamin C modestly reduces cold symptom duration in adults and children.
The common cold, or upper respiratory tract infection, usually is caused by one of several respiratory viruses, most commonly rhinovirus. These viruses, which concentrate in nasal secretions, are easily transmitted through sneezing, coughing, or nose blowing. Signs and symptoms of the common cold include fever, cough, rhinorrhea, nasal congestion, sore throat, headache, and myalgias.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Antibiotics should not be used for the treatment of cold symptoms in children or adults. | A | 7 |
| Over-the-counter cough and cold medications should not be used in children younger than four years because of potential harms and lack of benefit. | B | 4, 6, 11 |
| Treatment with buckwheat honey, Pelargonium sidoides (geranium) extract (Umcka Coldcare), nasal saline irrigation, vapor rub, or zinc sulfate may decrease cold symptoms in children. | B | 16–20 |
| Codeine is not effective for cough in adults. | A | 11, 24 |
| Antihistamine monotherapy (sedating and nonsedating) does not improve cold symptoms in adults. | A | 11, 23, 29 |
| Decongestants, antihistamine/decongestant combinations, and intranasal ipratropium (Atrovent) may improve cold symptoms in adults. | B | 11, 23, 32, 33 |
| Nonsteroidal anti-inflammatory drugs reduce pain secondary to upper respiratory tract infection in adults. | A | 34 |
| Andrographis paniculata (Kalmcold) and P. sidoides may reduce severity and duration of cold symptoms in adults. | B | 35–37 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Patients seek care for cold symptoms during all seasons of the year, with cough being the third most common and nasal congestion the 15th most common presenting symptom among all office visits.1 The common cold is the third most common primary diagnosis in office visits.1 Colds are self-limited, usually lasting up to 10 days; therefore, management is directed at symptom relief rather than treating the infection. Multiple remedies, including complementary and alternative medicine products, over-the-counter products, and prescription drugs, have been used to prevent and treat cold symptoms.
When medications are requested, physicians play an important role in educating patients about the treatment choices. Many familiar prescription cough and cold medications were removed from the market in early 2011 because the U.S. Food and Drug Administration had not evaluated them for safety, effectiveness, or quality.2 Physicians should caution patients about over-the-counter and complementary and alternative medicine products because manufacturers are not required to prove claims of therapeutic benefit.
Children
Cold and cough medications are among the top 20 substances leading to death in children younger than five years.3 In 2008, the U.S. Food and Drug Administration recommended that over-the-counter cough and cold medications be avoided in children younger than two years.4 After the removal of over-the-counter infant cough and cold medications from pharmacy shelves, the estimated number of emergency department visits for adverse events involving these medications was cut in half for children younger than two years.5 Manufacturers of these medications have voluntarily modified the product labels to state that they should not be used in children younger than four years.6
INEFFECTIVE INTERVENTIONS
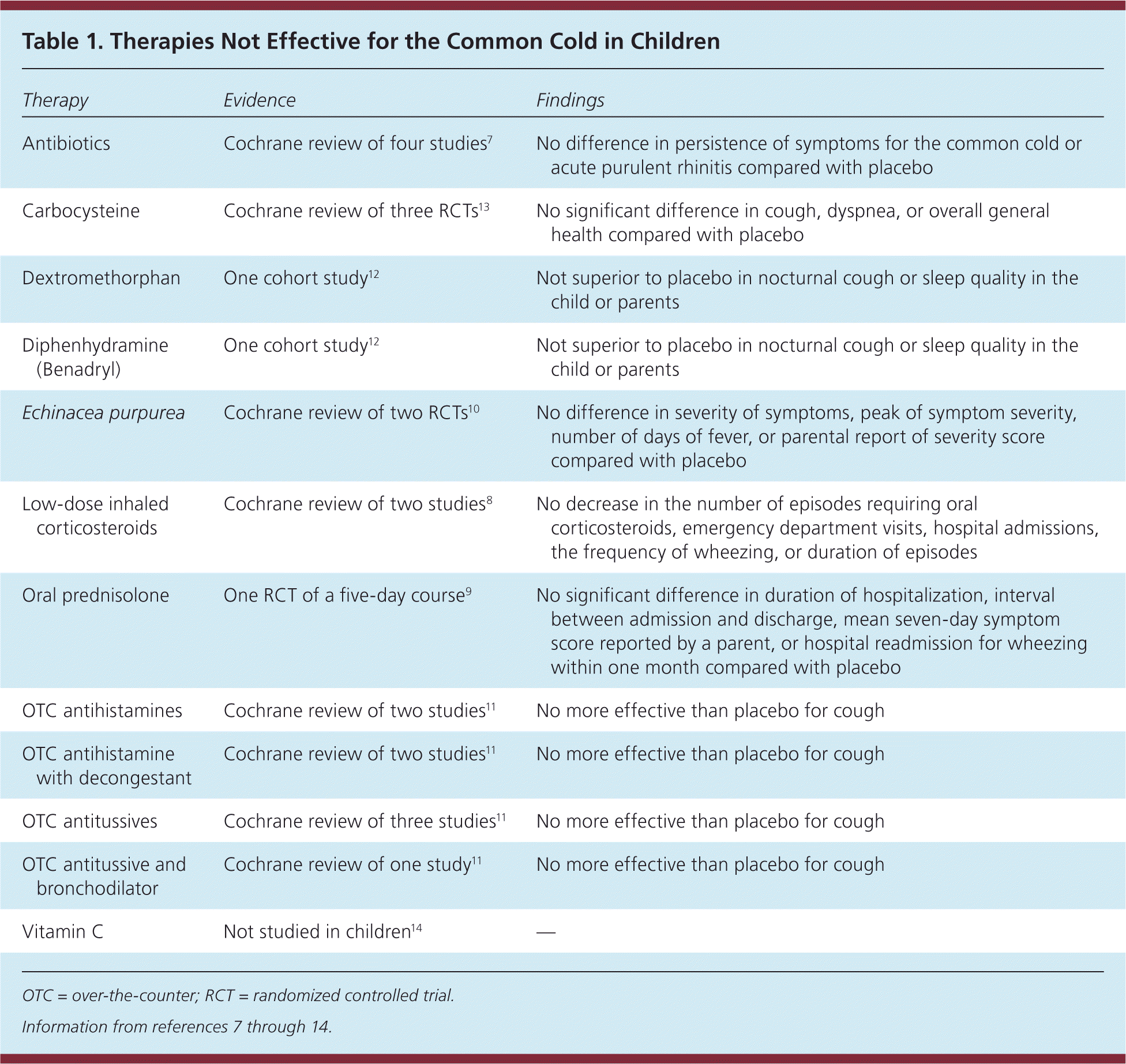
Prescription and Over-the-Counter Products. Because viruses cause most colds, antibiotics are ineffective.7 Low-dose inhaled corticosteroids8 and oral prednisolone9 do not improve outcomes in children without asthma. Echinacea products also are ineffective for treating cold symptoms in children.10 There is no evidence to support the use of most over-the-counter cough remedies in children.11,12 Table 1 summarizes findings of studies on these medications.7–14
Table 1. Therapies Not Effective for the Common Cold in Children
| Therapy | Evidence | Findings |
|---|---|---|
| Antibiotics | Cochrane review of four studies7 | No difference in persistence of symptoms for the common cold or acute purulent rhinitis compared with placebo |
| Carbocysteine | Cochrane review of three RCTs13 | No significant difference in cough, dyspnea, or overall general health compared with placebo |
| Dextromethorphan | One cohort study12 | Not superior to placebo in nocturnal cough or sleep quality in the child or parents |
| Diphenhydramine (Benadryl) | One cohort study12 | Not superior to placebo in nocturnal cough or sleep quality in the child or parents |
| Echinacea purpurea | Cochrane review of two RCTs10 | No difference in severity of symptoms, peak of symptom severity, number of days of fever, or parental report of severity score compared with placebo |
| Low-dose inhaled corticosteroids | Cochrane review of two studies8 | No decrease in the number of episodes requiring oral corticosteroids, emergency department visits, hospital admissions, the frequency of wheezing, or duration of episodes |
| Oral prednisolone | One RCT of a five-day course9 | No significant difference in duration of hospitalization, interval between admission and discharge, mean seven-day symptom score reported by a parent, or hospital readmission for wheezing within one month compared with placebo |
| OTC antihistamines | Cochrane review of two studies11 | No more effective than placebo for cough |
| OTC antihistamine with decongestant | Cochrane review of two studies11 | No more effective than placebo for cough |
| OTC antitussives | Cochrane review of three studies11 | No more effective than placebo for cough |
| OTC antitussive and bronchodilator | Cochrane review of one study11 | No more effective than placebo for cough |
| Vitamin C | Not studied in children14 | — |
OTC = over-the-counter; RCT = randomized controlled trial.
Fluids. Caregivers are often advised to increase a child's fluid intake. However, in two case series and a prevalence study, some children with respiratory infections but no signs of dehydration developed hyponatremia with increased fluids.15 Therefore, extra fluid intake is not advised in children because of potential harm.
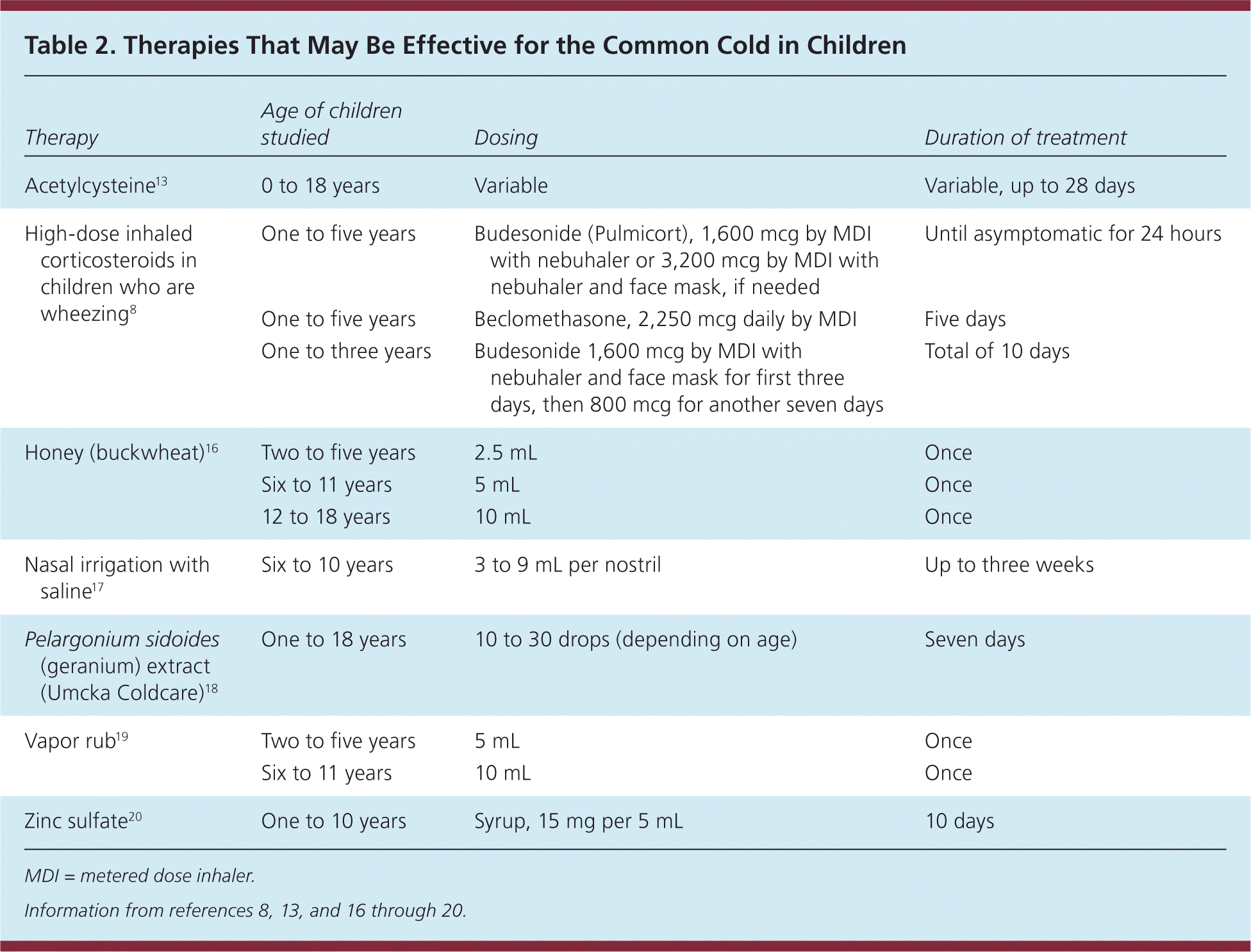
EFFECTIVE INTERVENTIONS
Table 2. Therapies That May Be Effective for the Common Cold in Children
| Therapy | Age of children studied | Dosing | Duration of treatment |
|---|---|---|---|
| Acetylcysteine13 | 0 to 18 years | Variable | Variable, up to 28 days |
| High-dose inhaled corticosteroids in children who are wheezing8 | One to five years | Budesonide (Pulmicort), 1,600 mcg by MDI with nebuhaler or 3,200 mcg by MDI with nebuhaler and face mask, if needed | Until asymptomatic for 24 hours |
| One to five years | Beclomethasone, 2,250 mcg daily by MDI | Five days | |
| One to three years | Budesonide 1,600 mcg by MDI with nebuhaler and face mask for first three days, then 800 mcg for another seven days | Total of 10 days | |
| Honey (buckwheat)16 | Two to five years | 2.5 mL | Once |
| Six to 11 years | 5 mL | Once | |
| 12 to 18 years | 10 mL | Once | |
| Nasal irrigation with saline17 | Six to 10 years | 3 to 9 mL per nostril | Up to three weeks |
| Pelargonium sidoides (geranium) extract (Umcka Coldcare)18 | One to 18 years | 10 to 30 drops (depending on age) | Seven days |
| Vapor rub19 | Two to five years | 5 mL | Once |
| Six to 11 years | 10 mL | Once | |
| Zinc sulfate20 | One to 10 years | Syrup, 15 mg per 5 mL | 10 days |
MDI = metered dose inhaler.
Complementary and Alternative Medicine Products. Several of these therapies provide relief from cold symptoms. Vapor rub applied to the chest and neck has been shown to improve cough severity and quality of sleep for the child and parents, but it has a strong smell that children may not tolerate.19 Studies regarding therapeutic use of zinc sulfate show a trend toward decreased duration of cold symptoms when it is taken within the first 24 hours of symptom onset.20 Adverse effects, such as bad taste and nausea, are more common with zinc lozenges than with syrup or tablets.20 Pelargonium sidoides (geranium) extract (Umcka Coldcare) may help resolve cough and sputum production in children with the common cold.18 Buckwheat honey is superior to placebo for reducing frequency of cough, reducing bothersome cough, and improving quality of sleep for the child.16 Honey should not be used in children younger than one year because of the risk of botulism.
Nasal Irrigation and Acetylcysteine. During acute illness, nasal irrigation with saline can help alleviate sore throat, thin nasal secretions, and improve nasal breathing and can reduce the need for nasal decongestants and mucolytics.17 A systematic review of six trials published in the 1990s found that acetylcysteine (commonly used in Europe, but not in the United States, as a mucolytic) may decrease cough after six to seven days of therapy in children older than two years.13 The main adverse effect of acetylcysteine is vomiting.
Inhaled Corticosteroids. Some children with viral cold symptoms also develop wheezing. Although low-dose corticosteroids are ineffective in these children, one review of high-dose inhaled corticosteroids found a trend toward decreased frequency of wheezing episodes that require oral corticosteroids, the duration of episodes, and the number of physician visits.8
PROPHYLAXIS
Table 3. Therapies That May Be Effective for Common Cold Prophylaxis in Children

| Therapy | Age of children studied | Dosing | Duration of treatment |
|---|---|---|---|
| Chizukit21 | One to three years | 5 mL twice daily | 12 weeks |
| Four to five years | 7.5 mL twice daily | 12 weeks | |
| Nasal irrigation with saline17 | Six to 10 years | 3 to 9 mL per nostril three times daily | Nine weeks |
| Probiotics*22 | Three to five years | 1 g (1 × 1010 colony-forming units) mixed with 120 mL of 1% milk twice daily | Six months |
| Vitamin C14 | < 12 years | 0.2 to 2 g daily | Two weeks to nine months |
| Zinc sulfate20 | One to 10 years | Syrup, 15 mg per 5 mL daily | Seven months |
| 6.5 to 16 years | Tablet, 10 mg daily | Six days per week for five months |
*—Lactobacillus acidophilus NCFM, alone or combined with Bifidobacterium animalis.
Complementary and Alternative Medicine Products. Some of these products may help prevent colds if taken regularly. Probiotics, such as Lactobacillus acidophilus NCFM, alone or combined with Bifidobacterium animalis, taken by healthy children during the winter may reduce day care absences; the incidence of fever, cough, and rhinorrhea; and the use of antibiotics.22
A Cochrane review showed a 13 percent decrease in cold symptoms in children who took 1 g of vitamin C daily before illness, although optimal duration of treatment to achieve these benefits is unknown.14 Zinc sulfate used prophylactically for at least five months reduces the incidence of viral colds, absences from school, and antibiotic use in children.20
The herbal preparation Chizukit contains 50 mg per mL of Echinacea, 50 mg per mL of propolis, and 10 mg per mL of vitamin C.21 In a randomized, placebo-controlled trial of 430 children one to five years of age, Chizukit decreased the number of cold episodes, the number of days the child was ill, and the number of days the child missed school. It also decreased the need for antipyretics and antibiotics; physician visits; and episodes of otitis media, pneumonia, and tonsillitis. However, children may not comply with taking the product because of its unpleasant taste.21
Nasal Saline Irrigation. Nasal irrigation with saline as a preventive measure in children is better than standard treatment for multiple cold symptoms. Overall, the treatment decreases illness and nasal secretions, improving nasal breathing. These children also use fewer antipyretics, nasal decongestants, and mucolytics and have fewer school absences.17
Adults
INEFFECTIVE INTERVENTIONS
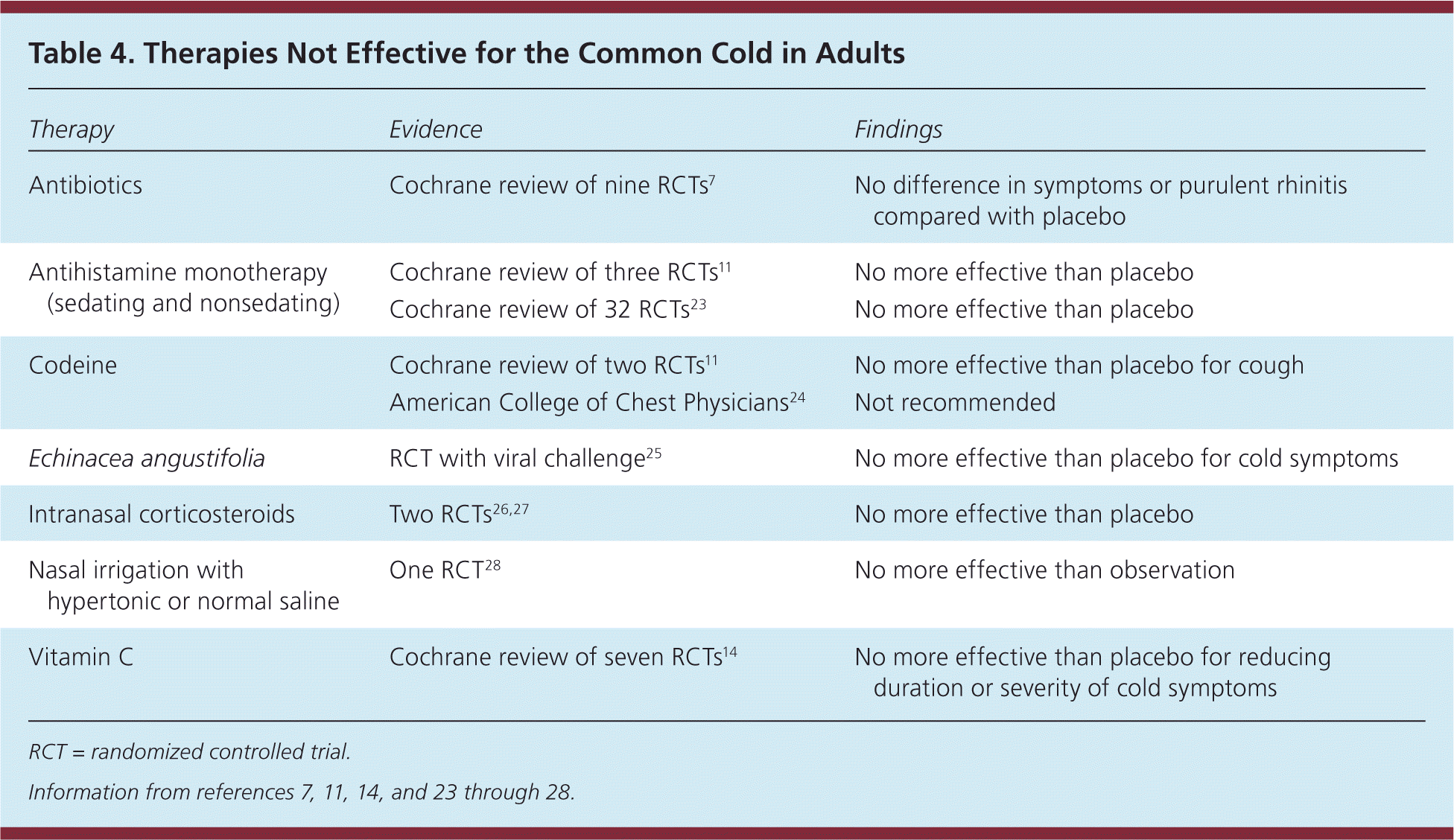
Table 4 summarizes studies of medications that are ineffective for the common cold in adults.7,11,14,23–28
Table 4. Therapies Not Effective for the Common Cold in Adults
| Therapy | Evidence | Findings |
|---|---|---|
| Antibiotics | Cochrane review of nine RCTs7 | No difference in symptoms or purulent rhinitis compared with placebo |
| Antihistamine monotherapy (sedating and nonsedating) | Cochrane review of three RCTs11 | No more effective than placebo |
| Cochrane review of 32 RCTs23 | No more effective than placebo | |
| Codeine | Cochrane review of two RCTs11 | No more effective than placebo for cough |
| American College of Chest Physicians24 | Not recommended | |
| Echinacea angustifolia | RCT with viral challenge25 | No more effective than placebo for cold symptoms |
| Intranasal corticosteroids | Two RCTs26,27 | No more effective than placebo |
| Nasal irrigation with hypertonic or normal saline | One RCT28 | No more effective than observation |
| Vitamin C | Cochrane review of seven RCTs14 | No more effective than placebo for reducing duration or severity of cold symptoms |
RCT = randomized controlled trial.
Antibiotics and Antihistamines. In adults, as in children, antibiotics do not decrease the duration or severity of illness, even when purulent rhinitis is present.7 Sedating and nonsedating antihistamines are ineffective for cough and other cold symptoms.11,23,29
Opioids, Intranasal Corticosteroids, and Nasal Saline Irrigation. Despite widespread use, codeine is no more effective than placebo for reducing cough.11,24 The American College of Chest Physicians (ACCP) does not recommend other opioids for the treatment of cough.24 Although intranasal corticosteroids reduce swelling and inflammation of the nasal mucosa, they have not been shown to significantly benefit patients with the common cold.26,27 Nasal irrigation with hypertonic or normal saline does not provide significant relief for cold symptoms in adults.28
Complementary and Alternative Medicine Products. When used solely for treatment of symptoms after they appear, vitamin C does not consistently reduce their duration or severity.14 Herbal preparations containing Echinacea angustifolia are not beneficial.25 Many physicians have recommended increased fluid intake and inhalation of heated, humidified air to thin secretions during a cold. No randomized trials have assessed the effect of increasing fluid intake in adults,30 and a Cochrane review found inconsistent study results for steam inhalation.31
EFFECTIVE INTERVENTIONS
Decongestants With or Without Antihistamines. Oral or topical decongestants alone seem to be somewhat effective for short-term relief of cold symptoms, compared with placebo.32 Pseudoephedrine and phenylephrine decrease nasal edema to improve air intake.32 Although antihistamines do not work as monotherapy, combination medications containing a first-generation antihistamine and decongestant may be slightly beneficial in relieving general symptoms, nasal symptoms,23 and cough.11 Combination medications are recommended by the ACCP to treat acute cough.29
Anticholinergics, Dextromethorphan, Guaifenesin. Ipratropium (Atrovent) is the only orally inhaled anticholinergic recommended by the ACCP for cough caused by a common cold,24 and one study showed that the nasal formulation decreases rhinorrhea and sneezing.33 Studies of dextromethorphan and guaifenesin for cough are almost evenly split, with some demonstrating benefit and others not.11,24
Nonsteroidal Anti-inflammatory Drugs. These medications effectively relieve pain from headache, myalgias, and arthralgias experienced during a cold; however, decreased sneezing is the only effect they have on respiratory symptoms.34 The ACCP has concluded that naproxen (Naprosyn) is beneficial in the treatment of acute cough.24
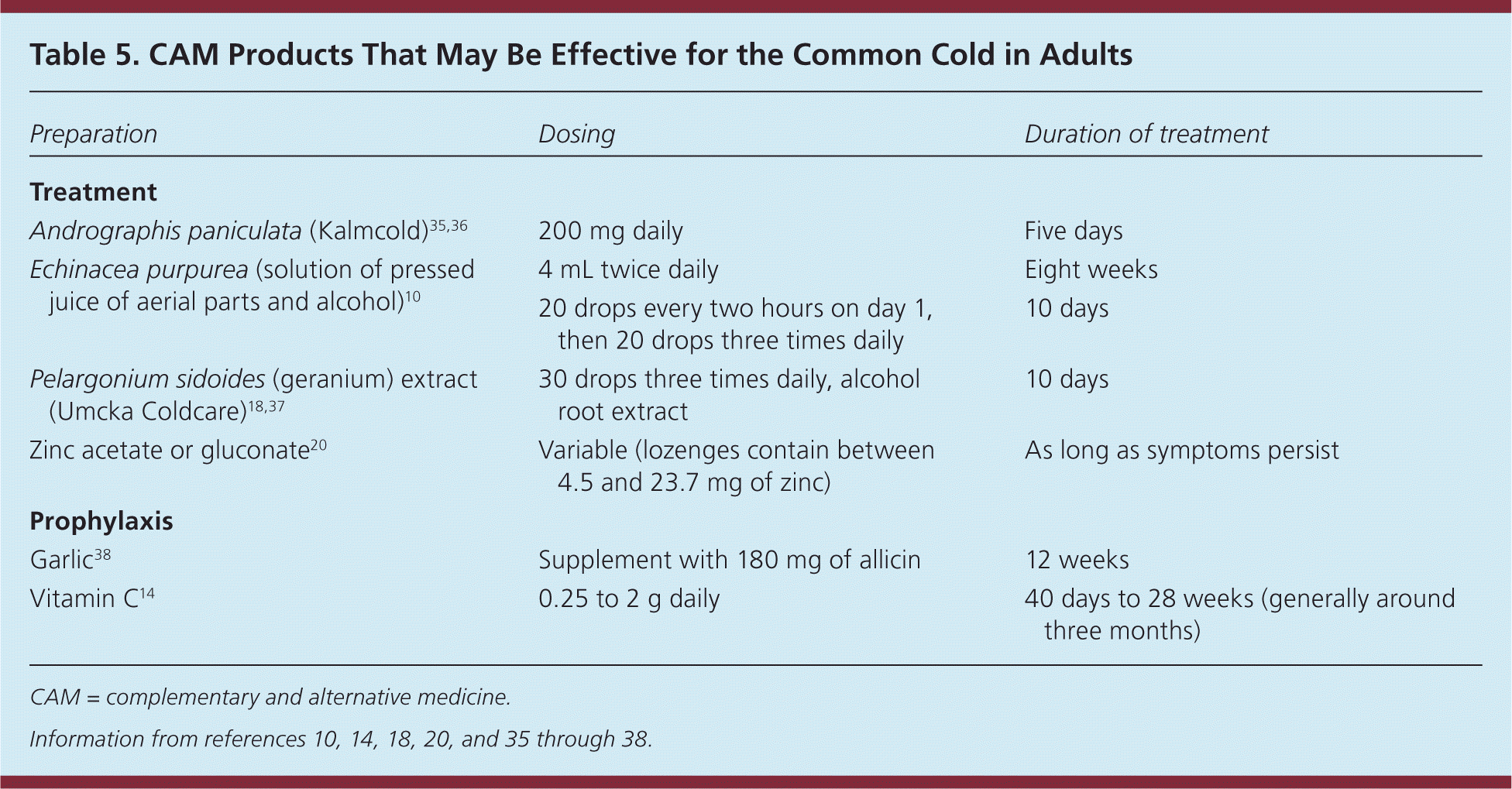
Complementary and Alternative Medicine Products. Table 5 summarizes the herbal preparations that may be effective in adults.10,14,18,20,35–38 An herbal solution containing P. sidoides was shown to reduce the duration and severity of 10 different cold symptoms in a randomized controlled trial.37 Another randomized controlled trial demonstrated the benefit of Andrographis paniculata (Kalmcold) in improving symptom scores.35 A systematic review also indicated that A. paniculata, alone or in combination with Acanthopanax senticosus, may be more effective for symptom relief than placebo.36
Table 5. CAM Products That May Be Effective for the Common Cold in Adults
| Preparation | Dosing | Duration of treatment |
|---|---|---|
| Treatment | ||
| Andrographis paniculata (Kalmcold)35,36 | 200 mg daily | Five days |
| Echinacea purpurea (solution of pressed juice of aerial parts and alcohol)10 | 4 mL twice daily | Eight weeks |
| 20 drops every two hours on day 1, then 20 drops three times daily | 10 days | |
| Pelargonium sidoides (geranium) extract (Umcka Coldcare)18,37 | 30 drops three times daily, alcohol root extract | 10 days |
| Zinc acetate or gluconate20 | Variable (lozenges contain between 4.5 and 23.7 mg of zinc) | As long as symptoms persist |
| Prophylaxis | ||
| Garlic38 | Supplement with 180 mg of allicin | 12 weeks |
| Vitamin C14 | 0.25 to 2 g daily | 40 days to 28 weeks (generally around three months) |
CAM = complementary and alternative medicine.
Information from references 10, 14, 18, 20, and 35 through 38.
Early use of Echinacea purpurea shortens duration and decreases severity of cold symptoms; preparations with the aerial parts versus the flowering parts are most effective.10 Although dosages and preparations of zinc are not standardized, a Cochrane review showed that starting zinc lozenges (acetate or gluconate) within the first 24 hours of symptom onset reduces the severity and duration of illness.20 Adverse effects of zinc include bad taste and nausea.20 Intranasal zinc should not be used because it may result in the permanent loss of smell.39
PROPHYLAXIS
Few medications have been shown to be beneficial in preventing the common cold in adults (Table 510,14,18,20,35–38 ). The prophylactic use of vitamin C does not reduce the incidence of colds, but decreases illness duration by 8 percent.14 Limited, poor-quality studies of garlic show a decrease in the number of self-reported colds, but no decrease in days to recovery. Adverse effects from garlic included bad odor and skin rash.38
Frequent hand washing can reduce the spread of respiratory viruses in all ages and can reduce transmission from children to other household members.40 In a large meta-analysis, the benefits of antibacterial and nonantibacterial soaps were not significantly different.41 Benzalkonium chloride–based hand sanitizers that foam and leave a residue have a protective effect against colds. Alcohol hand sanitizers are less effective.41
Data Sources: A search of Essential Evidence Plus was completed using the key words cold and respiratory tract infections. This search included InfoPOEMs, Cochrane reviews, and practice guidelines. We also searched Dynamed and the U.S. Food and Drug Administration Web site for specific information regarding changes in recommendations for the use of cough and cold medications in children. Search dates: March 22, 2011, to April 6, 2011.

