Guideline source: Infectious Diseases Society of America
Evidence rating system used? Yes
Literature search described? Yes
Guideline developed by participants without relevant financial ties to industry? No
Published source: Clinical Infectious Diseases, October 2011
Available at: http://cid.oxfordjournals.org/content/53/7/617.full
Previously published guidelines for the management of community-acquired pneumonia (CAP) in adults have been shown to decrease morbidity and mortality rates. Although the effectiveness of these guidelines in adults has been clearly established, the clinical course of CAP in children varies considerably from one child to the next. As a result, physicians may employ other approaches to the diagnosis and treatment of CAP in infants and children, even when infection is caused by the same pathogen. In response, the Pediatric Infectious Diseases Society (PIDS) and the Infectious Diseases Society of America (IDSA) have created new guidelines to address the management of CAP in infants and children.
The guidelines are designed to advise primary care physicians and subspecialists who are responsible for the management of CAP in otherwise healthy infants and children in inpatient and outpatient settings. Areas of discussion include site-of-care management, diagnosis, antimicrobial therapy, and adjunctive surgical therapy. The scope of the guidelines does not include management of CAP in newborns and infants younger than three months, children with compromised immune systems, children receiving home mechanical ventilation, or children with chronic conditions or underlying lung disease. This summary focuses on the management of CAP in infants and young children as normally seen by family physicians in the outpatient setting, such as an office or urgent care clinic.
Site-of-Care Management Decisions
When does a child or infant with CAP require hospitalization?
Children and infants who have moderate to severe CAP, including respiratory distress and hypoxemia (Table 1), should be hospitalized for management. Infants three to six months of age with suspected bacterial CAP will likely benefit from being hospitalized. If a child or infant is suspected of having CAP, or is known to have CAP as a result of a virulent pathogen such as community-associated methicillin-resistant Staphylococcus aureus, the patient should be hospitalized. If there is concern that the child or infant may not receive careful observation at home or may not be able to comply with therapy, or that the physician may be unable to have a follow-up visit with the child, the patient should be hospitalized.
Table 1. Criteria for Respiratory Distress in Children and Infants with Pneumonia

| Altered mental status | |
| Apnea | |
| Dyspnea | |
| Grunting | |
| Nasal flaring | |
| Pulse oximetry < 90 percent on room air | |
| Retractions (i.e., suprasternal, intercostal, or subcostal) | |
| Tachypnea, respiratory rate, breaths per minute* | |
| 0 to 2 months: > 60 | |
| 2 to 12 months: > 50 | |
| 1 to 5 years: > 40 | |
| > 5 years: > 20 | |
*—Adapted from World Health Organization criteria.
Adapted with permission from Bradley JS, Byington CL, Shah SS, et al. Executive summary: the management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin Infect Dis. 2011;53(7):620. Available at http://cid.oxfordjournals.org.
Diagnostic Testing for CAP in Children
Which diagnostic laboratory and imaging tests should be used in a child with suspected CAP in an outpatient setting?
Blood cultures usually are not needed in nontoxic, fully immunized children with CAP. If the child does not demonstrate clinical improvement, or if the child shows signs of clinical deterioration or a progression of symptoms after initial antibiotic therapy, then blood cultures should be obtained.
Repeat blood cultures are not needed to document resolution of pneumococcal bacteremia in children who demonstrate clear clinical improvement. If bacteremia is caused by S. aureus, repeated blood cultures should be obtained regardless of clinical status.
Although routine blood cell counts are not necessary in all children with suspected CAP in the outpatient setting, such testing may provide useful information in children with more serious illness when taken in the context of the clinical examination and other imaging and laboratory studies.
Pulse oximetry should be performed in all children with pneumonia and suspected hypoxemia; the presence of hypoxemia should determine decisions relating to site of care and further diagnostic testing.
Routine chest radiography is not necessary to confirm the presence of CAP in children and infants who are well enough to be treated in the outpatient setting, provided they have already been evaluated in the office, clinic, or emergency department setting. Posteroanterior and lateral chest radiography should be performed in any infants or children who may have or are known to have hypoxemia or significant respiratory distress (Table 1). Radiography is also indicated if an initial round of antibiotics has been ineffective in ascertaining the presence or absence of any complications associated with pneumonia, such as pneumothorax, parapneumonic effusions, and necrotizing pneumonia.
In children who recover from CAP without complications, repeat chest radiography is not usually necessary. However, it should be performed in children who do not demonstrate clinical improvement, and in children whose symptoms progress or who show signs of clinical deterioration within 48 to 72 hours of initial antibiotic therapy.
Follow-up radiography should be performed in infants and children who have complicated pneumonia with worsening respiratory distress or who are clinically unstable, or in patients with persistent fever that does not respond to therapy within 48 to 72 hours. In children and infants who have recurrent pneumonia that involves the same lobe, and in patients with collapse of the lobe during initial radiography, repeat chest radiography should be performed four to six weeks after diagnosis.
Anti-Infective Treatment
Which anti-infective therapy should be provided to a child with suspected CAP in the outpatient setting?
Because viral pathogens are responsible for most clinical disease, antimicrobial therapy is not routinely required for preschool-aged children with CAP. Amoxicillin provides appropriate coverage for Streptococcus pneumoniae, and should be used as a first-line therapy for previously healthy, appropriately immunized infants, children, and adolescents with mild to moderate CAP of suspected bacterial origin. For children who are allergic to amoxicillin, alternative agents include second- or third-generation cephalosporins (e.g., cefpodoxime, cefuroxime [Ceftin, Zinacef], cefprozil [Cefzil]), levofloxacin (Levaquin), and linezolid (Zyvox).
Physicians should also consider atypical bacterial pathogens and less common lower respiratory tract bacterial pathogens when choosing a course of management in school-aged children and adolescents. Macrolide antibiotics should be prescribed for school-aged and adolescent patients who have CAP caused by atypical pathogens. Laboratory testing for Mycoplasma pneumoniae should be performed if time permits. The preferred agent for atypical pathogens is azithromycin (Zithromax); alternatives include clarithromycin (Biaxin), erythromycin, doxycycline, levofloxacin, and moxifloxacin (Avelox).
In instances of widespread local circulation of influenza, antiviral therapy should be given to children with moderate to severe CAP consistent with influenza infection as soon as possible, especially in children whose disease is clinically worsening. Treatments should not be delayed until confirmation of positive influenza test results, because they may still provide some clinical benefit to patients with more severe illness, even after 48 hours of symptomatic infection. Influenza antiviral therapies include oseltamivir (Tamiflu), zanamivir (Relenza), amantadine, and rimantadine (Flumadine).
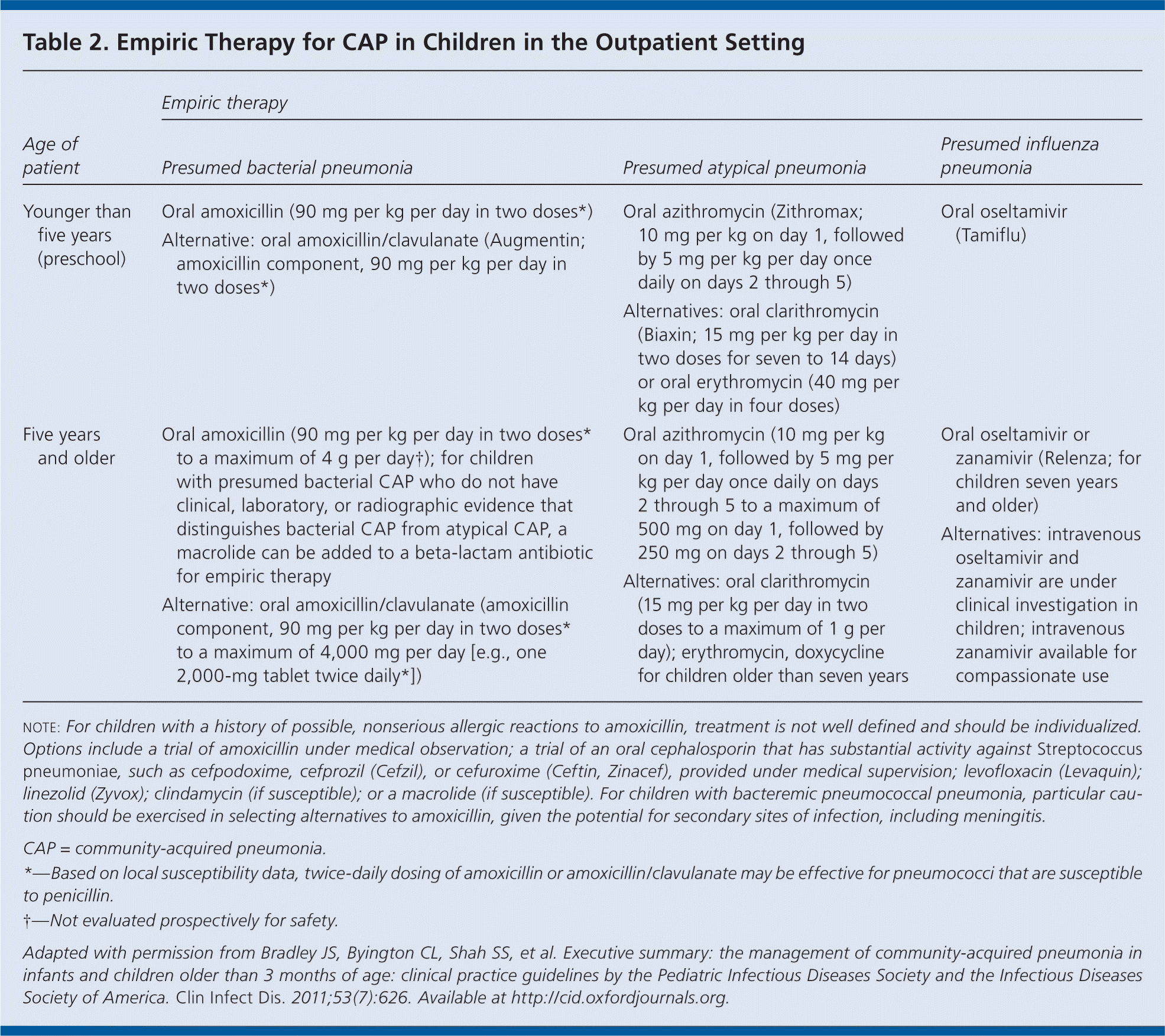
A list of preferred and alternative agents for pneumonia to be administered in the outpatient setting is provided in Table 2.
Table 2. Empiric Therapy for CAP in Children in the Outpatient Setting
| Empiric therapy | |||
|---|---|---|---|
| Age of patient | Presumed bacterial pneumonia | Presumed atypical pneumonia | Presumed influenza pneumonia |
| Younger than five years (preschool) | Oral amoxicillin (90 mg per kg per day in two doses*) | Oral azithromycin (Zithromax; 10 mg per kg on day 1, followed by 5 mg per kg per day once daily on days 2 through 5) | Oral oseltamivir (Tamiflu) |
| Alternative: oral amoxicillin/clavulanate (Augmentin; amoxicillin component, 90 mg per kg per day in two doses*) | Alternatives: oral clarithromycin (Biaxin; 15 mg per kg per day in two doses for seven to 14 days) or oral erythromycin (40 mg per kg per day in four doses) | ||
| Five years and older | Oral amoxicillin (90 mg per kg per day in two doses* to a maximum of 4 g per day†); for childrens with presumed bacterial CAP who do not have clinical, laboratory, or radiographic evidence that distinguishes bacterial CAP from atypical CAP, a macrolide can be added to a beta-lactam antibiotic for empiric therapy | Oral azithromycin (10 mg per kg on day 1, followed by 5 mg per kg per day once daily on days 2 through 5 to a maximum of 500 mg on day 1, followed by 250 mg on days 2 through 5) | Oral oseltamivir or zanamivir (Relenza; for children seven years and older) |
| Alternative: oral amoxicillin/clavulanate (amoxicillin component, 90 mg per kg per day in two doses* to a maximum of 4,000 mg per day [e.g., one 2,000-mg tablet twice daily*]) | Alternatives: oral clarithromycin (15 mg per kg per day in two doses to a maximum of 1 g per day); erythromycin, doxycycline for children older than seven years | Alternatives: intravenous oseltamivir and zanamivir are under clinical investigation in children; intravenous zanamivir available for compassionate use | |
note: For children with a history of possible, nonserious allergic reactions to amoxicillin, treatment is not well defined and should be individualized. Options include a trial of amoxicillin under medical observation; a trial of an oral cephalosporin that has substantial activity against Streptococcus pneumoniae , such as cefpodoxime, cefprozil (Cefzil), or cefuroxime (Ceftin, Zinacef), provided under medical supervision; levofloxacin (Levaquin); linezolid (Zyvox); clindamycin (if susceptible); or a macrolide (if susceptible). For children with bacteremic pneumococcal pneumonia, particular caution should be exercised in selecting alternatives to amoxicillin, given the potential for secondary sites of infection, including meningitis.
CAP = community-acquired pneumonia.
*—Based on local susceptibility data, twice-daily dosing of amoxicillin or amoxicillin/clavulanate may be effective for pneumococci that are susceptible to penicillin.
†—Not evaluated prospectively for safety.
Adapted with permission from Bradley JS, Byington CL, Shah SS, et al. Executive summary: the management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin Infect Dis. 2011;53(7):626. Available at http://cid.oxfordjournals.org.
How should the physician follow the child with CAP for the expected response to therapy?
Provided a child has received adequate therapy, he or she should show clinical and laboratory signs of improvement within 48 to 72 hours. For children whose condition deteriorates after initiation of antimicrobial therapy, or who show no improvement within 72 hours, further evaluation is needed.
Prevention
Can CAP in children be prevented?
To reduce the incidence of CAP, children should be immunized with vaccines for bacterial pathogens such as S. pneumoniae, Haemophilus influenzae type b, and pertussis. All infants six months and older, and all children and adolescents, should also receive an annual influenza virus immunization.
All parents and caretakers of infants younger than six months should be immunized with vaccines for pertussis and influenza to help protect infants from exposure to these diseases. Immunization against influenza also decreases the likelihood of pneumococcal CAP after influenza infection.
To decrease the risk of severe pneumonia and hospitalization caused by respiratory syncytial virus, high-risk infants should receive immune prophylaxis with virus-specific monoclonal antibody.

