Psychological distress is common in terminally ill persons and can be a source of great suffering. Grief is an adaptive, universal, and highly personalized response to the multiple losses that occur at the end of life. This response may be intense early on after a loss manifesting itself physically, emotionally, cognitively, behaviorally, and spiritually; however, the impact of grief on daily life generally decreases with time. Although pharmacologic interventions are not warranted for uncomplicated grief, physicians are encouraged to support patients by acknowledging their grief and encouraging the open expression of emotions. It is important for the physician to distinguish uncomplicated grief reactions from more disabling psychiatric disorders such as major depression. The symptoms of grief may overlap with those of major depression or a terminal illness or its treatment; however, grief is a distinct entity. Feelings of pervasive hopelessness, helplessness, worthlessness, guilt, lack of pleasure, and suicidal ideation are present in patients with depression, but not in those experiencing grief. Psychotherapy and antidepressant medications reduce symptoms of distress and improve quality of life for patients with depression. Physicians may consider psychostimulants, such as methylphenidate, for patients who have depression with a life expectancy of only days to weeks.
Patients, except for those who experience a sudden death, undergo some type of loss at the end of life. Initially these losses may include health, wealth, self-image, and sense of control. These losses accumulate over time and may progressively involve loss of relationships, privacy, independence, dignity, and cognitive and physical function.1,2 Grief is a universal, yet highly personalized, response to these losses, and is an expected part of living with a progressive terminal illness such as advanced cancer, congestive heart failure, or chronic obstructive pulmonary disease. Although grief may cause patients significant suffering, it is considered an adaptive and healthy reaction to loss.3
Major depression, although common in patients with terminal illnesses, is neither universal nor adaptive. Estimates of the prevalence of depression at the end of life vary widely.4–7 A meta-analysis of patients with cancer found a prevalence of major depression ranging from 5 to 30 percent, with a pooled prevalence of 14 percent.8
Depression shares some common features with grief, but they are distinct entities and must be differentiated.9 Depression may cause significant suffering,7 reduce quality of life,10 worsen physical symptoms such as pain,7 impair one's ability to find meaning in life,11 shorten survival in some illnesses,12 interfere with relationships, and cause distress to family and friends.13 Depression is also associated with worse treatment adherence,14 and increased risk of suicide and requests to hasten death.15,16 The challenge for a physician is to distinguish between normal and adaptive reactions to loss for patients living with terminal illness and the disabling diagnosis of major depression.
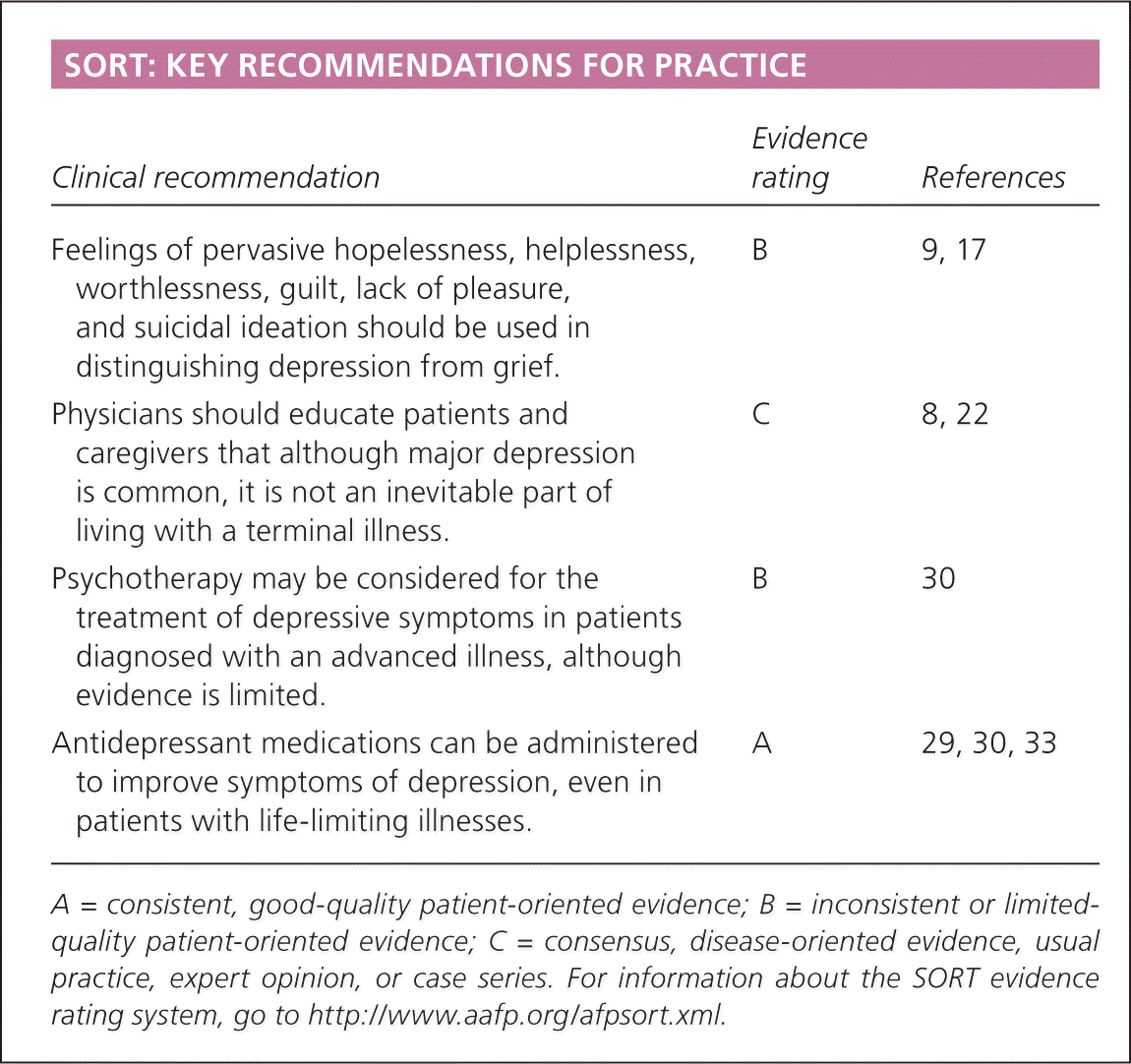
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Feelings of pervasive hopelessness, helplessness, worthlessness, guilt, lack of pleasure, and suicidal ideation should be used in distinguishing depression from grief. | B | 9, 17 |
| Physicians should educate patients and caregivers that although major depression is common, it is not an inevitable part of living with a terminal illness. | C | 8, 22 |
| Psychotherapy may be considered for the treatment of depressive symptoms in patients diagnosed with an advanced illness, although evidence is limited. | B | 30 |
| Antidepressant medications can be administered to improve symptoms of depression, even in patients with life-limiting illnesses. | A | 29, 30, 33 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Grief
Individuals experience grief physically, emotionally, cognitively, behaviorally, and spiritually. Symptoms of grief may include denial, anger, disbelief, yearning, anxiety, sadness, helplessness, guilt, sleep and appetite changes, fatigue, and social withdrawal. Persons often experience these feelings in waves that are sometimes overwhelming. This may lead to a sense of being out of control and a desire to avoid reminders of loss and illness.
For most patients, grief is an appropriate and adaptive response to loss and illness.3 Disruptions to daily life are expected, especially during the first few weeks to months following a loss, with normal daily functioning being difficult but still manageable. Grief-related distress typically diminishes over time, corresponding with an increase in acceptance of loss.
TREATMENT
Many patients who are grieving cope with their distress without involving health care professionals. Physicians can help patients who are grieving by encouraging them to use external sources of support, including family, friends, and faith communities. Physicians should acknowledge the loss and the associated grief, actively listen to and explore patients' concerns, reinforce patients' strengths in coping with their illness, and facilitate communication with loved ones.17,18 Exploring end-of-life issues is associated with improved outcomes for patients and their caregivers.19 In a prospective cohort study, patients with advanced cancer who did not report having end-of-life discussions with their physician received significantly more aggressive medical care in their last week of life, including resuscitation, ventilation, and admission to the intensive care unit.19 These types of medical care were associated with reduced patient quality of life and higher risk of major depressive disorder in bereaved caregivers. End-of-life discussions were not associated with increased emotional distress or psychiatric disorders such as depression or anxiety.19
Addressing psychosocial and existential distress through supportive–expressive group therapy and meaning-centered group psychotherapy may improve psychosocial outcomes in patients with advanced illness.20,21 Supportive–expressive group therapy encourages building bonds among the group's participants, expressing emotions, confronting existential issues, and improving the coping skills of participants. Meaning-centered group therapy uses didactics, discussion, and experiential exercises that focus on themes related to reviewing and enhancing the meaning one finds in life and in advanced illness.
Depression
A potential barrier to diagnosing and treating depression in patients who are at the end of life is the belief that depression is a universal experience in these patients. The majority of patients with advanced illness are not depressed, although they may complain of a depressed mood or other depressive symptoms.8,22 Although sadness is common in patients who are terminally ill,22,23 most persons are able to experience positive mood states in the last months of life22,24 and are able to find some pleasure in life. For a smaller subset of patients, pervasive sadness and despair occur, indicative of depression.11,22
DIAGNOSIS
Screening instruments may improve the rate of diagnosis of depression in patients with advanced illnesses. A two-item screening tool that includes questions on low mood (“Are you depressed?”) and low interest (“Have you experienced loss of interest in things or activities that you would normally enjoy?”)25 has a pooled sensitivity of 91 percent and specificity of 86 percent based on five studies of patients with cancer and those receiving palliative care.26 A positive screen using this tool is the patient answering “Yes” to both questions. The Hospital Anxiety and Depression Scale is a 14-item self-administered questionnaire that performs well in detecting symptoms of anxiety and depression in patients with physical illness.27 If initial screening is positive, physicians should perform a more detailed history and mental status examination that focuses on assessing mood, affect, cognition, and the psychological symptoms of depression, and on evaluating other potential causes or contributors to depressive symptoms (e.g., medications, pain).
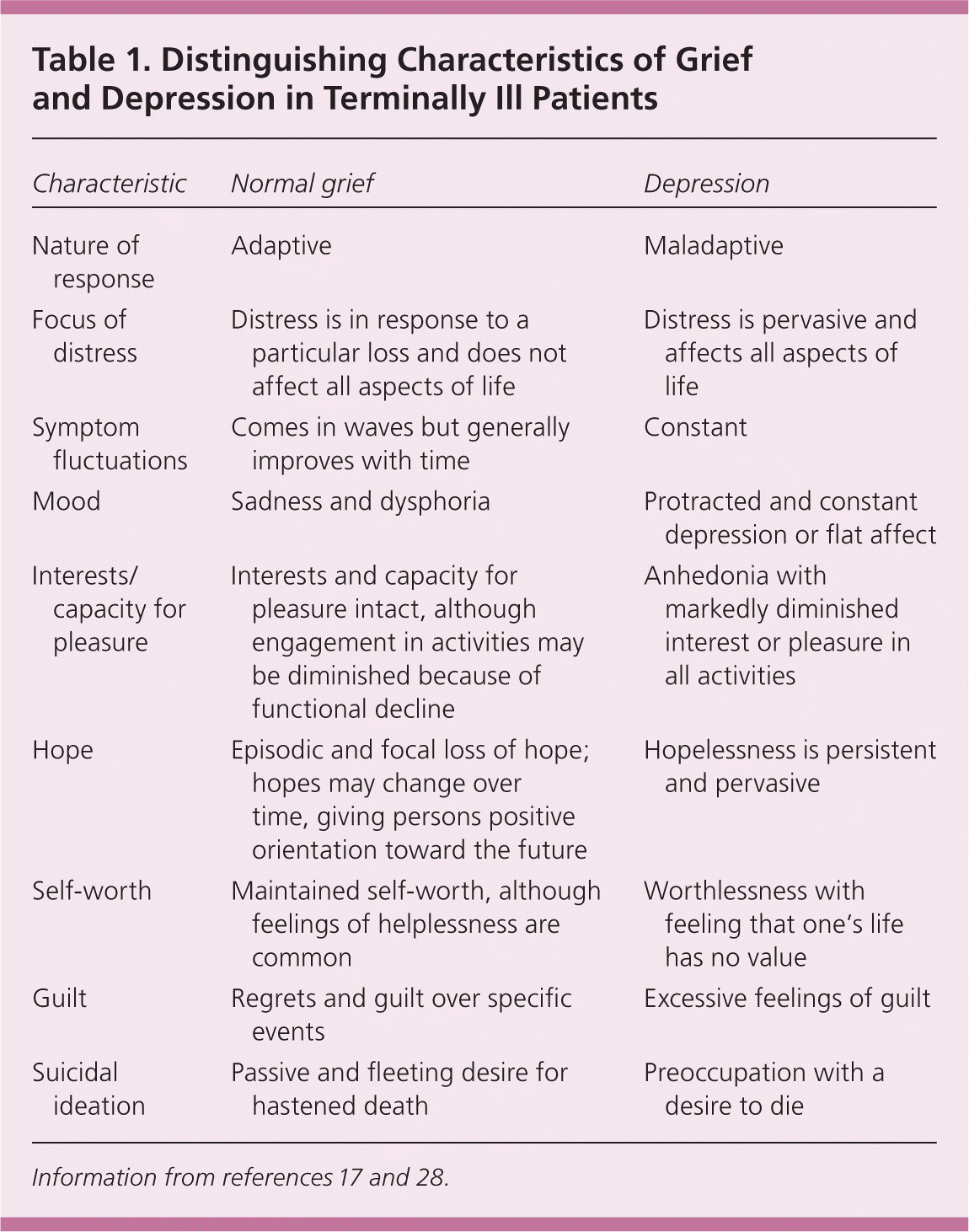
The Diagnostic and Statistical Manual of Mental Disorders, 4th ed. (DSM-IV) describes a major depressive episode as at least two weeks of depressed mood or loss of interest accompanied by at least four additional symptoms of depression (sleep disturbance; guilt and feelings of worthlessness; lack of energy; loss of concentration and difficulty making decisions; anorexia or weight loss; psychomotor agitation or retardation; and suicidal ideation). Because many of the symptoms listed in the DSM-IV criteria overlap with symptoms of a terminal illness and of grief, feelings of pervasive hopelessness, helplessness, worthlessness, guilt, lack of pleasure, and suicidal ideation are key in making a diagnosis of depression in the terminally ill patient.17 Additional features that distinguish grief from depression are listed in Table 1.17,28
Table 1. Distinguishing Characteristics of Grief and Depression in Terminally Ill Patients
| Characteristic | Normal grief | Depression |
|---|---|---|
| Nature of response | Adaptive | Maladaptive |
| Focus of distress | Distress is in response to a particular loss and does not affect all aspects of life | Distress is pervasive and affects all aspects of life |
| Symptom fluctuations | Comes in waves but generally improves with time | Constant |
| Mood | Sadness and dysphoria | Protracted and constant depression or flat affect |
| Interests/capacity for pleasure | Interests and capacity for pleasure intact, although engagement in activities may be diminished because of functional decline | Anhedonia with markedly diminished interest or pleasure in all activities |
| Hope | Episodic and focal loss of hope; hopes may change over time, giving persons positive orientation toward the future | Hopelessness is persistent and pervasive |
| Self-worth | Maintained self-worth, although feelings of helplessness are common | Worthlessness with feeling that one's life has no value |
| Guilt | Regrets and guilt over specific events | Excessive feelings of guilt |
| Suicidal ideation | Passive and fleeting desire for hastened death | Preoccupation with a desire to die |
The psychological symptoms of depression must also be seen in the context of the patient's illness. For example, guilt may be a normal reaction to an illness caused by a lifestyle choice, such as developing lung cancer after a long history of cigarette use. Depression should be considered when guilt becomes excessive or involves multiple facets of the patient's life. Additionally, feelings of helplessness may be a natural grief response to a significant loss of functional ability. When feelings of helplessness become noticeably out of proportion to the patient's actual situation, a major depressive episode is suggested.17
Physicians should consider other potential causes of or contributors to depressive symptoms. A primary concern should be the adequate control of symptoms of distress, such as poorly controlled pain. Patients with advanced illness may be receiving multiple medications associated with an increased risk of depressive symptoms. Drug and alcohol abuse, delirium or dementia, and other general medical conditions and mental health disorders may co-occur or be confused with depressive disorders.
TREATMENT
Depression tends to be undertreated in patients with advanced illness.17,29 Physicians should educate patients and caregivers that although major depression is common, it is not an inevitable part of the dying process in patients who have a terminal illness.22 In terminally ill patients with depression, psychotherapy and medications can diminish symptoms, improve quality of life, reduce stresses on family members, and may even prolong survival.
NONPHARMACOLOGIC THERAPY
Evidence from randomized controlled trials shows that psychotherapy, including cognitive behavioral therapy,30 improves symptoms in healthy adults with unipolar depression. (A review of cognitive therapy for depression appeared in the January 1, 2006, issue of American Family Physician.) Evidence is limited for the effectiveness of psychotherapy in patients with advanced illness. A meta-analysis of six randomized controlled trials of supportive-expressive group therapy, cognitive behavioral therapy, and problem-solving therapy for persons with advanced cancer concluded that psychotherapy has significant beneficial effect on the treatment of depressive symptoms.30 Caution is warranted in generalizing these data, because none of these trials focused solely on persons with clinically diagnosed depression. Complementary and alternative medicine therapies, including yoga and massage, may also be helpful, although methodologic flaws of studies examining these therapies limit any recommendations for their use.31,32
PHARMACOTHERAPY
A meta-analysis of 44 studies involving 3,372 adults with depression and physical illness revealed that selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants (TCAs) were more effective than placebo within four to five weeks of treatment.33 Limiting the population to patients with life-threatening illnesses revealed similar effectiveness in a separate meta-analysis.29 Results from these meta-analyses do not indicate the superiority of one class of antidepressants over another.29,33
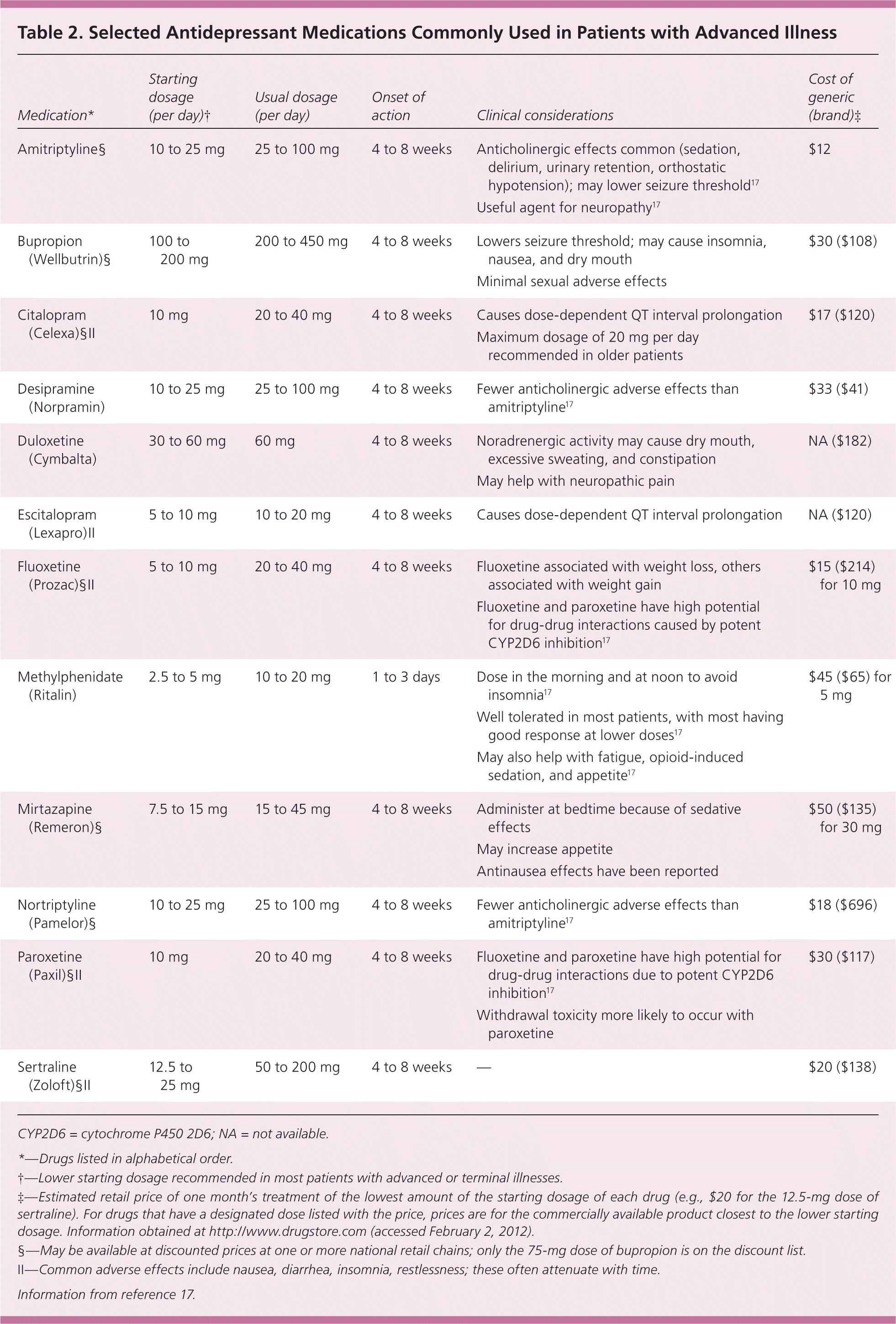
Selecting the appropriate pharmacologic agent should be based on the patient's symptoms, preferences, and likely prognosis; the antidepressant's adverse effect profile and cost; and the risk of drug-drug interactions (Table 217 ). Anticipated beneficial side effects may also help guide drug selection. For example, common side effects of mirtazapine (Remeron) include sedation and weight gain, making it a reasonable therapy to try in an individual who is distressed by insomnia and weight loss. Concomitant medications should also be considered when choosing an antidepressant, including possible effects on cytochrome P450 metabolism. For example, SSRIs such as fluoxetine (Prozac) and paroxetine (Paxil) are moderate-to-potent CYP2D6 inhibitors, and are associated with decreased tamoxifen activity.34,35
Table 2. Selected Antidepressant Medications Commonly Used in Patients with Advanced Illness
| Medication* | Starting dosage (per day)† | Usual dosage (per day) | Onset of action | Clinical considerations | Cost of generic (brand)‡ |
|---|---|---|---|---|---|
| Amitriptyline§ | 10 to 25 mg | 25 to 100 mg | 4 to 8 weeks | Anticholinergic effects common (sedation, delirium, urinary retention, orthostatic hypotension); may lower seizure threshold17 | $12 |
| Useful agent for neuropathy17 | |||||
| Bupropion (Wellbutrin)§ | 100 to 200 mg | 200 to 450 mg | 4 to 8 weeks | Lowers seizure threshold; may cause insomnia, nausea, and dry mouth | $30 ($108) |
| Minimal sexual adverse effects | |||||
| Citalopram (Celexa)§∥ | 10 mg | 20 to 40 mg | 4 to 8 weeks | Causes dose-dependent QT interval prolongation | $17 ($120) |
| Maximum dosage of 20 mg per day recommended in older patients | |||||
| Desipramine (Norpramin) | 10 to 25 mg | 25 to 100 mg | 4 to 8 weeks | Fewer anticholinergic adverse effects than amitriptyline17 | $33 ($41) |
| Duloxetine (Cymbalta) | 30 to 60 mg | 60 mg | 4 to 8 weeks | Noradrenergic activity may cause dry mouth, excessive sweating, and constipation | NA ($182) |
| May help with neuropathic pain | |||||
| Escitalopram (Lexapro)∥ | 5 to 10 mg | 10 to 20 mg | 4 to 8 weeks | Causes dose-dependent QT interval prolongation | NA ($120) |
| Fluoxetine (Prozac)§∥ | 5 to 10 mg | 20 to 40 mg | 4 to 8 weeks | Fluoxetine associated with weight loss, others associated with weight gain | $15 ($214) for 10 mg |
| Fluoxetine and paroxetine have high potential for drug-drug interactions caused by potent CYP2D6 inhibition17 | |||||
| Methylphenidate (Ritalin) | 2.5 to 5 mg | 10 to 20 mg | 1 to 3 days | Dose in the morning and at noon to avoid insomnia17 | $45 ($65) for 5 mg |
| Well tolerated in most patients, with most having good response at lower doses17 | |||||
| May also help with fatigue, opioid-induced sedation, and appetite17 | |||||
| Mirtazapine (Remeron)§ | 7.5 to 15 mg | 15 to 45 mg | 4 to 8 weeks | Administer at bedtime because of sedative effects | $50 ($135) for 30 mg |
| May increase appetite | |||||
| Antinausea effects have been reported | |||||
| Nortriptyline (Pamelor)§ | 10 to 25 mg | 25 to 100 mg | 4 to 8 weeks | Fewer anticholinergic adverse effects than amitriptyline17 | $18 ($696) |
| Paroxetine (Paxil)§|| | 10 mg | 20 to 40 mg | 4 to 8 weeks | Fluoxetine and paroxetine have high potential for drug-drug interactions due to potent CYP2D6 inhibition17 | $30 ($117) |
| Withdrawal toxicity more likely to occur with paroxetine | |||||
| Sertraline (Zoloft)§|| | 12.5 to 25 mg | 50 to 200 mg | 4 to 8 weeks | — | $20 ($138) |
CYP2D6 = cytochrome P450 2D6; NA = not available.
*—Drugs listed in alphabetical order.
†—Lower starting dosage recommended in most patients with advanced or terminal illnesses.
‡—Estimated retail price of one month's treatment of the lowest amount of the starting dosage of each drug (e.g., $20 for the 12.5-mg dose of sertraline). For drugs that have a designated dose listed with the price, prices are for the commercially available product closest to the lower starting dosage. Information obtained at http://www.drugstore.com (accessed February 2, 2012).
§—May be available at discounted prices at one or more national retail chains; only the 75-mg dose of bupropion is on the discount list.
||—Common adverse effects include nausea, diarrhea, insomnia, restlessness; these often attenuate with time.
Information from reference 17.
TCAs are effective for treating depression and pain in patients with advanced illness,29 although they are not first-line agents because of their narrow therapeutic window and common adverse effects. Anticholinergic adverse effects are especially problematic for older patients, and may include dry mouth, constipation, urinary retention, tachycardia, orthostatic hypotension, and delirium.
Serotonin-norepinephrine reuptake inhibitors, SSRIs, and TCAs all require four- to eight-week trials to evaluate effectiveness; in patients with short anticipated life expectancy, this delay in clinical effect may consign the patient to continued suffering.29,33 There is good evidence that psychostimulants reduce symptoms of depression within days, and should be considered for patients who have depression and a prognosis of only days to weeks.36–39 Methylphenidate (Ritalin) is generally well-tolerated; however, adverse effects such as restlessness, tachycardia, delirium, and insomnia may occur.38 In addition to their effects on mood, psychostimulants have other effects that may be beneficial to patients with advanced illness (Table 217 ).
When to Refer
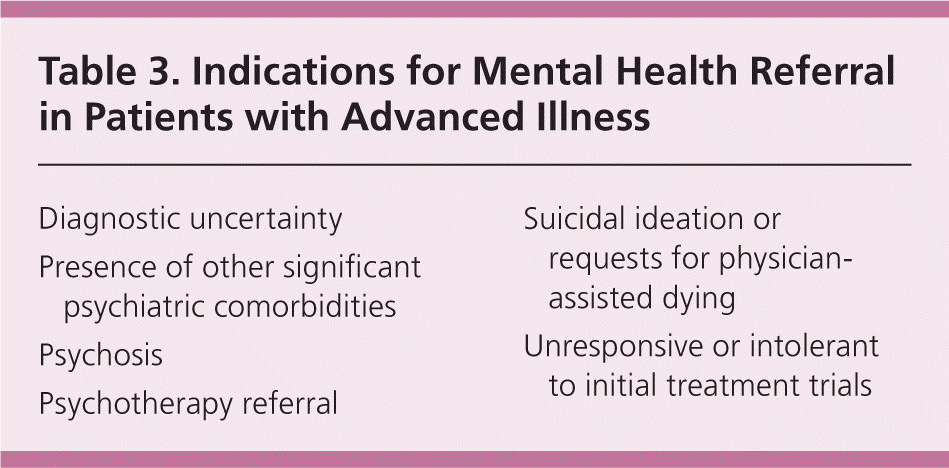
Table 3 lists common indications for mental health referral in patients with terminal illness. As with the treatment of grief, physicians should consider encouraging the use of other sources of support in the treatment of depression, including social work services or spiritual practitioners.
Table 3. Indications for Mental Health Referral in Patients with Advanced Illness
| Diagnostic uncertainty |
| Presence of other significant psychiatric comorbidities |
| Psychosis |
| Psychotherapy referral |
| Suicidal ideation or requests for physician-assisted dying |
| Unresponsive or intolerant to initial treatment trials |
Data Sources: A search was performed in MEDLINE, PsycINFO, the Cochrane database, Essential Evidence Plus, and the Agency for Healthcare Research and Quality (U.S.) Web site for peer-reviewed English-language articles from 1966 through September 2011. We cross-referenced the MeSH terms depression, depressive disorder, or grief with the MeSH terms terminal care, palliative care, hospice care, or terminally ill. There was no limitation on publication type. Further articles were identified by hand-searching references and using the related articles function in PubMed.

