Nonfebrile seizures may indicate underlying disease or epilepsy. The patient history can often distinguish epileptic seizures from nonepileptic disorders by identifying the events directly preceding the convulsion, associated conditions, and details of the seizure, including triggers, length, and type of movements. Laboratory testing, lumbar puncture, and neuroimaging may be indicated depending on the presentation, suspected etiology, and patient's age. Electroencephalography should be performed 24 to 48 hours after a first seizure because of its substantial yield and ability to predict recurrence. Neuroimaging is recommended for adults, infants, and children who have cognitive or motor developmental delay or a focal seizure. Neuroimaging may be scheduled on an outpatient basis for patients with stable vital signs who are awake and have returned to neurologic baseline. Emergent neuroimaging should be performed in patients with persistent decreased mental status or a new focal neurologic abnormality. Although magnetic resonance imaging is generally preferred to head computed tomography because of its greater sensitivity for intracranial pathology, computed tomography should be performed if intracranial bleeding is suspected because of recent head trauma, coagulopathy, or severe headache. Treatment with an antiepileptic drug after a first seizure does not prevent epilepsy in the long term, but it decreases the short-term likelihood of a second seizure. Adults with an unremarkable neurologic examination, no comorbidities, and no known structural brain disease who have returned to neurologic baseline do not need to be started on antiepileptic therapy. Treatment decisions should weigh the benefit of decreased short-term risk of recurrence against the potential adverse effects of antiepileptic drugs.
Epileptic seizures have three components: a distinct onset and offset, clinical signs, and abnormal synchronous electrical activity of the brain.1 A nonfebrile seizure may indicate underlying disease or may be the first sign of epilepsy. However, not all nonfebrile seizures are caused by epilepsy; by 85 years of age, approximately 10 percent of the population has had a nonfebrile seizure, and about 4 percent has been diagnosed with epilepsy.2 Seizure-related symptoms account for about 1 percent of all visits to emergency departments, with higher proportions among infants and young children.3 Approximately $1 billion is spent annually on prehospital and emergency seizure care in the United States.4
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Head computed tomography is recommended in the emergency setting for all patients with a first seizure. | C | 11, 24 |
| Adults who present to the emergency department after a first seizure and who have normal neurologic findings, no comorbidities, and no known structural brain disease may be discharged after they have returned to their baseline neurologic status if outpatient follow-up can be ensured. They do not need to be started on an antiepileptic drug. | C | 11 |
| Neuroimaging (preferably magnetic resonance imaging) is recommended in the outpatient setting after a first unprovoked seizure for all adults and for children with specific risk factors. | C | 26–29 |
| Serum glucose and sodium levels should be measured in all adults with a first seizure, and pregnancy testing should be performed for all women of childbearing age after a first seizure. | C | 11, 26, 31 |
| Lumbar puncture should be performed in all immunocompromised patients with a first seizure. | C | 11, 26 |
| Electroencephalography is recommended in all patients with a first unprovoked seizure, and should be performed no later than 24 to 48 hours after the event. | C | 26, 27 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Classification and Presentation
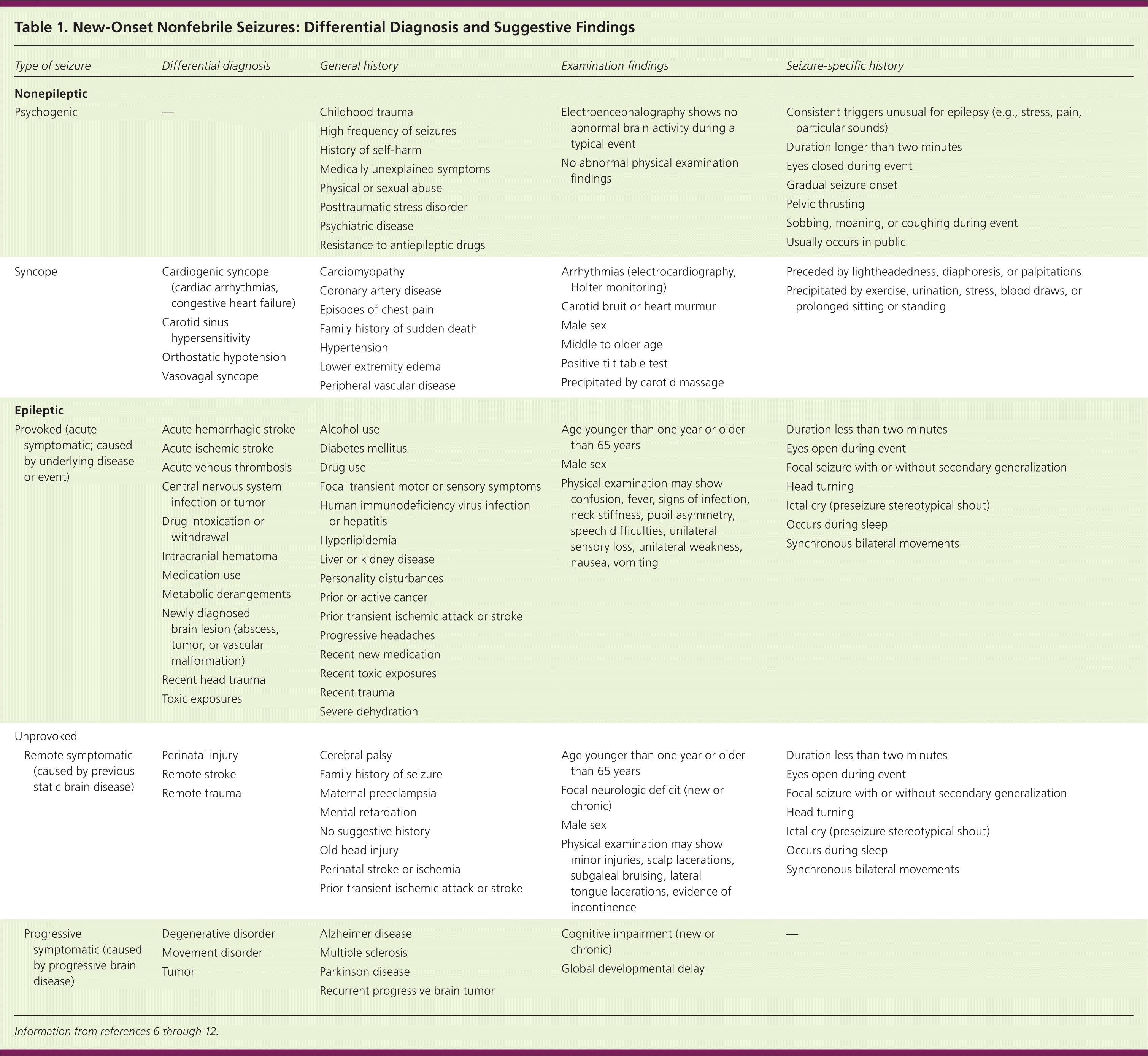
Seizures are primarily classified by the mode of onset and the propagation of electrical disturbance.5 Generalized seizures originate within and propagate throughout neuronal networks in the bilateral hemispheres of the brain. They involve loss of consciousness and may include tonic-clonic whole-body movements, atonia, and myoclonic jerking. Focal (partial) seizures originate within and propagate throughout a neuronal network limited to one hemisphere or one region of the brain. Widely variable in presentation, they may manifest as disturbances in motor, sensory, or autonomic function; emotional state; cognition; memory; or behavior. A focal seizure may progress to a generalized seizure, in which loss of consciousness occurs secondarily.5 Convulsions can be separated into three categories of differential diagnoses (Table 1).6–12
Table 1. New-Onset Nonfebrile Seizures: Differential Diagnosis and Suggestive Findings
| Type of seizure | Differential diagnosis | General history | Examination findings | Seizure-specific history | |
|---|---|---|---|---|---|
| Nonepileptic | |||||
| Psychogenic | — |
|
|
| |
| Syncope |
|
|
|
| |
| Epileptic | |||||
| Provoked (acute symptomatic; caused by underlying disease or event) |
|
|
|
| |
| Unprovoked | |||||
|
|
|
|
| |
|
|
|
|
| |
NONEPILEPTIC SEIZURES
Nonepileptic seizures present with a transient duration of symptoms, but without electrical disturbance in the brain. These include psychiatric diagnoses such as psychogenic nonepileptic seizures and panic attacks.13 About 20 percent of patients referred to epilepsy clinics may have psychogenic nonepileptic seizure.13 Red flags for this condition include resistance to several antiepileptic drugs; multiple seizures per day on most days; and comorbid depression, anxiety, or other psychiatric diagnoses. Unintended physical injury to oneself (particularly burns) is more common in patients with epileptic seizure than in those with psychogenic nonepileptic seizure.14 Objective evidence of oral lacerations (particularly on the lateral tongue) and incontinence during an event are also highly specific for epileptic seizure.15
Patients presenting with presumed nonepileptic seizures may actually have syncope of cardiac, vasovagal, or orthostatic origin.16 Syncope typically presents as a few minutes of motionless loss of consciousness, and may be preceded by lightheadedness, chest pain, palpitations, or nausea. Although brief motor jerking can occur in patients with syncope, it typically lasts only a second or two and does not resemble the synchronous 30- to 90-second tonic-clonic activity typical of epileptic seizures.6 Additionally, a large prospective study in France of 1,942 patients one month to 95 years of age showed that first seizures typically occur in younger patients (median age of 19 years), a group with a low likelihood for cardiac disease, and were usually characterized by major generalized motor symptoms,17 which would be difficult to mistake for syncopal twitching.
PROVOKED SEIZURES
Situational or provoked seizures (also called acute symptomatic seizures) are caused by an underlying disease or event (e.g., head injury, stroke, central nervous system infection or tumor, intracranial surgery, exposure to drugs or toxins, drug or alcohol withdrawal, fever) that disrupts brain circuitry or metabolic homeostasis near the time of ictus.18 Incidence is estimated at 20 to 39 cases per 100,000 person-years.19 Common underlying causes are listed in Table 1.6–12 One study found that 96.9 percent of patients with focal neurologic findings were ultimately diagnosed with an underlying acute etiology,7 confirming the importance of the physical examination in the diagnosis of acute symptomatic seizures.
UNPROVOKED SEIZURES
Unprovoked seizures occur in patients older than one month and have no acute precipitant.18 Incidence ranges from 41 to 63 cases per 100,000 person-years.19 Approximately 30 percent of unprovoked seizures may result from a remote epileptogenic brain injury (remote symptomatic seizure) or from a preexisting progressive neurologic disorder (progressive symptomatic seizure).19,20 Acute symptomatic seizures and unprovoked seizures are more common in men and in patients older than 65 years and younger than one year.19,20 Infants are predisposed to generalized seizures, and older adults to focal seizures.20
Evaluation
The patient history and physical examination should focus on events directly preceding the seizure, the number of seizures in the past 24 hours, the length and description of the seizure, focal aspects (e.g., unilateral movements, eye deviation, head turning to one side), length of the postictal period, and the neurologic examination.7,10,16 In the French prospective study mentioned earlier, history-taking showed that about one-half of patients who presented with a presumed first seizure had actually had a previous seizure, and many merited the diagnosis of epilepsy.17
Additional diagnostic studies should aim to identify emergency situations, distinguish between seizure categories, identify the etiology, and determine the risk of recurrence.
NEUROIMAGING
Computed tomography (CT) of the head has demonstrated structural lesions in about one-third of adults7 and one-half of infants younger than six months21 who present to the emergency department with a first seizure. Identification of lesions altered the acute medical or surgical management in up to 17 percent of adults22 and 8 percent of children.23 Accordingly, the American Academy of Neurology recommends considering emergent head CT for all patients with a first seizure, particularly those who have risk factors for abnormal neuroimaging (Table 2).24,25
Table 2. Risk Factors for Intracranial Pathology on Neuroimaging After a First Seizure

| Alcoholism* |
| Bleeding disorders or anticoagulation therapy |
| Focal seizure or a new focal deficit |
| History of or current cysticercosis (or recent travel to an endemic area) |
| History of stroke or malignancy |
| Human immunodeficiency virus infection/AIDS |
| Hydrocephalus or recent cerebrospinal fluid shunt surgery |
| Neurocutaneous disorders |
| Patient older than 65 years or younger than six months |
| Persistent altered mental status |
| Recent head trauma |
| Sickle cell disease |
*—An evidence-based review showed that the absence of alcohol abuse predicted abnormal neuroimaging because of the prevalence of alcohol withdrawal–related seizures.24 However, patients with alcoholism (and particularly those with a first seizure) have high rates of abnormal neuroimaging after a seizure.25 Therefore, withdrawal-related seizures should remain a diagnosis of exclusion. Information from references 24 and 25.
Head CT should be obtained to rule out life-threatening lesions in patients with persistent decreased consciousness, severe progressive headaches, or new focal neurologic deficits. Initial head CT should generally be performed without contrast media to rule out life-threatening lesions and hemorrhage that may require urgent neurosurgical intervention. CT should also be performed with contrast media in patients who have human immunodeficiency virus infection or a history of cancer to rule out an abscess or tumor.7
Because many patients with nonfocal symptoms have abnormal neuroimaging, the American College of Emergency Physicians recommends head CT for all patients who present to the emergency department with a first seizure.7,11 However, stable patients who have returned to baseline neurologic status may be discharged and scheduled for outpatient neuroimaging if follow-up can be ensured.11
Among patients who do not present to (or who are not evaluated in) the emergency department, outpatient neuroimaging after a first nonfebrile seizure is recommended for adults because of its substantial yield of detecting abnormalities that change management (10 percent).26 In children, however, it is recommended only in those younger than one year and in those with cognitive or motor developmental delay, unexplained neurologic abnormalities, a history of focal seizures, or findings on electroencephalography (EEG) that are incompatible with benign partial epilepsy of childhood or primary generalized epilepsy.27 Magnetic resonance imaging is generally the preferred imaging modality because it is more sensitive than CT at detecting intrinsic brain tumors, stroke, focal cortical dysplasia, mesial temporal sclerosis, vascular malformations, and cerebral dysgenesis.26–29 EEG and magnetic resonance imaging, combined with a clinical evaluation, may additionally lead to the diagnosis of an electroclinical syndrome.5,17,29
LABORATORY TESTS
Laboratory investigations should be tailored to the individual patient and driven primarily by findings from the history and physical examination.26,27,30 For example, a serum glucose level should be ordered for a patient with diabetes mellitus, and a comprehensive metabolic panel and ammonia level should be ordered for a patient with cirrhosis. Because an underlying seizure focus may be unmasked by the physiologic stress of pregnancy, a pregnancy test should be ordered for women of childbearing age.31 To distinguish seizures from psychogenic nonepileptic events, an elevated serum prolactin level (at least two times the baseline value) measured 10 to 20 minutes after an event is moderately sensitive and highly specific for generalized tonic-clonic seizures and focal seizures with altered consciousness.32 For healthy adult patients who have recovered and returned to their baseline neurologic status, the American College of Emergency Physicians recommends checking serum glucose and sodium levels because these are common disturbances that may be present in the absence of any other findings.11,31
LUMBAR PUNCTURE
Lumbar puncture is not routinely indicated after a first seizure, but should be performed if there is concern about central nervous system infection after obtaining negative head CT results.26,27 Infection should be suspected in patients with fever, meningeal signs, lethargy, toxic appearance, and persistent confusion, and in immunocompromised patients with or without other signs or symptoms.7,11,33 In patients with severe, persistent, thunderclap headaches that are different from usual headaches, lumbar puncture should be performed if head CT results are negative to rule out aneurysmal subarachnoid hemorrhage, which requires urgent neurosurgical intervention.
ELECTROENCEPHALOGRAPHY
EEG should be performed in all patients with suspected seizures of unknown etiology (e.g., unprovoked seizures).26,27 Epileptiform abnormalities are detected in 29 percent of adults and 59 percent of children with new-onset seizures.26,29 EEG does not generally need to be obtained in the emergency department unless there is concern about nonconvulsive status epilepticus or ongoing seizures in a pharmacologically paralyzed or comatose patient.8,31 EEG can detect focal lesions not visible with neuroimaging and show epileptiform findings that allow diagnosis of particular epilepsy syndromes.31,34 EEG-detected abnormalities may also be associated with a significantly higher risk of seizure recurrence, which may have implications for treatment.35,36 Ideally, EEG should be obtained 24 to 48 hours after the seizure, should be performed using hyperventilation/photic stimulation, and should capture asleep and awake states because these measures increase the likelihood of detecting abnormalities.27,29,35,37 If initial EEG findings are negative and clinical suspicion for epilepsy is high, sleep-deprived EEG is beneficial. This test detects abnormalities in 21 to 35 percent of patients with initially normal EEG findings, with the highest yield in the first three days after the seizure.29,38
Prognosis
One prospective population-based study of patients with new-onset nonfebrile epileptic seizures estimated that the risk of recurrence was 65 and 76 percent at one and two years, respectively.39 Seizures caused by an acute precipitant (e.g., metabolic derangement, alcohol intoxication) were less likely to recur than those caused by remote (e.g., previous stroke, previous head trauma), progressive (e.g., tumor), or unknown causes. Patients with neurologic deficits caused by a perinatal or congenital injury had a particularly high risk of recurrence.39 A review focusing on unprovoked new-onset nonfebrile seizures found a two-year recurrence rate of 40 to 50 percent for all patients, and identified two major risk factors for recurrence: epileptiform findings on EEG, and neurologic abnormalities (e.g., focal deficits found on neurologic examination, global developmental delay, underlying neurologic disease).35 Status epilepticus (a seizure, or several seizures without an interictal return to baseline, lasting more than 30 minutes) was a possible risk factor for recurrence only when it was associated with a neurologic abnormality.35 Conversely, patients with normal EEG findings and no neurologic abnormalities at presentation have a risk of recurrence of only 20 percent at one year and 25 percent at two years.40 Of the patients who do have recurrences, most will have the second seizure within a year of the initial event, usually within the first six months.39,40
Treatment
Decisions about the use of antiepileptic drugs after a first seizure should be individualized. A randomized controlled trial of 1,443 patients with nonfebrile unprovoked seizures demonstrated little long-term difference in seizure control and quality-of-life measures among patients who received immediate versus delayed treatment with antiepileptic drugs.41 Immediate treatment increased the time to seizure recurrence and reduced the time to achieve complete seizure remission. However, 92 percent of patients with a first seizure had achieved two-year remission by the five-year follow-up in both treatment groups.
Epilepsy is characterized by at least one epileptic seizure coupled with an enduring predisposition of the brain to generate further epileptic seizures.1 Immediate treatment is warranted in patients at risk of developing epilepsy, but identifying these patients can be challenging, and a neurology consultation for certain patients may be appropriate. Patients with a first seizure who have risk factors for recurrence (e.g., abnormal EEG results) or a previous or newly diagnosed epileptogenic brain injury/lesion (e.g., arteriovenous malformation, hemorrhagic stroke, subarachnoid hemorrhage, severe traumatic brain injury, encephalitis) should probably be treated because of the increased risk of future seizures.42,43 Patients who do not meet these criteria should be counseled about the excellent long-term prognosis after a first seizure, and physicians should consider delaying pharmacologic therapy until a second seizure occurs.
In certain circumstances, treatment may be appropriate in low-risk patients after a single seizure. Considerations include the patient's type of employment and the potential for extreme social or economic distress in the event of a second seizure. For example, a pilot, professional public speaker, or primary household wage earner who is dependent on his or her ability to drive may feel that the negative consequences of a second seizure outweigh the potential adverse effects of antiepileptic therapy.
The choice of antiepileptic drug is generally directed by the type of seizure, adverse effect profile, and patient characteristics such as age, childbearing potential, and comorbidities.44 Some potential adverse effects of antiepileptic drugs include osteoporosis, neuropathy, teratogenicity, weight gain, cognitive-behavioral slowing, and drug interactions.44,45
Most states require a seizure-free period of at least six months before driving a vehicle; patients should be referred to the local motor vehicle department or the Epilepsy Foundation Web site (http://www.epilepsyfoundation.org) for information about driving restrictions.
Data Sources: References were identified through English-language searches of PubMed and ISI Web of Science using the terms first seizure, nonfebrile, differential diagnosis, evaluation, neuroimaging, EEG, recurrence, and treatment. The search included meta-analyses, prospective observational studies, retrospective clinical studies, randomized controlled trials, and reviews. Also searched were the Agency for Healthcare Research and Quality, the Cochrane database, and Essential Evidence Plus. Search dates: July 1, 2011, to September 1, 2011.


