Chronic fatigue syndrome is characterized by debilitating fatigue that is not relieved with rest and is associated with physical symptoms. The Centers for Disease Control and Prevention criteria for chronic fatigue syndrome include severe fatigue lasting longer than six months, as well as presence of at least four of the following physical symptoms: postexertional malaise; unrefreshing sleep; impaired memory or concentration; muscle pain; polyarthralgia; sore throat; tender lymph nodes; or new headaches. It is a clinical diagnosis that can be made only when other disease processes are excluded. The etiology of chronic fatigue syndrome is unclear, is likely complex, and may involve dysfunction of the immune or adrenal systems, an association with certain genetic markers, or a history of childhood trauma. Persons with chronic fatigue syndrome should be evaluated for concurrent depression, pain, and sleep disturbances. Treatment options include cognitive behavior therapy and graded exercise therapy, both of which have been shown to moderately improve fatigue levels, work and social adjustment, anxiety, and postexertional malaise. No pharmacologic or alternative medicine therapies have been proven effective.
Chronic fatigue syndrome (CFS) is a widespread problem. It is estimated that more than 2 million Americans have CFS, many of whom have not been diagnosed.1 Women are twice as likely as men to have CFS,1 and it is more common in persons older than 40 years.1,2 There is not an established racial or educational predilection.1,2 CFS is often mentally and emotionally debilitating, and persons with this diagnosis are twice as likely to be unemployed as persons with fatigue who do not meet formal criteria for CFS.3 In 2002, the estimated annual cost of lost productivity was $9.1 billion dollars in the United States.4 In addition to economic hardships, persons with CFS are more likely to report subjective functional impairment than those with chronic fatigue.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Persons with chronic fatigue should have an evaluation, including history, physical examination, and initial laboratory testing (i.e., urinalysis; complete blood count; comprehensive metabolic panel; and measurement of thyroid-stimulating hormone, C-reactive protein, and phosphorus levels). | C | 7, 8 |
| Persons diagnosed with chronic fatigue syndrome should be evaluated and treated for comorbidities, such as sleep disturbance, depression, and pain. Any comorbidity identified should be treated. | C | 7, 8 |
| Persons diagnosed with chronic fatigue syndrome should be treated with cognitive behavior therapy, graded exercise therapy, or both. Cognitive behavior therapy and graded exercise therapy have been shown to improve fatigue, work and social adjustment, anxiety, and postexertional malaise. | A | 22, 23, 26, 28, 29 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.xml.
Diagnosis
CFS is a clinical diagnosis that can be made only when other etiologies of fatigue have been excluded. Specific diagnostic criteria for CFS were developed by the Centers for Disease Control and Prevention (CDC) in 1988.5 During this time, it was theorized that viral illness was the primary etiology of CFS; therefore, the criteria focused on physical symptoms. To parallel the World Health Organization categorization of CFS as a neurologic disorder, the Oxford criteria were developed in 1991 (Table 1).6 These criteria emphasize mental fatigue over physical symptoms.6 The CDC's criteria were revised in 1994 to broaden the definition, and at this time, are the most widely accepted diagnostic criteria for CFS (Table 2).7
Table 1. Oxford Criteria for Chronic Fatigue Syndrome

| Primary symptom is fatigue | |
| Definite onset of symptoms | |
| Fatigue is severe, disabling, and affects physical and mental functioning | |
| Symptoms for at least six months and present more than 50 percent of the time | |
| Other symptoms must be present, particularly myalgia, and mood and sleep disturbances | |
| Certain patients should be excluded: | |
| Those with an established medical condition known to produce chronic fatigue | |
| Those with a current diagnosis of schizophrenia, manic-depressive illness, substance abuse, eating disorder, or proven organic brain disease | |
note: All criteria must be met to make the diagnosis.
Information from reference 6.
Table 2. Centers for Disease Control and Prevention Diagnostic Criteria for Chronic Fatigue Syndrome

| Severe fatigue for longer than six months, and at least four of the following symptoms: | |
| Headache of new type, pattern, or severity | |
| Multijoint pain without swelling or erythema | |
| Muscle pain | |
| Postexertional malaise for longer than 24 hours | |
| Significant impairment in short-term memory or concentration | |
| Sore throat | |
| Tender lymph nodes | |
| Unrefreshing sleep | |
Information from reference 7.
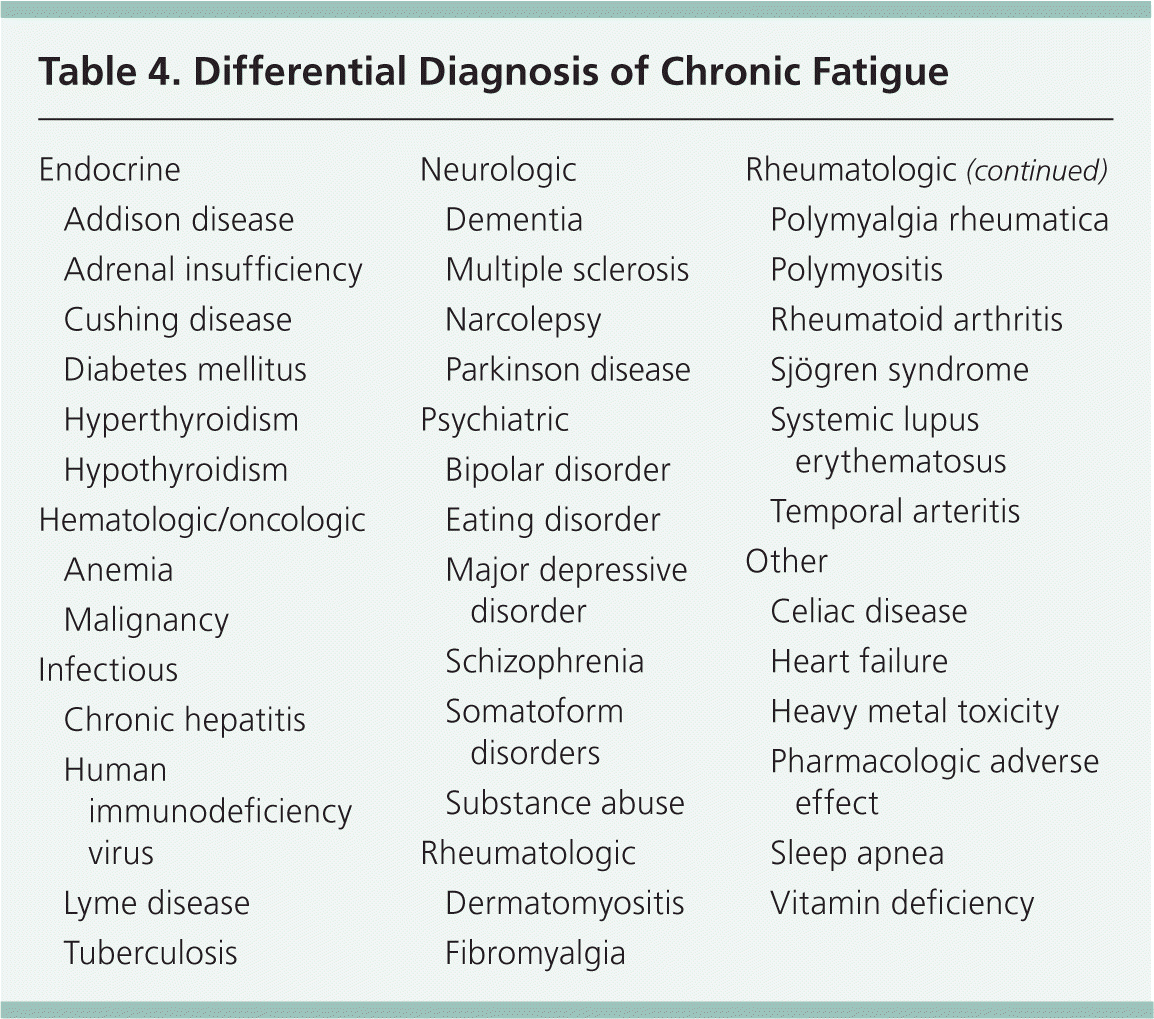
The general approach to a patient with chronic fatigue should start with a history and physical examination, focusing on identifying the most bothersome symptoms and red flag symptoms (Table 3) that may indicate a more serious underlying illness based on the National Institute for Health and Clinical Excellence (NICE) guidelines.8 Patients should have a mental status examination, including evaluation for depression, which is present in 39 to 47 percent of patients with CFS.3,9 Although the differential diagnosis for patients presenting with chronic fatigue is broad (Table 4), approximately one-third meet the criteria for CFS.3 No laboratory tests can be used to diagnose CFS; instead, they are used to rule out other causes of fatigue that would preclude the diagnosis of CFS. The CDC and NICE recommend a minimal set of tests for patients presenting with chronic fatigue.7,8
Table 3. Red Flag Symptoms in Persons with Suspected Chronic Fatigue Syndrome

| Red flags | Disease process indicated |
|---|---|
| Chest pain | Cardiac disease |
| Focal neurologic deficits | Central nervous system malignancy or abscess, multiple sclerosis |
| Inflammatory signs or joint pain | Autoimmune disease (e.g., rheumatoid arthritis, systemic lupus erythematosus) |
| Lymphadenopathy or weight loss | Malignancy |
| Shortness of breath | Pulmonary disease |
Information from reference 8.
Table 4. Differential Diagnosis of Chronic Fatigue
| Endocrine | |
| Addison disease | |
| Adrenal insufficiency | |
| Cushing disease | |
| Diabetes mellitus | |
| Hyperthyroidism | |
| Hypothyroidism | |
| Hematologic/oncologic | |
| Anemia | |
| Malignancy | |
| Infectious | |
| Chronic hepatitis | |
| Human immunodeficiency virus | |
| Lyme disease | |
| Tuberculosis | |
| Neurologic | |
| Dementia | |
| Multiple sclerosis | |
| Narcolepsy | |
| Parkinson disease | |
| Psychiatric | |
| Bipolar disorder | |
| Eating disorder | |
| Major depressive disorder | |
| Schizophrenia | |
| Somatoform disorders | |
| Substance abuse | |
| Rheumatologic | |
| Dermatomyositis | |
| Fibromyalgia | |
| Polymyalgia rheumatica | |
| Polymyositis | |
| Rheumatoid arthritis | |
| Sjögren syndrome | |
| Systemic lupus erythematosus | |
| Temporal arteritis | |
| Other | |
| Celiac disease | |
| Heart failure | |
| Heavy metal toxicity | |
| Pharmacologic adverse effect | |
| Sleep apnea | |
| Vitamin deficiency | |
The CDC recommends initial evaluation with urinalysis; complete blood count; comprehensive metabolic panel; and measurement of phosphorus, thyroid-stimulating hormone, and C-reactive protein.7 NICE also recommends using immunoglobulin A endomysial antibodies to screen for celiac disease, and if indicated by the history or physical examination, urine drug screening, rheumatoid factor testing, and antinuclear antibody testing.8 Viral titers are not recommended unless the patient's history is suggestive of an infectious process, because they do not confirm or eliminate the diagnosis of CFS.
Etiology
The etiology of CFS is unclear and is likely complex. It remains controversial whether there is a single etiology for CFS; there may be several poorly understood subsets of the illness, or there may be multiple factors that interact with each other. These complex factors, along with the numerous psychiatric comorbidities of CFS, have led some experts to question whether any organic etiology exists. Current research on CFS focuses on the immune and adrenal systems, genetics, the biopsychosocial model, and sleep and nutrition.
IMMUNE SYSTEM
Because many symptoms of viral infections and CFS overlap, some physicians have theorized that CFS has a postinfectious etiology. One popular theory is that CFS is caused by chronic Epstein-Barr virus infection; however, there is only mixed evidence of any association between specific viruses and CFS.10
GENETICS
Increasing evidence points to areas of genetic susceptibility in patients with CFS. One study found a difference in the expression of certain genes in patients with CFS after exercise that play a role in metabolism and immune responses.11 Another study has shown an association between specific genetic mutations, CFS, and certain viral infections that have been linked to CFS.12
BIOPSYCHOSOCIAL MODEL
CFS is often associated with depression, which has led many physicians to believe that CFS is a purely somatic illness. Evidence supporting this conclusion is lacking. Strong evidence suggests that childhood trauma increases the risk of CFS by as much as sixfold. Some persons may assume that childhood trauma decreases resiliency, but there is evidence to suggest that it may also play an organic role by increasing the risk of adrenal system dysfunction.13 It is important to note that social support systems for persons with CFS tend to be less reliable than for those who are healthy.14 Treatment for CFS is less likely to succeed in persons with poor social adjustment.15
ADRENAL SYSTEM
Hypocortisolism has been noted in persons with CFS; one study found cortisol levels in patients with CFS were about 5 mcg per dL (137.94 nmol per L) less than the levels in patients without CFS.16 This is likely secondary to impaired adrenal cortex responsiveness to adrenocorticotropic hormones and not to hypothalamopituitary dysfunction.17 It is unclear if such dysfunction is caused by infection, genetics, childhood trauma, unknown factors, or some combination of these.
SLEEP AND NUTRITION
There is an association between delayed dim light melatonin onset and CFS, suggesting that delayed circadian rhythm could contribute to CFS.18 Although melatonin is available over the counter for delayed dim light melatonin onset in the United States, there is no evidence for improvement in CFS with melatonin.18,19
One study has shown that persons with CFS have lower ratios of omega-3 to omega-6 unsaturated fatty acids and lower zinc levels than healthy patients.20 However, studies of nutritional supplementation in those with CFS have shown no benefit.21
Treatment
Family physicians should focus initially on management of symptoms that are often comorbid with CFS, including sleep disturbances, depression, and pain. Any comorbidity identified should be treated.7,8 Patients should be encouraged to take rest periods as necessary, and to practice relaxation techniques. Although there is no evidence these modalities are effective, they are unlikely to be harmful and may be helpful.8 There is substantial evidence for two treatments for CFS: cognitive behavior therapy (CBT) and graded exercise therapy. There is less clear evidence regarding the benefit of drug therapy for CFS in patients without comorbid depression or anxiety disorders.
COGNITIVE BEHAVIOR THERAPY
Trained psychotherapists providing CBT emphasize the role of thinking and its impact on how persons feel and act. They can help persons with CFS recognize how their fears of activity lead to behaviors that ultimately cause them to feel more fatigued and disabled. A large randomized controlled trial in adults with CFS confirmed that CBT has positive effects on fatigue levels, work and social adjustment, depression, anxiety, and postexertional malaise. Most patients in this study rated themselves as “much” or “very much” better after completion.22
A 2008 Cochrane review also supported the use of CBT for CFS.23 Several other studies have shown similar results,24,25 including in adolescents with CFS.26 One study found fewer school absences and improvements in fatigue and overall physical functioning in adolescents being treated with Internet-based CBT.27 CBT has been studied in group settings28 and in the form of self-guided instruction,29 with questionable effectiveness. Because of this, it is recommended that CBT be individualized to maximize benefit.8 Disadvantages of CBT include the need for expert consultation, time considerations, and cost. There are no data to suggest that CBT provided by trained family physicians is better or worse than CBT provided by psychotherapists.
EXERCISE
Graded exercise therapy involves a gradual increase in physical activity in the hopes of increasing function. A randomized trial found that graded exercise therapy was as effective as CBT for fatigue and the other aspects of functional impairment mentioned previously, except depression.22 Participants in this trial were encouraged to gradually increase the duration of their physical activity over 52 weeks to a final goal of 30 minutes of light exercise five days per week, taking caution not to exceed a target heart rate to avoid overexertion. Most patients chose to walk for exercise. Once this goal was achieved, the patients worked with the supervising physiotherapists monthly to increase the intensity of their aerobic exercise.
Several other studies have found consistent results.30–32 There is some evidence that the benefits of graded exercise therapy do not correlate with increases in exercise capacity, suggesting that the benefits of graded exercise therapy, like CBT, have more to do with decreasing symptom-focusing behavior in persons with CFS.33 Impediments to graded exercise therapy include time considerations and concerns from patients that exercise will exacerbate their condition.
OTHER NONPHARMACOLOGIC TREATMENTS
One study has shown that an educational intervention known as pragmatic rehabilitation provided by specially trained nurses improves fatigue in persons with CFS; however, the improvement did not persist after 70 weeks. The intervention included education about CFS, followed by a negotiated treatment plan of gradually increased activity.34 Although pragmatic rehabilitation is appealing because it avoids the need for expert consultation, more evidence is needed to determine if its effectiveness can be sustained.
Despite the positive results with CBT and graded exercise therapy, the effects are usually moderate and rarely lead to resolution of CFS. Patients with poor social adjustment, a strong belief in an organic cause for fatigue, or some sort of sickness benefit (i.e., financial incentive) tend to have worse responses to therapy.15,35 Unlike with many other illnesses, membership in a CFS support group was associated with worse outcomes.35
Other treatments that did not improve CFS symptoms in clinical trials include homeopathic treatments36 and multivitamins.21
PHARMACOLOGIC THERAPY
Several pharmacologic treatments for CFS have had disappointing results in clinical trials, with weak effects of questionable clinical significance or no evidence of benefit at all. There is no good evidence to support the use of antiviral medications, hydrocortisone, or fludrocortisone; only small or poorly designed studies exist.17,37,38
One study showed some clinical improvement in CFS after treatment with staphylococcus toxoid; the authors theorized that the treatment stimulated the hypoactive immune systems of persons with CFS and subsequently improved their fatigue. However, the treatment needed to be continued to prevent relapse of symptoms. Staphylococcus toxoid is not widely available and cannot currently be recommended as a treatment for CFS.39
Other treatments that did not improve CFS symptoms in clinical trials include methylphenidate,40 melatonin,19 citalopram (Celexa; used in patients without depression),41 and galantamine (Razadyne).42 More research is needed to clarify the etiology of CFS to better target potential treatments.
Data Sources: A PubMed search was completed using the MeSH term chronic fatigue syndrome. The search included randomized controlled trials and clinical trials in English from the past 10 years. We also searched the Cochrane database, Essential Evidence Plus, the National Institute for Health and Clinical Excellence guidelines, and the Centers for Disease Control and Prevention Web site. Search date: August 26, 2011.

