In 2011, through regular surveillance of more than 100 English-language research journals, a group of seven clinicians identified approximately 250 studies with the potential to improve the practice of primary care physicians and the outcomes of patients (designated as POEMs [patient-oriented evidence that matters]). Using a validated tool, Canadian primary care physicians have been rating the relevance of each POEM as they receive it in their e-mail. This article summarizes 20 of the most relevant, practice-changing POEMs from 2011 as determined by these raters. We believe this approach has greater relevance and validity than a subjective list of studies selected by experts or editors, because it is based on the actual ratings of practicing primary care physicians. These POEMs address topics that include how to best measure blood pressure, the lack of benefit of intensive glucose control, quantification of the benefit of statins for prevention of cardiac events, treatments for functional abdominal disorders, and management of low back pain.
Each year, a selection of 100 of the most widely read English-language research journals publish more than 20,000 articles.1 “Information mastery” is a framework for evaluating the usefulness of medical information.2 Based on this framework, the information deemed most useful is highly relevant (leading to improved patient outcomes), highly valid (the study was well-designed and without important biases), and takes little work to access (someone has summarized the results of the study). Studies that meet these criteria and have the potential to change practice are called POEMs, or patient-oriented evidence that matters.2 The term “patient-oriented” refers to outcomes that are important to patients, such as decreased morbidity and mortality, and improved quality of life, rather than disease-oriented outcomes, such as changes in physiologic variables like serum glucose levels, glomerular filtration rate, and electrocardiographic findings.
Every month, a team of seven clinicians with expertise in primary care, hospital medicine, women's health, and pharmacology reviews 110 English-language research journals to identify relevant POEMs for primary care physicians. In 2011, approximately 250 studies met the criteria to be designated as a POEM; these studies were summarized in brief, structured critical appraisals. The POEMs are e-mailed to subscribers, and members of the Canadian Medical Association can rate the usefulness and impact of each POEM using a validated tool called the Information Assessment Method.3 From the physicians' ratings, a clinical relevance of information index was developed to identify the relevance of POEMs. The index, which ranges from 0 to 1, is based on the proportion of “totally relevant” and “not relevant” ratings. It also takes into account the total number of responses. The clinical relevance of information index was used to identify an initial list of the top 30 POEMs. POEMs were then excluded if they described a practice guideline rather than an original research study; received fewer than 300 physician ratings; or the editors believed they did not provide clear impetus for practice change.
In the final list of the top 20 POEMs, at least 55 percent of raters identified each POEM as “totally relevant” and less than 21 percent rated each as “not relevant.” This article provides the clinical question and bottom-line answer for each of the POEMs, organized by topic and followed by a brief discussion. Although many journals publish a list of the top studies from the previous year, we believe this approach has greater relevance and validity than a subjective list of studies selected by experts or editors because it is based on the actual ratings of practicing primary care physicians.
Cardiovascular Disease
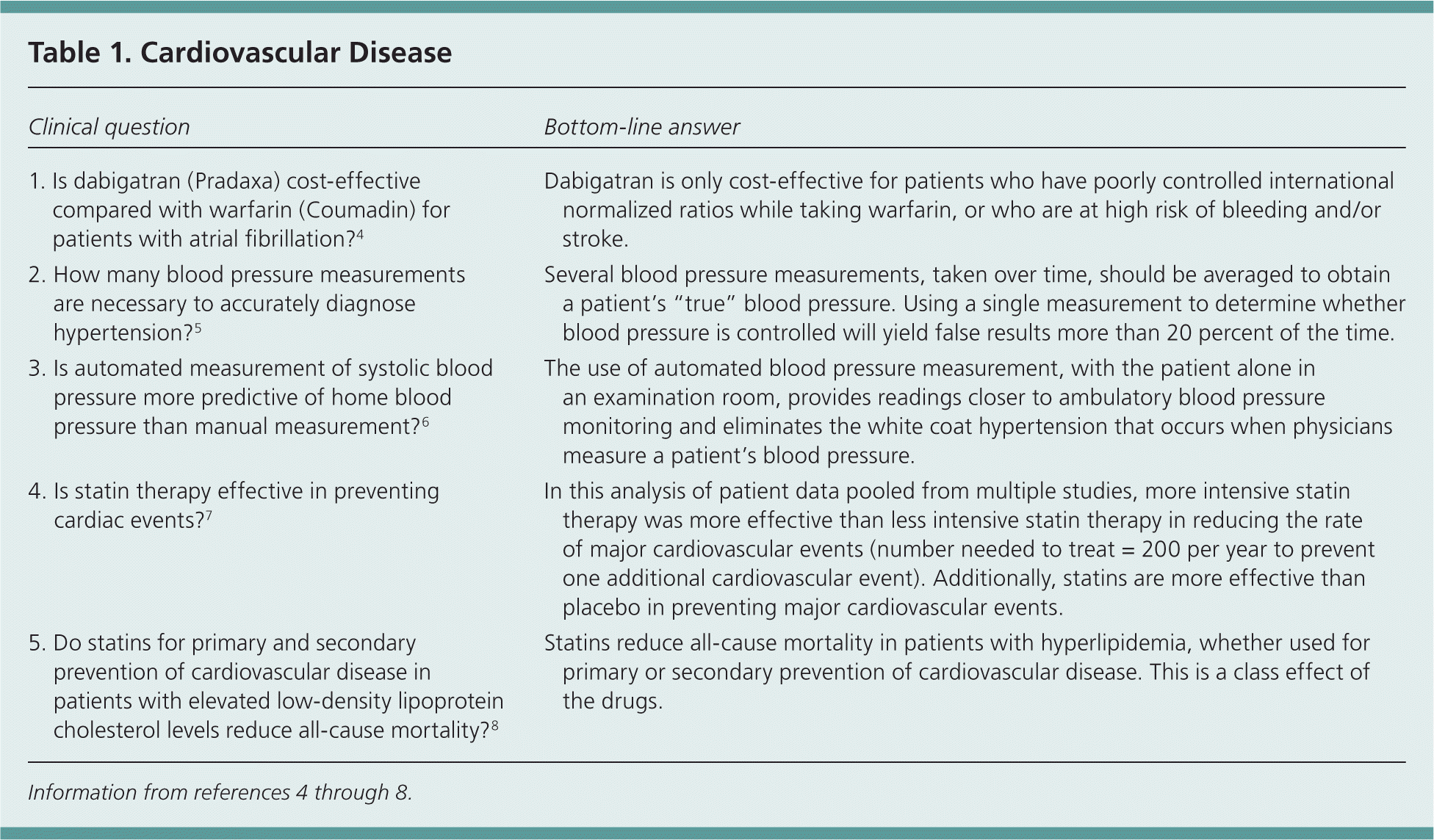
Table 1. Cardiovascular Disease
| Clinical question | Bottom-line answer |
|---|---|
| 1. Is dabigatran (Pradaxa) cost-effective compared with warfarin (Coumadin) for patients with atrial fibrillation?4 | Dabigatran is only cost-effective for patients who have poorly controlled international normalized ratios while taking warfarin, or who are at high risk of bleeding and/or stroke. [See full POEM] |
| 2. How many blood pressure measurements are necessary to accurately diagnose hypertension?5 | Several blood pressure measurements, taken over time, should be averaged to obtain a patient's “true” blood pressure. Using a single measurement to determine whether blood pressure is controlled will yield false results more than 20 percent of the time. [See full POEM] |
| 3. Is automated measurement of systolic blood pressure more predictive of home blood pressure than manual measurement?6 | The use of automated blood pressure measurement, with the patient alone in an examination room, provides readings closer to ambulatory blood pressure monitoring and eliminates the white coat hypertension that occurs when physicians measure a patient's blood pressure. [See full POEM] |
| 4. Is statin therapy effective in preventing cardiac events?7 | In this analysis of patient data pooled from multiple studies, more intensive statin therapy was more effective than less intensive statin therapy in reducing the rate of major cardiovascular events (number needed to treat = 200 per year to prevent one additional cardiovascular event). Additionally, statins are more effective than placebo in preventing major cardiovascular events. [See full POEM] |
| 5. Do statins for primary and secondary prevention of cardiovascular disease in patients with elevated low-density lipoprotein cholesterol levels reduce all-cause mortality?8 | Statins reduce all-cause mortality in patients with hyperlipidemia, whether used for primary or secondary prevention of cardiovascular disease. This is a class effect of the drugs. [See full POEM] |
The new oral anticoagulants, such as dabigatran (Pradaxa), are more convenient, but can cost up to $300 per month. Study 1 (Table 14–8 ) found that, for the average patient, dabigatran costs $86,000 for each additional quality-adjusted life-year gained.4 The researchers provide a useful diagram, available at http://circ.ahajournals.org/content/123/22/2562/F3.expansion.html, that helps clinicians identify the patients in whom the new drug is most cost-effective, based on the calculated risks of stroke and hemorrhage and time spent in the therapeutic international normalized ratio range.4
Studies 2 and 3 address one of the most common tasks performed in primary care: blood pressure measurement.5,6 Study 2, which evaluated 444 men with hypertension who had a total of more than 100,000 blood pressure measurements over several years, found that each patient's measurements vary significantly. The most reliable way to establish a patient's blood pressure is to take several measurements over several weeks and average them.5 Study 3 found that in the office setting, using an automated blood pressure cuff more closely approximates ambulatory blood pressure monitoring than manual measurement (2.3 mm higher versus 6.5 mm higher), especially compared with measurements when the physician is in the room.6
Studies 4 and 5 provide some of the best evidence regarding the benefits of statins.7,8 Study 4 pooled individual patient data from 26 studies and found that in patients with known cardiovascular disease, more intensive statin therapy was slightly more effective than less intensive therapy (number needed to treat [NNT] = 200 per year to prevent one additional cardiovascular event). However, all of the studies used fixed doses of statins, rather than aiming for specific low-density lipoprotein cholesterol targets, as is typically done in clinical practice. In the 14 placebo-controlled trials (including a mix of patients with and without preexisting cardiovascular disease), the NNT to prevent one cardiovascular event was 125 per year.7 Study 5 combined data from 76 trials with 170,255 patients and found that all-cause mortality was lower in patients taking a statin compared with patients taking placebo (NNT = 67 to prevent one death over approximately three years).8 Neither study found any difference between different types of statins.7,8
Musculoskeletal Disease
Table 2. Musculoskeletal Disease

| Clinical question | Bottom-line answer |
|---|---|
| 6. When should diagnostic imaging be used for patients with low back pain?9 | Routine imaging for patients with low back pain is not warranted, and is associated with increased cost, poorer health in recipients, increased risk of surgery, and no reduction in anxiety. Indications for imaging are few, but include major risk factors for cancer, signs of cauda equina syndrome, suspected infection, and severe neurologic deficits. Radiography should be performed after a trial of therapy in patients with weak risk factors for cancer, in young patients with signs of ankylosing spondylitis, and in older patients with risk factors for vertebral fracture. Magnetic resonance imaging should be limited to patients with radiculopathy or symptoms of spinal stenosis that do not respond to therapy. [See full POEM] |
| 7. Can massage improve disability and decrease symptoms in patients with chronic low back pain?10 | Weekly massage (a general relaxation massage or one aimed specifically at addressing musculoskeletal contributions to low back pain) for 10 weeks produces a clinically meaningful reduction in dysfunction and symptoms compared with usual care. The beneficial effect diminshes, but functional improvement persists for up to one year after the start of treatment. [See full POEM] |
| 8. Do oral bisphosphonates increase the risk of atypical hip and femur fractures in postmenopausal women?11 | Oral bisphosphonate use for longer than five years is associated with a significantly increased risk of atypical hip and femur fractures (subtrochanteric or femoral shaft). |
| A previous study found little, if any, benefit of extended bisphosphonate use beyond five years in reducing the risk of typical fractures of the femoral neck or intertrochanteric region.12 Although this study design (case-control) is classified as weak evidence, it may be the best available for some time. Thus, clinicians should consider stopping bisphosphonates for most women after five years, except in those at high risk of fracture (e.g., those taking steroids long term). [See full POEM] |
Study 6 (Table 29–12 ) summarizes several systematic reviews of the evaluation of back pain. Routine imaging actually increases the risk of surgery, and does not decrease patient anxiety. The indications for imaging are limited to patients at high risk of a serious underlying cause, such as infection, cancer, or cauda equina syndrome, and to those with severe radicular pain.9
Study 7 randomized 401 patients with chronic back pain to massage or usual care and found that weekly massage provides persistent improvement in pain and function.10 Study 8 found a small increase in the risk of femoral neck or intertrochanteric fracture in women who took bisphosphonates for longer than five years. Because other studies have not shown a clear benefit to treatment for longer than five years, the study authors suggest discontinuing the drugs at that point for most women.11
Diabetes Mellitus
Table 3. Diabetes Mellitus

| Clinical question | Bottom-line answer |
|---|---|
| 9. Does intensive glucose control in patients with type 2 diabetes improve outcomes more than usual glucose control?16 | This follow-up of the ACCORD (Action to Control Cardiovascular Risk in Diabetes) study confirms the initial findings that the best target for A1C in middle-aged or older patients with cardiovascular risk factors is between 7.0 and 7.9 percent. [See full POEM] |
| 10. Does intensive glucose control in patients with type 2 diabetes decrease the risk of death or sequelae of diabetes?17 | This meta-analysis, which combined the results of 13 trials with more than 34,500 patients, found no benefit to attempting intensive glucose control in adults with type 2 diabetes, with the exception of a decrease in the likelihood of nonfatal myocardial infarction (but not cardiovascular mortality). The more studies that accumulate, the less benefit is shown with intensive glucose control. [See full POEM] |
| 11. For patients at high cardiovascular risk, can dietary counseling on a Mediterranean-type diet decrease the incidence of type 2 diabetes?18 | Extensive and ongoing dietary counseling about a Mediterranean-type diet (including a high consumption of vegetables, legumes, nuts, and olive oil, and a low consumption of meat and dairy products) decreased the incidence of diabetes compared with counseling about a low-fat diet over four years in patients with three or more cardiovascular risk factors. The patients in this study were also supported with large quantities of free olive oil or mixed nuts. [See full POEM] |
Several large, well-designed randomized trials found no benefit to intensive glucose control (e.g., A1C target less than 6.5 percent) in middle-aged patients with type 2 diabetes.13–15 Studies 9 and 10 (Table 316–18 ) confirm these findings.16,17 Study 9 was a five-year follow-up of the ACCORD (Action to Control Cardiovascular Risk in Diabetes) study that found persistent elevation in all-cause mortality in persons randomized to intensive glucose control.16 Study 10 combined the results of 13 trials with more than 34,500 patients and found no improvement in all-cause mortality or cardiovascular death with intensive glucose control; the only benefit was a small reduction in the likelihood of nonfatal myocardial infarction.17
Preventing diabetes is obviously the best strategy. Study 11 randomized patients to dietary counseling about a Mediterranean-type diet, supported with free mixed nuts and olive oil, or to counseling about a low-fat diet. After four years, patients on a Mediterranean-type diet were less likely to develop diabetes (10 versus 18 percent; NNT = 12).18
Gastrointestinal Disease
Table 4. Gastrointestinal Disease

| Clinical question | Bottom-line answer |
|---|---|
| 12. Which patients with normal upper endoscopic findings and no evidence of Helicobacter pylori infection are likely to benefit from a proton pump inhibitor?19 | Among patients with dyspepsia who have no evidence of H. pylori infection and normal endoscopic findings, approximately one-half of those who are overweight or obese, and one-fifth of those who are not, will respond to a proton pump inhibitor. [See full POEM] |
| 13. Can probiotic treatment decrease the symptoms of irritable bowel syndrome?20 | The probiotic Bifidobacterium bifidum MIMBb75 is a normal gastrointestinal tract inhabitant (with several hundred other commensal organisms). This strain, found in some probiotic formulations, decreases overall symptoms in patients with irritable bowel syndrome and is an inexpensive and safe alternative to medications. [See full POEM] |
| 14. Are dried plums (prunes) as effective as psyllium (Metamucil) for the treatment of chronic constipation in adults?21 | Prunes are at least as effective as treatment with the bulk laxative psyllium in patients with chronic constipation. Bowel movement frequency will double with six prunes eaten twice per day, with improvements in stool consistency and constipation symptoms. Prunes are calorie dense; a dozen contain approximately 260 calories, though the glycemic index is low. [See full POEM] |
Functional abdominal problems can be frustrating to manage, but several new POEMs provide some useful insights. Study 12 (Table 419–21 ) identified patients with normal upper endoscopic findings and no evidence of Helicobacter pylori infection. Those randomized to receive a proton pump inhibitor instead of placebo were more likely to have a significant improvement in symptoms (36 versus 6 percent), but primarily if they had a body mass index greater than 25 kg per m2 (53 percent response rate).19
Study 13 randomized 132 adults with mild to moderate irritable bowel syndrome to receive a probiotic or placebo, and found that those taking the probiotic were more likely to have a clinically significant response (57 versus 21 percent; NNT = 3).20 Study 14 found that although consuming whole prunes leads to a significant improvement in constipation, a person would have to eat about 12 (260 calories worth) per day to benefit.21
Screening and Prevention
Table 5. Screening and Prevention

| Clinical question | Bottom-line answer |
|---|---|
| 15. Does asking about suicidal ideation increase a patient's feelings that life is not worth living?22 | Asking about suicide—even asking six questions on the topic—does not increase thoughts that life is not worth living in persons with depression. [See full POEM] |
| 16. Does varenicline (Chantix) increase the risk of serious adverse cardiovascular events?23 | In 14 clinical trials, varenicline increased the risk of adverse cardiovascular events. The relative risk was 1.72, which, if applied to a patient with known heart disease, results in a number needed to harm of 28 (95% confidence interval, 13 to 213). [See full POEM] |
| 17. Do patients who are obese and frail benefit most from exercise, weight loss, or both?24 | A combination of exercise and weight loss will provide the most improvements in physical performance and weight loss in older persons who are obese and frail. [See full POEM] |
Study 15 (Table 522–24 ) reassures physicians that asking about suicidal ideation does not “plant the thought” in patients with depression. The researchers randomized 443 patients with depression to either be asked six questions about suicidal thoughts and ideas, or six questions about health and lifestyle in general. At a follow-up visit, there was no difference in the proportion who had experienced suicidal ideation.22
Study 16, a meta-analysis of 14 randomized controlled trials, found that the risk of adverse cardiovascular events was significantly increased in persons taking varenicline (Chantix); however, most studies excluded persons with known heart disease. Of course, if smokers successfully quit smoking, their risk of cardiovascular events decreases, but it does suggest that alternative approaches be considered for those with known cardiovascular disease.23
In study 17, older adults who were obese and frail were randomized to weight loss, exercise (aerobic, resistance, and flexibility), both, or usual care. Patients in all of the intervention groups had improvements on a physical performance test at the end of one year, and both weight loss groups lost about 20 lb (9 kg), with the greatest improvement occurring in the group that was randomized to both weight loss and exercise.24
Miscellaneous
Table 6. Miscellaneous

| Clinical question | Bottom-line answer |
|---|---|
| 18. Does the use of inhaled corticosteroids in typical doses increase the long-term risk of fracture?25 | The use of inhaled corticosteroids as a treatment for chronic obstructive pulmonary disease in older adults increases the fracture risk somewhat, with one harmed for every 83 treated for three years. This must be balanced against a number needed to treat of 6 per year to prevent one exacerbation. [See full POEM] |
| 19. Is dispensing a one-year supply of oral contraceptives associated with less risk of unintended pregnancy?26 | Dispensing a one-year supply of oral contraceptives to low-income women receiving family planning services is associated with a significant reduction in unplanned pregnancies and abortions compared with dispensing a one-month or three-month supply. [See full POEM] |
| 20. Is freezing more effective than treatment with salicylic acid for plantar warts?27 | Cryotherapy with liquid nitrogen was no more effective than daily pumice stone use plus salicylic acid to remove plantar warts (verrucae) in patients at least 12 years of age. The success rates in both groups were low, with only approximately one-third of patients experiencing total clearance. [See full POEM] |
Almost every treatment has harms as well as benefits. A physician's task is to make sure the likelihood of benefit outweighs the likelihood of harm for most patients most of the time. Study 18 (Table 625–27 ) is a systematic review of corticosteroid inhalers in patients with chronic obstructive pulmonary disease. Although there is a known benefit of one fewer exacerbation per year for every six persons who use an inhaler, there is also one fracture every three years for every 83 patients.25
Many physicians prescribe only three packs of oral contraceptives at a time, and some state laws even prevent prescribing more than that at a time. Study 19 linked data from the California Medicaid program to a birth registry and found that women given 12 or 13 packs of oral contraceptives were less likely to become pregnant (1.2 versus 3.3 percent) and less likely to have an abortion (0.18 versus 0.63 percent) than women receiving three packs at a time. After adjusting for potential confounders, there was still a 30 percent reduction in pregnancy and a 46 percent reduction in the likelihood of induced abortion.26
Study 20 randomized 240 adolescents and adults with a plantar wart to up to four sessions of cryotherapy (mean of 1.6 sessions) or eight weeks of daily pumice stone use plus application of salicylic acid 50%. After six months, results were identical (and unimpressive) for both groups, although patients tended to prefer the cryotherapy.27

