A 72-year-old woman presented with a painful erythematous rash on her right upper back that had developed seven days earlier. The rash spread over the next two days into her right axilla and breast (Figures 1 and 2). The lesions started as red, swollen, tender patches with clear vesicles and bullae, and then became hemorrhagic after three days. She had no fever or chills. Her medical history included hypertension and rheumatoid arthritis. She was taking enalapril (Vasotec) and prednisone.
Figure 1.
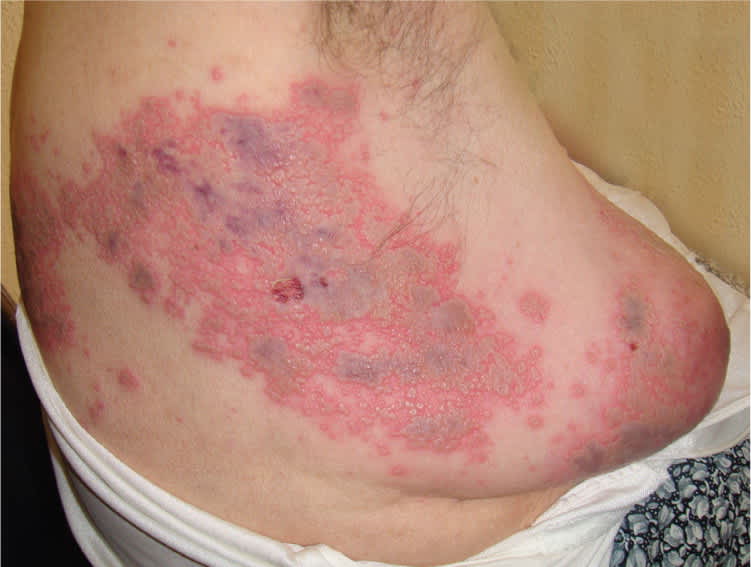
Figure 2.
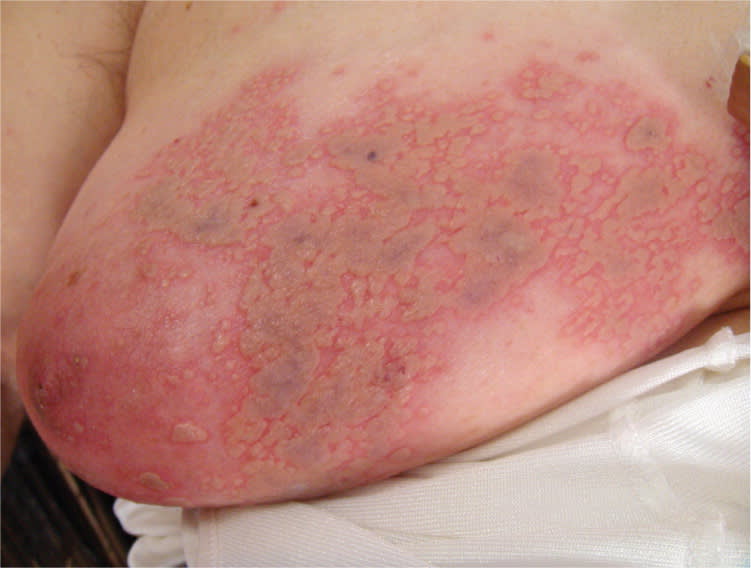
Physical examination showed vesicular lesions in a band from back to front on her right side. She was treated with amoxicillin for seven days, but the rash did not improve. After a few days, the patient reported a burning and lancinating pain in the area of the rash that was elicited with even slight pressure, such as touching clothes or bedsheets.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Herpes zoster.
B. Inflammatory breast cancer.
C. Mastitis.
D. Methicillin-resistant Staphylococcus aureus cellulitis.
Discussion
The answer is A: herpes zoster. Herpes zoster is caused by the reactivation of latent varicella virus that is dormant in nerve cell bodies. The virus spreads distally along one or several nerves, infecting the corresponding dermatome. The rash is characterized by tender vesicles and blisters, which may become hemorrhagic. Factors that decrease immune function play a role in reactivation of the virus. This patient was taking corticosteroids for rheumatoid arthritis, an important immunosuppressive factor that may have increased her risk of developing the condition.1
Herpes zoster is generally benign and self-limited. Postherpetic neuralgia (pain that persists after resolution of the rash) is the most common complication. Treatment of herpes zoster includes consideration of herpes zoster vaccine to prevent postherpetic neuralgia, as well as antivirals, tricyclic antidepressants, and anticonvulsants.
Inflammatory breast cancer leads to a red, swollen breast. The inflammation is due to the blockage of lymphatic vessels by the cancer cells. This causes slow skin changes in the breast area, such as peau d'orange, swelling, and redness. Patients may also have itching, nipple retraction, or discharge, and a chronic violaceous patch.2
Mastitis is an infection of the breast tissue that often occurs during pregnancy or breastfeeding. Symptoms typically develop quickly and may include skin redness and swelling, breast tenderness, fever, and general malaise.
Methicillin-resistant Staphylococcus aureus cellulitis is caused by staphylococcal bacteria that are resistant to methicillin and other beta-lactam antibiotics. Patients with compromised immune systems are at higher risk of infection. Cellulitis often begins after trauma, with redness, swelling, and skin that is warm to the touch. Patients quickly develop bullae and pustules, with subsequent tissue necrosis. Fever and general malaise are typically present.3
Summary Table
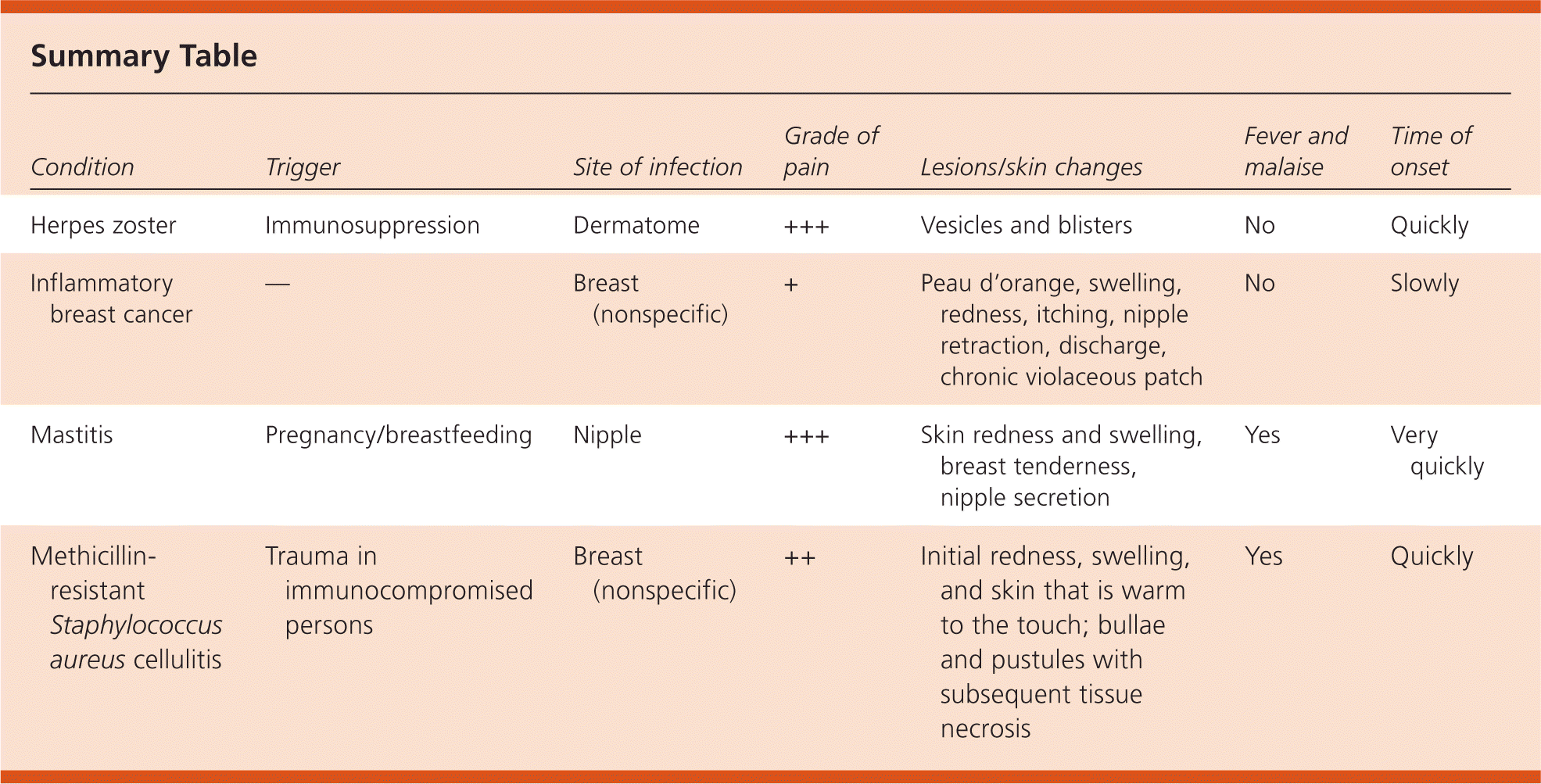
| Condition | Trigger | Site of infection | Grade of pain | Lesions/skin changes | Fever and malaise | Time of onset |
|---|---|---|---|---|---|---|
| Herpes zoster | Immunosuppression | Dermatome | +++ | Vesicles and blisters | No | Quickly |
| Inflammatory breast cancer | — | Breast (nonspecific) | + | Peau d'orange, swelling, redness, itching, nipple retraction, discharge, chronic violaceous patch | No | Slowly |
| Mastitis | Pregnancy/breastfeeding | Nipple | +++ | Skin redness and swelling, breast tenderness, nipple secretion | Yes | Very quickly |
| Methicillin-resistant Staphylococcus aureus cellulitis | Trauma in immunocompromised persons | Breast (nonspecific) | ++ | Initial redness, swelling, and skin that is warm to the touch; bullae and pustules with subsequent tissue necrosis | Yes | Quickly |

