The transgender population is a diverse group that crosses or transcends culturally defined categories of gender. The gender identity of these persons differs to varying degrees from the physical or genital sex they were assigned at birth. “Transgender” does not imply any specific form of sexual orientation; transgender persons display a range of sexual orientations similar to those who are not transgender. Transgender persons self-identify in a variety of ways, but common terms include transwoman (male to female) and transman (female to male).1
Transgender persons often seek a combination of medical, surgical, mental health, and other related treatments and services. Common treatments include cross-sex hormone therapy; genital reassignment surgery; nongenital surgical procedures of the face, breast, or body; speech and voice therapy; and facial hair removal.2 Transgender persons require ongoing primary and preventive care, in addition to transgender-specific care. Preventive care approaches are similar to those of nontransgender persons, with adjustments based on hormonal and anatomical differences, such as the need for cervical screening in transmen and breast cancer screening in transwomen.3
The World Professional Association for Transgender Health (WPATH) is an international multidisciplinary professional association that publishes recognized standards for the care of transgender and gender-variant persons. In September 2011, WPATH published the Standards of Care for the Health of Transsexual, Transgender, and Gender Nonconforming People, Seventh Version (SOC7).4 The SOC7 is more comprehensive than the prior version,5 and contains numerous updates that address changes in both the transgender community and in the practices of physicians who care for them. Although the SOC7 contains an evidence-based discussion of treatment options, adverse effects, and outcomes, specific treatment regimens (e.g., hormone dosing) are published elsewhere.3,6–9 As such, they are not presented in this guideline. Table 1 provides selected resources for transgender medical, surgical, and mental health care and cultural awareness.
The SOC7 states that primary care is an ideal setting for transgender health care, given that primary care physicians are knowledgeable of and often experienced with the administration of estrogens (for menopausal care and contraception), testosterone (for androgen deficient states such as with human immunodeficiency virus), and testosterone-blocking medications (for hirsutism and prostatic disease), and are aware of important mental and social health issues.10 This recommendation is also in line with the position statement recently released by the American College of Obstetricians and Gynecologists directing physicians to prepare themselves for the care of transgender persons.11
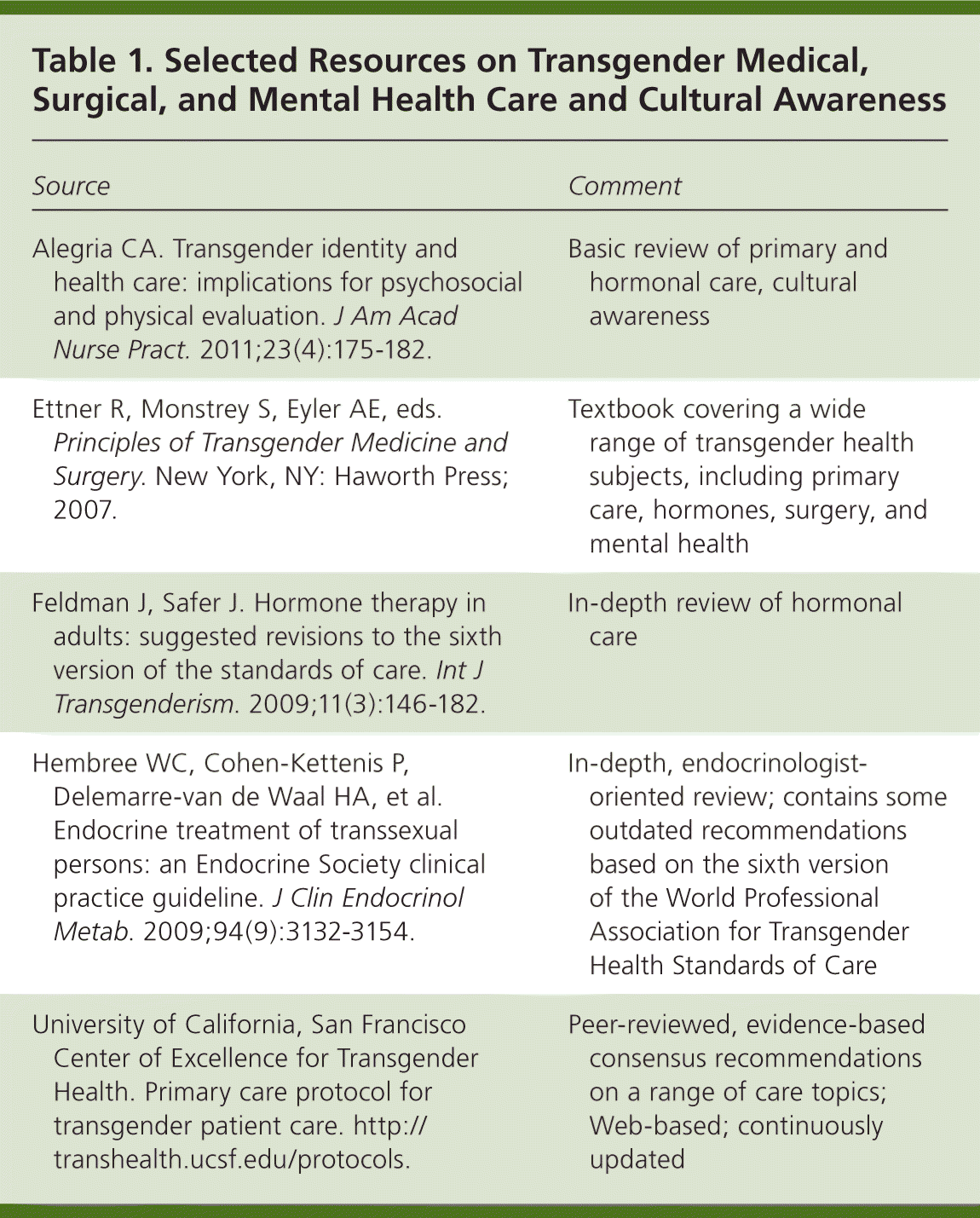
Table 1. Selected Resources on Transgender Medical, Surgical, and Mental Health Care and Cultural Awareness
| Source | Comment |
|---|---|
| Alegria CA. Transgender identity and health care: implications for psychosocial and physical evaluation. J Am Acad Nurse Pract. 2011;23(4):175–182. | Basic review of primary and hormonal care, cultural awareness |
| Ettner R, Monstrey S, Eyler AE, eds. Principles of Transgender Medicine and Surgery. New York, NY: Haworth Press; 2007. | Textbook covering a wide range of transgender health subjects, including primary care, hormones, surgery, and mental health |
| Feldman J, Safer J. Hormone therapy in adults: suggested revisions to the sixth version of the standards of care. Int J Transgenderism. 2009;11(3):146–182. | In-depth review of hormonal care |
| Hembree WC, Cohen-Kettenis P, Delemarrevan de Waal HA, et al. Endocrine treatment of transsexual persons: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2009;94(9):3132–3154. | In-depth, endocrinologist-oriented review; contains some outdated recommendations based on the sixth version of the World Professional Association for Transgender Health Standards of Care |
| University of California, San Francisco Center of Excellence for Transgender Health. Primary care protocol for transgender patient care. http://transhealth.ucsf.edu/protocols. | Peer-reviewed, evidence-based consensus recommendations on a range of care topics; Web-based; continuously updated |
Primary care physicians may see patients referred from a specialist who has initiated cross-sex hormone therapy. Conversely, a primary care physician inexperienced in the care of transgender persons may be approached by a patient seeking cross-sex hormone therapy. If the physician is not able to offer this therapy, the patient should be referred. WPATH maintains a database of health care professionals who provide transgender care, which is available at http://www.wpath.org/find_a_provider.cfm.
Accessing Cross-Sex Hormone Therapy
The SOC7 allows physicians to tailor their practices based on individual patient issues, special physician skills or knowledge, cultural variations, lack of resources, and the need for harm reduction strategies. In addition, the SOC7 notes that non–mental health physicians with experience in gender variance and training in general behavioral or mental health may evaluate patients for eligibility to receive cross-sex hormone therapy and make referrals themselves. Ultimately, primary care physicians will determine their own comfort levels with conducting such assessments.
The SOC7 criteria for hormone therapy are the presence of persistent and well-documented gender dysphoria, the patient having the capacity to make a fully informed decision and consent to treatment, and the patient being at the age of majority in a given country (a separate process exists within SOC7 for minors). The Diagnostic and Statistical Manual of Mental Disorders, 4th ed., criteria for gender identity disorder in adults can be used as a guide for evaluating for gender dysphoria; however, the manual does not provide a clear definition of the condition, and a revision of terminology and criteria is expected for the upcoming fifth edition.12,13
Any significant medical or mental health concerns must be reasonably well controlled before initiating cross-sex hormone therapy. Each physician should make an assessment based on the nature and severity of the comorbidity and the needs of the patient. For example, poorly controlled dyslipidemia should not prevent initiation of the therapy, whereas it may be delayed in a patient who has brittle diabetes or a poorly controlled psychotic disorder. The decision should be made on a case-by-case basis, and informed patient consent is crucial.
Statements of Medical Necessity and Individuality
In a 2008 statement, the WPATH Board of Directors defined all medical, surgical, and mental health care services related to gender dysphoria as medically necessary.14 The SOC7 reiterates this statement, and calls for universal insurance coverage of such services. This statement, as well as SOC7, affirms that each gender-variant person will have his or her own individual desires with respect to timing, the use of hormones and surgery, and the type of social transition being made. The health care of transgender persons has begun moving out of the shadows and into the spotlight; as transgender health care moves into the mainstream, primary care physicians will be increasingly called upon to provide compassionate and individualized care to this diverse community.

