Original Article: Common Finger Fractures and Dislocations
Issue Date: April 15, 2012
Available at: https://www.aafp.org/afp/2012/0415/p805.html
to the editor: Drs. Borchers and Best provide an excellent clinical review of the treatment of common finger fractures and dislocations. However, I believe their recommendations on the treatment of metacarpophalangeal (MCP) dislocation are not entirely correct. Reduction of these dislocations is different than that of proximal interphalangeal or distal interphalangeal dislocations because direct in-line traction may cause entrapment of soft tissues.1 MCP dislocation should be performed with the wrist in slight flexion, with pressure applied at the base of the proximal phalanx to slide the proximal phalanx over the MCP joint1 (Figure 1). This clarification should help readers avoid any potential complications should they encounter this uncommon dislocation.
Figure 1.
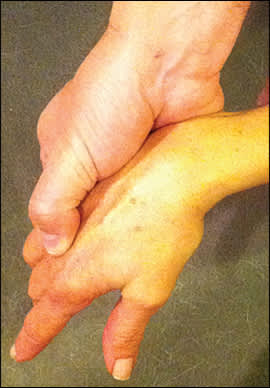
Reduction of a dorsal metacarpophalangeal dislocation. With the wrist in slight flexion, pressure is applied at the base of the proximal phalanx to slide it over the metacarpophalangeal joint.
Copyright © Matthew Gammons, MD.
REFERENCE
- 1.Dinh P, Franklin A, Hutchinson B, Schnall SB, Fassola I. Metacarpophalangeal joint dislocation. J Am Acad Orthop Surg. 2009;17(5):318-324.
in reply: I appreciate Dr. Gammons' response regarding the closed reduction of a simple metacarpophalangeal (MCP) dislocation. This uncommon dislocation usually occurs in the index finger and in a dorsal direction, similarly to a proximal interphalangeal dislocation.1,2
As Dr. Gammons correctly states, the reduction of these dislocations is different from common proximal interphalangeal dislocations. In MCP dislocations, the volar plate is often injured, and direct in-line traction in the axis of the metacarpal should be avoided to prevent interposition of the volar plate or other soft tissue between the base of the proximal phalanx and the head of the metacarpal.3 Proper technique of a closed reduction of a simple MCP dislocation should involve flexion of the wrist and interphalangeal joints to reduce tension on the flexor tendons during relocation. The dislocated MCP joint should then be hyperextended to 90 degrees. At this point, traction should be applied in the axis of the proximal phalanx, and the base of the proximal phalanx is reduced over the head of the metacarpal using volar pressure. Traction applied to the proximal phalanx in hyperextension at 90 degrees to the metacarpal axis does not have the same risk as in-line traction to the metacarpal axis. The MCP joint is then flexed to complete the reduction.4

