A 79-year-old woman presented with a rapidly growing nodule on her leg six months following surgical excision of a basal cell carcinoma. The nodule was about 1 × 1 cm in size and located at the surgical site.
Physical examination revealed an erythematous and centrally hyperkeratotic nodule at the inferior margin of the surgical scar (see accompanying figure). The lesion began to regress after two months without treatment.
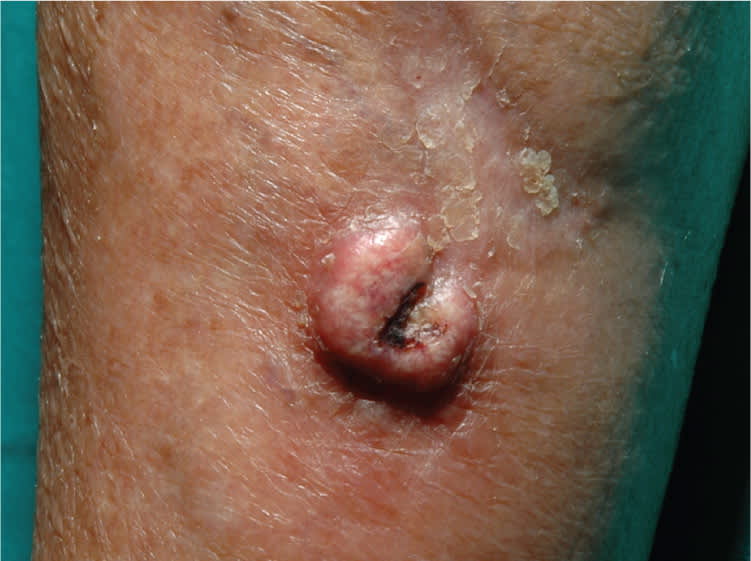
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Basal cell carcinoma recurrence.
B. Dermatofibrosarcoma protuberans.
C. Keloid.
D. Keratoacanthoma.
E. Subcutaneous fungal infection.
Discussion
The answer is D: keratoacanthoma. Keratoacanthomas are rapidly growing tumors that are generally considered a variant of squamous cell carcinoma. Rarely, keratoacanthomas can develop in postoperative wounds or scars.1
Keratoacanthomas are characterized by rapid growth over several weeks or months, usually followed by spontaneous resolution over four to six months. Most occur in sun-exposed areas of the skin. These lesions begin as a papule, which becomes a well-defined, uniform, firm, flesh-colored to brown nodule. Keratoacanthomas are elevated away from the surrounding skin and have a central hyperkeratotic plug. They are usually 1 to 2 cm in size, but may be larger.
The recurrence of basal cell carcinoma after nonradical surgical excision is typically characterized by telangiectasias and eventual central ulceration. Nodules are solid, flesh-colored, and often translucent with mother-of-pearl reflectance. There is no initial keratosis.
Dermatofibrosarcoma protuberans is a rare, nodular, sarcomatous neoplasm that can clinically resemble a keloid.2 It is a low-grade, slow-growing malignancy that appears as a firm, indurated, flesh-colored to red-brown plaque. Multiple exophytic nodules are often present.
Keloids are elevated hypertrophic scars that extend beyond the borders of the original wound, do not regress spontaneously, and usually recur after excision. They are more common in persons with darker skin pigmentation and appear as firm to hard, flesh-colored to red nodules with a smooth surface. Keloids may take months or years to develop.3
Subcutaneous fungal infections may lead to a single or multiple slow-growing, painless, erythematous or bluish nodules or plaques. These fungal infections have been reported in patients who have had a transplant, who are immunocompromised, who are from countries with poor sanitary conditions, or who have a history of a contaminated injury.4 They require surgical or antifungal therapy.
Summary Table
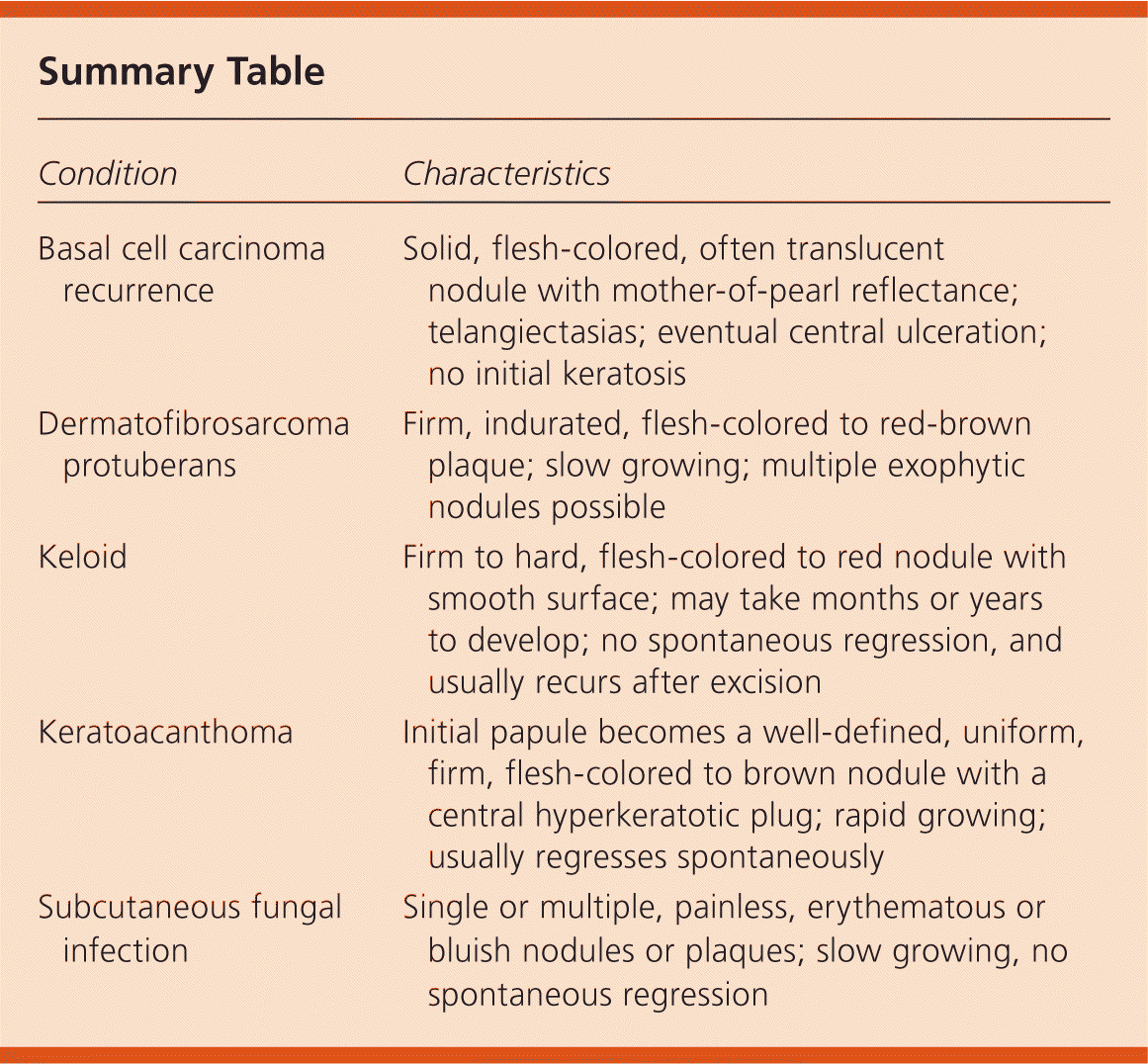
| Condition | Characteristics |
|---|---|
| Basal cell carcinoma recurrence | Solid, flesh-colored, often translucent nodule with mother-of-pearl reflectance; telangiectasias; eventual central ulceration; no initial keratosis |
| Dermatofibrosarcoma protuberans | Firm, indurated, flesh-colored to red-brown plaque; slow growing; multiple exophytic nodules possible |
| Keloid | Firm to hard, flesh-colored to red nodule with smooth surface; may take months or years to develop; no spontaneous regression, and usually recurs after excision |
| Keratoacanthoma | Initial papule becomes a well-defined, uniform, firm, flesh-colored to brown nodule with a central hyperkeratotic plug; rapid growing; usually regresses spontaneously |
| Subcutaneous fungal infection | Single or multiple, painless, erythematous or bluish nodules or plaques; slow growing, no spontaneous regression |

