Kidney stones develop when crystals separate from the urine and aggregate within the kidney papillae, renal pelvis, or ureter.
- The age of peak incidence for stone disease is 20 to 40 years, although stones are seen to occur in all age groups. The male-to-female ratio is 3:2.
The evidence from randomized controlled trials is somewhat sparse regarding the best treatments for persons with asymptomatic kidney stones.
- Both percutaneous nephrolithotomy and extracorporeal shock wave lithotripsy may reduce the need for further invasive surgery. However, these procedures are not without risk, and the risks and benefits should be weighed carefully in asymptomatic persons.
- We found no evidence from randomized controlled trials assessing ureteroscopy in persons with asymptomatic kidney stones.
For symptomatic kidney stones, percutaneous nephrolithotomy, ureteroscopy, and extracorporeal shock wave lithotripsy are all options for treatment.
- Percutaneous nephrolithotomy seems more effective than extracorporeal shock wave lithotripsy in removing symptomatic kidney stones, but it is associated with more complications.
- In highly selected, uncomplicated cases, tubeless percutaneous nephrolithotomy (i.e., no nephrostomy, but stented) and totally tubeless percutaneous nephrolithotomy (i.e., no nephrostomy or stent) seem to give an improved recovery profile.
- Ureteroscopy seems as effective as extracorporeal shock wave lithotripsy in removing symptomatic kidney stones, but it is associated with more complications.
- With extracorporeal shock wave lithotripsy, a slower rate of 60 shock waves per minute may result in greater treatment success.
- Individuals with larger stones are likely to take longer to pass stone fragments after extracorporeal shock wave lithotripsy. In these persons, percutaneous nephrolithotomy may be a more suitable option.
- Open nephrolithotomy has been largely superseded by percutaneous nephrolithotomy in developed countries.
For symptomatic ureteric stones, ureteroscopy seems to increase overall stone-free rates and decrease time to becoming stone free compared with extracorporeal shock wave lithotripsy.
Medical expulsive therapy with alpha blockers seems to increase stone-free rates and decrease time to stone passage compared with standard treatment.
- We found no evidence from randomized controlled trials examining ureterolithotomy (either open or laparoscopic) in persons with symptomatic ureteric stones.
Clinical Questions
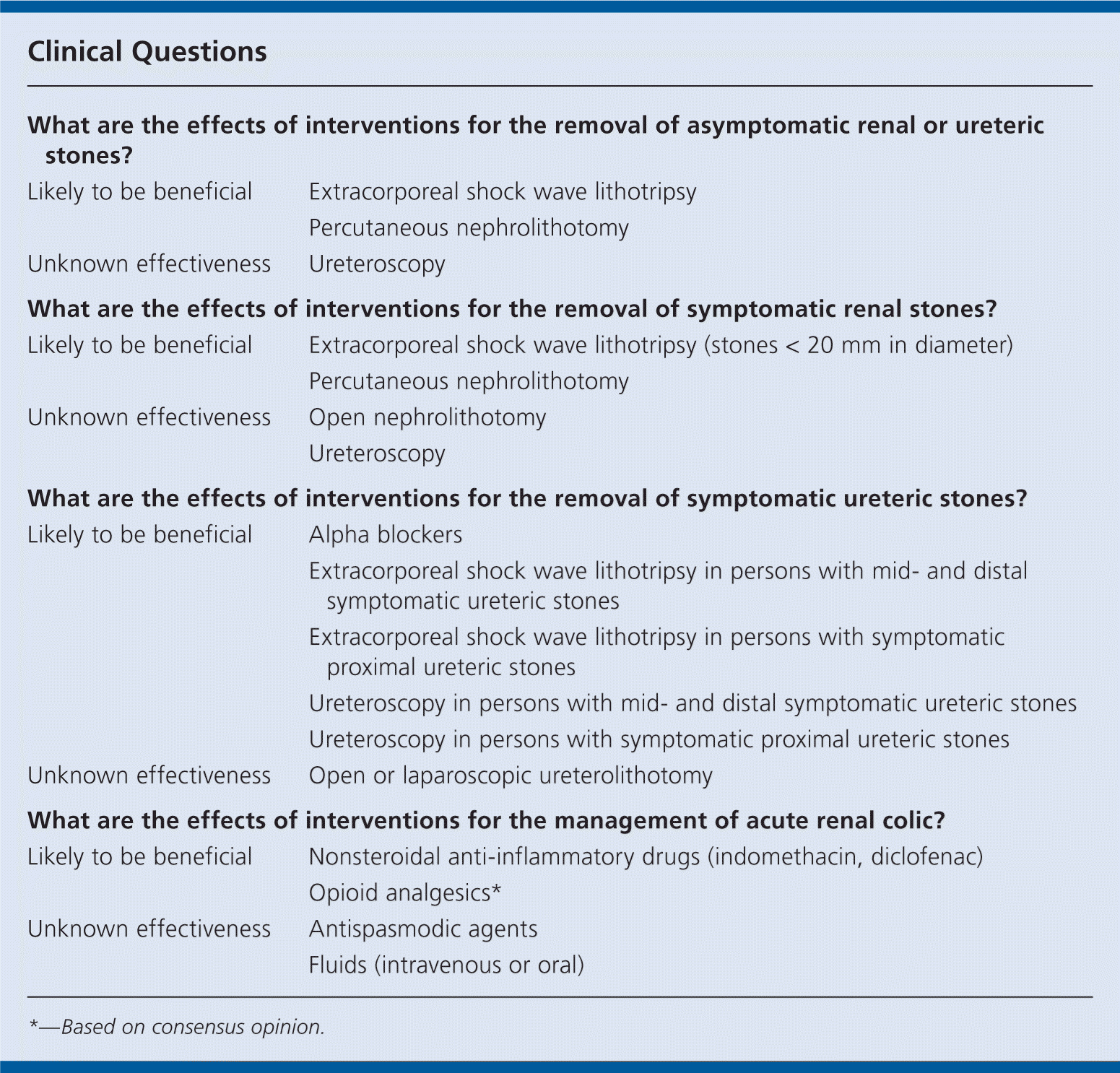
| What are the effects of interventions for the removal of asymptomatic renal or ureteric stones? | |
| Likely to be beneficial | Extracorporeal shock wave lithotripsy |
| Percutaneous nephrolithotomy | |
| Unknown effectiveness | Ureteroscopy |
| What are the effects of interventions for the removal of symptomatic renal stones? | |
| Likely to be beneficial | Extracorporeal shock wave lithotripsy (stones < 20 mm in diameter) |
| Percutaneous nephrolithotomy | |
| Unknown effectiveness | Open nephrolithotomy |
| Ureteroscopy | |
| What are the effects of interventions for the removal of symptomatic ureteric stones? | |
| Likely to be beneficial | Alpha blockers |
| Extracorporeal shock wave lithotripsy in persons with mid- and distal symptomatic ureteric stones | |
| Extracorporeal shock wave lithotripsy in persons with symptomatic proximal ureteric stones | |
| Ureteroscopy in persons with mid- and distal symptomatic ureteric stones | |
| Ureteroscopy in persons with symptomatic proximal ureteric stones | |
| Unknown effectiveness | Open or laparoscopic ureterolithotomy |
| What are the effects of interventions for the management of acute renal colic? | |
| Likely to be beneficial | Nonsteroidal anti-inflammatory drugs (indomethacin, diclofenac) |
| Opioid analgesics* | |
| Unknown effectiveness | Antispasmodic agents |
| Fluids (intravenous or oral) | |
*—Based on consensus opinion.
Definition
Nephrolithiasis is the presence of stones within the kidney; urolithiasis is a more general term for stones anywhere within the urinary tract. Urolithiasis is usually categorized according to the anatomical location of the stones (i.e., renal calyces, renal pelvis, ureter, bladder, and urethra). Ureteric urolithiasis is described further based on the portion of the urinary tract (proximal, middle, or distal) in which the stone is situated. This review assesses the effects of treatments only for the removal of asymptomatic or symptomatic renal and ureteric stones. It excludes pregnant women, in whom some diagnostic procedures and treatments for stone removal may be contraindicated, and persons with significant comorbidities (including severe cardiovascular and respiratory conditions) who may be at increased risk when under general anesthesia.
Diagnosis is usually based on clinical history, supported by investigations with diagnostic imaging. One-third of all kidney stones become clinically evident, typically causing pain (often severe in nature), renal angle tenderness, hematuria, or digestive symptoms such as nausea, vomiting, or diarrhea. The onset of pain is usually sudden, is typically felt in the sides between the lower ribs and pelvis and the lower part of the back, and radiates to the groin and genitalia (scrotum or labia).
Persons who have kidney stones are typically restless, find the pain excruciating, and describe it as the worst pain they have ever experienced. The cause and chemical composition of a stone may have some bearing on its diagnosis and management, and particularly on prevention of recurrence. Although the choices for surgical management generally remain the same for all types of stone disease, the recognition of a specific cause, such as recurrent infection with a urease-producing organism for struvite stones, or cystinuria for cystine stones, will inform further management.
Bleeding within the urinary tract may present with symptoms identical to those of kidney stones, particularly if blood clots are present within the renal pelvis or ureter. The differential diagnosis also includes urinary tract infection (which may be concurrent), ureteropelvic junction obstruction, and urothelial carcinoma. Patients who have papillary cell necrosis (which may occur in diabetes mellitus or sickle cell disease) may also present with renal colic.
Incidence and Prevalence
The age of peak incidence for stone disease is 20 to 40 years, although stones are seen to occur in all age groups. The male predominance of stone disease may be decreasing, with recent reports of the male-to-female ratio being approximately 3:2. In North America, calcium oxalate stones (the most common variety) have a recurrence rate of 10 percent at one year and 35 percent at five years after the first episode of kidney stone disease.
Etiology and Risk Factors
Kidney stones develop when crystals precipitate from the urine and aggregate within the kidney papillae, renal pelvis, or ureter. The most common type of stones contains calcium, usually calcium oxalate and, less commonly, calcium phosphate. Other metabolic stones are formed of uric acid, cystine, and xanthine. There are also infection stones, or struvite stones, which contain a mixture of magnesium, ammonium, and phosphate, and are associated with urease-forming organisms such as Klebsiella or Proteus species.
Predisposing factors for stone formation include dehydration, lifestyle, geographic location (dry arid climate), and certain specific risk factors. These may include anatomical or structural abnormalities (e.g., ureteropelvic junction obstruction, urinary diversion surgery, horseshoe kidney, calyceal diverticulum), underlying metabolic conditions (e.g., cystinuria, oxaluria, gout), certain drugs, and urease-producing infective organisms.
Prognosis
Most kidney stones pass within a few days to several weeks with expectant treatment (including adequate fluid intake and analgesia). Other stones may take longer to pass, and an observation period of four to six weeks is appropriate. Ureteric stones less than 5 mm in diameter will pass spontaneously in about 90 percent of persons, compared with 50 percent of ureteric stones 5 to 10 mm in diameter. Expectant (conservative) management is considered on an individual basis in persons with stones that are asymptomatic, mildly symptomatic, or small, or in persons with significant comorbidities for whom the risks of treatment may outweigh the benefits.
A stone that causes chronic constriction of a ureter may lead to hydronephrosis and renal atrophy. Ureteral obstruction may also result in serious complications including urinary infection, perinephric abscess, or urosepsis. Drainage of an infected obstructed kidney is a medical emergency. Infection may also occur after invasive procedures for stone removal. Some of these complications may cause kidney damage and compromised renal function.

