A 46-year-old woman presented with a facial rash that had worsened over nine months. She had been treated with several topical corticosteroids and topical antibiotics, which improved her symptoms only temporarily. She was taking no other medications. There were no specific triggers or contacts, and she had no significant medical history.
Examination revealed annular plaques with a raised erythematous border on the forehead (Figure 1) and both cheeks (Figure 2). Other areas of her body were not affected.
Figure 1.
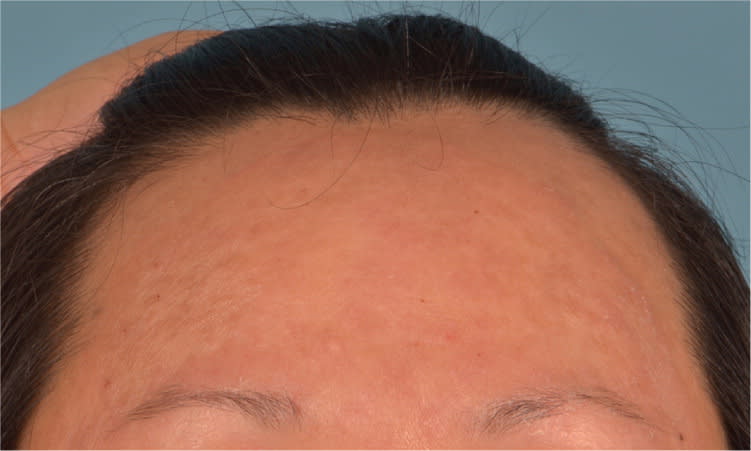
Figure 2.
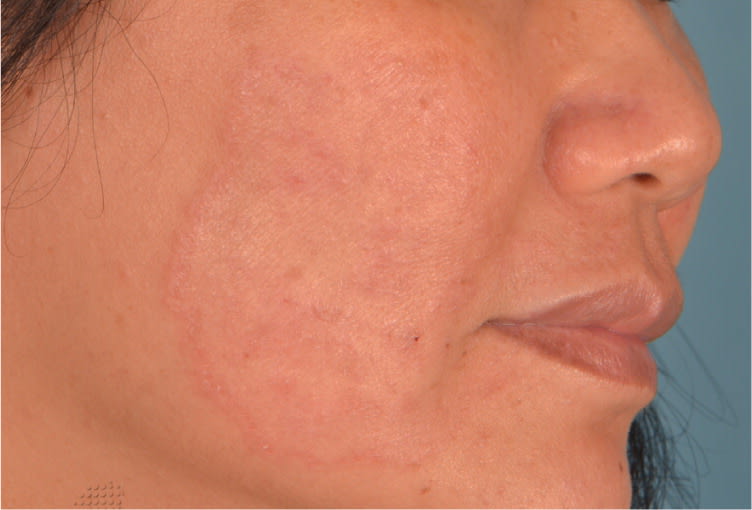
Figures reprinted with permission from the National Skin Centre.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Acne rosacea.
B. Acute cutaneous lupus erythematosus.
C. Atopic dermatitis.
D. Dermatomyositis.
E. Tinea faciei.
Discussion
The answer is E: tinea faciei. Tinea faciei, or dermatophytosis, is a common condition that results from a dermatophyte infection of the superficial epidermis. Papulosquamous plaques with an annular scaly edge should increase the clinical suspicion of tinea infections, particularly if they persist despite treatment with steroids. After the application of steroids, scaling and other clinical features of tinea infection may disappear, leading to tinea incognito. Tinea pedis and tinea cruris are the most common superficial fungal infections. However, tinea faciei accounts for about 3 to 4 percent of tinea corporis cases. It is more common in females and children, accounting for about 19 percent of all superficial fungal infections in children.1
A fungal infection can be confirmed using a skin scraping of the lesion borders. A culture can identify the specific dermatophyte species, although treatment is usually the same. The fungal scraping and culture can produce false-negative results, and sensitivity decreases after treatment with steroids and antifungal medications.2 Rarely, a punch biopsy is needed to diagnose the infection or evaluate for other possible causes.
Most tinea infections can be treated with topical antifungal medications. Systemic therapy should be considered for resistant, chronic, or extensive cases. Oral antifungal medications should be used if the infection involves hair or folliculitis because topical applications are unable to reach the depth of the hair follicles, where the dermatophytes reside.
Acne rosacea is a chronic inflammatory condition affecting the cheeks, forehead, and nose. The condition typically causes papules, pustules, and telangiectasias. Flushing and redness often occur with consumption of spicy foods or alcohol.
Acute cutaneous lupus erythematosus usually involves erythematous patches or plaques on the malar eminence and nasal bridge, resulting in the typical “butterfly” configuration. Systemic signs and symptoms of lupus erythematosus may also be present. The rash is most common in sun-exposed areas.
Atopic dermatitis, or endogenous eczema, is eczematous instead of papulosquamous and is most common on the flexor surfaces of the extremities. Patients with the condition often have a history of other atopic diseases, such as asthma or allergic rhinitis. The rash should respond to topical corticosteroids.
Dermatomyositis usually causes periorbital, symmetrical, violaceous patches (heliotrope rash), as well as symmetrical weakness in the proximal muscles.
Summary Table
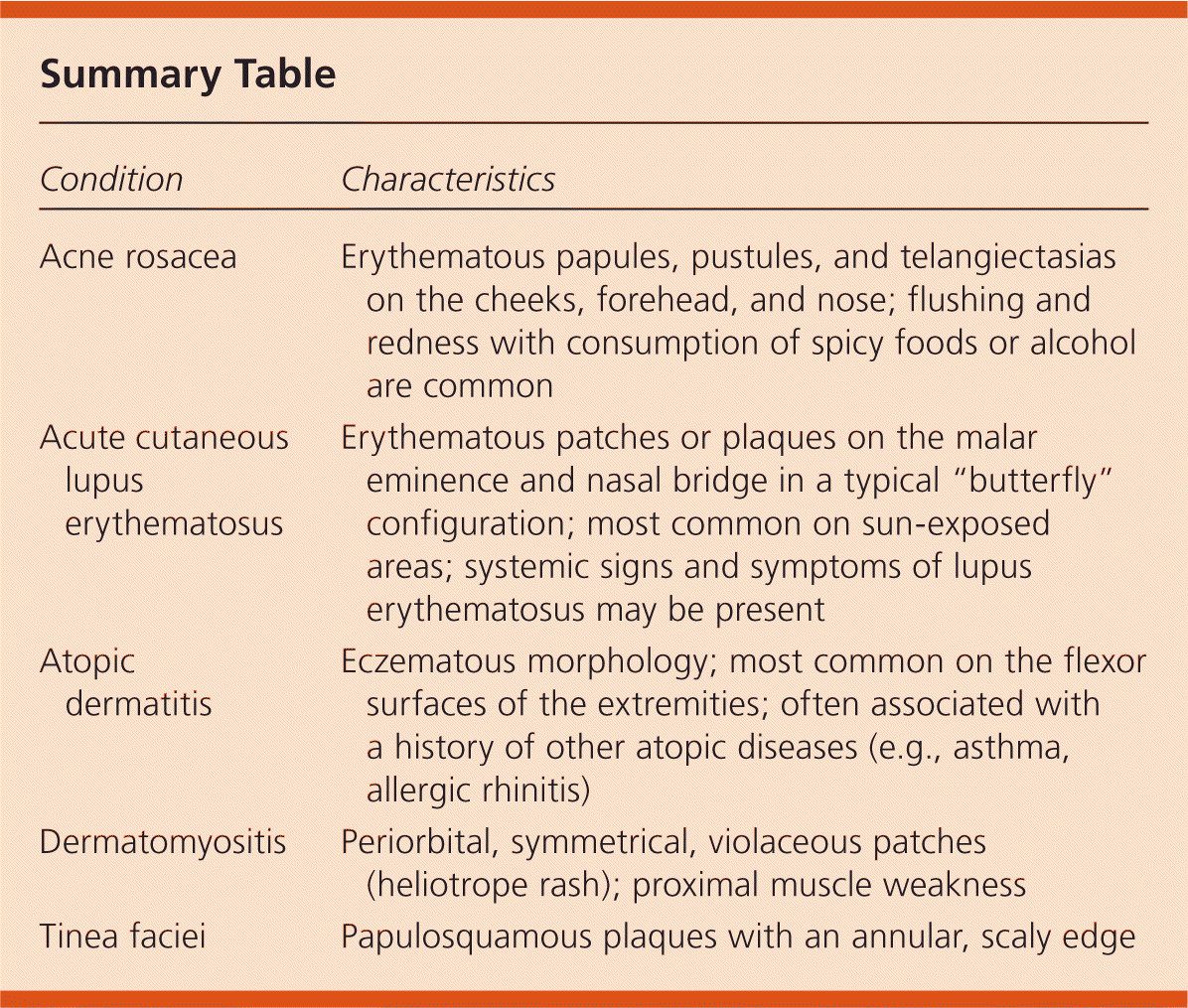
| Condition | Characteristics |
|---|---|
| Acne rosacea | Erythematous papules, pustules, and telangiectasias on the cheeks, forehead, and nose; flushing and redness with consumption of spicy foods or alcohol are common |
| Acute cutaneous lupus erythematosus | Erythematous patches or plaques on the malar eminence and nasal bridge in a typical “butterfly” configuration; most common on sun-exposed areas; systemic signs and symptoms of lupus erythematosus may be present |
| Atopic dermatitis | Eczematous morphology; most common on the flexor surfaces of the extremities; often associated with a history of other atopic diseases (e.g., asthma, allergic rhinitis) |
| Dermatomyositis | Periorbital, symmetrical, violaceous patches (heliotrope rash); proximal muscle weakness |
| Tinea faciei | Papulosquamous plaques with an annular, scaly edge |

