A 41-year-old man presented with a painful, erythematous, erosive, and scaly rash. It was symmetrically distributed over sun-exposed areas, involving his face, neck, dorsum of his hands and feet, and upper back (Figures 1 and 2). The rash and frequent loose stools had been present for several months.
Figure 1.
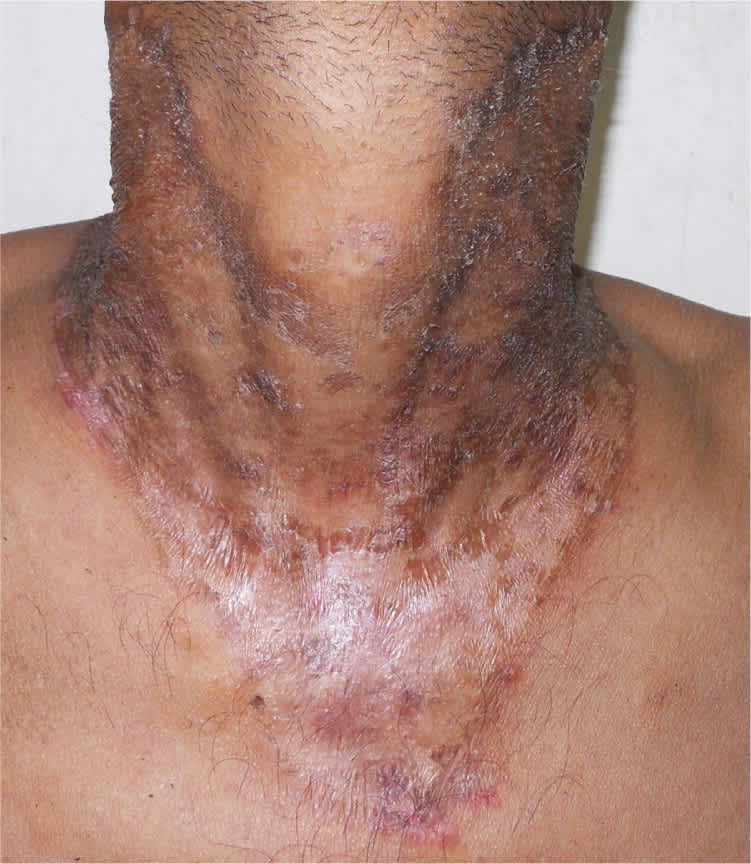
Figure 2.
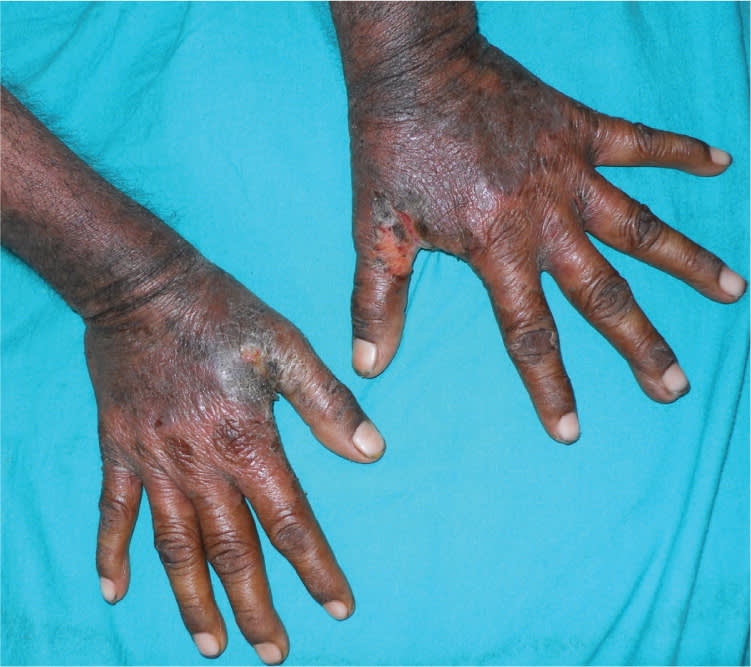
Neuropsychiatric evaluation revealed short-term memory loss, speech problems, and difficulties with activities of daily living. He had a long history of heavy alcohol use. He was not taking any medications. Results of routine laboratory testing were normal.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Atopic dermatitis.
B. Pellagra.
C. Photosensitive drug reaction.
D. Porphyria cutanea tarda.
E. Systemic lupus erythematosus.
Discussion
The answer is B: pellagra. Pellagra occurs in the late stage of severe niacin deficiency and can affect the gastrointestinal tract, nervous system, and skin. It is classically described by the three D's: diarrhea, dermatitis, and dementia.1 Although the exact incidence of pellagra is unknown, it is a relatively rare condition that is restricted to at-risk groups and typically affects adults.
Primary pellagra results from inadequate intake of niacin and/or tryptophan.1,2 The secondary form of the disease occurs when other conditions hamper the body's ability to absorb or process niacin. These conditions may include prolonged diarrhea, chronic alcoholism, chronic colitis, cirrhosis of the liver, tuberculosis of the gastrointestinal tract, malignant carcinoid tumor, Hartnup disease, and human immunodeficiency virus infection. Treatment with certain drugs, such as isoniazid, pyrazinamide, fluorouracil, phenytoin (Dilantin), and azathioprine (Imuran), can also cause the disorder.1,2
The first manifestations of the disease are anorexia, vomiting, abdominal pain, watery diarrhea, photosensitivity, lassitude, irritability, and fatigue. In the early stage, pellagra simulates sunburn with erythema and blister formation (wet pellagra).2 It may progress to a symmetric, scaly rash with a copper or mahogany hue.1,2 Typical locations include the neck (casal necklace) and extensor surface of the hands and forearms. There is often a dull erythema on the bridge of the nose with fine, yellowish scales on the follicular orifices.1 As the disease progresses, neuropsychiatric manifestations, such as depression, photophobia, asthenia, and memory loss, become more prominent.
Untreated pellagra can lead to frank psychosis and sometimes death.1 The diagnosis is based on the distinctive clinical presentation and confirmed by the rapid response to oral niacin supplementation. Skin biopsy findings can support the diagnosis but are not specific.1,2
Atopic dermatitis often occurs with other atopic diseases, such as bronchial asthma, allergic conjunctivitis, and hay fever, and is chronic or relapsing. In adults, an intensely pruritic, eczematous skin rash predominantly affects the flexures and hands, and is accompanied by prominent xerosis.1,3
Patients with a photosensitive drug reaction have a history of exposure to a medication. Skin eruption of varied morphology (e.g., macules, papules, lichenoid, vesiculobullous) usually occurs on sun-exposed areas. Systemic features (e.g., diarrhea, neuropsychiatric manifestations) do not accompany the skin lesions.1
Porphyria cutanea tarda usually causes photosensitivity, resulting in blisters and erosions on the sun-exposed areas. These lesions heal slowly, with scarring, milia, and dyspigmentation. Dark-colored urine (pink or red fluorescence under a Wood lamp), hypertrichosis, and sclerodermatous skin thickening may also occur.1,4
Systemic lupus erythematosus usually presents as a characteristic butterfly-like malar rash, discoid rash, painless oral ulcer, and alopecia. The disease may cause prominent musculoskeletal, renal, hematologic, cardiovascular, respiratory, and central nervous system problems.1,5
Summary Table

| Diagnosis | Characteristics |
|---|---|
| Atopic dermatitis | Chronic or relapsing dermatitis; personal or family history of atopy; intense pruritus, eczematous skin rash mostly over the flexures and hands in adults; prominent xerosis |
| Pellagra | Watery diarrhea, photosensitive dermatitis, and neuropsychiatric manifestations; sunburn-like rash with erythema and blisters (wet pellagra) on the neck (casal necklace) and extensor surface of the hands and forearms; progresses to a dull erythema on the bridge of the nose with fine, yellowish scales on the follicular orifices |
| Photosensitive drug reaction | History of medication use; skin eruption of varied morphology on sun-exposed areas |
| Porphyria cutanea tarda | Photosensitivity resulting in blisters and erosions on sun-exposed areas; slow healing with scarring, milia, and dyspigmentation; hypertrichosis and sclerodermatous skin thickening; dark-colored urine exhibiting pink or red fluorescence under a Wood lamp |
| Systemic lupus erythematosus | Butterfly-like malar rash, discoid rash, painless oral ulcer, and alopecia; prominent musculoskeletal, renal, hematologic, cardiovascular, respiratory, and central nervous system problems |

