Optimal management of myocardial infarction in the subacute period focuses on improving the discharge planning process, implementing therapies early to prevent recurrent myocardial infarction, and avoiding hospital readmission. Evidence-based guidelines for the care of patients with acute coronary syndrome are not followed up to 25% of the time. Antiplatelet therapy, renin-angiotensin-aldosterone system inhibitors, beta blockers, and statins constitute the foundation of medical therapy. Early noninvasive stress testing is an important risk assessment tool, especially in patients who do not undergo revascularization. Discharge preparation should include a review of medications, referral for exercise-based cardiac rehabilitation, activity recommendations, education about lifestyle modification and recognition of cardiac symptoms, and a clear follow-up plan. Because nonadherence to medications is common in patients after a myocardial infarction and is associated with increased mortality risk, modifiable factors associated with medication self-discontinuation should be addressed before discharge. Structured discharge processes should be used to enhance communication and facilitate the transition from the hospital to the family physician's care.
Cardiovascular disease causes one in six deaths in the United States annually.1 In 2008, medical costs of heart disease were an estimated $190 billion, and are projected to triple over the next 20 years.1 A myocardial infarction (MI), defined as clinical evidence of myocardial necrosis consistent with myocardial ischemia, is diagnosed every 34 seconds in the United States.1,2 Acute coronary syndrome (ACS), which encompasses non–ST elevation MI and ST elevation MI, resulted in 1.2 million hospital admissions in 2009.1
Studies show that care consistent with established guidelines results in decreased mortality during hospitalization and at six months postdischarge, but up to 25% of opportunities to provide guideline-recommended care are missed.3,4 Preventing readmissions is also a concern; in a study of 16,000 patients with ACS, 20% were rehospitalized within one year, highlighting a need for more effective discharge planning and care transitions.5
Family physicians, in partnership with a cardiovascular subspecialist, have a vital role in the management of MI during the subacute period. This period begins after a revascularization procedure has been performed or after the decision to not revascularize is made, and lasts for one to three months.6 This article focuses on the management of MI during this critical period, and emphasizes the importance of the care transition from the hospital to the outpatient setting.
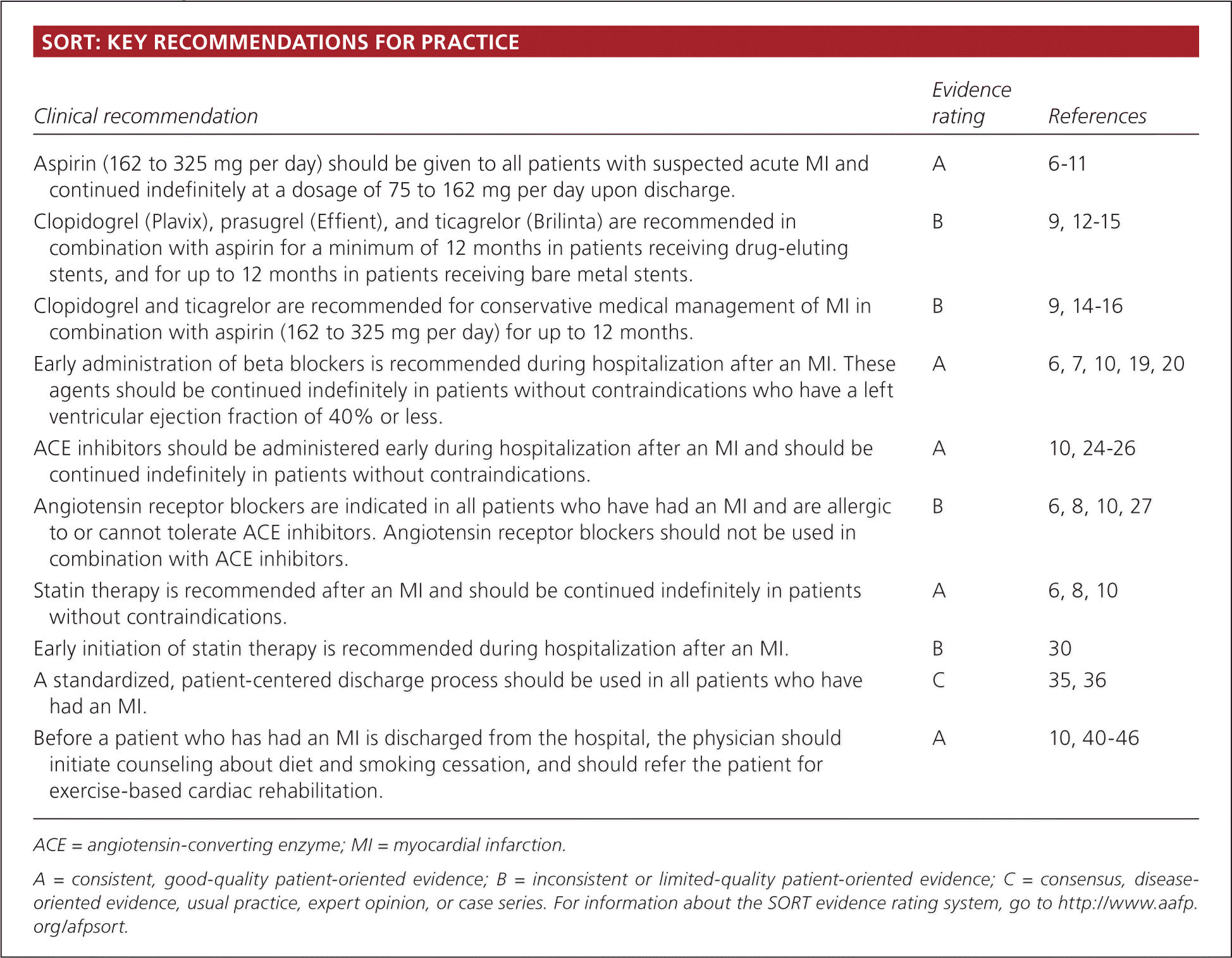
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Aspirin (162 to 325 mg per day) should be given to all patients with suspected acute MI and continued indefinitely at a dosage of 75 to 162 mg per day upon discharge. | A | 6–11 |
| Clopidogrel (Plavix), prasugrel (Effient), and ticagrelor (Brilinta) are recommended in combination with aspirin for a minimum of 12 months in patients receiving drug-eluting stents, and for up to 12 months in patients receiving bare metal stents. | B | 9, 12–15 |
| Clopidogrel and ticagrelor are recommended for conservative medical management of MI in combination with aspirin (162 to 325 mg per day) for up to 12 months. | B | 9, 14–16 |
| Early administration of beta blockers is recommended during hospitalization after an MI. These agents should be continued indefinitely in patients without contraindications who have a left ventricular ejection fraction of 40% or less. | A | 6, 7, 10, 19, 20 |
| ACE inhibitors should be administered early during hospitalization after an MI and should be continued indefinitely in patients without contraindications. | A | 10, 24–26 |
| Angiotensin receptor blockers are indicated in all patients who have had an MI and are allergic to or cannot tolerate ACE inhibitors. Angiotensin receptor blockers should not be used in combination with ACE inhibitors. | B | 6, 8, 10, 27 |
| Statin therapy is recommended after an MI and should be continued indefinitely in patients without contraindications. | A | 6, 8, 10 |
| Early initiation of statin therapy is recommended during hospitalization after an MI. | B | 30 |
| A standardized, patient-centered discharge process should be used in all patients who have had an MI. | C | 35, 36 |
| Before a patient who has had an MI is discharged from the hospital, the physician should initiate counseling about diet and smoking cessation, and should refer the patient for exercise-based cardiac rehabilitation. | A | 10, 40–46 |
ACE = angiotensin-converting enzyme; MI = myocardial infarction.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Early Hospital Care
Irrespective of the timing or nature of the decision to revascularize, several therapies have proven benefit in reducing adverse cardiovascular events during the subacute period. Figure 1 provides an overview of the subacute management of MI.6–10
Figure 1. Management of Myocardial Infarction
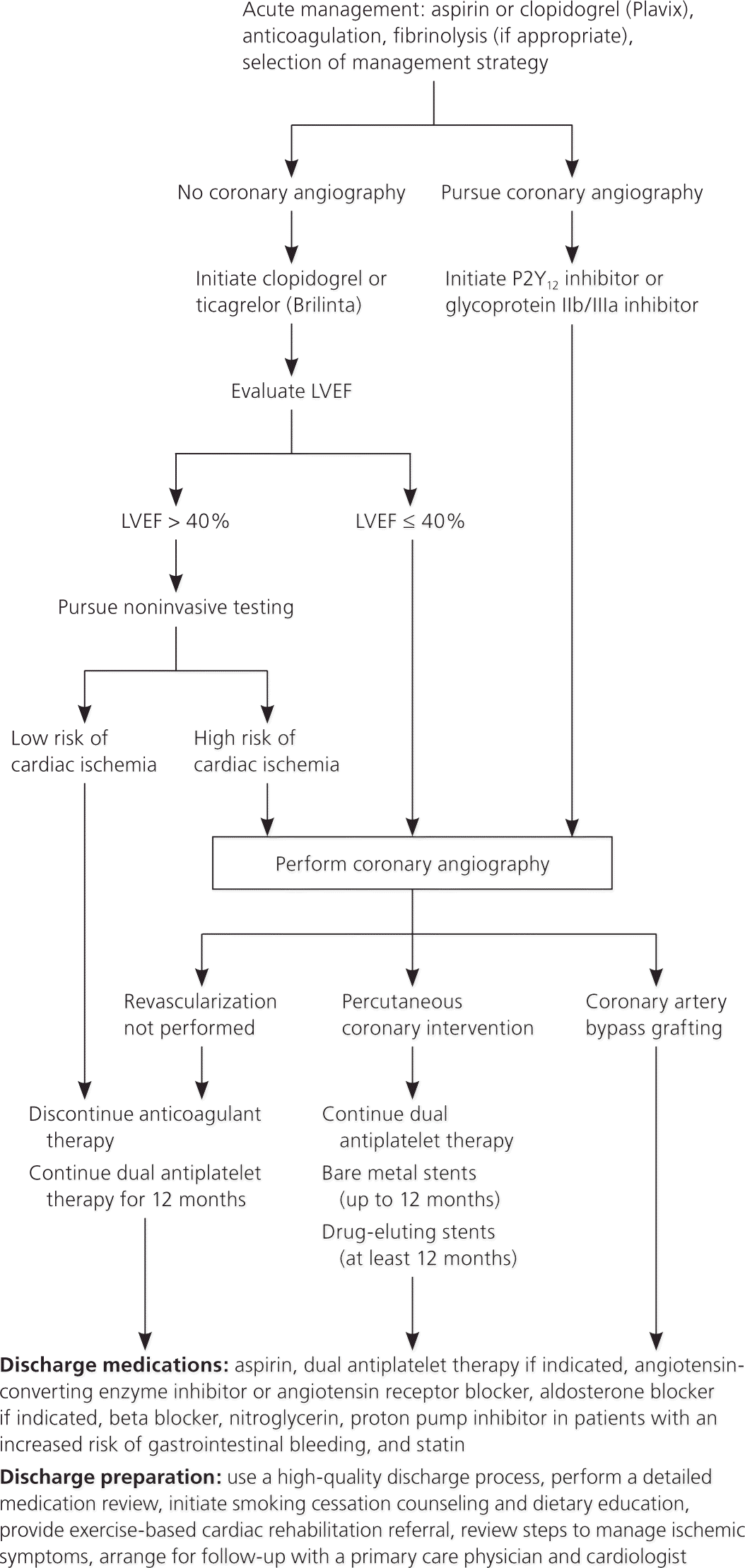
Overview of the subacute management of myocardial infarction. (LVEF = left ventricular ejection fraction.)
Information from references 6 through 10.
ANTIPLATELET THERAPY
Aspirin. An inhibitor of platelet aggregation, aspirin should be given to all patients with suspected ACS. A systematic review of 15 trials showed that aspirin therapy in patients who had experienced an MI reduced stroke, repeat MI, and death (absolute risk reduction [ARR] = 3.8%; number needed to treat [NNT] = 26).11 An adequate dosage in the acute period is 162 to 325 mg per day; the dosage should be reduced to 75 to 162 mg per day upon discharge and continued indefinitely for prevention of recurrent MI.6–11
P2Y12Inhibitors. P2Y12 inhibitors, including clopidogrel (Plavix), prasugrel (Effient), and ticagrelor (Brilinta), represent a class of antiplatelet agents that, when used in combination with aspirin therapy, decrease major cardiovascular events in patients with ACS who are undergoing percutaneous coronary intervention.12–14 Guidelines suggest that this combination, known as dual antiplatelet therapy, continue for a minimum of 12 months in patients receiving drug-eluting stents and for up to 12 months in those receiving bare metal stents, but the optimal duration is unknown.8,9
The benefits of dual antiplatelet therapy in decreasing the combined end points of cardiovascular mortality, subsequent MI, and stroke were noted at 30 days through 12 months for clopidogrel when compared with placebo (ARR = 2.1%; NNT = 48), and at 15 months and 12 months with prasugrel and ticagrelor, respectively, when compared with clopidogrel.14–16 Of the three P2Y12 inhibitors, only ticagrelor has been shown to improve all-cause mortality.12–14 Guidelines from the American College of Cardiology (ACC) and the American Heart Association (AHA) advocate dual antiplatelet therapy using clopidogrel and ticagrelor for up to 12 months in conservatively treated patients after an MI, but the optimal length of treatment is unclear.9 Proton pump inhibitors are recommended for patients receiving dual antiplatelet therapy who have a history of or risk factors for gastrointestinal bleeding.8,17 Clopidogrel is recommended for patients with aspirin intolerance or allergy, regardless of the initial management strategy.8,18
BETA BLOCKERS
Several systematic reviews have established the long-term mortality benefits of beta-blocker therapy in patients who have had an MI.19,20 The AHA recommends that oral beta-blocker therapy be initiated in all patients without contraindications within 24 hours after an MI, and continued at discharge.6,7,10 However, a Cochrane review that investigated antihypertensive agents initiated within 24 hours of a cardiovascular event found no mortality benefit from beta-blocker therapy within the first month.21 In patients with a left ventricular ejection fraction (LVEF) of 40% or less, beta-blocker therapy should be titrated gradually and continued indefinitely.6,7 Bisoprolol (Zebeta), carvedilol (Coreg), and metoprolol have exhibited a mortality benefit in patients with a reduced LVEF after an MI.22 Guidelines suggest using beta blockers for at least three years in patients with preserved systolic function, but this recommendation is based on limited data.7 One prospective cohort study of 14,043 patients with a remote history of MI concluded that beta-blocker use may not improve cardiovascular outcomes.23
RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM INHIBITORS
Angiotensin-Converting Enzyme Inhibitors and Angiotensin Receptor Blockers. Angiotensin-converting enzyme (ACE) inhibitors are strongly recommended after an MI in patients with hypertension, diabetes mellitus, an LVEF of 40% or less, or chronic kidney disease.6,10 Randomized controlled trials (RCTs) have established that ACE inhibitors reduce mortality in patients who have had an MI.24–26 One review of 22 RCTs concluded that early (within 48 hours) administration of ACE inhibitors after an MI reduced mortality in as early as one month (NNT = 167), and the benefits were greater at one year for early and late administration, with an ARR of 3.7% (NNT = 27) and 2.2% (NNT = 45), respectively.26 A Cochrane review concluded that ACE inhibitors administered within 24 hours of a cardiovascular event can prevent three to five deaths per 1,000 patients at 10 days.21 Unless contraindicated, ACE inhibitors should be continued indefinitely for prevention of recurrent cardiovascular events.8
Angiotensin receptor blockers are recommended in patients who have indications for, but cannot tolerate, ACE inhibitors.6,8,10 Compared with monotherapy, combination therapy with ACE inhibitors and angiotensin receptor blockers leads to increased adverse events with no mortality benefit in patients after an MI, and is not recommended.27 ACE inhibitors and angiotensin receptor blockers should be avoided in patients with hyperkalemia, hypotension, and acute renal failure until these conditions resolve.10
Aldosterone Blockers. Based on the Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study, aldosterone blockers initiated as early as three days after an MI reduced all-cause mortality and cardiac death (ARR = 1.4%; NNT = 71) compared with placebo in patients with a low LVEF and signs of heart failure.28 Guidelines from the ACC/AHA recommend the use of aldosterone blockers in patients who have heart failure or diabetes, have an LVEF of 40% or less, are receiving ACE inhibitors and beta blockers, and have a serum potassium level less than 5.0 mEq per L (5.0 mmol per L) and a creatinine clearance greater than 30 mL per minute per 1.73 m2 (0.50 mL per second per m2).6,8,10
STATIN THERAPY
The role of statins in reducing mortality and ACS in patients with cardiovascular disease is well established.8,29 Consequently, current guidelines advocate initiating these agents before discharge, despite questionable mortality benefit in the subacute period, and continuing therapy indefinitely.6,8,10,29 A Cochrane review found that early initiation of statins in patients with ACS reduced episodes of unstable angina within four months without decreasing mortality or recurrent MI.29 A meta-analysis of 21 trials concluded that statins initiated as early as one day before percutaneous coronary intervention reduced the risk of postprocedural MI (ARR = 6%; NNT = 17) and reduced atrial fibrillation after coronary artery bypass grafting.30 Although the choice of statin does not matter, higher doses may yield more benefits. An RCT of 4,162 patients hospitalized for ACS found a 29% reduction in recurrent unstable angina and a 14% reduction in revascularization in patients receiving 80 mg per day of atorvastatin (Lipitor) compared with those receiving 40 mg per day of pravastatin (Pravachol).31 Consequently, high-dose atorvastatin may be considered in patients with ACS who are already receiving a lower dose or a less potent statin. The ACC and AHA recommend obtaining low-density lipoprotein cholesterol measurements within 24 hours of hospitalization as part of a cardiac risk assessment and guide to initiating lipid-lowering therapy.6,10
Noninvasive Testing
Noninvasive testing, with or without imaging, is an important risk-assessment tool in patients who have had an MI but are not undergoing angiography. LVEF assessment is essential and should guide decisions about care (Figure 1).6–10 The testing modality is based on exercise tolerance, baseline electrocardiography, and test availability. Intermediate- to low-risk patients who have been stable for 48 to 72 hours are candidates for symptom-limited stress testing.6,10 Guidelines from the ACC/AHA recommend submaximal exercise stress testing at four to six days, or symptom-limited stress testing at two to three weeks if predischarge testing was not performed.32 One study found early symptom-limited stress testing (three to seven days after MI) comparable to late testing (one month postdischarge) for diagnostic and prognostic evaluation, but noted that 50% of cardiovascular events within one year of follow-up occurred within the first month, making earlier testing the preferred option.33 However, data addressing the relative safety of early symptom-limited stress testing are scant.10
Preparing for Discharge
A multidisciplinary approach before discharge includes medication review, referral for cardiac rehabilitation, activity recommendations, education about lifestyle modifications and recognition of cardiac symptoms, and a clear follow-up plan. Inadequate communication can hamper transitions of care; a review of 73 studies found that discharging physicians directly communicated with the patient's primary care physician only 3% to 20% of the time.34 Project RED (Re-Engineered Discharge) is a standardized, patient-centered discharge process that can be applied to patients with MI. An RCT of 749 adults with multiple medical conditions who were hospitalized in an urban medical center showed a 30% decrease in combined readmission rates and emergency department visits within 30 days of discharge when Project RED was implemented.35 Table 1 summarizes the components of this quality-focused discharge process.35,36
Table 1. Components of a Standardized, Patient-Centered Discharge Process

| Assess the patient's understanding of the discharge plan; ask the patient to explain in his or her own words; identify and resolve barriers to understanding. |
| Educate the patient about problem-solving strategies, including contacting the primary care physician. |
| Educate the patient about the diagnosis and plan of care during hospitalization. |
| Expedite transmission of the discharge summary to clinicians and services who will care for the patient after discharge. |
| Make appointments for outpatient follow-up and postdischarge testing; stress the importance of follow-up care and ensure that transportation arrangements are in place. |
| Organize postdischarge services; arrange appointments and address barriers to receiving the recommended services. |
| Provide a written summary detailing the indication for admission, clinical course, follow-up, and medication indications and instructions. |
| Provide the patient with steps to take if a concern about his or her condition arises, and explain which symptoms warrant an emergency. |
| Reconcile the discharge plan of care with nationally accepted evidence-based guidelines. |
| Review the patient's medications; discuss any changes and potential adverse effects. |
| Talk to the patient about tests performed in the hospital and how to follow up on the results. |
| Telephone the patient two to three days after discharge to address concerns. |
MEDICATION REVIEW
Therapy with a combination of antiplatelets, statins, beta blockers, and ACE inhibitors has been shown to decrease mortality at six months in patients with ACS, with incremental benefit as more agents are used.37 Table 2 summarizes the most pertinent medications for post-MI care.6–10 Nonadherence to therapy is common and is associated with increased mortality risk; in a prospective cohort study, patients who discontinued use of medications by one month after an MI were nearly four times as likely to die by one year as those who adhered to therapy.38 Modifiable factors associated with medication self-discontinuation are highlighted in Table 3 and should be addressed before discharge.39
Table 2. Summary of Medications for the Subacute Management of Myocardial Infarction
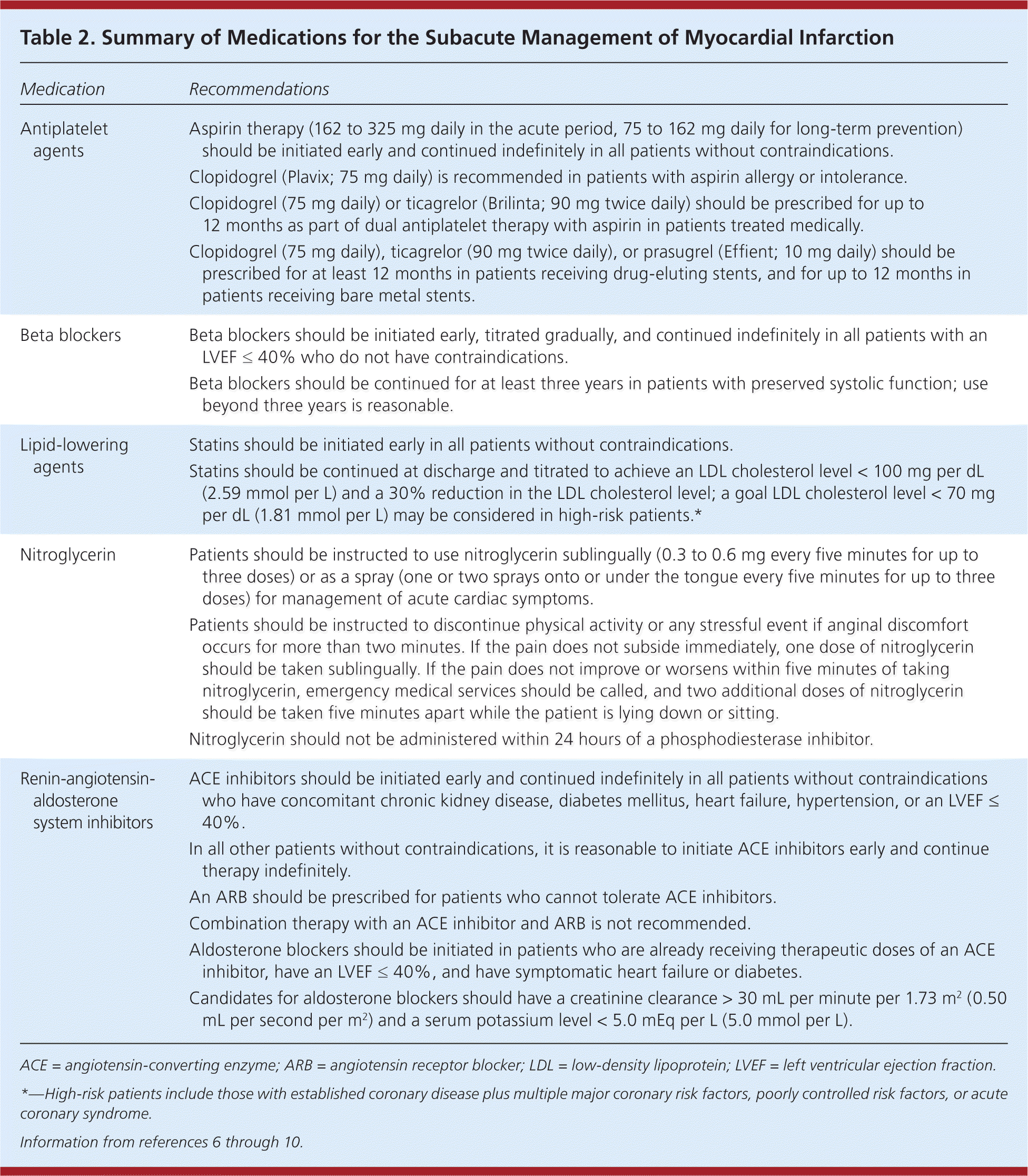
| Medication | Recommendations |
|---|---|
| Antiplatelet agents | Aspirin therapy (162 to 325 mg daily in the acute period, 75 to 162 mg daily for long-term prevention) should be initiated early and continued indefinitely in all patients without contraindications. |
| Clopidogrel (Plavix; 75 mg daily) is recommended in patients with aspirin allergy or intolerance. | |
| Clopidogrel (75 mg daily) or ticagrelor (Brilinta; 90 mg twice daily) should be prescribed for up to 12 months as part of dual antiplatelet therapy with aspirin in patients treated medically. | |
| Clopidogrel (75 mg daily), ticagrelor (90 mg twice daily), or prasugrel (Effient; 10 mg daily) should be prescribed for at least 12 months in patients receiving drug-eluting stents, and for up to 12 months in patients receiving bare metal stents. | |
| Beta blockers | Beta blockers should be initiated early, titrated gradually, and continued indefinitely in all patients with an LVEF ≤ 40% who do not have contraindications. |
| Beta blockers should be continued for at least three years in patients with preserved systolic function; use beyond three years is reasonable. | |
| Lipid-lowering agents | Statins should be initiated early in all patients without contraindications. |
| Statins should be continued at discharge and titrated to achieve an LDL cholesterol level < 100 mg per dL (2.59 mmol per L) and a 30% reduction in the LDL cholesterol level; a goal LDL cholesterol level < 70 mg per dL (1.81 mmol per L) may be considered in high-risk patients.* | |
| Nitroglycerin | Patients should be instructed to use nitroglycerin sublingually (0.3 to 0.6 mg every five minutes for up to three doses) or as a spray (one or two sprays onto or under the tongue every five minutes for up to three doses) for management of acute cardiac symptoms. |
| Patients should be instructed to discontinue physical activity or any stressful event if anginal discomfort occurs for more than two minutes. If the pain does not subside immediately, one dose of nitroglycerin should be taken sublingually. If the pain does not improve or worsens within five minutes of taking nitroglycerin, emergency medical services should be called, and two additional doses of nitroglycerin should be taken five minutes apart while the patient is lying down or sitting. | |
| Nitroglycerin should not be administered within 24 hours of a phosphodiesterase inhibitor. | |
| Renin-angiotensin-aldosterone system inhibitors | ACE inhibitors should be initiated early and continued indefinitely in all patients without contraindications who have concomitant chronic kidney disease, diabetes mellitus, heart failure, hypertension, or an LVEF ≤ 40%. |
| In all other patients without contraindications, it is reasonable to initiate ACE inhibitors early and continue therapy indefinitely. | |
| An ARB should be prescribed for patients who cannot tolerate ACE inhibitors. | |
| Combination therapy with an ACE inhibitor and ARB is not recommended. | |
| Aldosterone blockers should be initiated in patients who are already receiving therapeutic doses of an ACE inhibitor, have an LVEF ≤ 40%, and have symptomatic heart failure or diabetes. | |
| Candidates for aldosterone blockers should have a creatinine clearance > 30 mL per minute per 1.73 m2 (0.50 mL per second per m2) and a serum potassium level < 5.0 mEq per L (5.0 mmol per L). |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker; LDL = low-density lipoprotein; LVEF = left ventricular ejection fraction.
*—High-risk patients include those with established coronary disease plus multiple major coronary risk factors, poorly controlled risk factors, or acute coronary syndrome.
Table 3. Strategies to Prevent Medication Discontinuation Within 90 Days of an Acute Coronary Syndrome

| Avoid prescribing expensive medications when less expensive and equally effective alternatives are available. |
| Enroll the patient in a diet and exercise program. |
| Enroll the patient in a postdischarge comprehensive cardiac rehabilitation program. |
| Help the patient find programs that help pay for medications. |
| Minimize the number of medications given at discharge. |
| Schedule a follow-up appointment with a cardiologist. |
| Use a system of medication tracking (e.g., pillbox, calendar, alarm). |
Information from reference 39.
LIFESTYLE MODIFICATION COUNSELING
Crucial elements of lifestyle modification that should be discussed at discharge include diet, exercise, and smoking cessation. One study found that patients with ACS who did not adhere to dietary recommendations, remained sedentary, and continued to smoke at the 30-day follow-up had a fourfold increase in mortality within six months compared with those who adhered to all three components.40 Dietary counseling should include information about the Mediterranean diet, which has been shown to improve cardiovascular and all-cause mortality rates.41,42 Guidelines encourage setting a goal of at least 150 minutes per week of moderate-intensity aerobic activity, such as brisk walking.8 Smoking cessation rates improve in patients with cardiovascular disease when behavioral interventions are initiated in the hospital setting and are coupled with one month of supportive contact.43 The addition of nicotine replacement therapy increases the likelihood of cessation and is safe in patients with ACS.43,44
Postdischarge Interventions
CARDIAC REHABILITATION
The ACC and AHA recommend cardiac rehabilitation for patients with non–ST elevation MI or ST elevation MI.6,10 A Cochrane review found a 13% reduction in all-cause mortality and a 26% reduction in cardiovascular mortality in patients who underwent an exercise-based rehabilitation program, with similar results in those who underwent comprehensive (exercise and dietary management) programs.45 Specifically, reductions were noted in all-cause and cardiovascular mortality in patients who had follow-up at or beyond 12 months. In addition to their mortality benefit, these programs improve fitness, symptoms, lipid profiles, stress level, and overall well-being.46 Although benefits are clear, cardiac rehabilitation remains an underutilized resource. A Medicare claims data analysis found that it was used in only 14% of patients hospitalized for MI, emphasizing the need for its inclusion in a comprehensive discharge plan.47
ACTIVITY RECOMMENDATIONS
Guidelines from the ACC/AHA for management of non–ST elevation MI advise that patients may begin walking soon after discharge, resume sexual activity in as early as one week, and drive within three weeks after symptom resolution, although recovery times will vary depending on individual circumstances.6 Air travel should be avoided for two weeks unless the patient is symptom free, possesses nitroglycerin, has a traveling partner, and avoids situations requiring increased physical demands.6 After ST elevation MI, patients are encouraged to return to physical activity as tolerated, ideally with guidance after an exercise stress test.10
RECOGNITION OF CARDIAC SYMPTOMS
Patients who have had an MI and their families should be taught to recognize cardiac symptoms, initiate the emergency response system, and use prescribed nitroglycerin. Resources for cardiopulmonary resuscitation training programs should be readily available.10
FOLLOW-UP VISITS
Patients who have had an MI should have follow-up appointments prescheduled with their cardiologist and primary care physician, and these appointments should be included in the discharge summary. Components of an effective follow-up visit include a review of symptoms, medication reconciliation, cardiovascular risk assessment, psychosocial status (including screening for depression), activity limitations, and referrals to cardiac rehabilitation if not already done.10
Data Sources: A PubMed search was completed to include meta-analyses, randomized controlled trials, guidelines, and reviews limited to the English language. Search terms included unstable angina, non–ST segment elevation myocardial infarction, management guidelines, acute coronary syndrome, percutaneous coronary intervention, and transition of care. Also searched were Google Scholar, the Cochrane Database of Systematic Reviews, and Essential Evidence Plus. In addition, references from these sources and in UpToDate were searched. Search dates: January to May 2012, October 2012 to January 2013, and August 2013.

