There are approximately 20 million students in U.S. colleges and universities. Although this population is characterized as having good health, 600,000 students report some form of disability or some type of medical problem, including attention-deficit/hyperactivity disorder, learning disabilities, psychiatric disorders, and chronic illnesses, among others. Physicians can enhance youth transition to an adult model of health care; the use of self-care skills checklists is one recommended method to assist with the transition. Stimulant medications are effective for treating adults with attention-deficit/hyperactivity disorder, but physicians should use caution when prescribing stimulants to college students because of the high rates of medication diversion in this population. Depression, anxiety, posttraumatic stress disorder, sleep problems, and eating disorders are common in college students and can significantly impact performance. Emphasis on immunization of students for influenza, meningococcus, and pertussis is necessary because of the low rates of compliance. Screening and interventions for obesity, tobacco use, and substance abuse are important because of the high prevalence of these problems in college students. Screening for alcohol abuse facilitates identification of students with problem drinking behaviors. Students who are war veterans should be monitored for suicidal ideation and posttraumatic stress disorder. Lesbian, gay, bisexual, transgender, and questioning students are at risk of harassment and discrimination. Caution should be exercised when prescribing medications to college athletes to avoid violation of National Collegiate Athletic Association eligibility rules.
There are approximately 20 million full- and part-time students enrolled in American colleges and universities. Of these, 12 million are younger than 24 years, 56% are women, and 35% are minorities. Although this population is characterized as having good health, approximately 600,000 students report some form of disability or some type of medical problem, including attention-deficit/hyperactivity disorder (ADHD), learning disabilities, psychiatric disorders, and chronic illnesses, among others.1 Meeting the needs of the college student involves management of not only common illnesses and chronic conditions, but of behaviors and stressors that are unique to students. Common medical conditions in college students, which are treated in the same manner as in the general population, are addressed in Table 1.2
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A structured, coordinated health care transition from the child health care model to the adult health care model will optimize the care of college students. | C | 3 |
| Pharmacologic and cognitive behavior therapy demonstrate effectiveness in the treatment of attention-deficit/hyperactivity disorder in adults. | A | 12–16, 18 |
| Additional time on classroom tests and examinations is commonly encouraged for persons with attention-deficit/hyperactivity disorder or learning disabilities. | C | 19 |
| Tobacco use screening and cessation interventions are recommended for college students. | B | 36 |
| Alcohol use and misuse counseling is recommended for college students. | B | 39–41 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Table 1. Common Self-Reported Medical Conditions in College Students

| Condition | Frequency (%) | Comment |
|---|---|---|
| Acute or chronic conditions | ||
| Allergies | 22 |
|
| Sinus infection | 17 | |
| Back pain | 12 | |
| Strep throat | 11 | |
| Asthma | 9 | |
| Urinary tract infection | 9 | |
| Broken bone/fracture/sprain | 8 | |
| Ear infection | 7.5 | |
| Migraine | 7 | |
| Bronchitis | 6 | |
| Disabling conditions | ||
| Attention-deficit/hyperactivity disorder | 6 |
|
| Learning disability | 4 |
|
| Psychiatric condition | 4 |
|
| Chronic illness (e.g., cancer, diabetes mellitus, autoimmune disorders) | 3.5 |
|
| Deaf/hard of hearing | 1.5 | |
| Partially sighted/blind | 1.5 | |
| Mobility/dexterity disability | 1 | |
| Speech or language disorder | 1 | |
| Other disability | 2 | |
NOTE : 94% of male students and 91% of female students describe their health as good, very good, or excellent.
Information from reference 2.
Preparing for the Transition to College
HEALTH CARE INDEPENDENCE
College students often are assuming primary responsibility for their education and health for the first time. Promoting health care independence involves more than the provision of the medical record and immunization history. A structured, coordinated health care transition plan from the child to the adult health care model will optimize the care of college students.3 Figure 1 is a health care transition planning algorithm developed by the American Academy of Family Physicians (AAFP), American Academy of Pediatrics, and American College of Physicians.3
Figure 1. Health Care Transition Planning for Youth and Young Adults
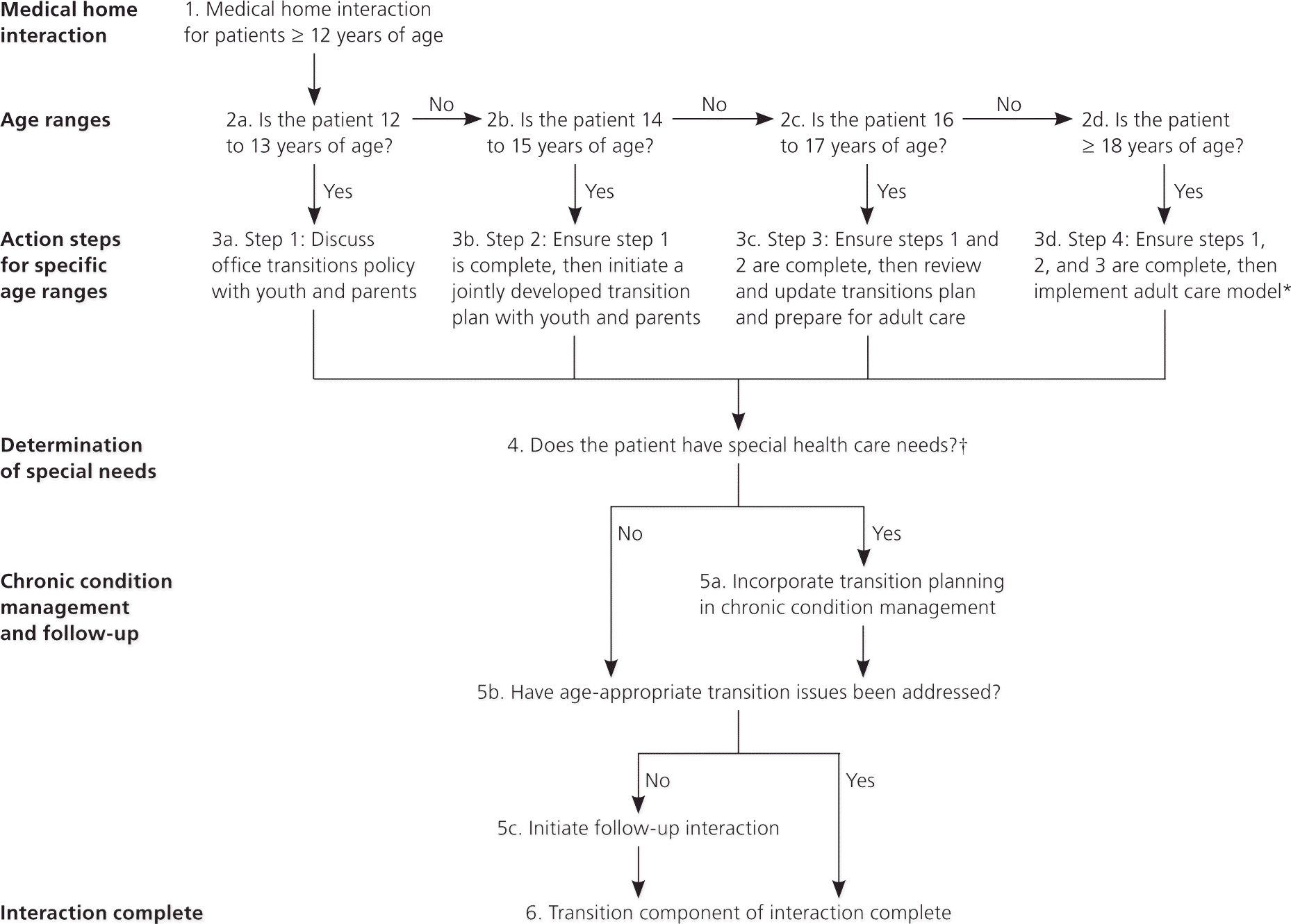
Health care transition planning algorithm for all youth and young adults within a medical home interaction.
Adapted from Cooley WC, Sagerman PJ; American Academy of Pediatrics; American Academy of Family Physicians; American College of Physicians; Transitions Clinical Report Authoring Group. Supporting the health care transition from adolescence to adulthood in the medical home. Pediatrics. 2011;128(1):185–186. Copyright © 2011 by the AAP.
The “sending” medical practice should ensure that the departing student has a transition plan, and that the family and student are ready for the transition. A transition checklist for clinicians is provided in Table 2. A health care skills checklist (eFigure A) is one recommended method to assess the needs of the patient and to develop goals for the transition to a health care model that expects assumption of adult responsibilities. Group visits to complete the clinical and educational activities for transitioning students could be considered to enhance counseling efficiency. “Receiving” practices should assess the developmental readiness of the student and respond accordingly, orienting the student to the clinical practice and adult health care model. Ideally, some students would benefit from direct coordination of care with the college or university student health service.
Table 2. Clinician Checklist for Transitioning College Students

| Meet privately with the patient for part of the visit | |
| Encourage assumption of increased responsibility for his/her health care management: | |
| Ensure that the patient understands his/her health conditions and medications | |
| Send copies of reports, letters, and tests to the patient and his/her family | |
| Provide anticipatory guidance: | |
| Nutrition and fitness | |
| Sexuality and relationships | |
| Substance abuse and smoking | |
| Specific health condition(s):________________ | |
| Health insurance | |
| Sports/athletics | |
| Functional independence | |
| College/work plans | |
| Functional independence and community inclusion (for patients with disabilities) | |
| Medical decision making/privacy at age of majority (state specific) | |
| Legal matters (e.g., advance medical directive, power of attorney) | |
| Voting/selective service | |
| Assess patient and family readiness for transfer to a new physician: | |
| Initiate discussion about transfer to adult health care model | |
| Identify possible physician | |
| Initiate communication with the physician selected | |
| Implement the transfer to the new practice: | |
| Transfer medical records | |
| Discuss nuances of care with the selected physician or clinic | |
| Follow-up after the transfer | |
| Assess the patient's ability to make independent decisions regarding health care, finances, and other adult concerns to determine whether there is a need for guardianship or conservatorship | |
| Provide a pocket card of conditions and medications | |
eFigure A. Health Care Skills and Supplies: A Checklist for the College Student
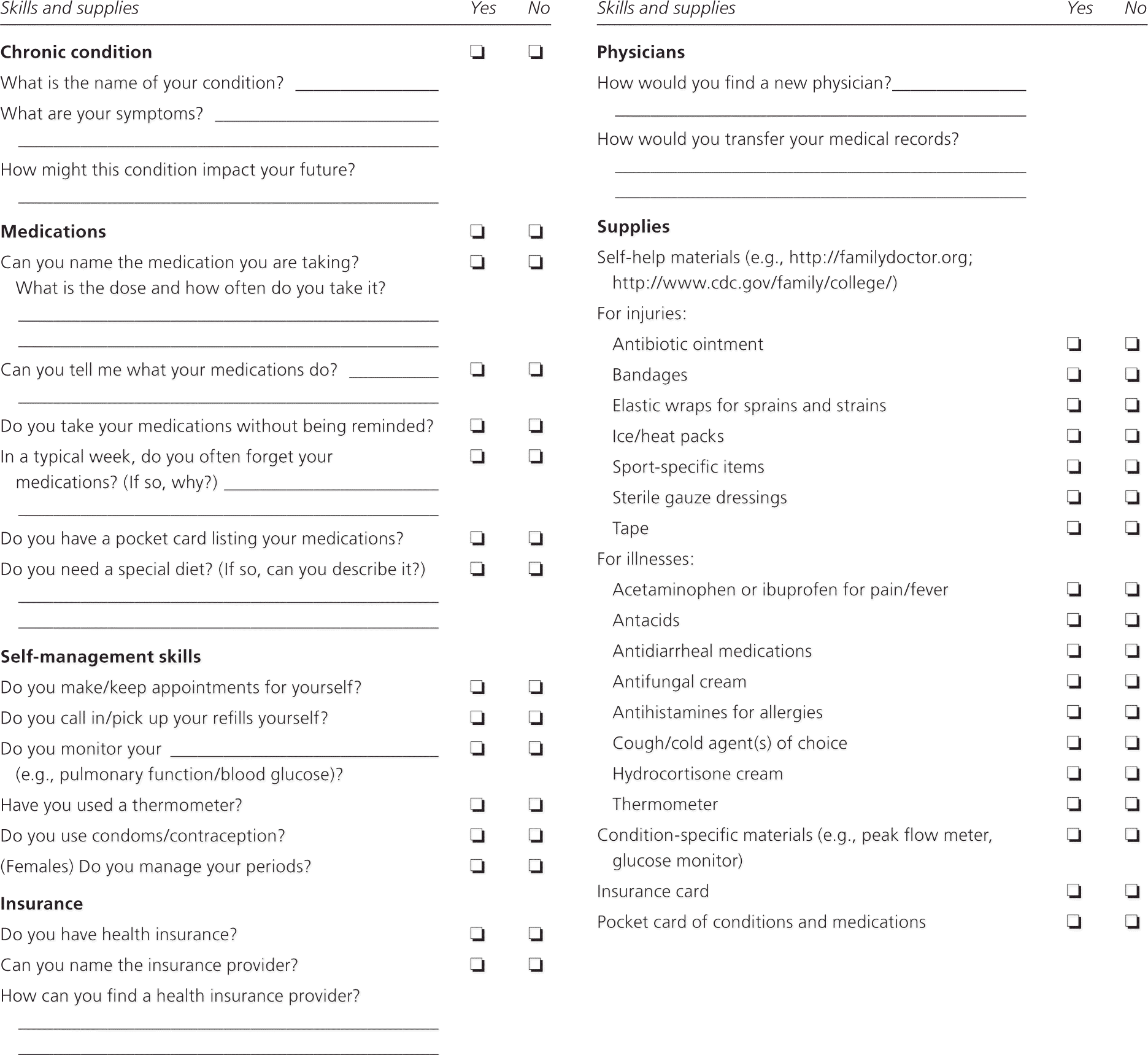
A health care skills checklist is one recommended method to assess the needs of the patient and to develop goals for the transition to a health care model that expects assumption of adult responsibilities.
Health care independence is also fostered by availability of medical self-help books and online resources, such as FamilyDoctor. org (https://familydoctor.org), and by basic medical supplies to handle common medical problems and injuries. The Centers for Disease Control and Prevention provides useful health resources for college students and their families at http://www.cdc.gov/family/college.
HEALTH CARE COVERAGE
Most college students (64%) have health insurance through their parents' plan, and another 13% are covered by college/university-sponsored plans. Approximately 9% are uninsured.4 Although student health insurance coverage requirements under the Affordable Care Act provide certain protections to the college student, there is still diversity among available plans. It is incumbent on students to have a working knowledge of their insurance plan, coverage, and claims process. Coverage of vaccinations and contraceptives varies by plan.5 A health care insurance toolkit for young adults is available at http://www.gettingcovered.org/Toolkit.
Common Learning and Mental Health Concerns
LEARNING ISSUES
Attention-Deficit/Hyperactivity Disorder. The prevalence of ADHD among college students is estimated to be 2% to 8%6,7; 50% of students receiving accommodative services in college demonstrate ADHD.8 Students with symptoms of ADHD are at increased risk of psychosocial and substance use problems.9
Adolescents and young adults who have ADHD demonstrate less hyperactivity, but report more mental restlessness, anxiety, irritability, and academic, social, mood, and sleep problems compared with children who have ADHD.10,11 Higher demands on executive function and less direct social support from family contribute to struggling and the need for pharmacologic and nonpharmacologic interventions in students who were previously undiagnosed.
Pharmacotherapy, including amphetamines, methylphenidate (Ritalin), bupropion (Wellbutrin), and atomoxetine (Strattera), is effective in adults.12–15 Stimulant medications are more effective than nonstimulant medications for treating adult ADHD.16 Few studies have examined the effectiveness of these medications specifically in college students.
Cognitive behavior therapy for ADHD focuses on teaching patients ways to adapt their thinking and behaviors to increase daily functioning. When used in conjunction with medication, cognitive behavior therapy improves functioning and ADHD symptoms in adults17; it is unknown whether these findings can be generalized to college students.
In treating ADHD, an additional concern specific to college students is stimulant misuse; 5% to 35% of college students misuse or divert their ADHD medications.18 Those with a history of substance abuse or conduct disorder may be more likely to misuse or divert their medications.18 Educating recipients of prescribed stimulants and remaining vigilant for misuse among high-risk students may be helpful.6
Learning Disabilities. About 3% of college students surveyed report having a learning disability.7 Physicians may discover learning disabilities when evaluating students for other conditions, such as depression, sleep disorders, ADHD, and thyroid disease. There is no consensus regarding how to assess learning disabilities in college students,19 and the lack of agreement on the definition of a learning disability has resulted in few evidence-based treatment strategies. Given the difficulties associated with treatment of learning disabilities, educational accommodations are important to consider. Allowing students with ADHD or learning disabilities more time on classroom tests and examinations is commonly encouraged, and physicians may be approached to write medical statements requesting this accommodation on behalf of the patient.19 However, there are limited data suggesting that such accommodations significantly improve performance. Students with learning disabilities typically have their condition comanaged by their physician, psychologists, and educators.
SELECTED MENTAL HEALTH AND BEHAVIORAL PROBLEMS
Physicians should be alert for depression, anxiety, suicidal ideation, posttraumatic stress disorder (PTSD), and sleep and eating disorders, because they are highly prevalent in college students. Detailed information about treatment is widely available and does not differ from that for the general population.
Anxiety and Depression. Anxiety and depression, which can have a significant impact on academic performance, are the most common mental health problems reported by college students.7 Within the previous 12 months, 30.7% felt so depressed that it was difficult to function and 48.4% experienced overwhelming anxiety. Less than one-half of students experiencing depressive and anxiety symptoms seek care.20
Suicidal Ideation. Recent data suggest that suicide is the most common cause of death in college students.21 Suicidal ideation is reported in nearly 7% of students; about 2% report having a plan, and 0.5% report making an attempt in the previous year.22 Of those with suicidal ideation, approximately 50% seek help. Depression, low social support, parent-student conflict, affective dysregulation, and alcohol use disorders are risk factors for suicidal ideation.23 Systematic reviews conclude that there is insufficient evidence regarding psychosocial and pharmacologic treatments for suicide-related behaviors.24 Family physicians should be particularly vigilant for suicidal thoughts and behaviors in college students, and should direct students to outpatient care if there is no immediate risk. Information and resources about suicide are available at http://www.sprc.org/collegesanduniversities.
Posttraumatic Stress Disorder. Most students report experiencing a traumatic event in their lifetime.25 Probable PTSD is most commonly associated with sexual assault.25,26 Although it has not been tested in college settings, the Primary Care PTSD Screen, a four-item screening tool, may be useful for identifying students experiencing PTSD symptoms.27–29
Sleep Disorders. Studies suggest that as many as 60% of college students report poor sleep quality,30 and sleep difficulties impact academic performance in 20% of college students.7 Sleep deprivation is associated with impaired cognitive functioning, mood problems, somatic symptoms, and decreased life satisfaction, and is a risk factor for illicit substance and alcohol use and motor vehicle crashes.31 Inadequate sleep hygiene, delayed sleep phase disorder, and insomnia are the most common sleep disorders in college students.31
Eating Disorders. About 1% of surveyed college students report that an eating disorder affected their performance.7 Self-help programs, cognitive behavior therapy, and interpersonal therapy have good evidence for treating bulimia nervosa and binge eating disorder. Antidepressants may be a primary treatment for bulimia nervosa, and anorexia nervosa should be treated in a tertiary care setting.32
Preventive Measures
IMMUNIZATIONS
College entrance physical examinations and routine visits provide opportunities for updating and administering immunizations. The 2010 National College Health Assessment indicated that only 40% of college students report receiving influenza vaccinations, and only 55% report receiving meningococcal vaccinations.4 Adequate pertussis immunization has also received national emphasis.
Current immunization schedules for adolescents and adults are provided by the AAFP (https://www.aafp.org/patient-care/immunizations/schedules.html) and the Advisory Committee on Immunization Practices (http://www.cdc.gov/vaccines/acip/recs/index.html).33
EVIDENCE-BASED PREVENTIVE RECOMMENDATIONS
The AAFP and the U.S. Preventive Services Task Force have general recommendations that are applicable to college students. The focus of these recommendations is on counseling to reduce the risk-taking behaviors more common in young adults. Additionally, U.S. Preventive Services Task Force guidelines focus on lifestyle choices related to diet, exercise, and healthy relationships that are amenable to counseling and modification when intervention occurs before obesity, inactivity, and unhealthy relationships become habits.
Obesity is an epidemic on college campuses.3 During the first year of college, students gain an average of 3.9 lb (1.8 kg).34 Systematic approaches to target obesity on college campuses are fragmented and have not been reviewed. Physicians should refer students to student health centers offering weight control services.35
Tobacco use is also common in this population.4 Evidence-based recommendations for targeting tobacco use among adolescents, including tobacco use screening and cessation interventions, apply to college students.36
Alcohol use and abuse are common in college students.4 Among those who consumed alcohol, 51% reported that within the previous 12 months they experienced some negative consequence associated with their alcohol consumption.4 Two primary subsets of college students are at greatest risk of problem drinking. The first subset consists of white, male, sensation-seeking students engaged in a social environment with a high drinking norm (e.g., Greek organizations). The second subset consists of female students who were more likely to experience negative affect and respond to distress by drinking.37
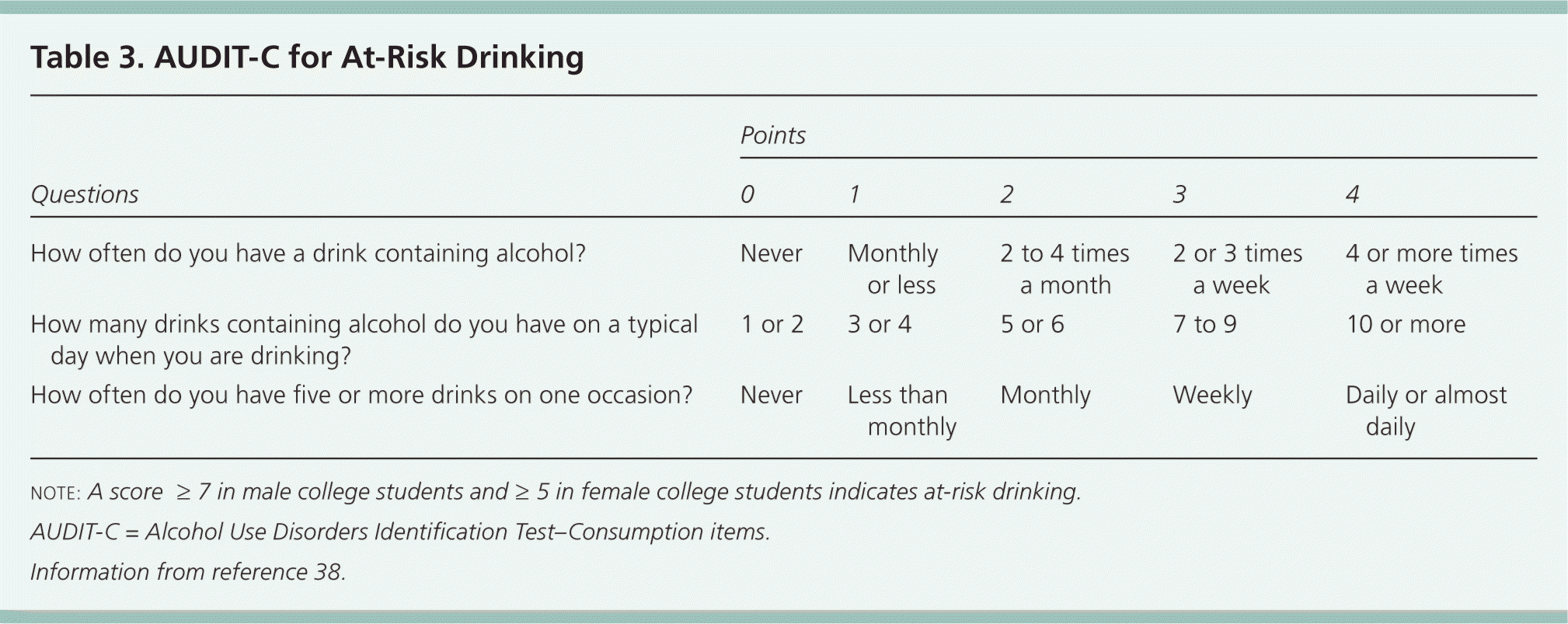
Screening for alcohol abuse facilitates identification of students with problem drinking behaviors. The first three consumption items of the Alcohol Use Disorders Identification Test (AUDIT-C ; Table 3) are recommended for identifying at-risk drinking among college students, using a cutoff score of 7 for males and 5 for females.38 Effective intervention programs increase motivation to change drinking habits, change expectations about the effects of alcohol, provide face-to-face or computer-based feedback on student-based norms of drinking behavior, emphasize cognitive behavior skills training, and offer a plan for reducing alcohol use.39,40 Ineffective programs include efforts to increase basic awareness and provide education.39,40 Mailed feedback, social marketing, and group feedback are also not effective.41 The website College Drinking–Changing the Culture (http://www.collegedrinkingprevention.gov) provides updated, evidence-based information about the prevention, assessment, and treatment of alcohol abuse in college settings.
Table 3. AUDIT-C for At-Risk Drinking
| Questions | Points | ||||
|---|---|---|---|---|---|
| 0 | 1 | 2 | 3 | 4 | |
| How often do you have a drink containing alcohol? | Never | Monthly or less | 2 to 4 times a month | 2 or 3 times a week | 4 or more times a week |
| How many drinks containing alcohol do you have on a typical day when you are drinking? | 1 or 2 | 3 or 4 | 5 or 6 | 7 to 9 | 10 or more |
| How often do you have five or more drinks on one occasion? | Never | Less than monthly | Monthly | Weekly | Daily or almost daily |
NOTE: A score ≥ 7 in male college students and ≥ 5 in female college students indicates at-risk drinking.
AUDIT-C = Alcohol Use Disorders Identification Test–Consumption items.
Information from reference 38.
Use of illicit substances can complicate the diagnosis and treatment of academic or behavioral health conditions. Marijuana is the most commonly used illicit substance on college campuses.3 Other common illicit substances are listed in Table 4.42 Guidelines for providing drug education and administring drug testing are published by the American College Health Association (http://www.acha.org/Topics/atod.cfm).
Table 4. Illicit Substances Commonly Used on College Campuses

| Drug name | Street name | Form | Psychoactive effect | Adverse effects |
|---|---|---|---|---|
| Cocaine | Blow, snow, king's habit, coke | Snorted, injected, smoked | Stimulant | Hypertension, tachycardia, anosmia, rhinorrhea, bloody nose, paranoia, stroke, seizures |
| Flunitrazepam (Rohypnol) | Roofies, rophies, roche, Mexican valium, forget-me pill | Pill (taken orally or ground up and snorted) | Central nervous system depressant | Sedation, amnesia |
| Gamma-hydroxybutyrate (GHB) | Liquid X, liquid ecstasy, soap, easy lay, Georgia home boy, grievous bodily harm, G, goop | Liquid or powder (often mixed with alcohol and other beverages) | Central nervous system depressant | Sedation, euphoria, loss of consciousness, hallucinations, amnesia |
| Ketamine | Special K, vitamin K, cat valium | Snorted, intramuscular injection | Dissociative anesthetic | Hallucinations, psychosis, nausea, vomiting, hypertension, tachycardia |
| Marijuana (delta-9-tetrahydrocannabinol [THC]) | Pot, ganja, weed, grass, reefer, Mary Jane (MJ) | Smoked (joints, water pipes, bongs, blunts), swallowed | Cannabinoid | Euphoria, palpitations, impaired cognition, sedation, increased appetite |
| Methamphetamine | Speed, meth, ice, chalk, crystal, glass, crank, fire | Powder (orally, snorted, injected), crystals(heated and smoked) | Stimulant | Palpitations, tachycardia, restlessness, insomnia, anorexia, gastrointestinal upset, seizures, headaches |
| Methylenedioxymethamphetamine (MDMA) | Ecstasy, E, XTC, X Adam, hug, beans, clarity, lover's speed, love drug | Pill, tablet, or capsule, often of different colors and with cartoon-like images | Multiple | Stimulant, hallucinogen, depression, anxiety, sleep problems |
Information from reference 42.
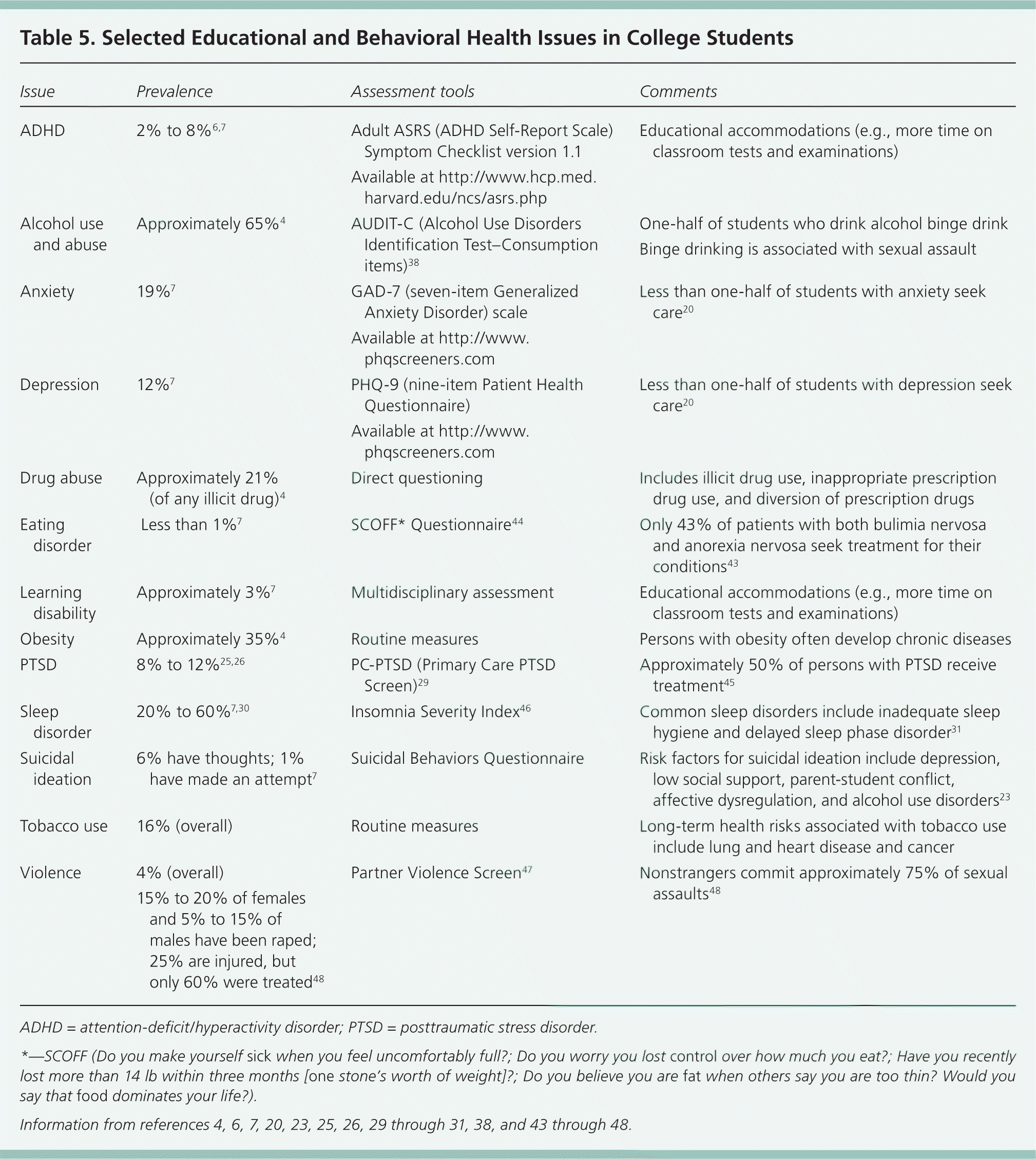
Table 5 lists common educational and behavioral health issues for college students, and primary care assessment tools that can be used for examination.4,6,7,20,23,25,26,29–31,38,43–48
Table 5. Selected Educational and Behavioral Health Issues in College Students
| Issue | Prevalence | Assessment tools | Comments |
|---|---|---|---|
| ADHD | 2% to 8%6,7 | Adult ASRS (ADHD Self-Report Scale) Symptom Checklist version 1.1 | Educational accommodations (e.g., more time on classroom tests and examinations) |
| Available at http://www.hcp.med.harvard.edu/ncs/asrs.php | |||
| Alcohol use and abuse | Approximately 65%4 | AUDIT-C (Alcohol Use Disorders Identification Test–Consumption items)38 | One-half of students who drink alcohol binge drink Binge drinking is associated with sexual assault |
| Anxiety | 19%7 | GAD-7 (seven-item Generalized Anxiety Disorder) scale Available at http://www.phqscreeners.com | Less than one-half of students with anxiety seek care20 |
| Depression | 12%7 | PHQ-9 (nine-item Patient Health Questionnaire) | Less than one-half of students with depression seek care20 |
| Available at http://www.phqscreeners.com | |||
| Drug abuse | Approximately 21% (of any illicit drug)4 | Direct questioning | Includes illicit drug use, inappropriate prescription drug use, and diversion of prescription drugs |
| Eating disorder | Less than 1%7 | SCOFF* Questionnaire44 | Only 43% of patients with both bulimia nervosa and anorexia nervosa seek treatment for their conditions43 |
| Learning disability | Approximately 3%7 | Multidisciplinary assessment | Educational accommodations (e.g., more time on classroom tests and examinations) |
| Obesity | Approximately 35%4 | Routine measures | Persons with obesity often develop chronic diseases |
| PTSD | 8% to 12%25,26 | PC-PTSD (Primary Care PTSD Screen)29 | Approximately 50% of persons with PTSD receive treatment45 |
| Sleep disorder | 20% to 60%7,30 | Insomnia Severity Index46 | Common sleep disorders include inadequate sleep hygiene and delayed sleep phase disorder31 |
| Suicidal ideation | 6% have thoughts; 1% have made an attempt7 | Suicidal Behaviors Questionnaire | Risk factors for suicidal ideation include depression, low social support, parent-student conflict, affective dysregulation, and alcohol use disorders23 |
| Tobacco use | 16% (overall) | Routine measures | Long-term health risks associated with tobacco use include lung and heart disease and cancer |
| Violence | 4% (overall) | Partner Violence Screen47 | Nonstrangers commit approximately 75% of sexual assaults48 |
| 15% to 20% of females and 5% to 15% of males have been raped; 25% are injured, but only 60% were treated48 |
ADHD = attention-deficit/hyperactivity disorder; PTSD = posttraumatic stress disorder.
*—SCOFF (Do you make yourself sick when you feel uncomfortably full?; Do you worry you lost control over how much you eat?; Have you recently lost more than 14 lb within three months [one stone's worth of weight]?; Do you believe you are fat when others say you are too thin? Would you say that food dominates your life?).
Information from references 4, 6, 7, 20, 23, 25, 26, 29 through 31, 38, and 43 through 48.
Special Populations
On college campuses, approximately 8% of students describe their sexual orientation as lesbian, gay, bisexual, transgender, or “unsure.” 7 These students report more harassment and discrimination, and have more negative perceptions of campus climates compared with heterosexual men and women.49 The Gay and Lesbian Medical Association published guidelines for caring for lesbian, gay, bisexual, transgender, and questioning patients, which can be found at http://www.glma.org/index.cfm?fuseaction=Page.viewPage&pageId=1037&parentID=568&nodeID=1.
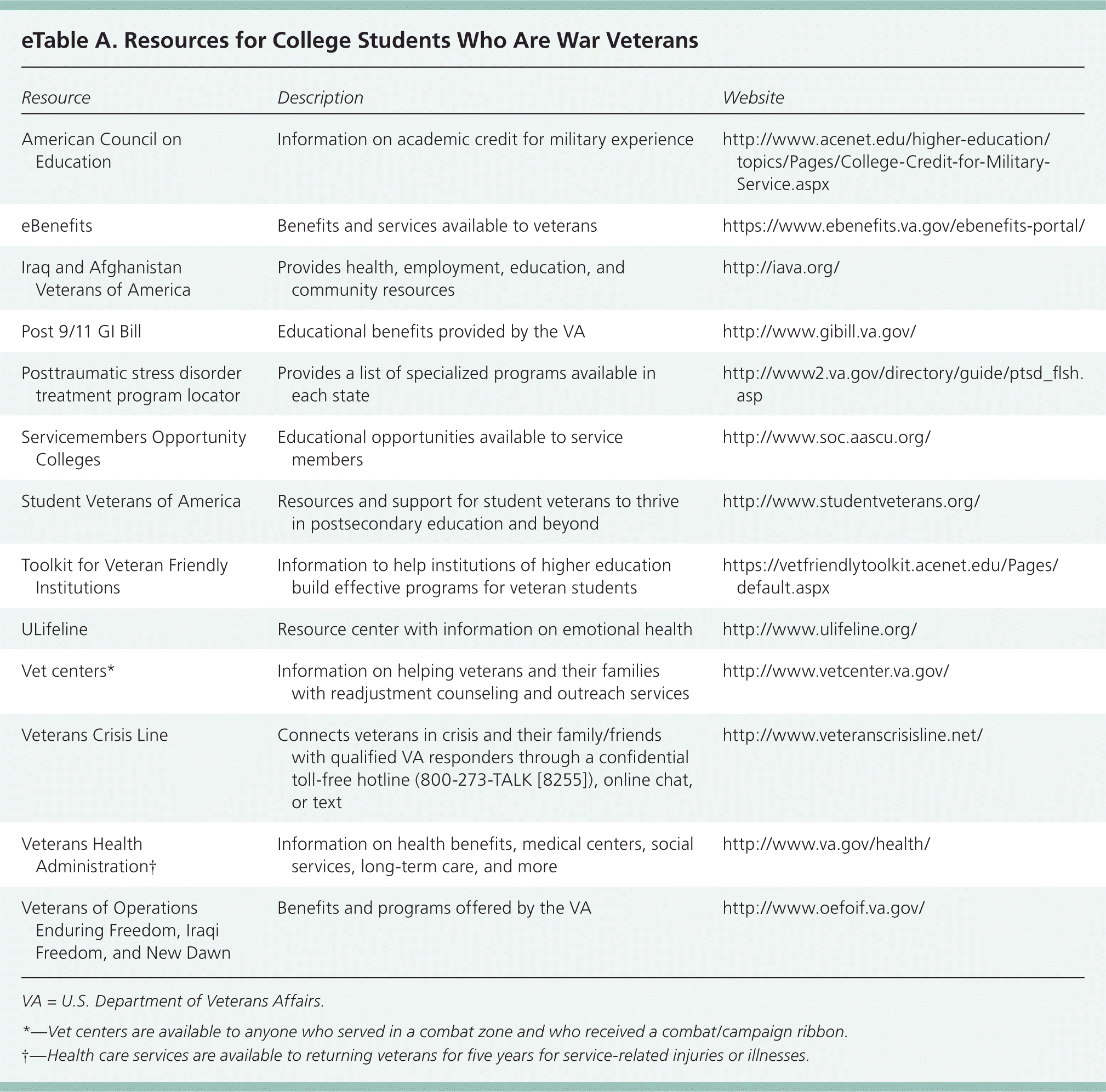
Students who are war veterans demonstrate high levels of suicidal ideation (46%), and many report having a plan (20%) and think that they are likely or very likely to commit suicide (approximately 4%).50 Student veterans with PTSD were more likely to report being in in a physical fight during the previous 12 months, and were more likely to participate in high-risk drinking.51 Student veterans should be monitored for suicidal ideation and PTSD. The Primary Care PTSD Screen is available at http://www.ptsd.va.gov/professional/pages/assessments/pc-ptsd.asp.29 Organizations such as the Student Veterans of America (http://www.studentveterans.org) may help student veterans connect with resources and students with similar backgrounds. eTable A lists resources for student veterans.
eTable A. Resources for College Students Who Are War Veterans
| Resource | Description | Website |
|---|---|---|
| American Council on Education | Information on academic credit for military experience | http://www.acenet.edu/higher-education/topics/Pages/College-Credit-for-Military-Service.aspx |
| eBenefits | Benefits and services available to veterans | https://www.ebenefits.va.gov/ebenefits-portal/ |
| Iraq and Afghanistan Veterans of America | Provides health, employment, education, and community resources | http://iava.org/ |
| Post 9/11 GI Bill | Educational benefits provided by the VA | http://www.gibill.va.gov/ |
| Posttraumatic stress disorder treatment program locator | Provides a list of specialized programs available in each state | http://www2.va.gov/directory/guide/ptsd_flsh.asp |
| Servicemembers Opportunity Colleges | Educational opportunities available to service members | http://www.soc.aascu.org/ |
| Student Veterans of America | Resources and support for student veterans to thrive in postsecondary education and beyond | http://www.studentveterans.org/ |
| Toolkit for Veteran Friendly Institutions | Information to help institutions of higher education build effective programs for veteran students | https://vetfriendlytoolkit.acenet.edu/Pages/default.aspx |
| ULifeline | Resource center with information on emotional health | http://www.ulifeline.org/ |
| Vet centers* | Information on helping veterans and their families with readjustment counseling and outreach services | http://www.vetcenter.va.gov/ |
| Veterans Crisis Line | Connects veterans in crisis and their family/friends with qualified VA responders through a confidential toll-free hotline (800-273-TALK [8255]), online chat, or text | http://www.veteranscrisisline.net/ |
| Veterans Health Administration† | Information on health benefits, medical centers, social services, long-term care, and more | http://www.va.gov/health/ |
| Veterans of Operations Enduring Freedom, Iraqi Freedom, and New Dawn | Benefits and programs offered by the VA | http://www.oefoif.va.gov/ |
VA = U.S. Department of Veterans Affairs.
*—Vet centers are available to anyone who served in a combat zone and who received a combat/campaign ribbon.
†—Health care services are available to returning veterans for five years for service-related injuries or illnesses.
Student athletes are not only at higher risk of sports-related injuries, but also of loss of eligibility because of inadvertent violation of National Collegiate Athletic Association (NCAA) rules related to the use of supplements, over-the-counter medications, and prescription drugs. Current rules and standards are available at http://www.ncaa.org/wps/wcm/connect/public/ncaa/ssi/policy/drug+testing+landing+page. eTable B lists banned drugs, restricted drugs, and drugs that can be used after a formal medical exception is processed with the NCAA. Athletes should be counseled to clear the use of all dietary supplements and over-the-counter medications with their team medical staff or a physician so as not to inadvertently violate NCAA rules.
eTable B. NCAA Banned and Restricted Drugs
| Drug | Status |
|---|---|
| Anabolic agents | Banned |
| Antiestrogens (aromatase inhibitors) | Banned |
| Possible medical exception: permitted if required for treatment of specific endocrinopathy | |
| Beta2 agonists | Banned |
| Possible medical exception: permitted for inhalation to treat asthma | |
| Beta blockers | Banned for rifle only |
| Caffeine | Concentrations in urine cannot be greater than 15 mcg per mL |
| Diuretics | Banned |
| Possible medical exception: if no appropriate alternative available | |
| Glucocorticoids | Prohibited in competition |
| Possible medical exception: permitted for specific short-term indication | |
| Hormones (growth hormone and erythropoietin) | Banned |
| Stimulants | Banned |
| Possible medical exception: for attention-deficit/hyperactivity disorder treatment (strict enforcement) |
NCAA = National Collegiate Athletic Association.
Information from National Collegiate Athletic Association. NCAA banned drug list. http://www.ncaa.org/wps/wcm/connect/public/ncaa/health+and+safety/drug+testing/resources/ncaa+banned+drugs+list. Accessed March 20, 2012.
Data Sources: Specific, evidence-based research on college students is relatively limited. We used PubMed as the primary literature search engine. Key words: college student and university student, plus the selected content (e.g., alcohol, tobacco). Key sources of data: American College Health Association, Essential Evidence, review articles in American Family Physician, federal reports on selected content, Cochrane reviews. Search dates: April 2011 through March 2012, and August 2012 through October 2012.

