Onychomycosis is a fungal infection of the nails that causes discoloration, thickening, and separation from the nail bed. Onychomycosis occurs in 10% of the general population, 20% of persons older than 60 years, and 50% of those older than 70 years. It is caused by a variety of organisms, but most cases are caused by dermatophytes. Accurate diagnosis involves physical and microscopic examination and culture. Histologic evaluation using periodic acid–Schiff staining increases sensitivity for detecting infection. Treatment is aimed at eradication of the causative organism and return to a normal appearance of the nail. Systemic antifungals are the most effective treatment, with meta-analyses showing mycotic cure rates of 76% for terbinafine, 63% for itraconazole with pulse dosing, 59% for itraconazole with continuous dosing, and 48% for fluconazole. Concomitant nail debridement further increases cure rates. Topical therapy with ciclopirox is less effective; it has a failure rate exceeding 60%. Several nonprescription treatments have also been evaluated. Laser and photodynamic therapies show promise based on in-vitro evaluation, but more clinical studies are needed. Despite treatment, the recurrence rate of onychomycosis is 10% to 50% as a result of reinfection or lack of mycotic cure.
Onychomycosis is a fungal infection of the fingernails or toenails that causes discoloration, thickening, and separation from the nail bed. Onychomycosis occurs in 10% of the general population but is more common in older adults; the prevalence is 20% in those older than 60 years and 50% in those older than 70 years.1 The increased prevalence in older adults is related to peripheral vascular disease, immunologic disorders, and diabetes mellitus. The risk of onychomycosis is 1.9 to 2.8 times higher in persons with diabetes compared with the general population.2 In patients with human immunodeficiency virus infection, the prevalence ranges from 15% to 40%.3
Onychomycosis affects toenails more often than fingernails because of their slower growth, reduced blood supply, and frequent confinement in dark, moist environments. It may occur in patients with distorted nails, a history of nail trauma, genetic predisposition, hyperhidrosis, concurrent fungal infections, and psoriasis. It is also more common in smokers and in those who use occlusive footwear and shared bathing facilities.1,4
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| When preparing a nail specimen to test for onychomycosis, the nail should be cleaned with 70% isopropyl alcohol, then samples of the subungual debris and eight to 10 nail clippings should be obtained. The specimen should be placed on a microscope slide with a drop of potassium hydroxide 10% to 20% solution, then allowed to sit for at least five minutes before viewing under a microscope. | C | 8, 11 |
| Periodic acid–Schiff staining should be ordered to confirm infection in patients with suspected onychomycosis. | C | 14 |
| Systemic antifungal agents are the most effective treatment for onychomycosis, but cure rates are much less than 100%. Terbinafine (Lamisil) is the most effective systemic agent available. | C | 23 |
| When prescribing the topical agent ciclopirox, patients should be informed that it has some benefit in the treatment of onychomycosis, but also has a high failure rate. | C | 28, 31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Microbiology
Onychomycosis is caused by various organisms, most often dermatophytes of the genus Trichophyton. Other organisms include Candida, which is more common in fingernail infections (eFigure A) and in patients with chronic mucocutaneous candidiasis.1 Nondermatophyte molds are a less common cause in the general population. Recent studies, however, have demonstrated that they are the predominant organisms in patients with onychomycosis and human immunodeficiency virus infection3 (eTable A).
eFigure A.
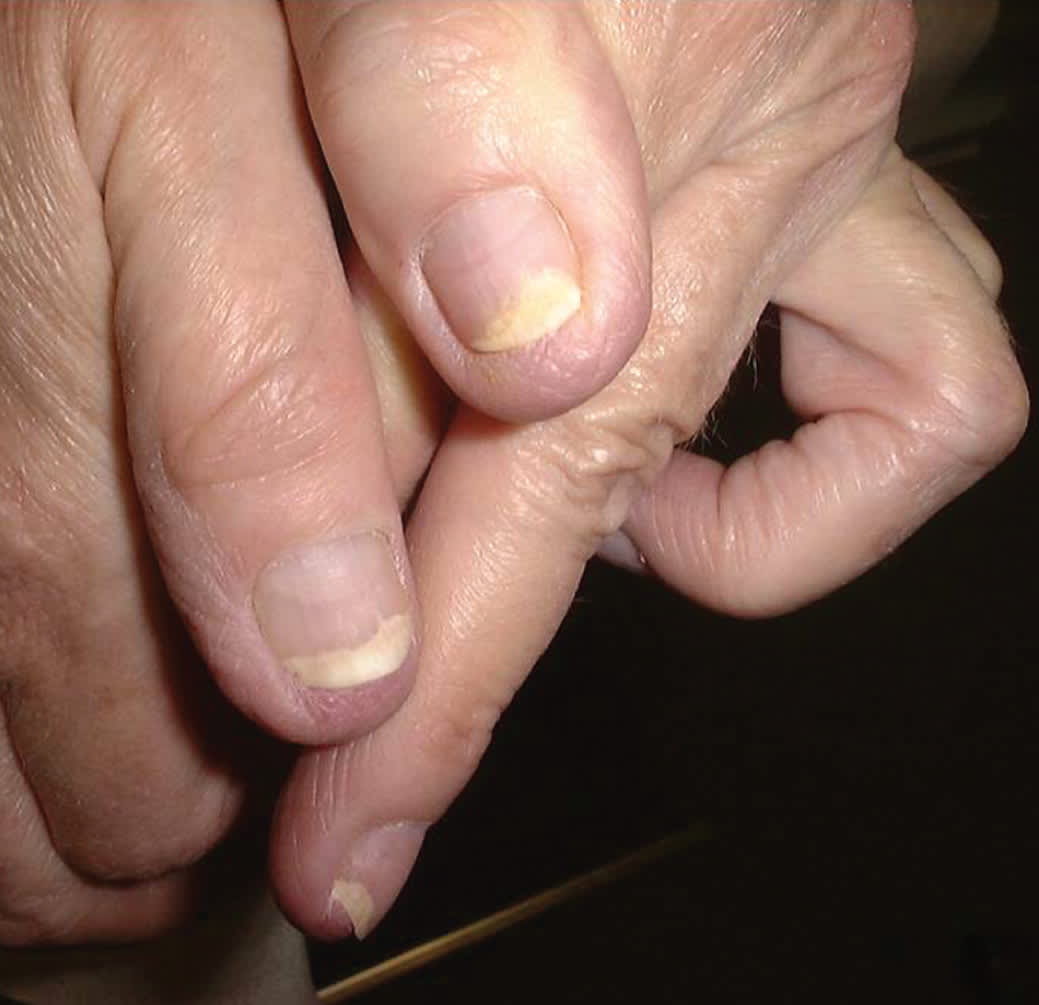
Candidal subungual onychomycosis.
Photo provided by Robert T. Brodell, MD.
eTable A. Common Pathogens in Onychomycosis

| Dermatophytes (80% to 90%) |
| Epidermophyton floccosum |
| Microsporum species |
| Trichophyton interdigitale |
| Trichophyton mentagrophytes |
| Trichophyton rubrum |
| Trichophyton tonsurans |
| Nondermatophyte molds (2% to 10%)* |
| Acremonium species |
| Alternaria species |
| Aspergillus species |
| Cladosporium carrionii |
| Fusarium species |
| Geotrichum candidum |
| Lasiodiplodia theobromae |
| Onychocola species |
| Scopulariopsis species |
| Scytalidium species |
| Yeast (2% to 11%) |
| Candida albicans |
| Candida guilliermondii |
| Candida parapsilosis |
*—Nondermatophyte molds are the predominant organism in patients with human immunodeficiency virus infection.
Information from:
Alberhasky RC. Laboratory diagnosis of onychomycosis. Clin Podiatr Med Surg. 2004;21(4):565–578, vi.
Kaur R, Kashyap B, Bhalla P. Onychomycosis—epidemiology, diagnosis and management. Indian J Med Microbiol. 2008;26(2):108–116.
Surjushe A, Kamath R, Oberai C, et al. A clinical and mycological study of onychomycosis in HIV infection. Indian J Dermatol Venereol Leprol. 2007;73(6):397–401.
Welsh O, Vera-Cabrera L, Welsh E. Onychomycosis. Clin Dermatol. 2010;28(2):151–159.
Classification
Onychomycosis is divided into several classes based on morphologic patterns and mode of invasion of the nail (Table 1).5 Classification provides a framework for diagnosis and expected response to treatment, and can help predict the prognosis. The classes include distal and lateral subungual onychomycosis (Figures 1 and 2), proximal subungual onychomycosis (Figure 3), superficial onychomycosis (Figure 4), and total dystrophic onychomycosis (Figure 5). A fifth class, endonyx subungual onychomycosis, is rare. Some nails have features from a combination of classes.
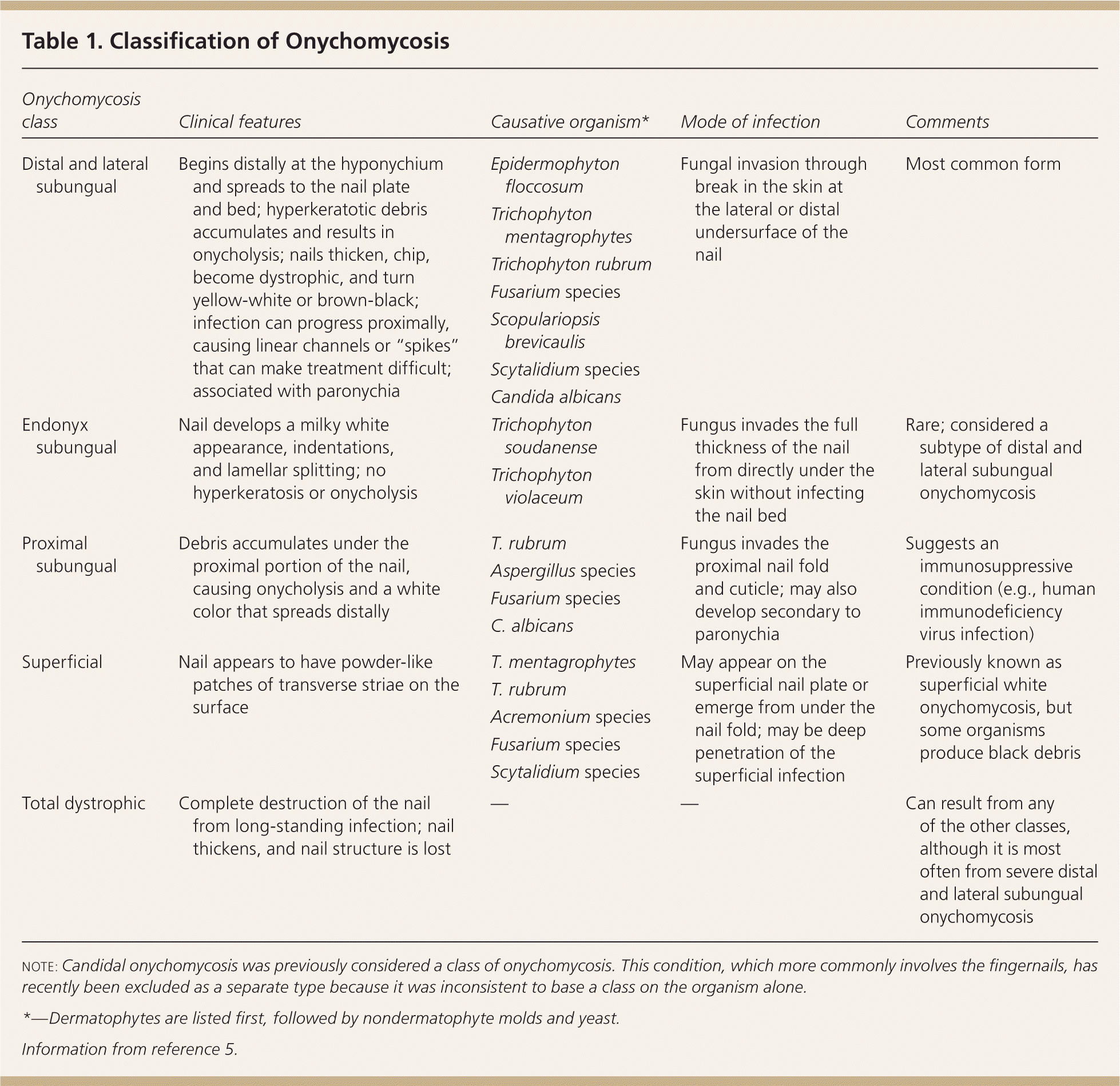
Table 1. Classification of Onychomycosis
| Onychomycosis class | Clinical features | Causative organism* | Mode of infection | Comments |
|---|---|---|---|---|
| Distal and lateral subungual | Begins distally at the hyponychium and spreads to the nail plate and bed; hyperkeratotic debris accumulates and results in onycholysis; nails thicken, chip, become dystrophic, and turn yellow-white or brown-black; infection can progress proximally, causing linear channels or “spikes” that can make treatment difficult; associated with paronychia | Epidermophyton floccosum | Fungal invasion through break in the skin at the lateral or distal undersurface of the nail | Most common form |
| Trichophyton mentagrophytes | ||||
| Trichophyton rubrum | ||||
| Fusarium species | ||||
| Scopulariopsis brevicaulis | ||||
| Scytalidium species | ||||
| Candida albicans | ||||
| Endonyx subungual | Nail develops a milky white appearance, indentations, and lamellar splitting; no hyperkeratosis or onycholysis | Trichophyton soudanense | Fungus invades the full thickness of the nail from directly under the skin without infecting the nail bed | Rare; considered a subtype of distal and lateral subungual onychomycosis |
| Trichophyton violaceum | ||||
| Proximal subungual | Debris accumulates under the proximal portion of the nail, causing onycholysis and a white color that spreads distally | T. rubrum | Fungus invades the proximal nail fold and cuticle; may also develop secondary to paronychia | Suggests an immunosuppressive condition (e.g., human immunodeficiency virus infection) |
| Aspergillus species | ||||
| Fusarium species | ||||
| C. albicans | ||||
| Superficial | Nail appears to have powder-like patches of transverse striae on the surface | T. mentagrophytes | May appear on the superficial nail plate or emerge from under the nail fold; may be deep penetration of the superficial infection | Previously known as superficial white onychomycosis, but some organisms produce black debris |
| T. rubrum | ||||
| Acremonium species | ||||
| Fusarium species | ||||
| Scytalidium species | ||||
| Total dystrophic | Complete destruction of the nail from long-standing infection; nail thickens, and nail structure is lost | — | — | Can result from any of the other classes, although it is most often from severe distal and lateral subungual onychomycosis |
NOTE: Candidal onychomycosis was previously considered a class of onychomycosis. This condition, which more commonly involves the fingernails, has recently been excluded as a separate type because it was inconsistent to base a class on the organism alone.
*—Dermatophytes are listed first, followed by nondermatophyte molds and yeast.
Information from reference 5.
Figure 1.
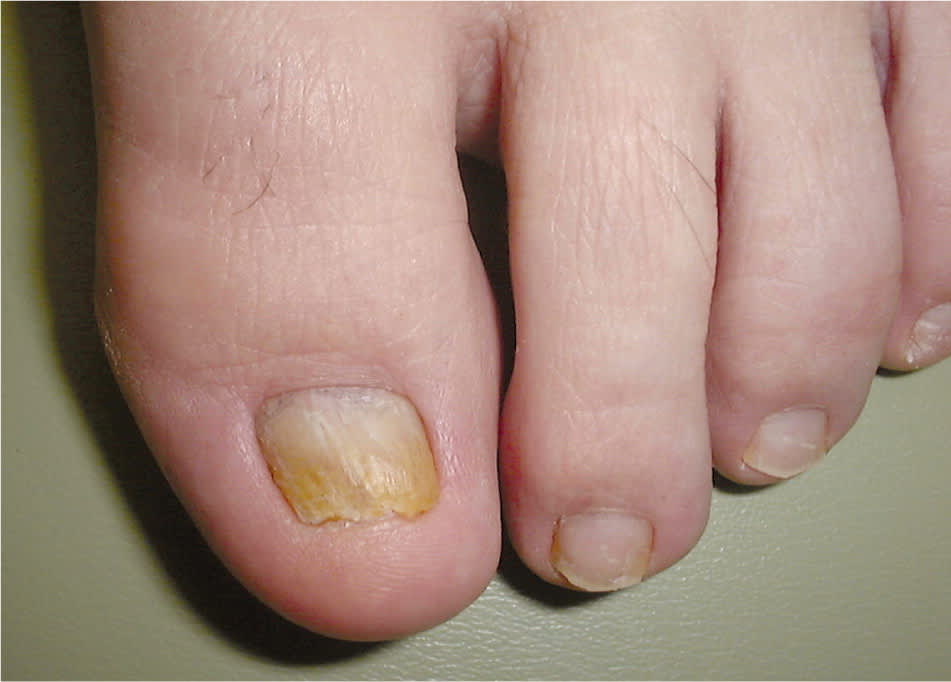
Distal and lateral subungual onychomycosis.
Figure 2.
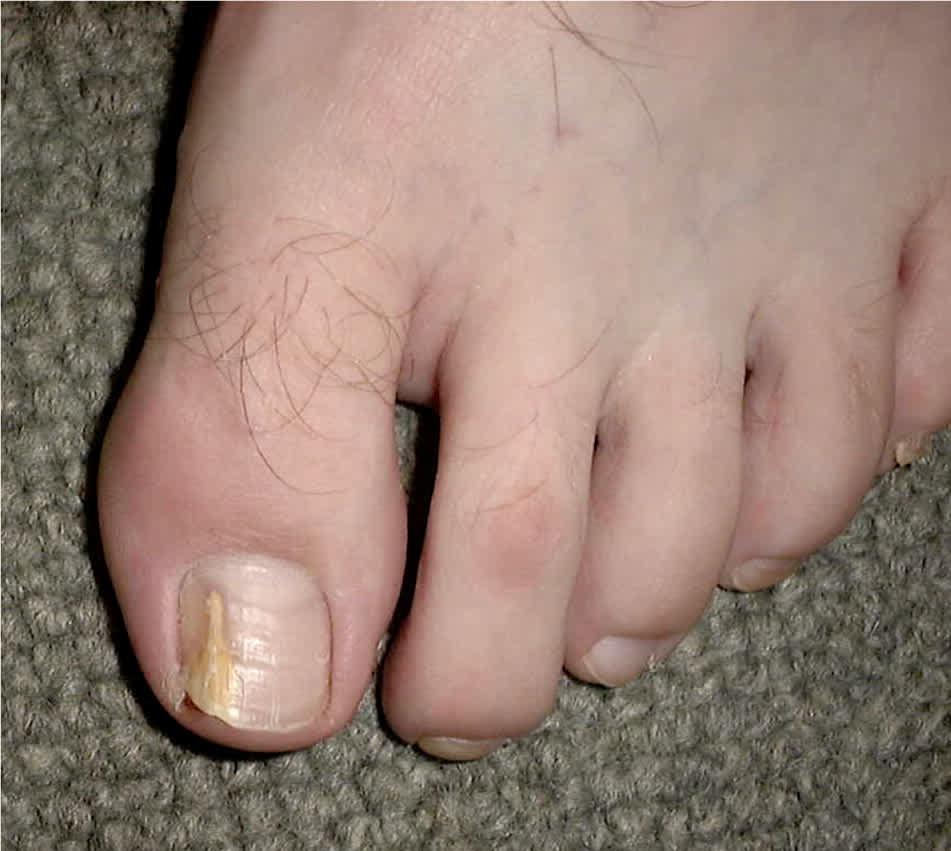
Distal and lateral subungual onychomycosis with spike deformity.
Figure 3.
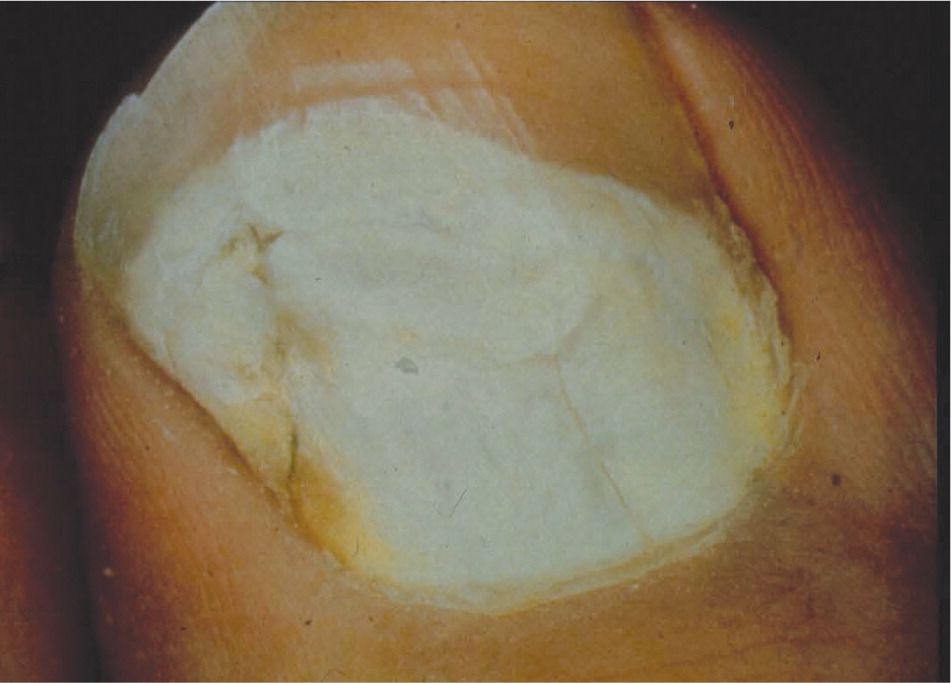
Proximal subungual onychomycosis.
Figure 4.
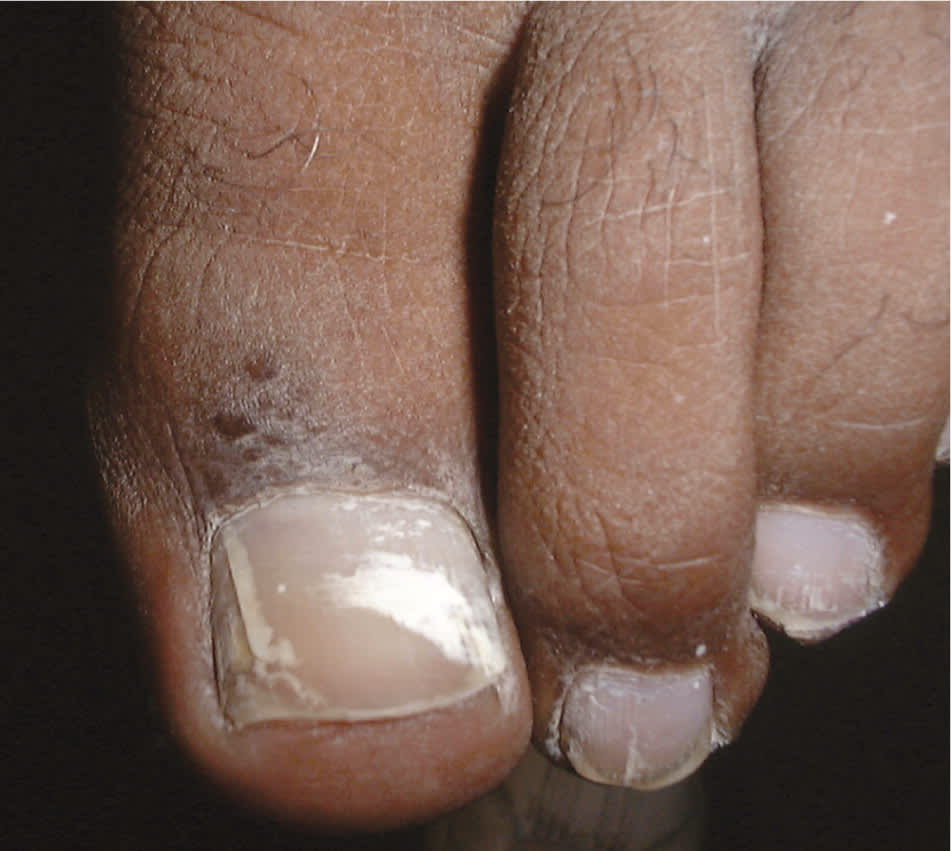
Superficial onychomycosis.
Figure 5.
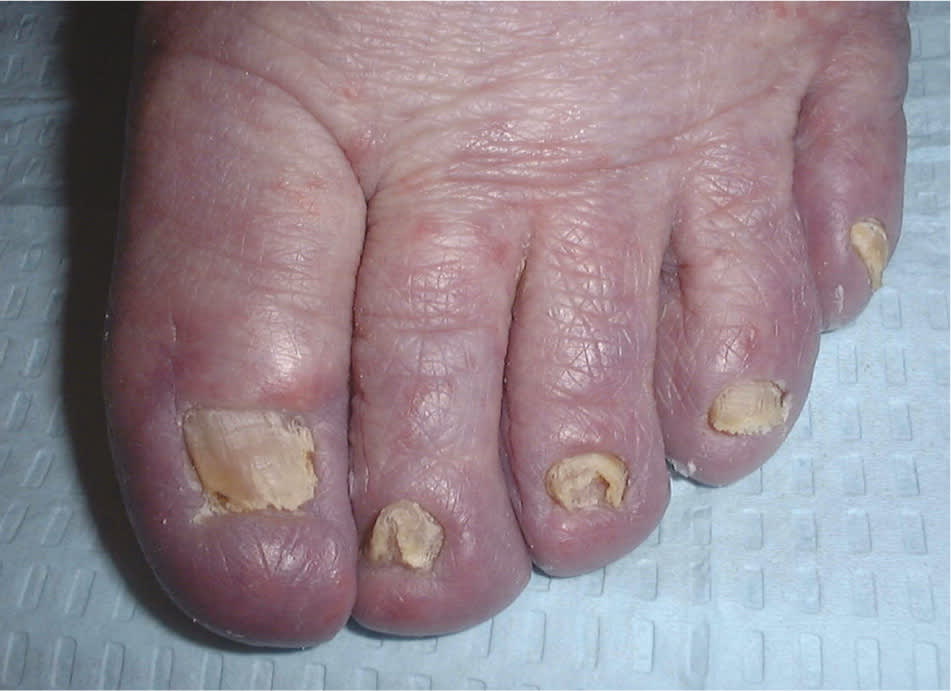
Total dystrophic onychomycosis.
Diagnosis
Accurate diagnosis is crucial for successful treatment and requires identification of physical changes and positive laboratory analysis. Only 50% of nail problems are caused by onychomycosis,6 and clinical diagnosis by physical examination alone can be inaccurate. Psoriasis, chronic nail trauma, and other causes must also be considered. The differential diagnosis of onychomycosis is presented in Table 2,7 and an algorithm outlining a suggested diagnostic approach is shown in Figure 6.
Table 2. Common Conditions That Can Mimic Onychomycosis

| Condition | Features |
|---|---|
| Infections | |
| Chronic paronychia | Chronic inflammation of the proximal paronychium; cross-striations of the nail; Streptococcus, Staphylococcus, or Candida found on smear and culture; common in children |
| Viral warts | Localized in nail folds and subungual tissue; longitudinal depressed grooves in the nail plate |
| Skin disorders | |
| Chronic dermatitis | Subungual dermatitis, hyperkeratosis, Beau lines, and pitting; thickened nail with corrugated surface |
| Lichen planus | Longitudinal grooves and fissures; usually affects fingernails |
| Psoriasis | Nail pitting, splinter hemorrhages, “oil staining,” yellow-gray or silvery white nails (eFigure B) |
| Twenty-nail dystrophy | Dystrophy of all 20 nails; usually resolves in childhood; associated with the lesions of lichen planus (eFigure C) |
| Trauma | |
| Footwear | Oncholysis, ingrown toenails, subungual keratosis, nail plate discoloration and irregularities; caused by friction against the shoe |
| Manipulation (e.g., manicures, pedicures, rubbing) | Horizontal parallel nail plate grooves, inflammation from Staphylococcus aureus or Pseudomonas infection (eFigure D) |
| Tumors | |
| Bowen disease | Squamous cell carcinoma; bleeding, pain, nail deformity, and nail discoloration |
| Fibroma | Oval or spherical, white or yellow nodule; causes tunnel-like melanonychia; fibrous dermatofibroma or periungual fibroma |
| Melanoma | Brown-yellow nail with dark pigment extending into the periungual skin folds; poor prognosis |
Information from reference 7.
eFigure B.
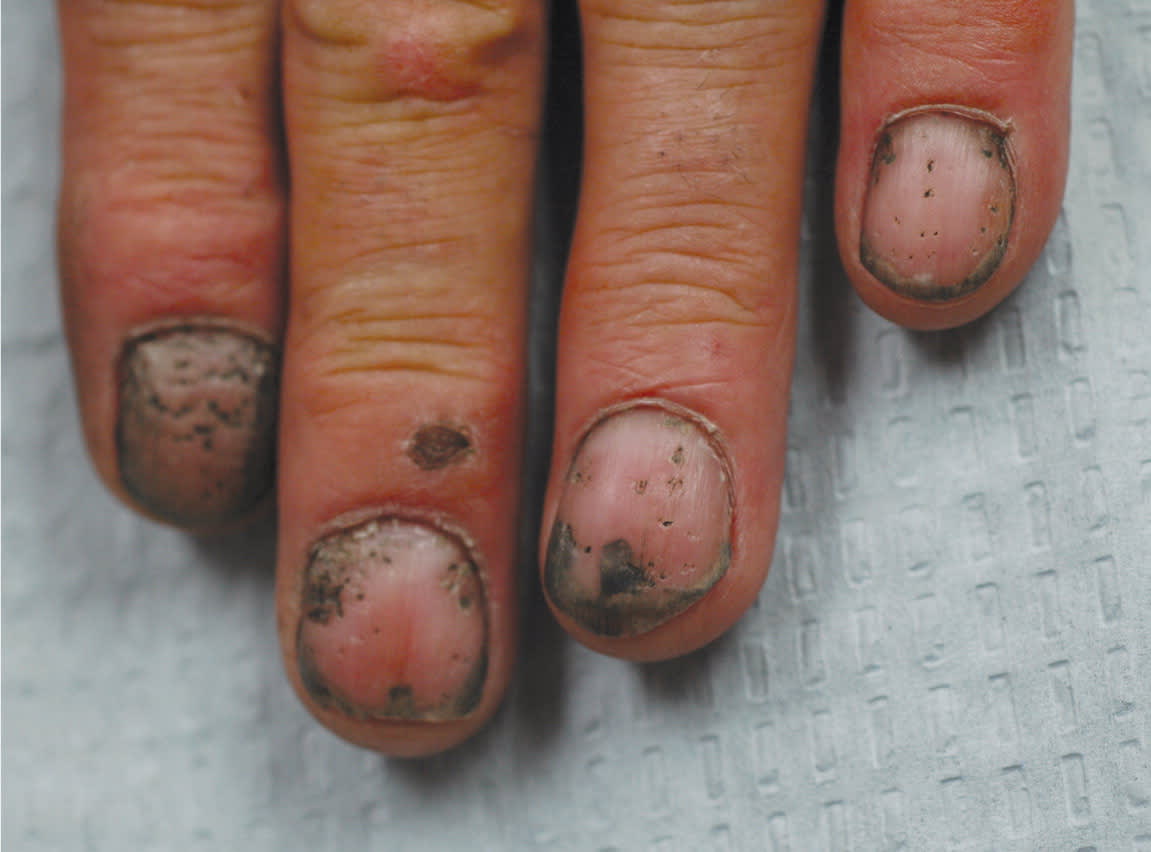
Nail pitting in a patient with psoriasis. The pits are enhanced by the presence of grease.
Photo provided by Robert T. Brodell, MD.
eFigure C.
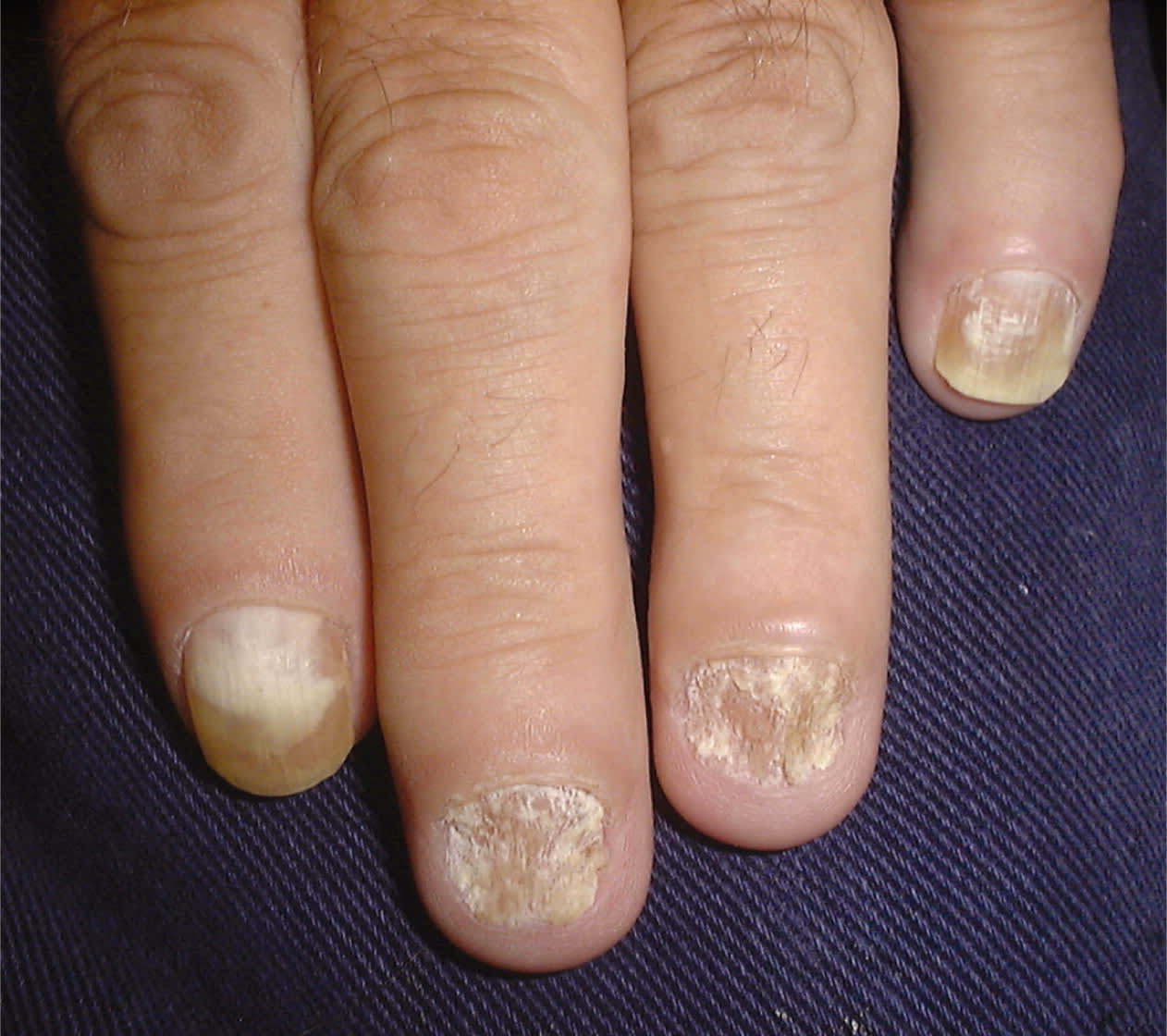
Twenty-nail dystrophy (also called sandpaper nails) is characterized by longitudinal ridges on all 20 nails. The nails may become discolored.
Photo provided by Robert T. Brodell, MD.
eFigure D.
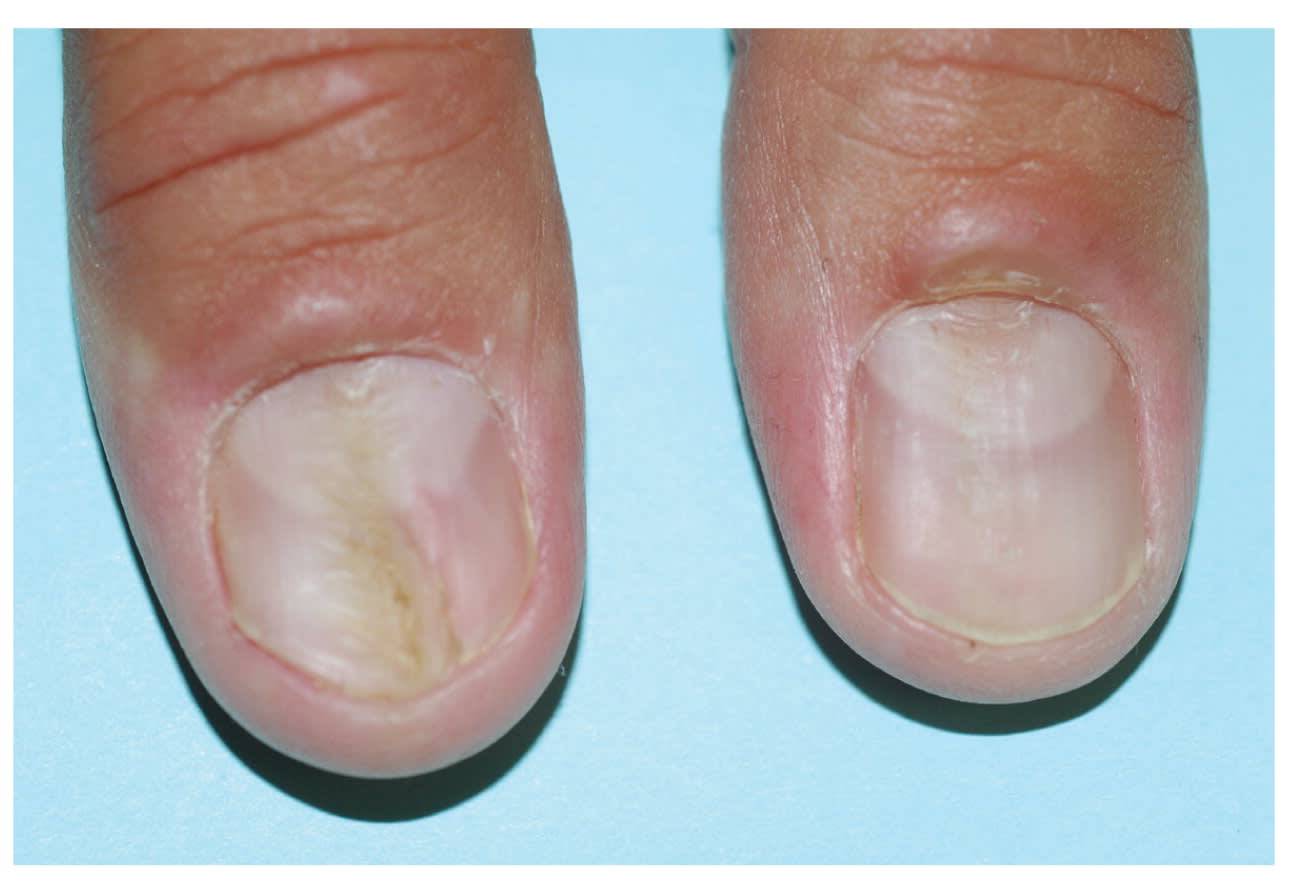
Median nail dystrophy caused by repetitive trauma to the nail from habitual rubbing.
Photo provided by Robert T. Brodell, MD.
Figure 6. Diagnosis of Onychomycosis
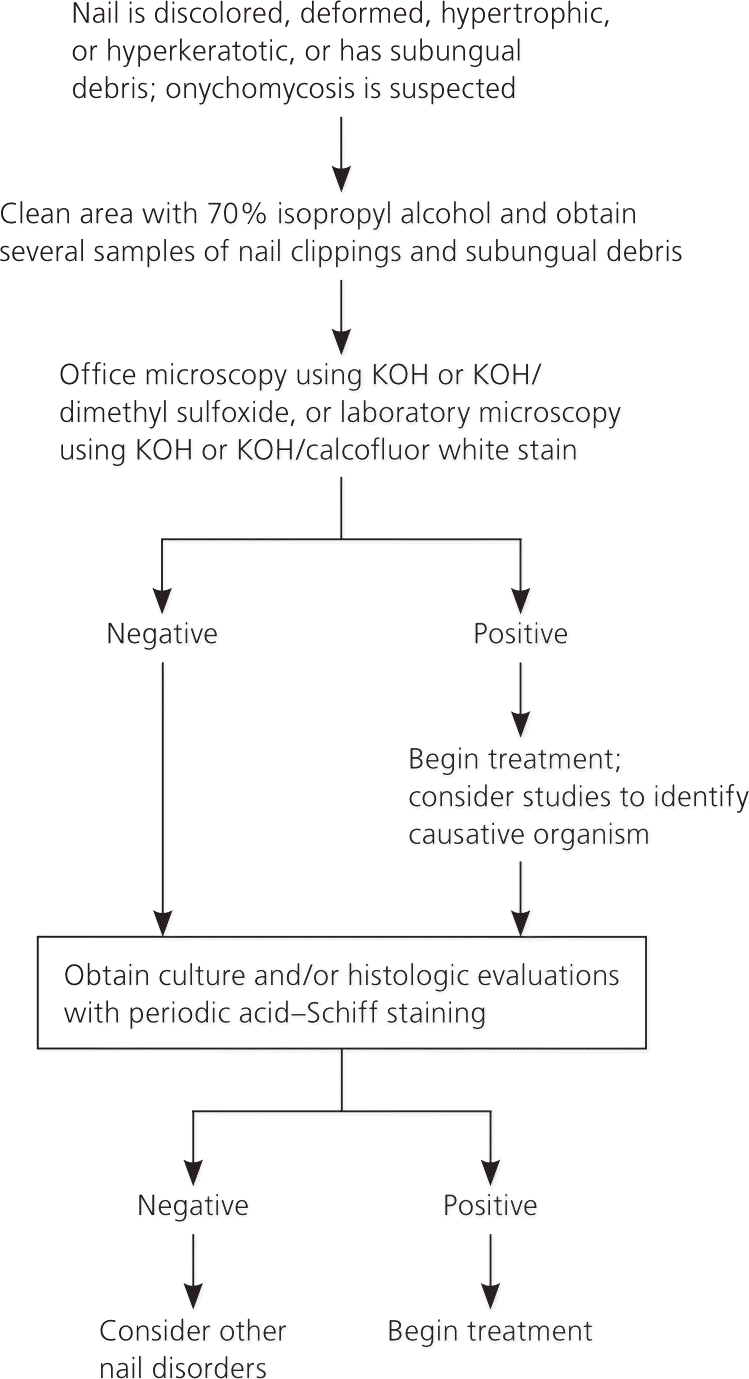
Algorithm for the diagnosis and treatment of onychomycosis. (KOH = potassium hydroxide.)
Laboratory analysis involves evaluation of nail clippings and subungual debris from the involved portion of the nail. Samples should be collected after cleansing the area with 70% isopropyl alcohol to prevent contamination. Clippings should be obtained with a sterile nail clipper or curette, and subungual debris using a No. 15 surgical blade or a 2-mm curette. To improve accuracy, eight to 10 nail shards should be collected.8 Diagnostic precision is enhanced if the sample is collected with a nail drill 9 and if it is taken from a more proximal location on the nail in patients with suspected distal and lateral onychomycosis.10 In those with suspected proximal subungual onychomycosis, the upper nail plate of the proximal nail is debrided, and underlying debris is collected. In those with suspected superficial onychomycosis, the superficial aspect of the nail is scraped.
Once the specimen has been obtained, office microscopy can be performed by preparing the samples with potassium hydroxide (KOH) 10% to 20% solution. The KOH will dissolve keratin, leaving the fungal cell intact. The specimen should be placed on a slide with a drop of KOH solution, then set aside at room temperature for five to 30 minutes; heating the slide or adding a dimethyl sulfide 40% solution will enhance keratin dissolution.11 Commercial laboratories may use KOH with calcofluor white stain, which binds to cellulose and enhances the fungal components in fluorescent microscopy.11
Identification of hyphae, pseudohyphae, or spores confirms infection but does not identify the organism. To identify the organism, culture can be performed in a laboratory.12 Samples should be sent in a sterile container, and results are usually available in four to six weeks. Histologic evaluation can also be helpful for identification of the organism, and it can provide results within 24 hours. Periodic acid–Schiff (PAS) staining and methenamine silver stains are used. PAS staining is less expensive,13 and in a study of 1,146 nail clippings comparing PAS histologic examination with KOH light microscopy and culture, PAS staining was the most sensitive test (82% sensitivity, compared with 53% for culture and 48% for KOH microscopy).14 Combining PAS staining with culture increased sensitivity to 96%. In a review of cases in which treatment was initiated before specimens were obtained, PAS staining had the highest sensitivity, and culture had the least.14
Polymerase chain reaction testing has been shown to be more accurate than culture, and results can be available in three days. However, it is not yet widely available.15,16
Treatment
Onychomycosis is widely believed to be only a cosmetic problem, but it can be uncomfortable and can lead to cellulitis in older adults17 and foot ulcers in patients with diabetes.18 Eradication of the infection is key to improving appearance and avoiding these complications, but it is not easily accomplished because nails are made of keratin, which is nonvascular and impermeable to many agents.19 Because of poor drug delivery to nails, results of treatment may not be apparent for a year.
Treatment varies depending on the severity of nail changes, the organism involved, and concerns about adverse effects and drug interactions. Treatments also have varying effectiveness, based on cure parameters that are defined differently among studies. Mycotic cure denotes that no organism is identified on microscopy and culture. Clinical cure refers to improvement in the appearance of the nail, often defined as a normal appearance in 80% to 100% of the nail. It is a subjective measure that is difficult to compare across studies.20 Complete cure indicates that mycotic and clinical cure have been achieved.
ORAL AZOLES AND ALLYLAMINES
Antifungals from the azole and allylamine classes are the most widely used oral medications for the treatment of onychomycosis. The azole class includes itraconazole (Sporanox), fluconazole (Diflucan), and ketoconazole; however, ketoconazole is rarely prescribed because of drug interactions and hepatotoxicity. The allylamine class is represented by terbinafine (Lamisil). These medications and their dosing regimens are shown in Table 3.21–27
Table 3. Commonly Prescribed Medications for Treatment of Onychomycosis in Adults
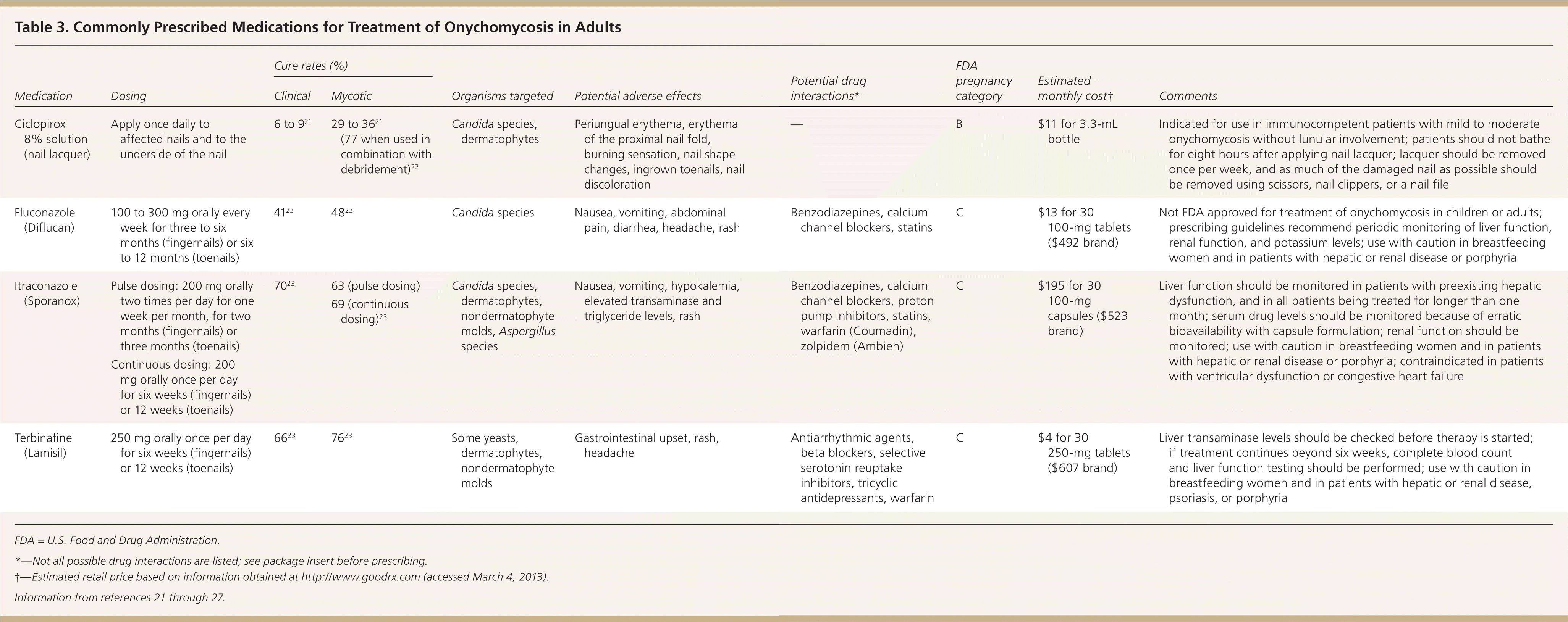
| Medication | Dosing | Cure rates (%) | Organisms targeted | Potential adverse effects | Potential drug interactions* | FDA pregnancy category | Estimated monthly cost† | Comments | |
|---|---|---|---|---|---|---|---|---|---|
| Clinical | Mycotic | ||||||||
| Ciclopirox 8% solution (nail lacquer) | Apply once daily to affected nails and to the underside of the nail | 6 to 921 | 29 to 3621 (77 when used in combination with debridement)22 | Candida species, dermatophytes | Periungual erythema, erythema of the proximal nail fold, burning sensation, nail shape changes, ingrown toenails, nail discoloration | — | B | $11 for 3.3-mL bottle | Indicated for use in immunocompetent patients with mild to moderate onychomycosis without lunular involvement; patients should not bathe for eight hours after applying nail lacquer; lacquer should be removed once per week, and as much of the damaged nail as possible should be removed using scissors, nail clippers, or a nail file |
| Fluconazole (Diflucan) | 100 to 300 mg orally every week for three to six months (fingernails) or six to 12 months (toenails) | 4123 | 4823 | Candida species | Nausea, vomiting, abdominal pain, diarrhea, headache, rash | Benzodiazepines, calcium channel blockers, statins | C | $13 for 30 100-mg tablets ($492 brand) | Not FDA approved for treatment of onychomycosis in children or adults; prescribing guidelines recommend periodic monitoring of liver function, renal function, and potassium levels; use with caution in breastfeeding women and in patients with hepatic or renal disease or porphyria |
| Itraconazole (Sporanox) | Pulse dosing: 200 mg orally two times per day for one week per month, for two months (fingernails) or three months (toenails) Continuous dosing: 200 mg orally once per day for six weeks (fingernails) or 12 weeks (toenails) | 7023 | 63 (pulse dosing) 69 (continu ous dosing)23 | Candida species, dermatophytes, nondermatophyte molds, Aspergillus species | Nausea, vomiting, hypokalemia, elevated transaminase and triglyceride levels, rash | Benzodiazepines, calcium channel blockers, proton pump inhibitors, statins, warfarin (Coumadin), zolpidem (Ambien) | C | $195 for 30 100-mg capsules ($523 brand) | Liver function should be monitored in patients with preexisting hepatic dysfunction, and in all patients being treated for longer than one month; serum drug levels should be monitored because of erratic bioavailability with capsule formulation; renal function should be monitored; use with caution in breastfeeding women and in patients with hepatic or renal disease or porphyria; contraindicated in patients with ventricular dysfunction or congestive heart failure |
| Terbinafine (Lamisil) | 250 mg orally once per day for six weeks (fingernails) or 12 weeks (toenails) | 6623 | 7623 | Some yeasts, dermatophytes, nondermatophyte molds | Gastrointestinal upset, rash, headache | Antiarrhythmic agents, beta blockers, selective serotonin reuptake inhibitors, tricyclic antidepressants, warfarin | C | $4 for 30 250-mg tablets ($607 brand) | Liver transaminase levels should be checked before therapy is started; if treatment continues beyond six weeks, complete blood count and liver function testing should be performed; use with caution in breastfeeding women and in patients with hepatic or renal disease, psoriasis, or porphyria |
FDA = U.S. Food and Drug Administration.
*—Not all possible drug interactions are listed; see package insert before prescribing.
†—Estimated retail price based on information obtained at http://www.goodrx.com (accessed March 4, 2013).
A meta-analysis of treatments for toenail onychomycosis determined that mycotic cure rates were 76% for terbinafine, 63% for itraconazole with pulse dosing, 59% for itraconazole with continuous dosing, and 48% for fluconazole.23 Clinical cure rates were 66% for terbinafine, 70% for itraconazole with pulse dosing, 70% for itraconazole with continuous dosing, and 41% for fluconazole. Common adverse effects included headache, gastrointestinal problems, and rash; these drugs also have been associated with Stevens-Johnson syndrome, prolonged QT interval, and ventricular dysfunction. The use of these agents is discouraged in patients with liver, renal, or heart disease, and in those receiving medications with which there may be significant drug-drug interactions.25 Liver function studies are recommended before beginning treatment and after one month of therapy.24 A meta-analysis concluded that the risk of asymptomatic elevation of transaminase levels in immunocompetent patients receiving oral antifungal agents was 2%, and that the risk of elevations requiring termination of therapy was 1%.28 Although these medications are not approved for use in children, they have been used in children with positive results.29
TOPICAL AGENTS
Several topical agents are used for the treatment of onychomycosis. These agents have few contraindications and no drug-drug interactions.
Ciclopirox 8% solution is the only topical prescription medication available in the United States for the treatment of onychomycosis. It is a synthetic hydroxypyridine antifungal formulated as a nail lacquer. Adverse effects include burning, itching, and stinging at the application site.30 It may be used in patients who cannot take oral antifungals and in those with less than 50% of the distal nail affected and no lunular involvement.21 It has been used in children, although it is not approved for use in patients younger than 12 years.29 When used alone, ciclopirox has a mycotic cure rate of 29% to 36%, and a clinical cure rate of 6% to 9%.21 A Cochrane review noted that the treatment failure rate was 61% to 64% after 48 weeks of use.31
Ciclopirox has also been used in combination with oral agents to improve effectiveness. In one comparative study, a combination of ciclopirox and oral terbinafine had a mycotic cure rate of 88% and a complete cure rate of 68%, whereas terbinafine alone had a mycotic cure rate of 65% and a complete cure rate of 50%.32
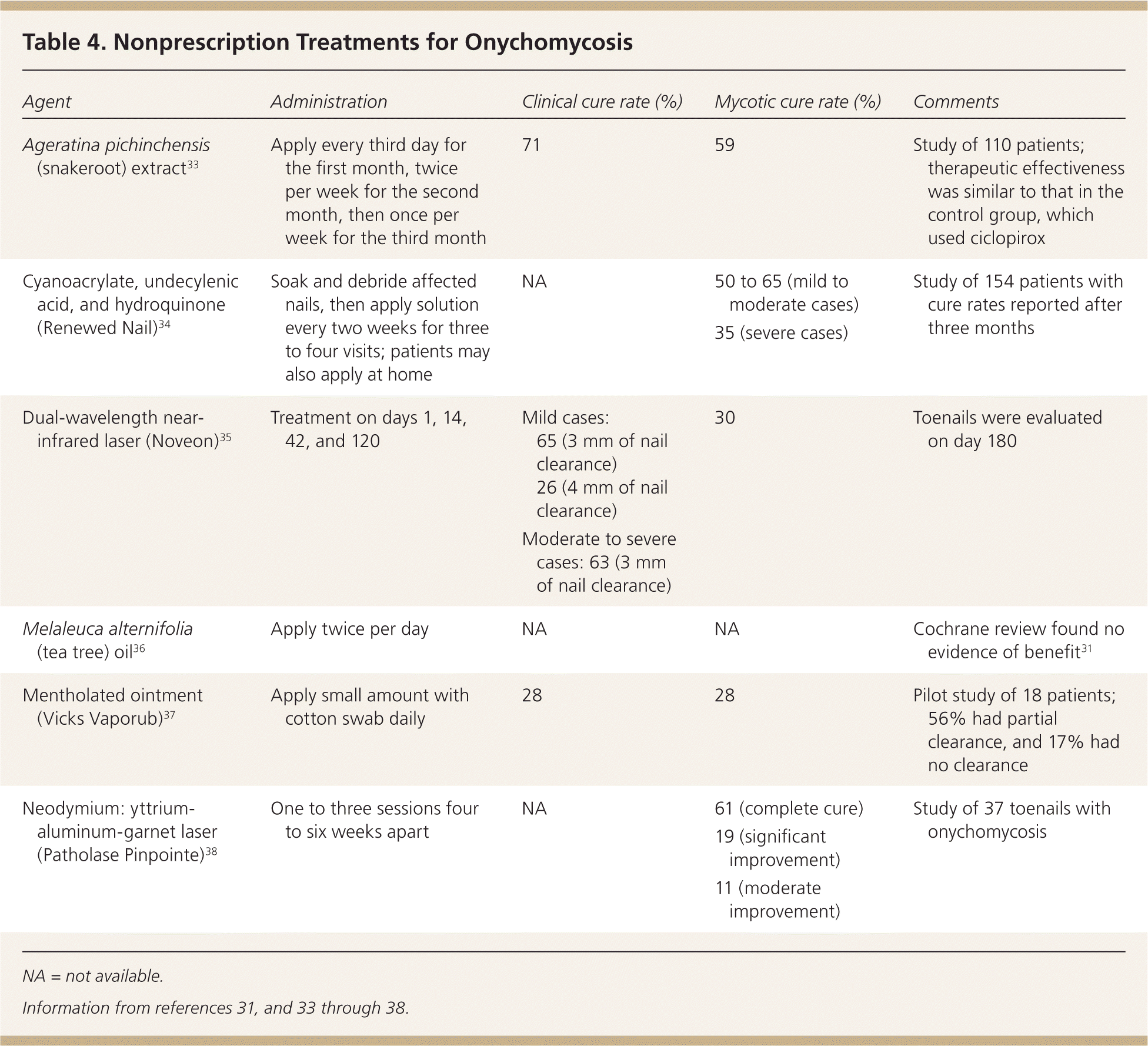
Nonprescription agents have also been used for treatment of onychomycosis (Table 4).31,33–38 These therapies have been evaluated in only a small number of studies involving few patients. Topical mentholated ointment (Vicks Vaporub) was used in a small study involving 18 patients.37 After 48 weeks, 28% had mycotic and clinical cure, 56% had partial clearance, and 17% had no improvement. Tea tree oil (Melaleuca alternifolia) has been evaluated in two studies. Although one trial was favorable, combined data from both studies did not demonstrate significant benefit.29,36 Snakeroot extract (Ageratina pichinchensis) is an antifungal derived from plants of the sunflower family. It was studied in a randomized trial involving 96 patients who applied the extract or ciclopirox for six months to nails with confirmed infections.33 Mycotic cure occurred in 59% of patients receiving the extract and in 64% of those receiving ciclopirox. Clinical cure occurred in 71% and 81% of patients, respectively. Differences between the two treatments were not statistically significant. A small study showed that a combination of cyanoacrylate, undecylenic acid, and hydroquinone (marketed as Renewed Nail) demonstrated mycotic cure in 78 of 154 participants (50%).34
Table 4. Nonprescription Treatments for Onychomycosis
| Agent | Administration | Clinical cure rate (%) | Mycotic cure rate (%) | Comments |
|---|---|---|---|---|
| Ageratina pichinchensis (snakeroot) extract33 | Apply every third day for the first month, twice per week for the second month, then once per week for the third month | 71 | 59 | Study of 110 patients; therapeutic effectiveness was similar to that in the control group, which used ciclopirox |
| Cyanoacrylate, undecylenic acid, and hydroquinone (Renewed Nail)34 | Soak and debride affected nails, then apply solution every two weeks for three to four visits; patients may also apply at home | NA | 50 to 65 (mild to moderate cases) | Study of 154 patients with cure rates reported after three months |
| 35 (severe cases) | ||||
| Dual-wavelength near-infrared laser (Noveon)35 | Treatment on days 1, 14, 42, and 120 | Mild cases: 65 (3 mm of nail clearance) 26 (4 mm of nail clearance) | 30 | Toenails were evaluated on day 180 |
| Moderate to severe cases: 63 (3 mm of nail clearance) | ||||
| Melaleuca alternifolia (tea tree) oil36 | Apply twice per day | NA | NA | Cochrane review found no evidence of benefit31 |
| Mentholated ointment (Vicks Vaporub)37 | Apply small amount with cotton swab daily | 28 | 28 | Pilot study of 18 patients; 56% had partial clearance, and 17% had no clearance |
| Neodymium: yttrium-aluminum-garnet laser (Patholase Pinpointe)38 | One to three sessions four to six weeks apart | NA | 61 (complete cure) | Study of 37 toenails with onychomycosis |
| 19 (significant improvement) | ||||
| 11 (moderate improvement) |
NA = not available.
PHYSICAL TREATMENTS
Nail trimming and debridement are often performed concomitantly with other treatments and appear to offer benefit. Study groups that received nail debridement with oral terbinafine had higher clinical cure rates than those who received oral terbinafine alone.39 When debridement was performed with concurrent administration of ciclopirox, the mycotic cure rate was 77%, higher than that for ciclopirox alone.22 Improvement in nail appearance was reported, but clinical cure rates were not.
Although they are expensive, laser and photodynamic therapies have become popular based on the success of in-vitro studies. Several neodymium:yttrium-aluminum-garnet (Nd:YAG) laser therapies have been approved by the U.S. Food and Drug Administration for treatment of onychomycosis.40 The Pinpointe Foot-laser, Cutera GenesisPlus laser, and Cooltouch Varia laser are short-pulse laser systems, whereas the Light Age Q-Clear laser is a Q-switched laser. However, there are only limited data about the use of these therapies in patients. In one study, Nd:YAG laser light was used to treat 37 nails, with one to three treatments given four to eight weeks apart. At 16 weeks, 61% were completely cured, 19% had significant improvement in the nail appearance, and 11% had moderate improvement in the nail appearance.38
Another laser treatment, the dual-wavelength near-infrared laser (Noveon), is approved for dermatologic use, but not specifically for treatment of onychomycosis.41 This treatment was used on 26 nails on days 1, 14, 42, and 120. After 180 days, 91% of nails with mild infection showed clinical improvement (3 to 4 mm of the nail free of clinical infection); however, only 30% had mycotic cure.42
Photodynamic therapy using photosensitizing drugs and light to destroy fungal cells has shown some success in the treatment of onychomycosis, but further evaluation is needed.43
Treatment Failure
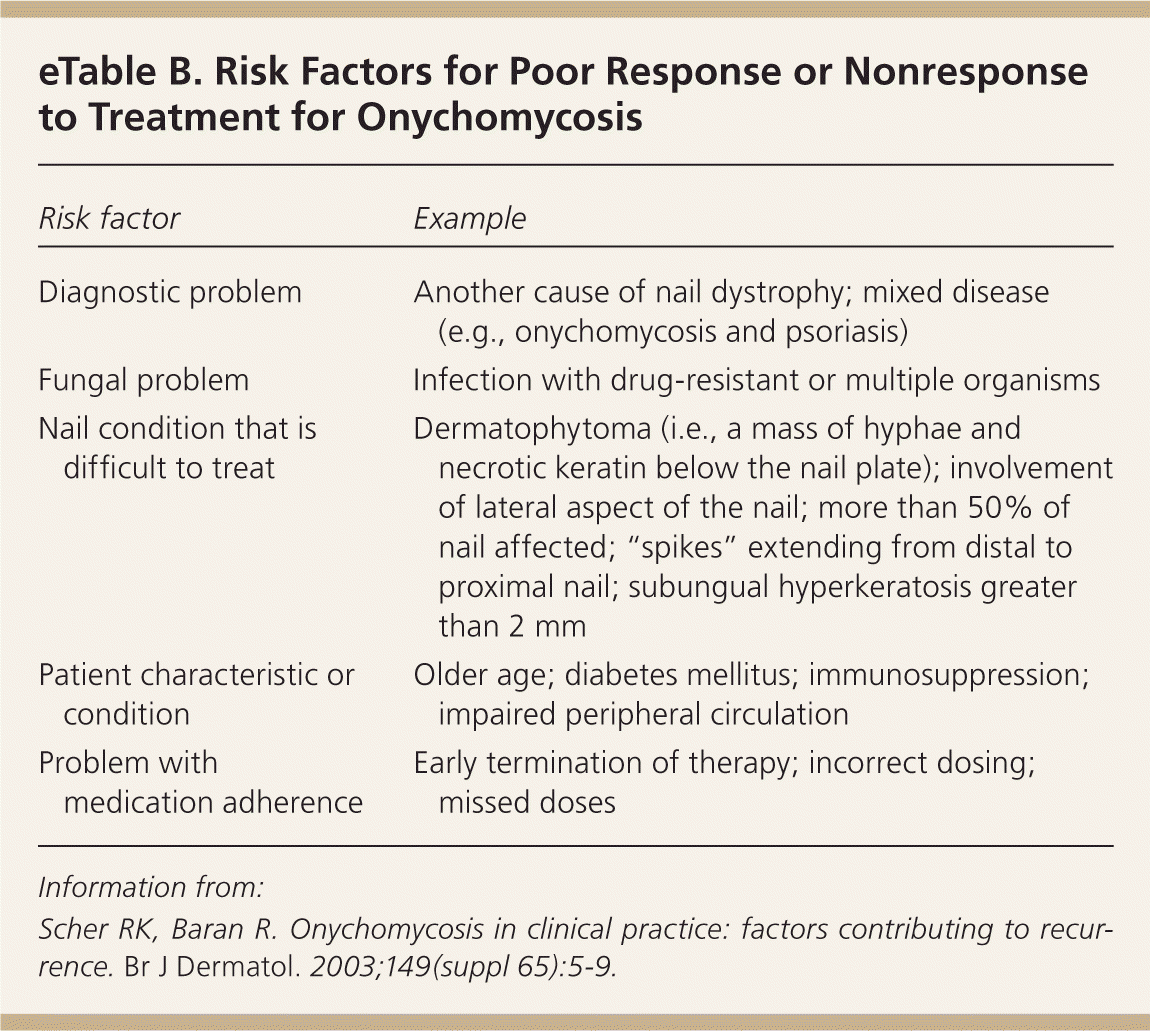
Despite the number of available treatments, not all patients with onychomycosis are cured. Numerous factors have been cited to explain the lack of response to therapy, such as nonadherence to treatment, incorrect diagnosis, or advanced disease. Factors contributing to poor response or nonresponse to treatment are listed in eTable B.
eTable B. Risk Factors for Poor Response or Nonresponse to Treatment for Onychomycosis
| Risk factor | Example |
|---|---|
| Diagnostic problem | Another cause of nail dystrophy; mixed disease (e.g., onychomycosis and psoriasis) |
| Fungal problem | Infection with drug-resistant or multiple organisms |
| Nail condition that is difficult to treat | Dermatophytoma (i.e., a mass of hyphae and necrotic keratin below the nail plate); involvement of lateral aspect of the nail; more than 50% of nail affected; “spikes” extending from distal to proximal nail; subungual hyperkeratosis greater than 2 mm |
| Patient characteristic or condition | Older age; diabetes mellitus; immunosuppression; impaired peripheral circulation |
| Problem with medication adherence | Early termination of therapy; incorrect dosing; missed doses |
Information from:
Scher RK, Baran R. Onychomycosis in clinical practice: factors contributing to recurrence. Br J Dermatol. 2003;149(suppl 65):5–9.
For those who appear to be cured, recurrent infection is a risk, with a number of factors increasing the chance of recurrence. Risk factors include concomitant disease, genetic factors, immunosuppression, incorrect dosing or duration of treatment, moisture, occlusive footwear, older age, poor hygiene, tinea pedis, and trauma.44 Recurrence can be caused by lack of mycotic cure or reinfection, and the reported rate of clinical recurrence of onychomycosis ranges from 10% to 53%, regardless of the treatment method used.45 Many patients tire of continued unsuccessful treatments or recurrences, and ultimately elect to undergo permanent nail removal.
Data Sources: A PubMed search was performed using the term onychomycosis combined with prevalence, classification, diagnosis, and treatment. The search included meta-analyses and systematic reviews, including those from the Cochrane database. The initial search strategy was supplemented by searches for randomized controlled trials of specific treatments identified during the review of meta-analyses and systematic reviews. Search date: March 2012.

