An 18-year-old athlete presented to the emergency department after he was hit in the face during football practice. He had pain over his nose, but no blurred vision or loss of consciousness. He had no relevant medical history.
Physical examination revealed bleeding from his nostrils and pain over the nasal bridge. His neurologic examination was unremarkable. Radiography and computed tomography of the facial bones revealed a nasal fracture and an intracranial abnormality. Magnetic resonance imaging (MRI) without contrast media was performed for better evaluation of this abnormality (Figures 1 and 2).
Figure 1.
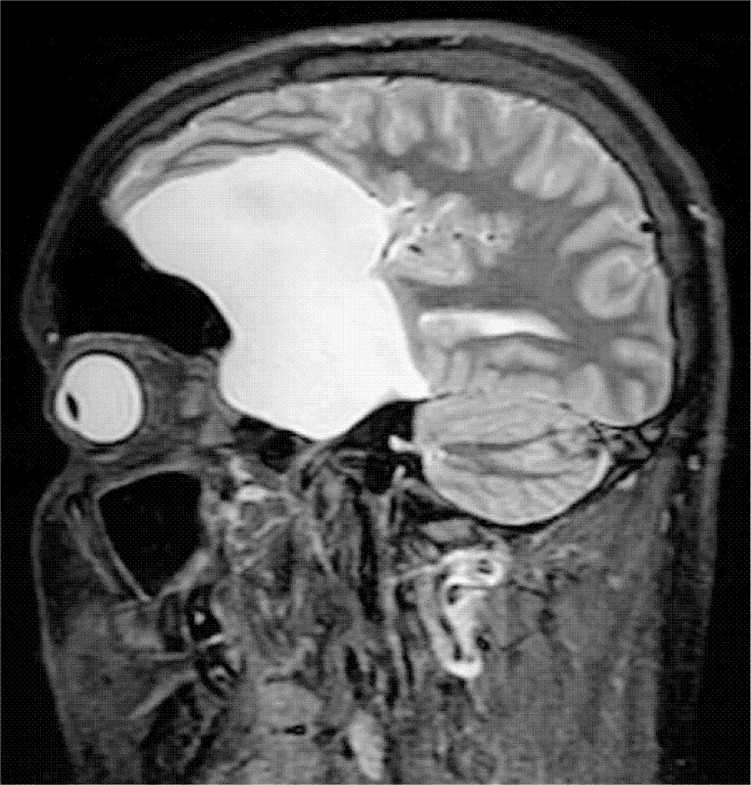
Figure 2.
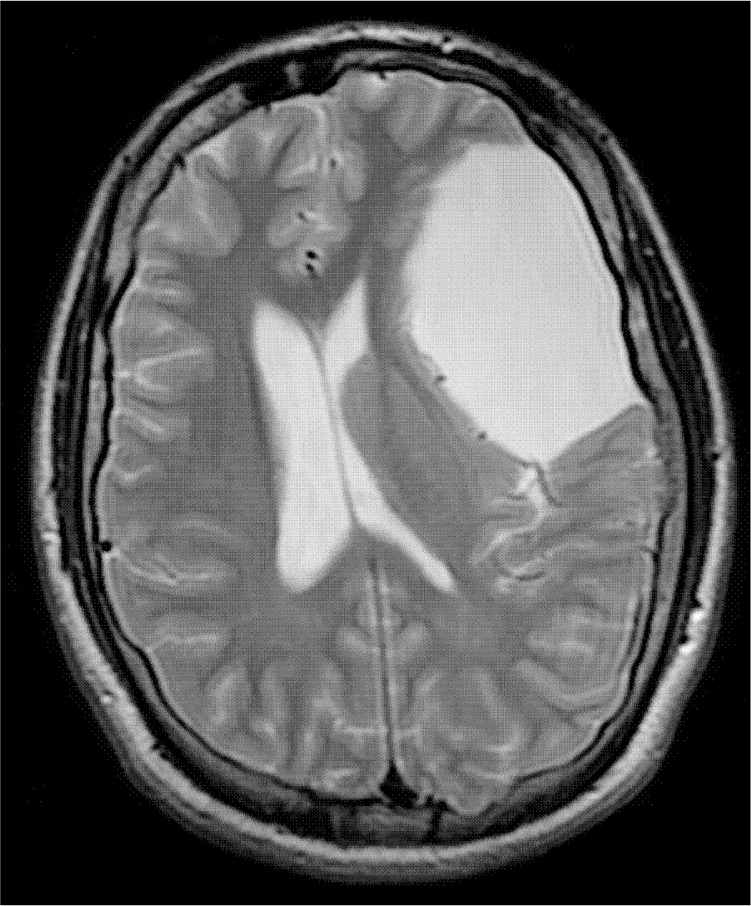
Question
Based on the patient's history, physical examination, and imaging findings, which one of the following is the most likely diagnosis?
A. Arachnoid cyst.
B. Choroid plexus cyst.
C. Epidural hematoma.
D. Meningioma.
Discussion
The answer is A: arachnoid cyst. Arachnoid cysts are congenital intracranial lesions that are thought to develop from splitting or duplication of the arachnoid membrane during development.1 They represent 1% to 2% of all intracranial lesions.2 Most arachnoid cysts are asymptomatic and are discovered incidentally during an unrelated evaluation. Symptomatic arachnoid cysts cause a mass effect on the brain, and headache is the most common symptom.3
Arachnoid cysts are filled with cerebrospinal fluid (CSF); therefore, the signal intensity on MRI is identical to that of CSF elsewhere in the brain. The cysts have homogeneous signal intensity, do not have internal architecture, and do not enhance with contrast media. They are sharply demarcated. Arachnoid cysts may increase the risk of intracranial bleeding while playing contact sports. Indications for surgery are symptoms from significant mass effect on the adjacent brain causing distorted gyral pattern or midline shift.4
Choroid plexus cysts are common intracranial cysts, usually on the choroid plexus of the lateral ventricles. The cysts are hyperintense compared with CSF on MRI, and they enhance with contrast media.
An epidural hematoma is a rapidly enlarging arterial bleed between the inner skull and the dura from trauma. It often causes rapid neurologic decline and has a biconvex shape, as opposed to the scalloped appearance of an arachnoid cyst.5 The blood of an epidural hematoma does not have the same signal intensity of CSF.
Meningiomas are benign tumors of the dura mater. MRI findings typically include a heterogeneous signal uptake because these tumors have a large amount of intersubstance matter. This matter may consist of calcifications, hemorrhage, cysts, or vascularity.
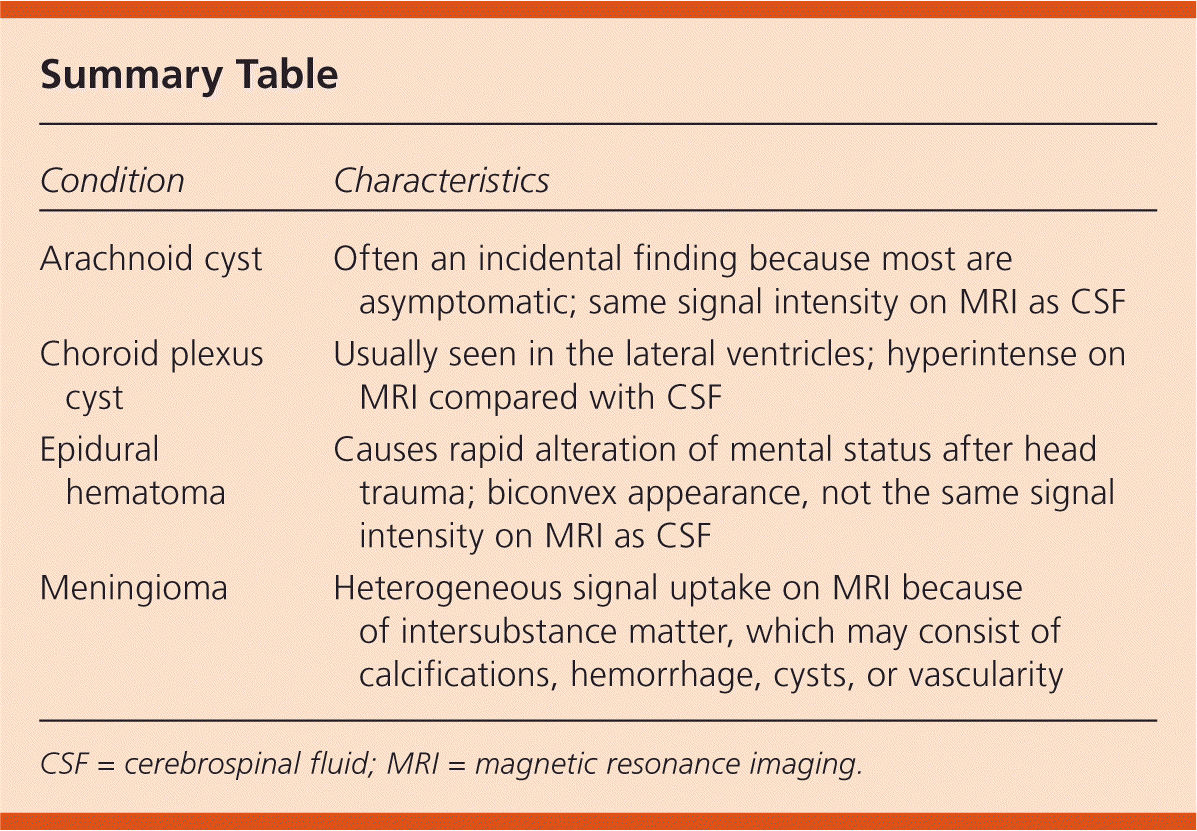
Summary Table
| Condition | Characteristics |
|---|---|
| Arachnoid cyst | Often an incidental finding because most are asymptomatic; same signal intensity on MRI as CSF |
| Choroid plexus cyst | Usually seen in the lateral ventricles; hyperintense on MRI compared with CSF |
| Epidural hematoma | Causes rapid alteration of mental status after head trauma; biconvex appearance, not the same signal intensity on MRI as CSF |
| Meningioma | Heterogeneous signal uptake on MRI because of intersubstance matter, which may consist of calcifications, hemorrhage, cysts, or vascularity |
CSF = cerebrospinal fluid; MRI = magnetic resonance imaging.

