Approximately 3 million work-related injuries were reported by private industries in 2011, and primary care physicians provided care for approximately one out of four injured workers. To appropriately individualize the treatment of an injured worker and expedite the return to work process, primary care physicians need to be familiar with the workers' compensation system and treatment guidelines. Caring for an injured worker begins with a medical history documenting preexisting medical conditions, use of potentially impairing medications and substances, baseline functional status, and psychosocial factors. An understanding of past and current work tasks is critical and can be obtained through patient-completed forms, job analyses, and the patient's employer. Return to work in some capacity is an important part of the recovery process. It should not be unnecessarily delayed and should be an expected outcome communicated to the patient during the initial visit. Certain medications, such as opioids, may delay the return to work process, and their use should be carefully considered. Accurate and legible documentation is critical and should always include the location, date, time, and mechanism of injury.
The evaluation and treatment of the injured worker has become a common challenge in the practice of medicine. In 2011, about 3 million workplace injuries were reported in private industries.1 More than one-half of these involved an injury severe enough that work restrictions, job transfer, or time off from work was required.1 The occupations with the most injuries requiring time off were laborers (construction trades), nursing aides/attendants, and janitors/cleaners.2 Persons 45 to 54 years of age had the highest incidence of injuries, with sprains, strains, and tears the most common diagnoses, accounting for 38% of all injuries requiring time off work.2 The back (36%), shoulder (12%), and knee (12%) were most often injured.2 In 2007, the costs for workers' compensation care in the United States was approximately $50 billion, about four times the cost of breast cancer treatment.3
Occupational medicine is one of the smallest medical specialties, producing about 130 board-eligible physicians annually.4 With the shortage of occupational medicine specialists, primary care physicians are often tasked with evaluating injured workers. Overall, 25% of patients with work-related conditions are cared for by primary care physicians, providing nearly three times as many visits for injured workers compared with occupational medicine specialists.5
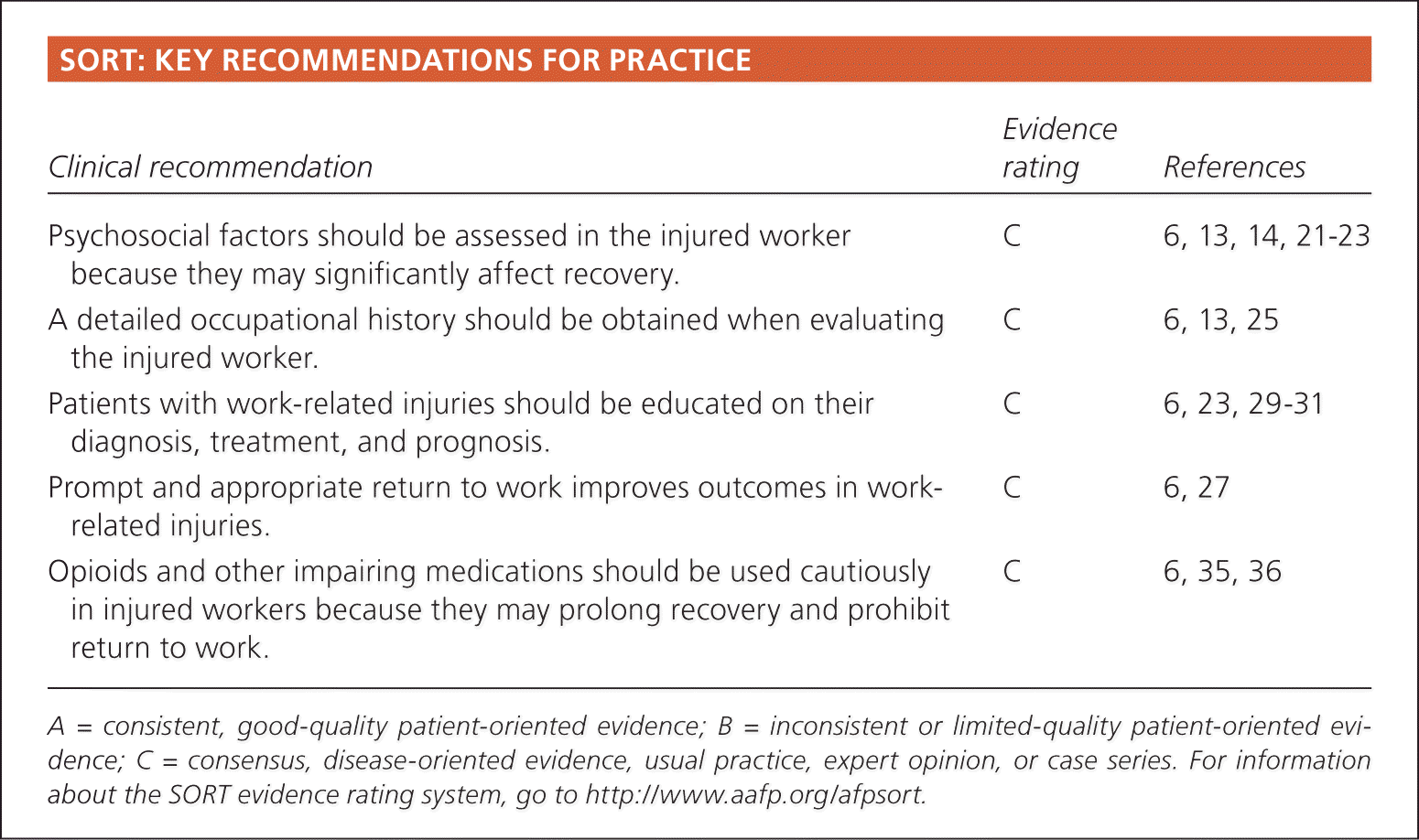
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Psychosocial factors should be assessed in the injured worker because they may significantly affect recovery. | C | 6, 13, 14, 21–23 |
| A detailed occupational history should be obtained when evaluating the injured worker. | C | 6, 13, 25 |
| Patients with work-related injuries should be educated on their diagnosis, treatment, and prognosis. | C | 6, 23, 29–31 |
| Prompt and appropriate return to work improves outcomes in work-related injuries. | C | 6, 27 |
| Opioids and other impairing medications should be used cautiously in injured workers because they may prolong recovery and prohibit return to work. | C | 6, 35, 36 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Evaluation
The evaluation of the injured worker extends beyond determining an appropriate diagnosis and treatment plan. The evaluation also assesses how related the condition is to work, the hazards within the work and nonwork environments, and the patient's functional abilities, pertinent psychosocial factors, and occupational history.
It is important to note that, in some circumstances, employers and workers' compensation insurance providers have arranged for injured employees to be evaluated by specific clinicians. The injured worker may not be aware of such an arrangement. Ideally, employers should be contacted before or at the time of worker presentation to ensure eligibility for care and to discuss the need for additional services, such as postaccident drug testing.
MEDICAL HISTORY
The assessment of an injured worker begins with a medical history.6 Workers can be exposed to many hazards, and a high suspicion for serious medical conditions is prudent, especially following acute injuries. Common sources of fatal injuries in the workplace from a 2012 census included motor vehicle crashes, falls and trips, strikes by equipment or objects, acts of violence, and exposure to harmful substances or environments.7
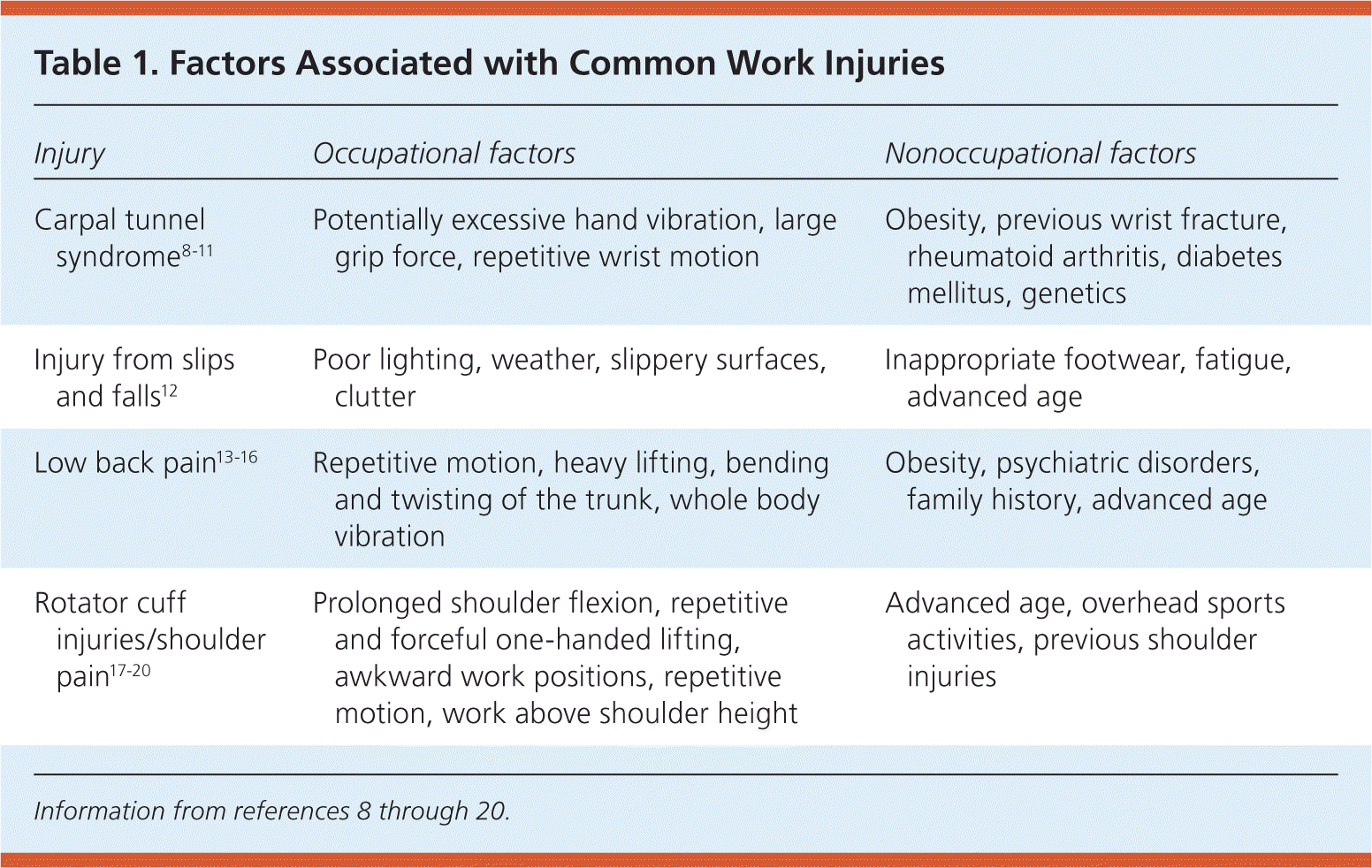
A detailed medical history is necessary for two reasons. First, preexisting medical conditions can make workers more prone to certain injuries and can impact recovery. Transparency of such a history is necessary for proper treatment (Table 1).8–20 Second, one of the primary goals of treating the injured worker is the return to preinjury medical status. A description of preexisting function, specifically in regards to activities of daily living, and comparison with functional deficits following an injury are useful in assessing recovery and setting feasible treatment goals.
Table 1. Factors Associated with Common Work Injuries
| Injury | Occupational factors | Nonoccupational factors |
|---|---|---|
| Carpal tunnel syndrome8–11 | Potentially excessive hand vibration, large grip force, repetitive wrist motion | Obesity, previous wrist fracture, rheumatoid arthritis, diabetes mellitus, genetics |
| Injury from slips and falls12 | Poor lighting, weather, slippery surfaces, clutter | Inappropriate footwear, fatigue, advanced age |
| Low back pain13–16 | Repetitive motion, heavy lifting, bending and twisting of the trunk, whole body vibration | Obesity, psychiatric disorders, family history, advanced age |
| Rotator cuff injuries/shoulder pain17–20 | Prolonged shoulder flexion, repetitive and forceful one-handed lifting, awkward work positions, repetitive motion, work above shoulder height | Advanced age, overhead sports activities, previous shoulder injuries |
Medications (prescription and over the counter), illicit substances (e.g., marijuana), and alcohol can contribute to work-related injuries or hazards and impair recovery. This is the impetus for the postaccident drug and alcohol testing required by many employers. When documenting the medication regimen, special attention should be made to dosing schedules. Medications used while away from work (e.g., at night only) do not necessarily affect work safety.
Psychosocial risk factors may be associated with work-related injuries and can affect recovery.6,13,14,21–23 Psychiatric comorbidities and maladaptive pain coping behaviors are associated with delayed recovery from low back pain.24 A stressful work environment has been associated with increased risks of shoulder injuries and pain.18 Guidelines from the American College of Occupational and Environmental Medicine describe psychosocial factors that should be assessed6 (Table 26,13,21,23,25 ). The presence of these factors warrants consideration of additional treatment options, such as fear avoidance behavior training, and a neuropsychological evaluation. It is important to note that psychosocial factors may operate consciously and subconsciously, and their presence does not equate to malingering in cases of delayed improvement.23
Table 2. Psychosocial Factors Affecting Recovery from Work-Related Injuries and Potential Treatments

| Psychosocial factors |
| Excessive stress |
| Family, friends, or peers receiving disability compensation |
| Fear avoidance behaviors (e.g., self-imposed limitation in spine range of motion) |
| Heavy labor position |
| Job dissatisfaction |
| Legal representation |
| Mental health conditions |
| Monotonous work |
| Poor relationship with supervisors and fellow employees |
| Potential treatments |
| Fear avoidance behavior training |
| Inpatient pain rehabilitation |
| Medical management of anxiety and depression |
| Neuropsychological assessment |
| Pain counseling |
| Physical activity |
OCCUPATIONAL HISTORY
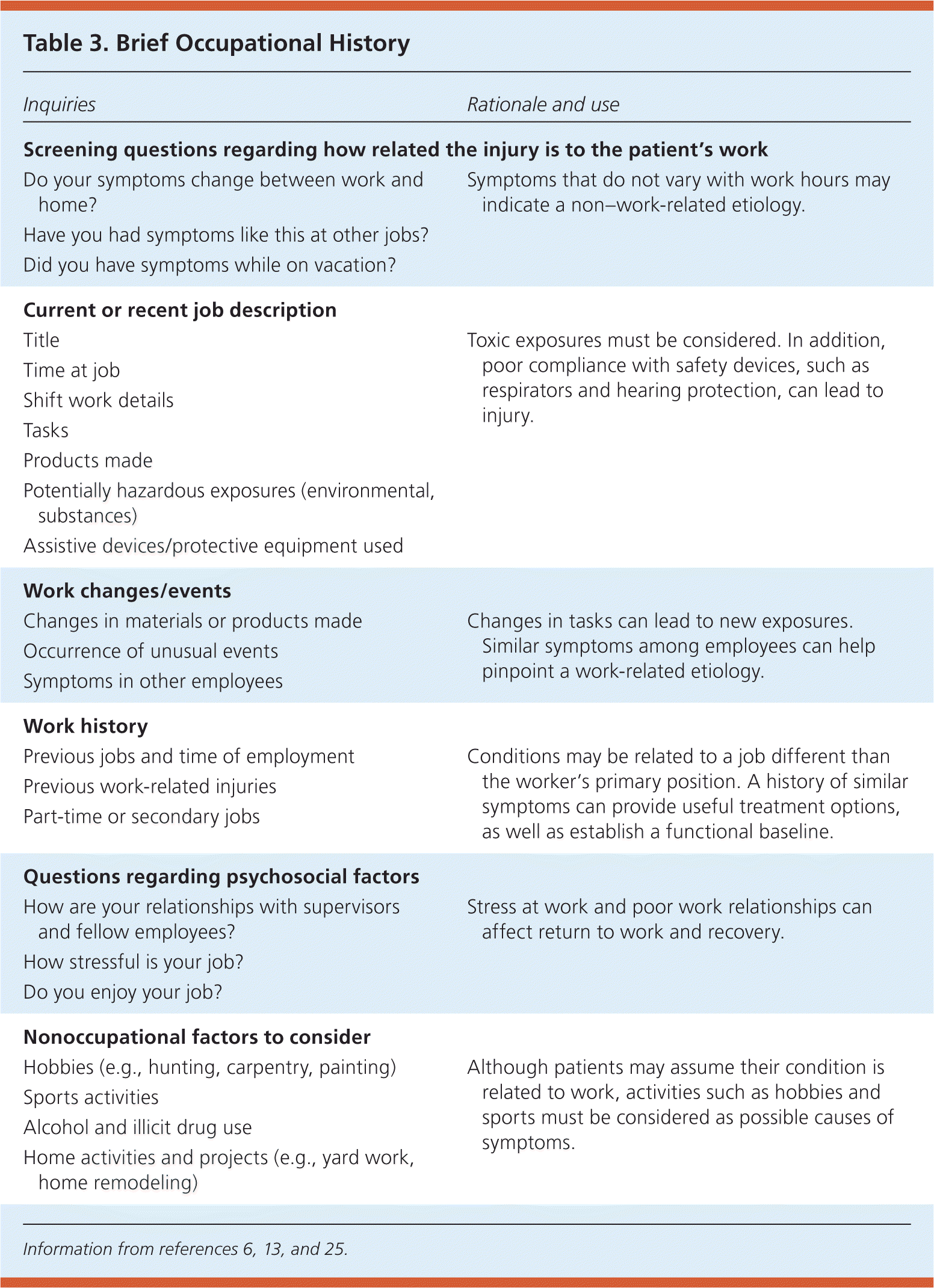
Occupational history is an often overlooked component of the medical history. Only 28% of patients have their work history recorded by physicians.26 An understanding of a patient's work and occupational history is critical for clarifying how related the injury is to work, preventing future injuries, and maximizing the return to work process.27 Typically, the most accessible source of occupational information is the patient. Although obtaining an occupational history can be time-consuming, this can be alleviated by the use of patient-completed forms administered before the evaluation13,28 (Table 36,13,25 ). Another important source of information is the job analysis. Job analyses provide details of work tasks, physical requirements, necessary skills, and potential exposures to hazardous materials or environments. The employer is also a valuable resource for work information, and consultation is recommended if permitted.27
Table 3. Brief Occupational History
| Inquiries | Rationale and use |
|---|---|
| Screening questions regarding how related the injury is to the patient's work | |
| Do your symptoms change between work and home? | Symptoms that do not vary with work hours may indicate a non–work-related etiology. |
| Have you had symptoms like this at other jobs? | |
| Did you have symptoms while on vacation? | |
| Current or recent job description | |
| Title | Toxic exposures must be considered. In addition, poor compliance with safety devices, such as respirators and hearing protection, can lead to injury. |
| Time at job | |
| Shift work details | |
| Tasks | |
| Products made | |
| Potentially hazardous exposures (environmental, substances) | |
| Assistive devices/protective equipment used | |
| Work changes/events | |
| Changes in materials or products made | Changes in tasks can lead to new exposures. Similar symptoms among employees can help pinpoint a work-related etiology. |
| Occurrence of unusual events | |
| Symptoms in other employees | |
| Work history | |
| Previous jobs and time of employment | Conditions may be related to a job different than the worker's primary position. A history of similar symptoms can provide useful treatment options, as well as establish a functional baseline. |
| Previous work-related injuries | |
| Part-time or secondary jobs | |
| Questions regarding psychosocial factors | |
| How are your relationships with supervisors and fellow employees? | Stress at work and poor work relationships can affect return to work and recovery. |
| How stressful is your job? | |
| Do you enjoy your job? | |
| Nonoccupational factors to consider | |
| Hobbies (e.g., hunting, carpentry, painting) | Although patients may assume their condition is related to work, activities such as hobbies and sports must be considered as possible causes of symptoms. |
| Sports activities | |
| Alcohol and illicit drug use | |
| Home activities and projects (e.g., yard work, home remodeling) | |
Treatment
There are a variety of common work-related injuries; a discussion of specific treatments is outside the scope of this article. Consensus guidelines, such as those published by the American College of Occupational and Environmental Medicine,6 can be consulted for treatment details. However, there are tenets of care that can be applied across a variety of injuries to maximize recovery.
PATIENT COMMUNICATION AND ENGAGEMENT
Uncertainty of the treatment course and prognosis can impair and prolong the recovery process. Efficient and succinct patient education on diagnosis, expected time to improvement, and long-term prognosis can improve outcomes.23,29,30 Setting a return to work date and informal education on how to prevent reinjury were both associated with early return to work.31 However, some written education materials such as “back books” have not been shown to produce consistent improvements.32 In the absence of serious pathology, the patient should be reassured of a likely favorable outcome.6,29 Treatment goals, including functional abilities, should be clearly stated. Frequent reassessments are recommended to facilitate monitoring of recovery and the effectiveness of treatment modalities.6,23
RETURN TO WORK
Work participation helps maintain physical conditioning, self-confidence, quality of life, and function.6,27,33 Absence from work is associated with poor outcomes, including increased morbidity, financial loss, and increased workers' compensation costs.6,27,33 To maximize outcomes and minimize prolonged disability, prompt and safe return to work, even if duties are modified, is critical. Of those patients who have remained off work for more than three months, only 50% return to employment.23
Motivated by their desire to support the patient, many physicians place unnecessary work restrictions on injured workers.34 Thus, successful return to work requires a paradigm shift. Effective return to work begins at the initial visit by stressing the importance of work in the treatment process.27 Physicians should also emphasize that pain is part of the healing process and that returning to work in some capacity, even at a reduced activity level, should not be delayed until pain has resolved.6,27 Thus, employers should be encouraged to provide temporary alternative or reduced duties and workplace accommodations to facilitate a prompt return to work when patients cannot perform their usual tasks.
Effective communication and collaboration between the physician and various stakeholders are of paramount importance.30 Stakeholders can include the employer, insurance representatives, and family members. Before communicating with an employer about a work-related injury, it is imperative that the physician understands what information may be transmitted to an employer. Typically, only information necessary to describe work restrictions and capabilities should be disclosed. Regulations regarding the sharing of work-related injury information vary between jurisdictions. Local policies should be clarified with the applicable workers' compensation insurance representatives or legal counsel before any information is disclosed.27
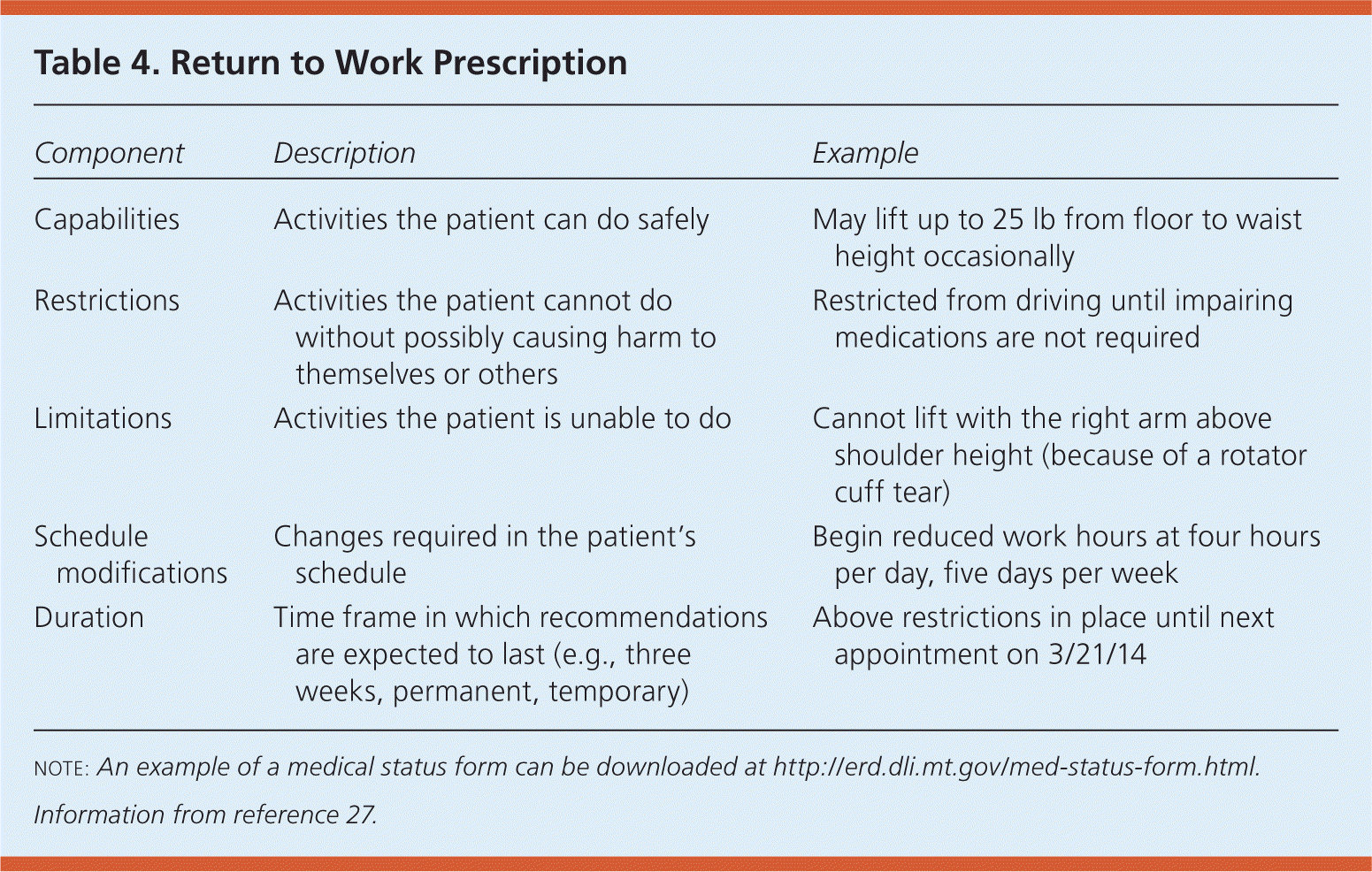
Activity recommendations for the return to work should include a detailed description of abilities, restrictions, limitations, safety concerns, schedule changes, necessary assistive devices, and duration of recommendations6 (Table 4).27 In addition, describing social and environmental limitations or restrictions may be necessary with some injuries. Such information may be communicated in a variety of ways, including through letters and standardized forms.
Table 4. Return to Work Prescription
| Component | Description | Example |
|---|---|---|
| Capabilities | Activities the patient can do safely | May lift up to 25 lb from floor to waist height occasionally |
| Restrictions | Activities the patient cannot do without possibly causing harm to themselves or others | Restricted from driving until impairing medications are not required |
| Limitations | Activities the patient is unable to do | Cannot lift with the right arm above shoulder height (because of a rotator cuff tear) |
| Schedule modifications | Changes required in the patient's schedule | Begin reduced work hours at four hours per day, five days per week |
| Duration | Time frame in which recommendations are expected to last (e.g., three weeks, permanent, temporary) | Above restrictions in place until next appointment on 3/21/14 |
NOTE: An example of a medical status form can be downloaded at http://erd.dli.mt.gov/med-status-form.html.
Information from reference 27.
MEDICATIONS
With the high prevalence of musculoskeletal conditions in patients with work-related injuries, the management of acute pain is a common occurrence. The purpose of pain management is not just to decrease pain, but also to improve physical and emotional functioning.35 In most patients, acute pain can be controlled adequately with the use of acetaminophen or ibuprofen.36
Occasionally, severe acute pain may require stronger medications such as opioids. The use of opioids for the treatment of non–cancer-related pain has increased significantly in recent years, and a similar trend has occurred in the treatment of injured workers. For example, between 1999 and 2007, opioid use increased by 50% in Washington's workers' compensation cases.37 Early opioid use in the treatment of work-related back injuries has been associated with prolonged disability, higher medical costs, increased risk of surgery, and long-term opioid use.36
Opioids may also limit an injured worker's ability to return to work. Opioids, as well as benzodiazepines and muscle relaxants, are associated with reduced alertness, sedation, and cognitive limitations. Although current research is inconclusive regarding the potential impairments on function associated with opioids, numerous employers have adopted policies that prevent employees from working while using impairing medications.35 Job tasks should be considered when prescribing medications. Any potential work safety concerns secondary to the use of impairing medications should be discussed with the patient and, with adequate permission, the patient's employer.
Specialized Examinations
The management of work-related injuries, especially in the setting of workers' compensation, can often require the input of additional clinicians. Such input can consist of unique examinations and reports, many of which are unfamiliar to primary care physicians. One common evaluation is the independent medical examination. It is an extensive one-time evaluation performed by a clinician or a panel of clinicians not involved in the care of the patient. Independent medical examinations serve several purposes, such as to review treatment and assess how related the injuries are to work.
Another type of examination that may be needed is the functional capacity evaluation, which assesses functional ability using one of several validated instruments.38 Functional capacity evaluations are usually performed by a physical or occupational therapist and can provide useful information about the ability of the patient to undertake essential job-related physical demands.
An impairment rating is also commonly performed for work injuries. It is a consensus-based estimation (represented as a percentage) of anatomic, physiologic, and psychological changes in function.38 Also accounted for is the effect of these changes on activities of daily living.39 Impairment rating assessments are typically performed by physicians and utilize the American Medical Association's Guides to the Evaluation of Permanent Impairment. There are six editions of the guides, and different jurisdictions use different editions.39 Impairment ratings can provide useful information about functional abilities and medical history, but it should be noted that impairment does not necessarily correlate with disability.39
A neuropsychological examination can provide information on psychiatric disorders, personality traits, and psychosocial factors that may affect treatment and recovery. This examination includes an array of tests to help develop a detailed psychological profile of a patient. It is usually performed by a clinical psychologist or psychiatrist over several hours.6,39
Documentation
Significant legal and financial ramifications can be associated with a work-related injury, and it should be expected that documentation pertaining to the injury will be scrutinized by multiple stakeholders including nurse case managers, claims adjusters, medical peer reviewers, and attorneys. Clinical documentation is used by claims adjusters and insurance providers to determine the extent of medical coverage. Failure to adequately document an injury can severely limit a worker's legitimate access to care. In addition, accurate documentation can help control rising workers' compensation costs by better conveying how related an injury is to work.34
Documentation must include a list of potential injuries and sources of pain, and detailed physical examination findings. For acute injuries, the location, date, time, and mechanism of injury should be recorded clearly. The necessary history elements in an acute work-related injury can be recalled by using the American College of Occupational and Environmental Medicine's four W's (where [location of event], when [time and date], who [witness and other persons involved], and what [mechanism of injury and circumstances]).6
Data Sources: A search in PubMed was conducted using terms such as evaluation of work injuries, work injuries, opioids and workers compensation, return to work, and occupational evaluation. Clinical Queries and MESH were used. In addition, searches of the Agency for Healthcare Research and Quality evidence reports, Bandolier, Clinical Evidence, the Cochrane database, Database of Abstracts of Reviews of Effects, the Institute for Clinical Systems Improvement, the National Guideline Clearinghouse database, and UpToDate were performed. Search date: October 1, 2012; reviewed on September 15, 2013.

