Case Scenario
A 54-year-old man presents for his routine follow-up appointment at the office where I recently started working. I inherited him as part of a panel of patients who had belonged to one of the founding physicians, who recently retired after 38 years in practice. At the visit, the patient states that he is experiencing low energy and poor sleep, both of which have been ongoing for more than a year. The patient's medical history includes hypertension, hyperlipidemia, insomnia, anxiety, chronic low back pain, and gastroesophageal reflux disease. His medication list includes once-daily dosages of furosemide (Lasix), 20 mg; omeprazole (Prilosec), 20 mg; fluoxetine (Prozac), 20 mg; lisinopril (Zestril), 40 mg; and pravastatin (Pravachol), 40 mg. He also takes oxycodone (Roxicodone), 5 mg three times daily as needed, and alprazolam (Xanax), 0.5 mg three times daily as needed.
He has no known drug allergies. He has been receiving monthly prescriptions for oxycodone and alprazolam for the past five years. Periodic urine toxicology screening has been repeatedly negative for illicit substances, but consistently demonstrates benzodiazepines and oxycodone, as expected. What is the best management approach when inheriting a patient with a challenging medication regimen?
Commentary
Inheriting a patient on an inappropriate or questionable medical regimen is a scenario that every physician confronts when practicing continuity care. It can present frustrating challenges, especially for resident physicians, who, because of the nature of training programs, care for patient panels with high turnover rates. Regardless of the practice setting, several issues pertaining to certain medication categories should be considered.
In this example, the physician could question (1) the use of a loop diuretic, apparently prescribed to treat hypertension, without a clear, evidence-based indication such as congestive heart failure; (2) long-term use of a proton pump inhibitor (PPI) for reflux maintenance management; and (3) chronic use of a benzodiazepine and an opioid. Addiction issues, whether physical, psychological, or both, can present further challenges in weaning. Table 1 describes clinical considerations and suggested approaches for the four medication classes noted in the case scenario.1–11
Table 1. Selected Medication Classes to Review with Inherited Patients
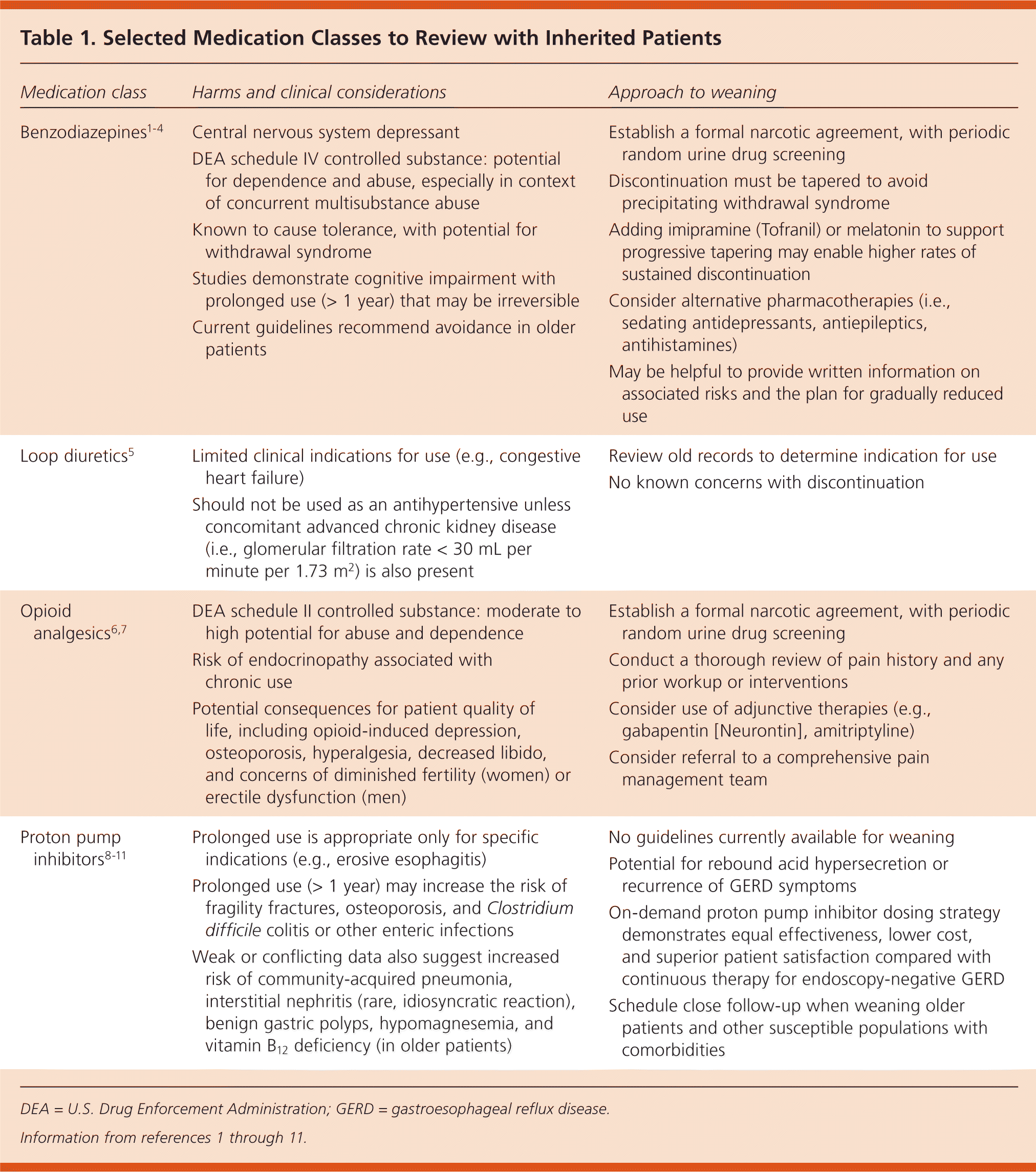
| Medication class | Harms and clinical considerations | Approach to weaning |
|---|---|---|
| Benzodiazepines1–4 |
|
|
| Loop diuretics5 |
|
|
| Opioid analgesics6,7 |
|
|
| Proton pump inhibitors8–11 |
|
|
DEA = U.S. Drug Enforcement Administration; GERD = gastroesophageal reflux disease.
Successfully navigating these concerns requires establishing a strong and trusting relationship with the patient, exploring alternative treatment modalities, and communicating clearly with the patient about risks associated with continuing these medications. Often a de novo medication assessment that employs a model of shared decision making can effectively facilitate this partnership. The physician should attempt to obtain and review old records to identify the original rationale for instituting the medications, and to clarify any previous dosage changes or escalations. The patient must be actively engaged in the weaning process. If weaning is too challenging at present, the physician should revisit the concerns regularly over time, attempting to make the regimen as appropriate as possible.
The physician should also weigh various mitigating factors that may influence the approach, such as the patient's age, anticipated life expectancy, and level of resiliency. For example, an older patient with a longstanding commitment to PPI therapy for reflux symptoms may find discontinuation too onerous. It may be more prudent to focus on eliminating other higher-risk medications, such as benzodiazepines, and to defer conversation about the PPI. As is often the case, it is important to “pick your battles” to develop the best possible therapeutic relationship.

