Key Clinical Issue
What are the potential benefits and adverse effects associated with dietary and pharmacologic interventions to prevent recurrence of kidney stones in adults 18 years and older?
Evidence-Based Answer
There is limited evidence that fluid intake to maintain urine output greater than 2 L per day; eliminating soft drinks containing only phosphoric acid (i.e., no citric acid); or consuming a normal-calcium (1,200 mg per day), low-sodium, low–animal protein, decreased-oxalate, and increased-water diet may each reduce the risk of calcium stone recurrence. (Strength of Recommendation [SOR]: C, based on disease-oriented evidence.) Diets with high fiber or reduced animal protein as solitary interventions may not help prevent stone recurrence. The effectiveness of other dietary interventions is not clear. When added to increased fluid intake, thiazide diuretics, citrate, and allopurinol (in patients with elevated blood or urine uric acid levels) each reduce the risk of recurrent calcium stones more than increased fluid intake alone. (SOR: C, based on disease-oriented evidence.) Patients receiving pharmacologic interventions (particularly thiazide diuretics and citrate) may experience adverse effects, such as gastrointestinal problems, that lead to stopping treatment. The evidence is too limited to determine the role of baseline or follow-up laboratory testing in predicting stone recurrence.
Clinical Bottom Line: Preventing Recurrent Nephrolithiasis in Adults
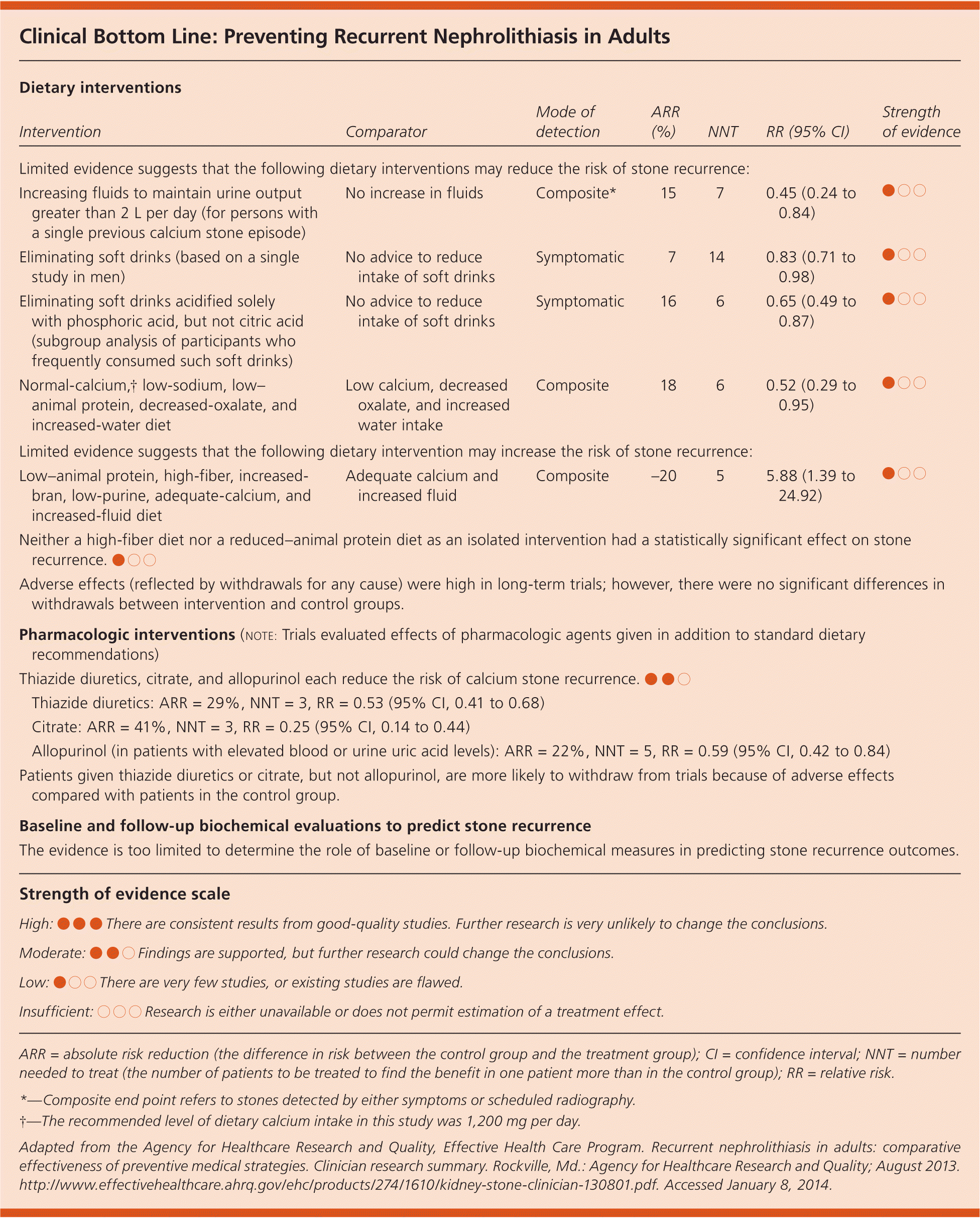
| Dietary interventions | |||||||
|---|---|---|---|---|---|---|---|
| Intervention | Comparator | Mode of detection | ARR (%) | NNT | RR (95% CI) | Strength of evidence | |
| Limited evidence suggests that the following dietary interventions may reduce the risk of stone recurrence: | |||||||
| Increasing fluids to maintain urine output greater than 2 L per day (for persons with a single previous calcium stone episode) | No increase in fluids | Composite* | 15 | 7 | 0.45 (0.24 to 0.84) | ●○○ | |
| Eliminating soft drinks (based on a single study in men) | No advice to reduce intake of soft drinks | Symptomatic | 7 | 14 | 0.83 (0.71 to 0.98) | ●○○ | |
| Eliminating soft drinks acidified solely with phosphoric acid, but not citric acid (subgroup analysis of participants who frequently consumed such soft drinks) | No advice to reduce intake of soft drinks | Symptomatic | 16 | 6 | 0.65 (0.49 to 0.87) | ●○○ | |
| Normal-calcium,† low-sodium, low–animal protein, decreased-oxalate, and increased-water diet | Low calcium, decreased oxalate, and increased water intake | Composite | 18 | 6 | 0.52 (0.29 to 0.95) | ●○○ | |
| Limited evidence suggests that the following dietary intervention may increase the risk of stone recurrence: | |||||||
| Low–animal protein, high-fiber, increased-bran, low-purine, adequate-calcium, and increased-fluid diet | Adequate calcium and increased fluid | Composite | –20 | 5 | 5.88 (1.39 to 24.92) | ●○○ | |
| Neither a high-fiber diet nor a reduced–animal protein diet as an isolated intervention had a statistically significant effect on stone recurrence. ●○○ | |||||||
| Adverse effects (reflected by withdrawals for any cause) were high in long-term trials; however, there were no significant differences in withdrawals between intervention and control groups. | |||||||
| Pharmacologic interventions ( | |||||||
Thiazide diuretics, citrate, and allopurinol each reduce the risk of calcium stone recurrence. ●●○
| |||||||
| Patients given thiazide diuretics or citrate, but not allopurinol, are more likely to withdraw from trials because of adverse effects compared with patients in the control group. | |||||||
| Baseline and follow-up biochemical evaluations to predict stone recurrence | |||||||
| The evidence is too limited to determine the role of baseline or follow-up biochemical measures in predicting stone recurrence outcomes. | |||||||
| Strength of evidence scale | |||||||
| High: ●●● There are consistent results from good-quality studies. Further research is very unlikely to change the conclusions. | |||||||
| Moderate: ●●○ Findings are supported, but further research could change the conclusions. | |||||||
| Low: ●○○ There are very few studies, or existing studies are flawed. | |||||||
| Insufficient: ○○○ Research is either unavailable or does not permit estimation of a treatment effect. | |||||||
ARR = absolute risk reduction (the difference in risk between the control group and the treatment group); CI = confidence interval; NNT = number needed to treat (the number of patients to be treated to find the benefit in one patient more than in the control group); RR = relative risk.
*—Composite end point refers to stones detected by either symptoms or scheduled radiography.
†—The recommended level of dietary calcium intake in this study was 1,200 mg per day.
Adapted from the Agency for Healthcare Research and Quality, Effective Health Care Program. Recurrent nephrolithiasis in adults: comparative effectiveness of preventive medical strategies. Clinician research summary. Rockville, Md.: Agency for Healthcare Research and Quality; August 2013. http://www.effectivehealthcare.ahrq.gov/ehc/products/274/1610/kidney-stone-clinician-130801.pdf. Accessed January 8, 2014.
Practice Pointers
Nephrolithiasis generally occurs when the urinary concentration of calcium, oxalate, or uric acid is high, or the urinary concentration of citrate is low. Overall, 80% of stones are composed of calcium oxalate or calcium phosphate; the remainder are struvite or uric acid stones.1 Dietary factors associated with stone formation include low oral fluid and calcium intake and high fructose consumption.1 The average lifetime recurrence rate is 30% to 40%; about one-half of these patients have just one recurrence.2
This Agency for Healthcare Research and Quality (AHRQ) review analyzed 28 randomized controlled trials (RCTs) addressing the effectiveness of biochemical analysis and dietary and pharmacologic treatments to prevent kidney stone recurrence.1 Almost all eligible trials were limited to patients with a history of calcium stones. Most trials reported the composite outcome of radiographically detected and symptomatic stone recurrence, thereby combining disease-oriented and patient-oriented outcomes.
Two small RCTs comparing increased fluid intake over three to five years to maintain urine output greater than 2 to 2.5 L per day vs. no treatment showed a reduced risk of the composite outcome of symptomatic stone passage or radiographic detection and an increased time to stone recurrence.3,4 One RCT (N = 1,009) found that reduced soft drink consumption in men with high baseline soft drink intake (median of 80 oz per week) was associated with a reduction in symptomatic stone formation, particularly in those whose soft drinks were acidified by phosphoric acid (e.g., colas).5
Seven RCTs included in the AHRQ review comparing patients taking thiazide diuretics (50 mg total daily dosage) over three years with patients in control groups showed a reduced risk of the composite outcome of radiographic stone detection or stone passage/removal in six pooled trials (N = 447), but no reduced risk of symptomatic stone recurrence in the one small trial (N = 51) reporting this outcome.1 Six RCTs included in the AHRQ review comparing citrate therapy in varying dosages vs. placebo over 25 months showed a reduction in the composite outcome of radiographic stone detection or stone passage/removal in four pooled studies (N = 197), but no difference in radiographic stone recurrence.1 Two RCTs compared patients taking allopurinol, 300 mg per day, with patients taking placebo or in control groups over 24 to 60 months and reported symptomatic stone recurrence or composite risk of radiographic stone detection or stone passage/removal.6,7 The one trial of 60 participants that reported symptomatic stone recurrence showed no difference between allopurinol and placebo in symptomatic stone recurrence,6 whereas pooled analysis of this and one other trial (N = 152) showed a reduced composite risk of recurrence.6,7
Adverse effects of thiazide diuretics include orthostatic reactions, gastrointestinal upset, erectile dysfunction, fatigue, and muscle symptoms. Gastrointestinal problems were the most commonly reported adverse effects in citrate trials, whereas adverse effects in allopurinol trials included rash and acute gout.1
Expert consensus guidelines recommend that patients with acute kidney stones undergo laboratory evaluation, including analysis of stone composition and possibly urine (spot urine dipstick test and microscopy or culture) and blood testing (e.g., measurement of creatinine, uric acid, ionized calcium).8 Patients at high risk of recurrence based on underlying family history, medical conditions, and type of stone should undergo further stone-specific biochemical testing. However, the AHRQ review identified no literature to determine whether such biochemical testing predicts treatment effectiveness.1
In summary, for patients with calcium kidney stones, increased oral fluid intake, reduced soft drink consumption, thiazide diuretics, citrate supplementation, and allopurinol appear to reduce risk of stone recurrence.
EDITOR'S NOTE: American Family Physician SOR ratings are different from the AHRQ Strength of Evidence (SOE) ratings.

