A 79-year-old man presented with a 20-year history of diarrhea that was diagnosed as irritable bowel syndrome. He had regular cycles of liquid stools (about 4 cups per day) for several days, followed by constipation with small, pellet-like stools for the next two days. He did not have hematochezia, nocturnal stooling, weight loss, ill contacts, or recent travels, and he did not own pets. Colonoscopy findings two years earlier were negative, other than poor bowel preparation. He used loperamide (Imodium) on days he had diarrhea.
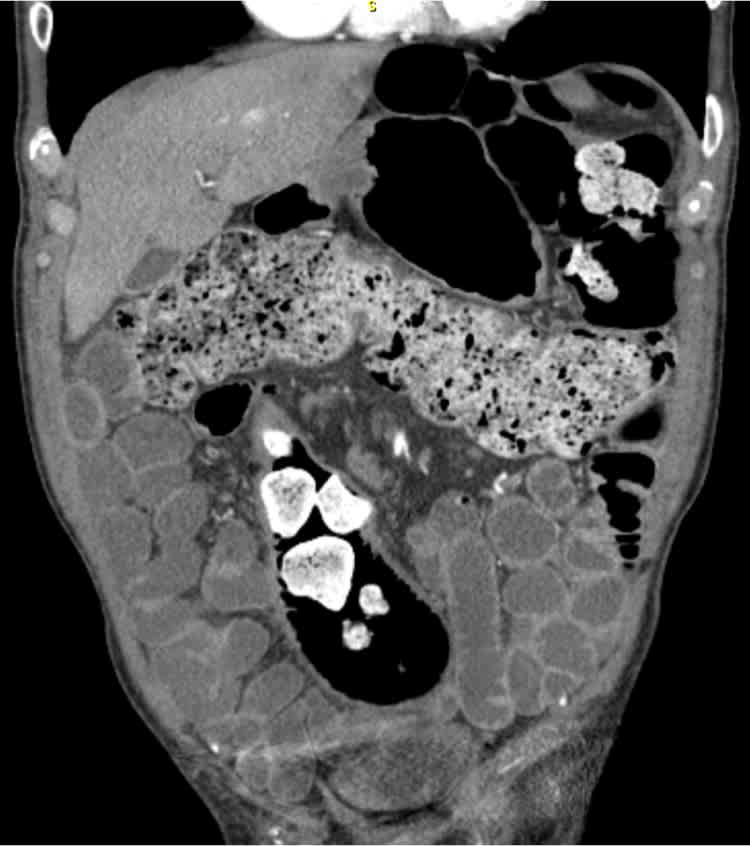
Physical examination revealed a palpable mass in the right lower quadrant that was firm but nontender. The mass was present while examining the patient in multiple positions. Rectal examination was significant for the presence of hard stool. Initial laboratory tests were notable only for a hemoglobin level of 11.9 g per dL (119 g per L). Because of the concern for possible malignancy, computed tomography enterography was performed (see accompanying figure).
Figure.
Question
Based on the patient's history, physical examination, and imaging findings, which one of the following is the most likely diagnosis?
A. Carcinoid syndrome.
B. Celiac disease.
C. Colorectal cancer.
D. Fecal impaction with overflow diarrhea.
E. Irritable bowel syndrome.
Discussion
The answer is D: fecal impaction with overflow diarrhea. Fecal impaction is common and can affect individuals of any age. It occurs in 2% of persons with long-standing constipation and may be associated with anatomic, metabolic, neurogenic, dietary, or pharmacologic etiologies.1 Groups at particular risk include nursing home residents; persons with advanced neurologic, psychiatric, or cardiac diseases; and persons taking medications that delay colonic transit.2–4 Fecal impaction usually occurs in the rectum and may lead to rectal distention and, ultimately, overflow of liquid stool around the impacted fecal mass. This may further result in fecal incontinence, depending on factors such as the degree of anorectal sensory impairment, pelvic floor muscle integrity, and mobility.5
Although fecal impaction with overflow diarrhea is not rare, it is often initially misdiagnosed or worsened with use of antidiarrheal medication. The patient history typically includes constipation and pellet-like stools alternating regularly with small-volume diarrhea (with or without incontinence). Although nonspecific, other symptoms may include rectal and/or abdominal discomfort, nausea, and anorexia. Complications of delayed diagnosis include stercoral ulceration, syncope, and systemic inflammatory response syndrome.6,7
Enemas may be sufficient to treat mild impaction, although manual disimpaction is indicated if enemas are unsuccessful. Surgical consultation should be obtained if the impaction cannot be resolved. A maintenance bowel regimen and minimization of constipating medications (e.g., anticholinergics) can reduce the likelihood of recurrence.
Carcinoid syndrome refers to the complex of symptoms related to carcinoid tumors. Symptoms can include flushing, diarrhea, or bronchospasm, but typically occur only in patients with hepatic metastases because the liver otherwise inactivates bioactive factors secreted into the portal circulation.
Celiac disease is characterized by small bowel mucosal inflammation from intolerance to dietary gluten and is most common in whites of northern European ancestry. It can occur at any age with varying presentations, including subclinical disease, diarrhea and bloating, and nongastrointestinal manifestations (e.g., arthritis, dermatitis herpetiformis, neuropsychiatric disease).
Colorectal cancer should be considered in patients with unexplained iron deficiency anemia, rectal bleeding, or a change in bowel habits. Patients older than 50 years are at highest risk of colorectal cancer, which underscores the importance of screening.
Irritable bowel syndrome usually presents as abdominal pain and altered bowel habits, including diarrhea, constipation, or alternating constipation and diarrhea. It is more common in younger patients and women. It should not be diagnosed until other etiologies are excluded, especially in patients older than 50 years or in patients with red flag symptoms.
Summary Table
| Condition | Characteristics |
|---|---|
| Carcinoid syndrome | A complex of symptoms such as flushing, diarrhea, and bronchospasm mediated by factors secreted by carcinoid tumors; symptoms from intestinal carcinoids occur only with hepatic metastases |
| Celiac disease | Inflammatory small bowel disorder that is a reaction to dietary gluten; symptoms vary but may include subclinical disease, diarrhea and bloating, and nongastrointestinal manifestations; most common in whites of northern European ancestry |
| Colorectal cancer | Should be considered in patients with iron deficiency anemia, rectal bleeding, or change in bowel habits; more common in those older than 50 years |
| Fecal impaction with overflow diarrhea | Rectal and/or abdominal discomfort, nausea, anorexia; intermittent leakage of liquid stool; hard stool mass palpable on digital rectal examination |
| Irritable bowel syndrome | Presents with abdominal pain and altered bowel habits (i.e., diarrhea, constipation, or both); diagnosed after ruling out other etiologies |

