
Am Fam Physician. 2014;89(11):872
Author disclosure: No relevant financial affiliations.
Tobacco use and obesity are linked to most deaths and significant disability in the United States, and family physicians are uniquely positioned to address these issues. This highlights a need for transforming primary care practices and teams to systematize the recognition and management of unhealthy behaviors, and for alternative payment models that support these efforts.
Tobacco use, obesity, unhealthy diet, and lack of physical activity are associated with roughly 65% of deaths and 35% of years of life lost to premature mortality or lived with disability in the United States.1 Family physicians play a key role in helping patients address these risk factors through clinic-based interventions and in collaboration with communities.2 Engagement in these efforts is consistent with the goals of family medicine to provide first-contact care, with a whole-person orientation, delivered in the context of family and community. Despite the potential reduction in preventable deaths and disability arising from decreased tobacco use and obesity, family physicians remain poorly reimbursed for the provision of related clinical services.3
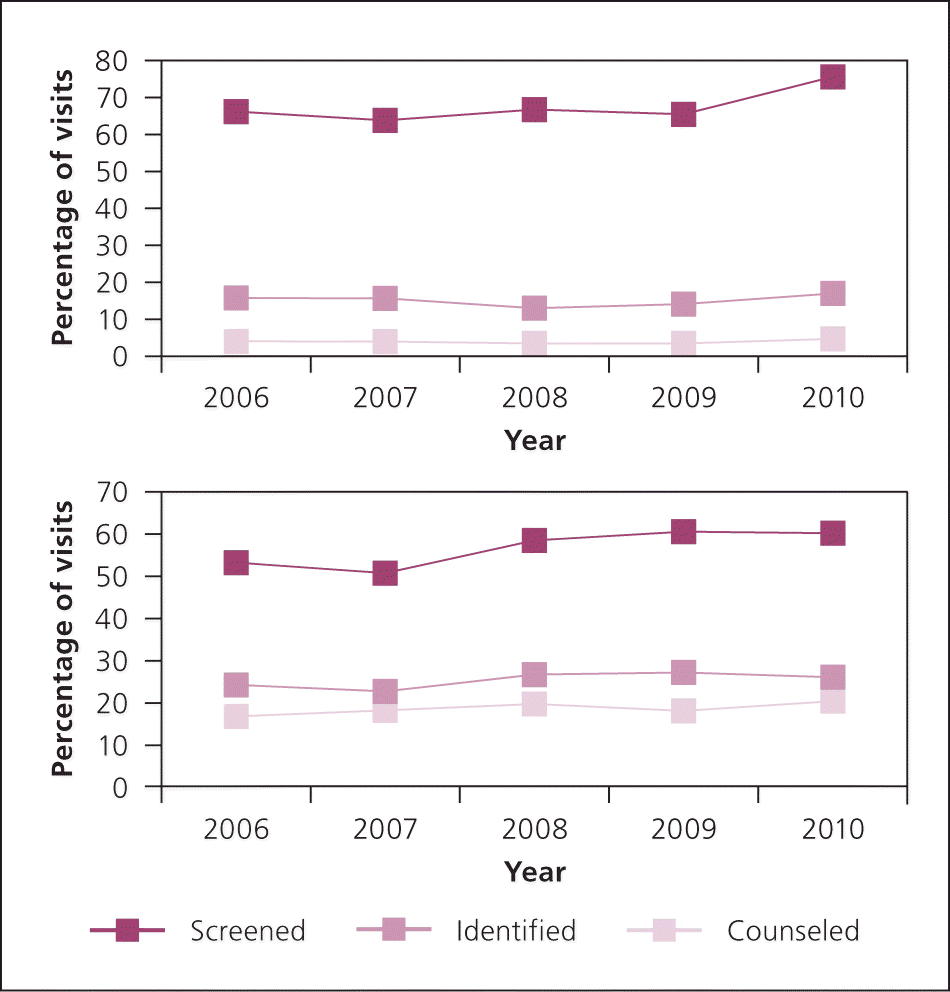
Data from the National Ambulatory Medical Care Survey reveal that from 2006 to 2010, reported screening among family physicians increased slightly for tobacco use (from 66% to 76% of all visits) and for diet, exercise, or weight problems (from 53% to 60% of all visits). Despite this apparent increase in screening, data from 2010 suggest that family physicians did not screen for tobacco use and obesity at as many as 24% and 40% of adult visits, respectively. These data are limited primarily by variations in quality and completeness of reporting over time and by the inability to identify factors that influence the provision of counseling after tobacco use or obesity has been identified.4 The accompanying figure illustrates screening rates.4
Tobacco use and obesity are considered winnable battles by the Centers for Disease Control and Prevention, but success will require the full engagement of primary care practices with their patient panels and within the communities they serve.5 This may require increased attention to these risk factors in training and continuing education, and practice transformation into team-based entities operating within “communities of solution.”6 Better reimbursement models are also likely necessary.
