Clinical Question
What is the best way to use the clinical examination to diagnose group A beta-hemolytic streptococcal (GABHS) pharyngitis?
Evidence Summary
Sore throat was the chief symptom in 1.3% of all outpatient office visits in 2010, and is even more common in primary care practice.1,2 An Australian study found that among families with at least one child three to 12 years of age, the incidence of sore throat was 33 and 14 episodes per 100 person-years in children and their parents, respectively. These episodes were caused by GABHS bacteria in about 40% of children and 25% of adults.3 Other studies in adults (with or without children) found that rates of GABHS pharyngitis were somewhat lower at 5% to 15% among those presenting to a physician with sore throat.4–6
A systematic review of studies in children and adults found that tonsillar exudates (positive likelihood ratio [LR+] = 3.4), pharyngeal exudates (LR+ = 2.1), and exposure to someone with strep throat in the previous two weeks (LR+ = 1.9) increase the likelihood of GABHS pharyngitis, whereas the absence of enlarged tonsils (negative likelihood ratio [LR–] = 0.6), the absence of tender cervical adenopathy (LR– = 0.6), and the absence of exudate (LR– = 0.7) decrease the likelihood.7 In children, scarlatiniform rash (LR+ = 3.9), palatine petechiae (LR+ = 2.7), pharyngeal exudates (LR+ = 1.9), vomiting (LR+ = 1.8), and tender cervical adenopathy (LR+ = 1.7) are all associated with GABHS pharyngitis.8
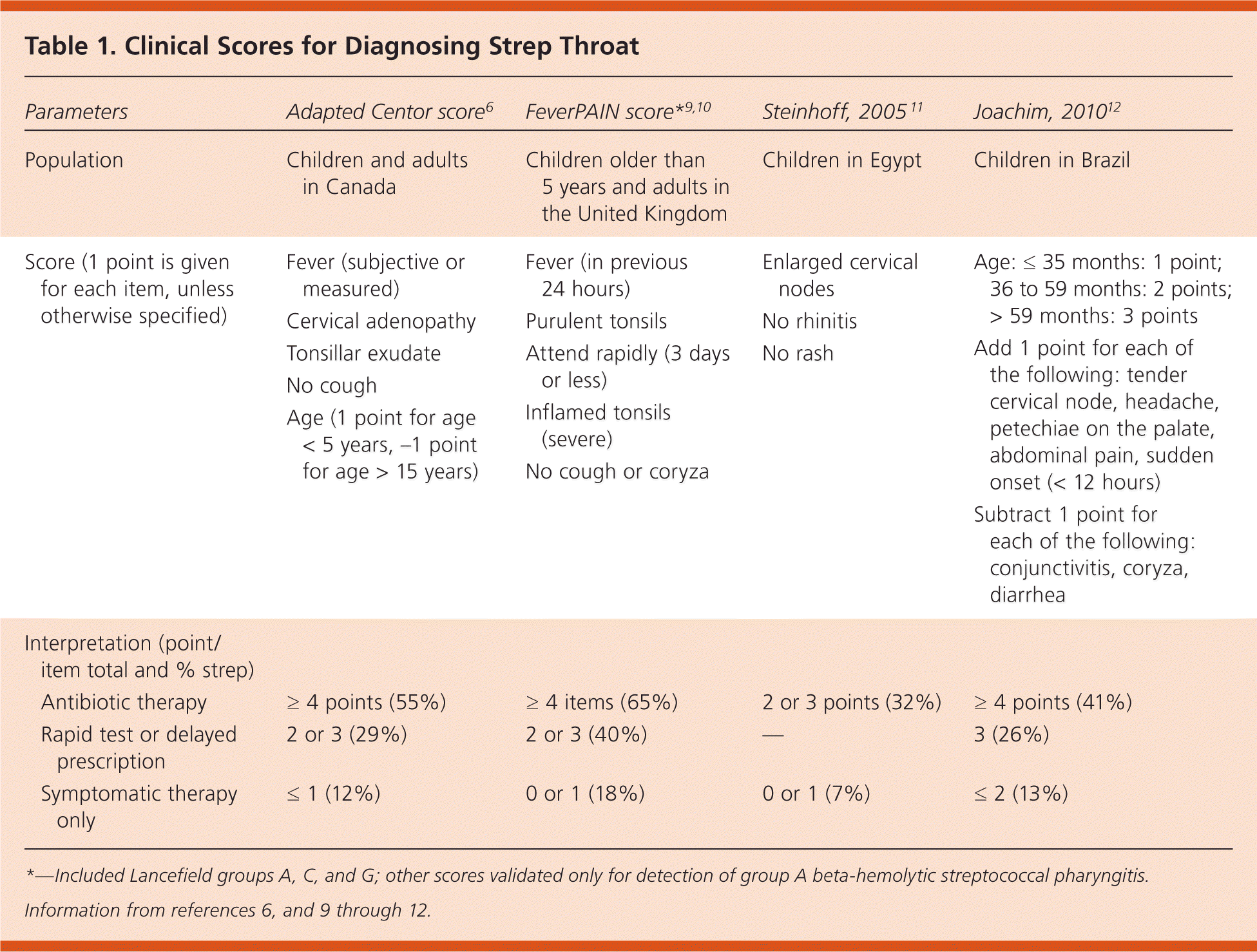
Because individual signs and symptoms have limited value, a number of clinical decision rules have been developed to diagnose GABHS pharyngitis (Table 1).6,9–12 The Centor score for strep pharyngitis was adapted by adding the patient's age; the adapted version has been validated in adults and children.6,13 A more recent study proposed the FeverPAIN (fever, purulence, attend rapidly, inflamed tonsils, no cough or coryza) score, which has been shown to reduce use of antibiotics by 30% without worsening other outcomes, reduce costs, and reduce antibiotic resistance. The FeverPAIN score was validated for detection of Lancefield groups A, C, and G streptococcus, resulting in somewhat higher percentages of those with strep throat in each risk group.9,10
Table 1. Clinical Scores for Diagnosing Strep Throat
| Parameters | Adapted Centor score6 | FeverPAIN score*9,10 | Steinhoff, 200511 | Joachim, 201012 | |
|---|---|---|---|---|---|
| Population | Children and adults in Canada | Children older than 5 years and adults in the United Kingdom | Children in Egypt | Children in Brazil | |
|
|
|
|
| |
| Interpretation (point/item total and % strep) | |||||
| Antibiotic therapy | ≥ 4 points (55%) | ≥ 4 items (65%) | 2 or 3 points (32%) | ≥ 4 points (41%) | |
| Rapid test or delayed prescription | 2 or 3 (29%) | 2 or 3 (40%) | — | 3 (26%) | |
| Symptomatic therapy only | ≤ 1 (12%) | 0 or 1 (18%) | 0 or 1 (7%) | ≤ 2 (13%) | |
*—Included Lancefield groups A, C, and G; other scores validated only for detection of group A beta-hemolytic streptococcal pharyngitis.
The World Health Organization has proposed a simple heuristic for use in underresourced settings: treat for GABHS pharyngitis in all children with pharyngeal exudate plus enlarged, tender cervical lymph nodes. Although this approach is highly specific (more than 90%), the sensitivity is very low (less than 15%), and it cannot be recommended.14 However, two recent studies have identified more sensitive scores with adequate specificity that can be used for children with sore throat in underresourced settings. One suggests that GABHS pharyngitis be empirically treated in any child with sore throat and at least two of the following: no rhinitis, no rash, or enlarged cervical nodes.11 Another score is somewhat more complex, taking into account age, symptoms suggesting GABHS pharyngitis, and symptoms suggesting viral pharyngitis.12
All of the scores summarized in Table 1 effectively stratify patients into high-, low-, and, in some cases, moderate-risk groups.6,9–12 Using empiric therapy for high-risk patients, symptomatic therapy and follow-up for low-risk patients, and delayed prescription or rapid antigen testing for moderate-risk patients is a sensible strategy. The adapted Centor strep score and the FeverPAIN score have been shown to reduce inappropriate antibiotic prescribing, an important goal in the management of pharyngitis.

