Motion sickness is a common syndrome that occurs upon exposure to certain types of motion. It is thought to be caused by conflict between the vestibular, visual, and other proprioceptive systems. Although nausea is the hallmark symptom, it is often preceded by stomach awareness, malaise, drowsiness, and irritability. Early self-diagnosis should be emphasized, and patients should be counseled about behavioral and pharmacologic strategies to prevent motion sickness before traveling. Patients should learn to identify situations that will lead to motion sickness and minimize the amount of unpleasant motion they are exposed to by avoiding difficult conditions while traveling or by positioning themselves in the most stable part of the vehicle. Slow, intermittent exposure to the motion can reduce symptoms. Other behavioral strategies include watching the true visual horizon, steering the vehicle, tilting their head into turns, or lying down with their eyes closed. Patients should also attempt to reduce other sources of physical, mental, and emotional discomfort. Scopolamine is a first-line medication for prevention of motion sickness and should be administered transdermally several hours before the anticipated motion exposure. First-generation antihistamines, although sedating, are also effective. Nonsedating antihistamines, ondansetron, and ginger root are not effective in the prevention and treatment of motion sickness.
Motion sickness is a syndrome that occurs when a patient is exposed to certain types of motion and usually resolves soon after its cessation. It is a common response to motion stimuli during travel. Although nausea is a hallmark symptom, the syndrome includes symptoms ranging from vague malaise to completely incapacitating illness. These symptoms, which can affect the patient's recreation, employment, and personal safety, can occur within minutes of experiencing motion and can last for several hours after its cessation.
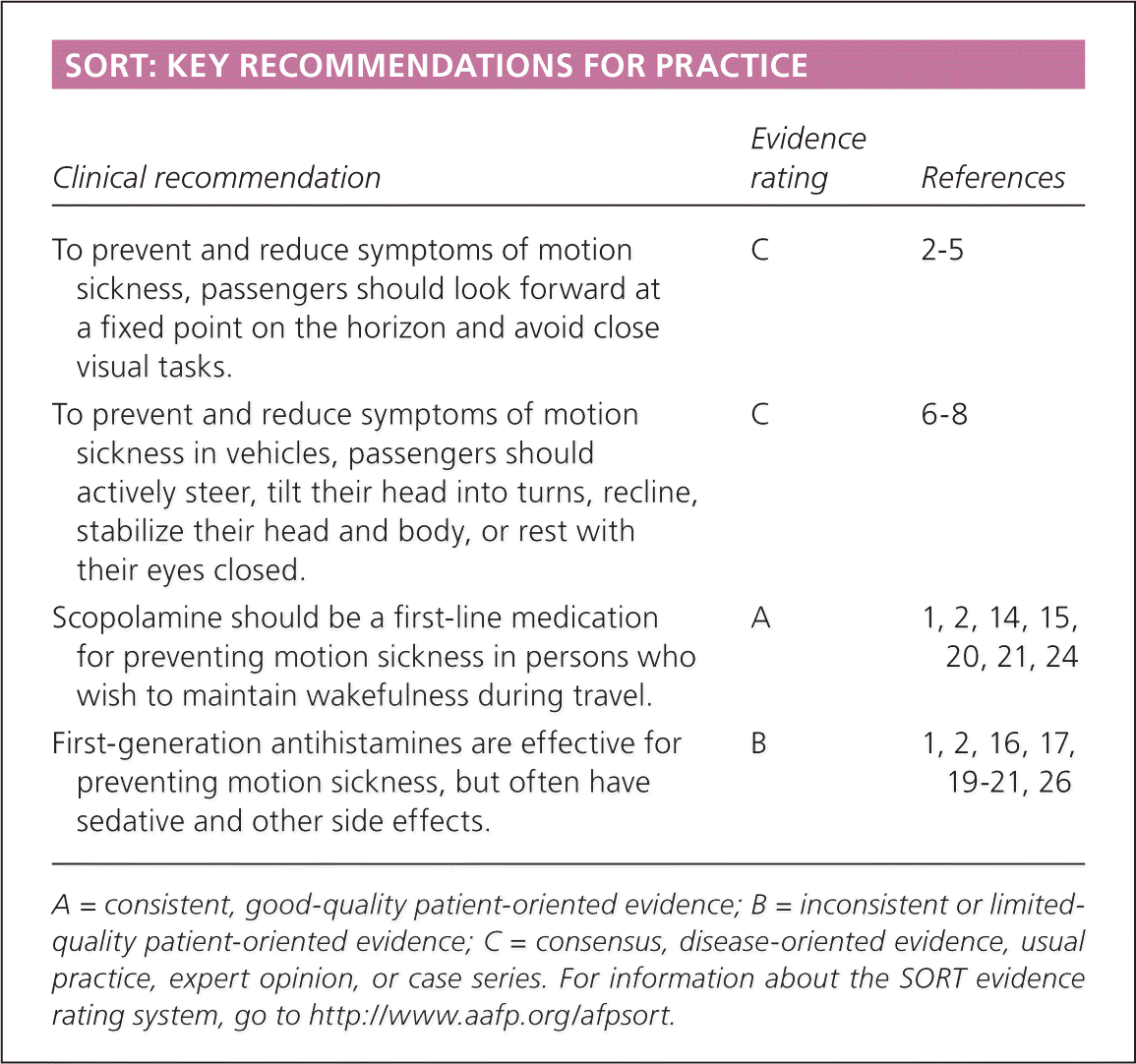
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| To prevent and reduce symptoms of motion sickness, passengers should look forward at a fixed point on the horizon and avoid close visual tasks. | C | 2–5 |
| To prevent and reduce symptoms of motion sickness in vehicles, passengers should actively steer, tilt their head into turns, recline, stabilize their head and body, or rest with their eyes closed. | C | 6–8 |
| Scopolamine should be a first-line medication for preventing motion sickness in persons who wish to maintain wakefulness during travel. | A | 1, 2, 14, 15, 20, 21, 24 |
| First-generation antihistamines are effective for preventing motion sickness, but often have sedative and other side effects. | B | 1, 2, 16, 17, 19–21, 26 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Nearly all persons will have symptoms in response to severe motion stimuli, and a history of motion sickness best predicts future symptoms.1 Females, children two to 15 years of age, and persons with conditions associated with nausea (e.g., early pregnancy, migraines, vestibular syndromes) report increased susceptibility.
Etiology
The pathogenesis of motion sickness is not clearly understood, but it is thought to be related to conflict between the vestibular, visual, and other proprioceptive systems.2 Rotary, vertical, and low-frequency motions produce more symptoms than linear, horizontal, and high-frequency motions.1
Clinical Presentation
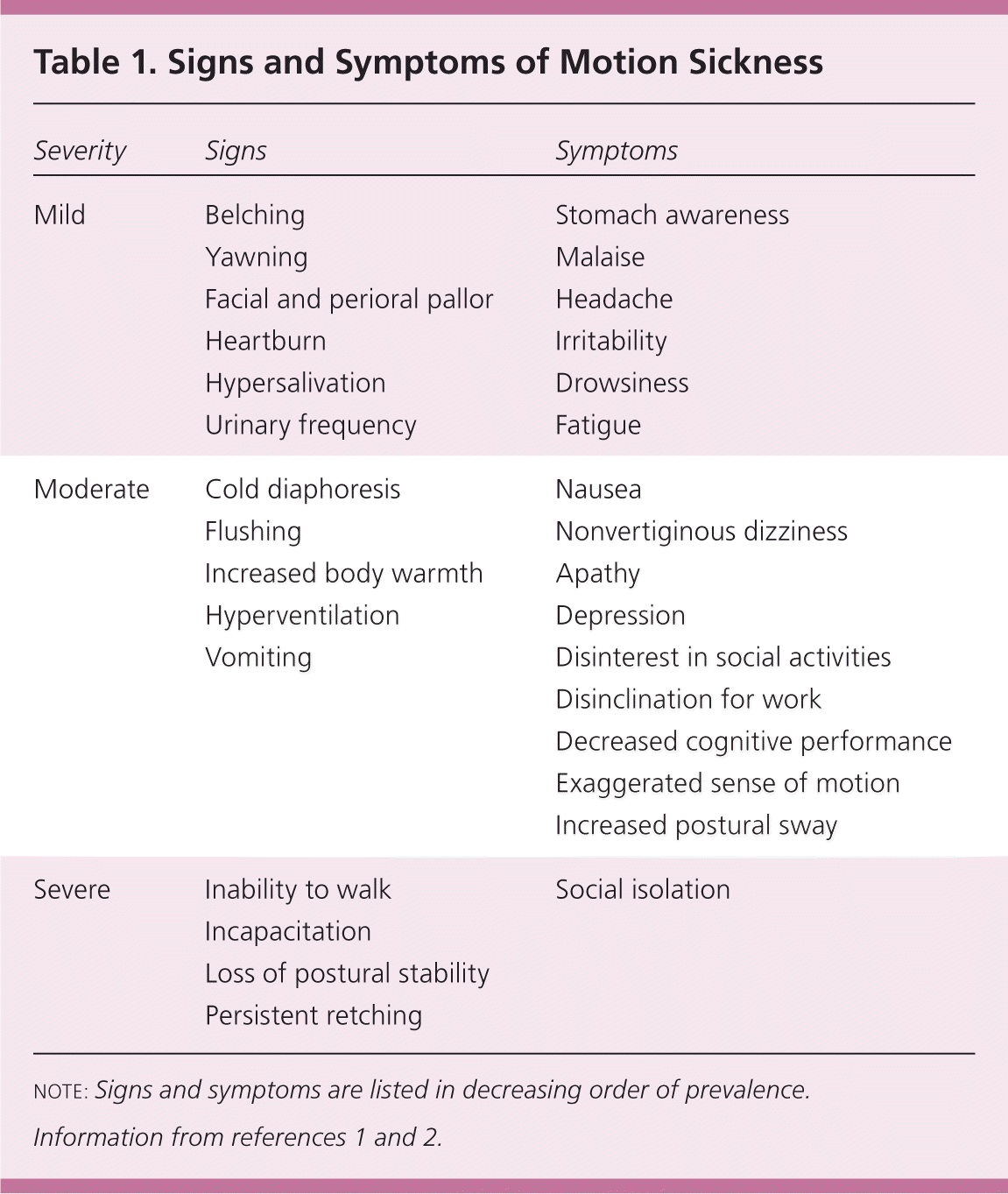
Although nausea may be the first recognized symptom of motion sickness, it is almost always preceded by other subtle symptoms such as stomach awareness (i.e., a sensation of fullness in the epigastrium), malaise, drowsiness, and irritability. Failure to attribute early symptoms to motion sickness may lead to delays in diagnosis and treatment. Although mild symptoms are common, severely debilitating symptoms are rare2 (Table 11,2 ).
Table 1. Signs and Symptoms of Motion Sickness
| Severity | Signs | Symptoms |
|---|---|---|
| Mild |
|
|
| Moderate |
|
|
| Severe |
|
|
note: Signs and symptoms are listed in decreasing order of prevalence.
Behavioral Interventions
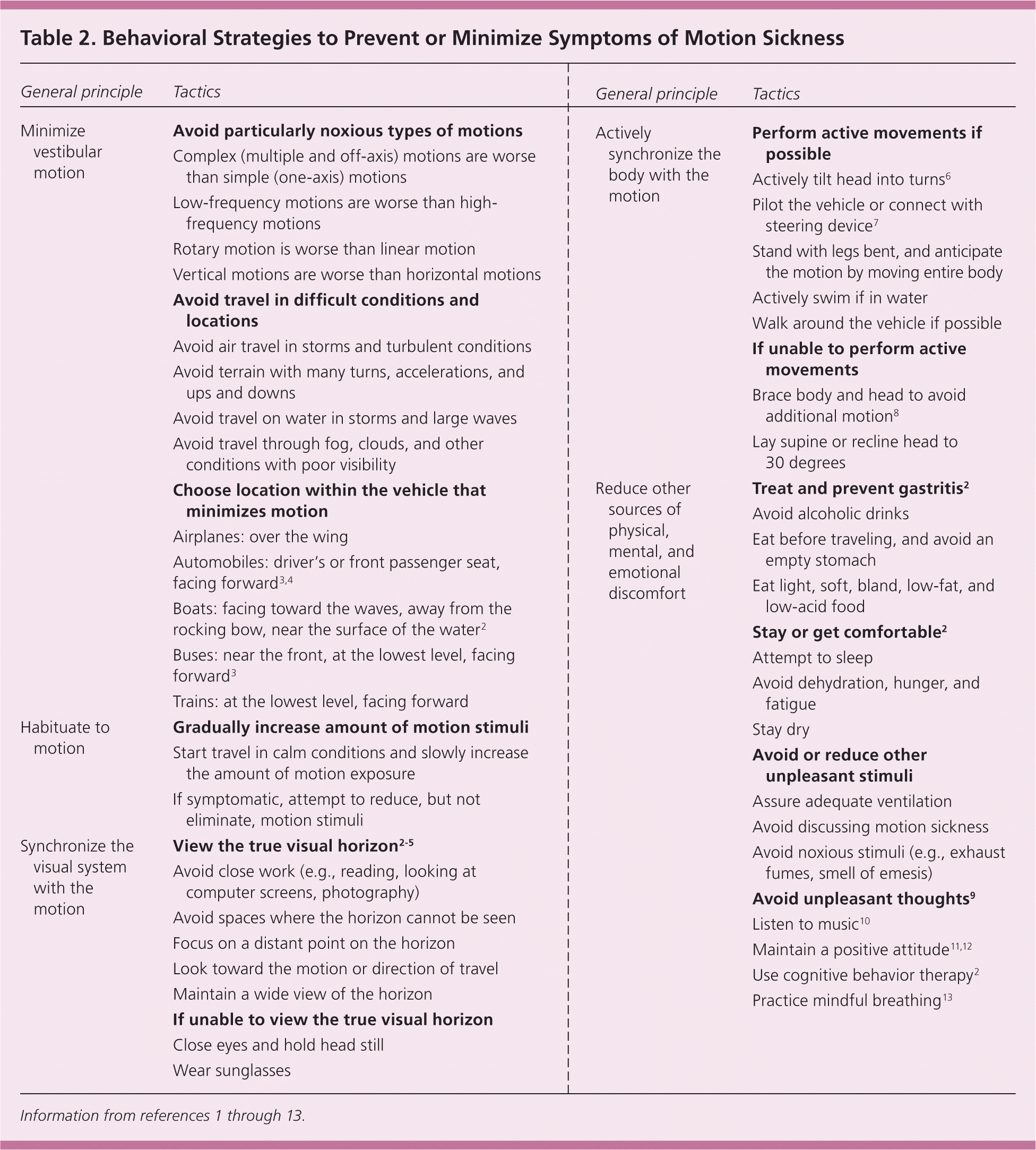
Prevention of motion sickness is more effective than treating symptoms after they have occurred. Therefore, patients should learn to identify situations that may lead to motion sickness and be able to initiate behavioral strategies to prevent or minimize symptoms1,2 (Table 21–13 ).
Table 2. Behavioral Strategies to Prevent or Minimize Symptoms of Motion Sickness
| General principle | Tactics |
|---|---|
| Minimize vestibular motion |
|
| Habituate to motion |
|
| Synchronize the visual system with the motion |
|
| Actively synchronize the body with the motion |
|
| Reduce other sources of physical, mental, and emotional discomfort |
|
MINIMIZE VESTIBULAR MOTION
Patients should be advised to avoid traveling in difficult weather conditions. If they must travel, they should sit in the part of the vehicle with the least amount of rotational and vertical motion.2 This is usually the lowest level in trains and buses, close to water level and in the center of boats, and over the wing on airplanes.
HABITUATE TO MOTION
With continuous exposure to motion, symptoms of motion sickness will usually subside in one to two days. Alternatively, slow, intermittent habituation to motion is an effective strategy to reduce symptoms.1 For example, spending the first night aboard a boat in the marina, followed by a day acclimating in the harbor, is preferable to going straight into the open ocean.
SYNCHRONIZE THE VISUAL SYSTEM WITH THE MOTION
A small study found that focusing on the true horizon (skyline) minimized symptoms of motion sickness.5 A survey of 3,256 bus passengers suggested that forward vision was helpful in reducing symptoms.3 Another study indicated that forward vision in a car can reduce symptoms.4
ACTIVELY SYNCHRONIZE THE BODY WITH THE MOTION
Actively steering the vehicle is an accepted strategy for reducing symptoms of motion sickness, although evidence is limited.7 Additionally, a small study of automobile passengers found that actively tilting the head into turns was effective in preventing symptoms.6 A survey of 260 cruise ship passengers supported the common advice to recline and passively stabilize themselves if they are unable to initiate active movements.8
REDUCE OTHER SOURCES OF PHYSICAL, MENTAL, AND EMOTIONAL DISCOMFORT
Frequent consumption of light, soft, bland, low-fat, and low-acid food can minimize symptoms of motion sickness.2 Treating gastritis is useful,2 as is avoiding nausea-inducing stimuli (e.g., alcohol, noxious odors). Discussing symptoms with others can exacerbate the condition. Passengers should be well rested, well hydrated, well fed, and comfortable before beginning travel. Small studies have shown that cognitive behavior therapy, mindful breathing, and listening to music may also reduce symptoms of motion sickness.9,10,13
Medications
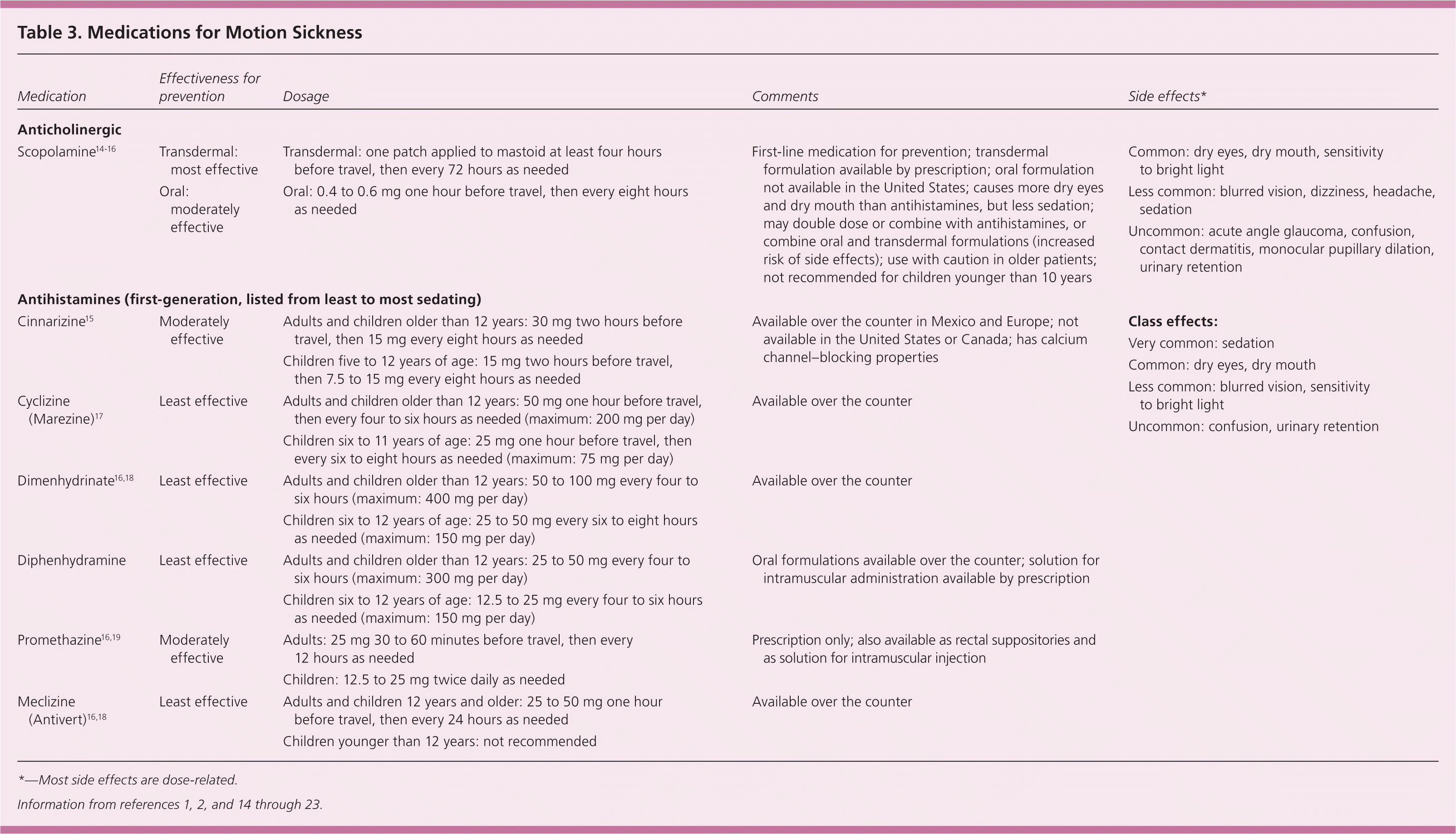
Medications are most effective when taken prophylactically before traveling, or as soon as possible after the onset of symptoms2 (Table 31,2,14–23 ). Medications are most effective when combined with behavioral strategies. To familiarize themselves with common side effects, patients should first take medications in a comfortable environment before using them for motion sickness during travel.
Table 3. Medications for Motion Sickness
| Medication | Effectiveness for prevention | Dosage | Comments | Side effects* |
|---|---|---|---|---|
| Anticholinergic | ||||
| Scopolamine14–16 | Transdermal: most effective | Transdermal: one patch applied to mastoid at least four hours before travel, then every 72 hours as needed |
|
|
| Oral: moderately effective | Oral: 0.4 to 0.6 mg one hour before travel, then every eight hours as needed | |||
| Antihistamines (first-generation, listed from least to most sedating) | ||||
| Cinnarizine15 | Moderately effective |
|
|
|
| Cyclizine (Marezine)17 | Least effective |
|
| |
| Dimenhydrinate16,18 | Least effective |
|
| |
| Diphenhydramine | Least effective |
|
| |
| Promethazine16,19 | Moderately effective |
|
| |
| Meclizine (Antivert)16,18 | Least effective |
|
| |
*—Most side effects are dose-related.
SCOPOLAMINE
Scopolamine, an anticholinergic, is a first-line option for preventing motion sickness in persons who wish to maintain wakefulness during travel.2,20,24 A Cochrane review of 14 randomized controlled trials (RCTs) showed that scopolamine is effective for the prevention of motion sickness.14 A more recent RCT of 76 naval crew members showed that transdermal scopolamine is more effective and has fewer side effects than the antihistamine cinnarizine (not available in the United States).15 If the recommended dose of scopolamine does not adequately relieve symptoms, the dose may be doubled. Adding a second patch of transdermal scopolamine was well tolerated in a small RCT of 20 sailors.25
ANTIHISTAMINES
First-generation antihistamines have been used to treat motion sickness since the 1940s.1 They are generally recommended for patients who can tolerate their sedative effects.2,20 Cyclizine (Marezine), dimenhydrinate, promethazine, and meclizine (Antivert) demonstrated effectiveness in small RCTs of varying quality.16–19 Nonsedating antihistamines are not effective in preventing or treating motion sickness.26
OTHER MEDICATIONS
Benzodiazepines are occasionally administered for severe symptoms of motion sickness and have been proven effective in a single small study.27 The serotonin agonist rizatriptan (Maxalt) reduced motion sickness symptoms in a single RCT of 25 patients with recurrent migraines.28 The serotonin antagonist ondansetron (Zofran) is ineffective for the prevention and treatment of motion sickness.29,30
COMPLEMENTARY AND ALTERNATIVE THERAPIES
Although ginger root is often reported to prevent motion sickness, it had no statistically significant effects in an RCT of 80 naval cadets.31 A single RCT of pregnant women showed that stimulation of the P6 acupressure point on the anterior wrist increased their tolerance of motion stimuli.32 Controlled trials of behavioral, pharmacologic, or alternative therapies for motion sickness have demonstrated strong placebo effects. Therefore, treatments are likely to be most effective if the patient believes that they will work.11,12
Data Sources: PubMed was searched using the MeSH headings motion sickness, ships, movement, space motion sickness, and travel. Additional searches were performed in Essential Evidence Plus, UpToDate, Medscape, and BMJ Clinical Evidence. Search dates: March 2012 through March 2014.

