Childhood constipation is common and almost always functional without an organic etiology. Stool retention can lead to fecal incontinence in some patients. Often, a medical history and physical examination are sufficient to diagnose functional constipation. Further evaluation for Hirschsprung disease, a spinal cord abnormality, or a metabolic disorder may be warranted in a child with red flags, such as onset before one month of age, delayed passage of meconium after birth, failure to thrive, explosive stools, and severe abdominal distension. Successful therapy requires prevention and treatment of fecal impaction, with oral laxatives or rectal therapies. Polyethylene glycol–based solutions have become the mainstay of therapy, although other options, such as other osmotic or stimulant laxatives, are available. An increase in dietary fiber may improve the likelihood that laxatives can be discontinued in the future. Education is equally important as medical therapy and should include counseling families to recognize withholding behaviors; to use behavior interventions, such as regular toileting and reward systems; and to expect a chronic course with prolonged therapy, frequent relapses, and a need for close follow-up. Referral to a subspecialist is recommended only when there is concern for organic disease or when the constipation persists despite adequate therapy.
Constipation is one of the most common chronic disorders of childhood, affecting 1% to 30% of children worldwide.1 Constipation is responsible for 3% of all primary care visits for children and 10% to 25% of pediatric gastroenterology visits.2 Children with constipation cost the health care system three times as much as children without constipation,3 and the negative effect on quality of life often persists into adulthood.4
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A history and physical examination are usually sufficient to distinguish functional constipation from constipation caused by organic conditions. | C | 2, 10 |
| Abdominal radiography is of limited value in diagnosing chronic constipation because it lacks interobserver reliability and accuracy. | C | 2, 14, 15 |
| Polyethylene glycol–based solutions (Miralax) are effective, easy to administer, noninvasive, and well tolerated in children with constipation. | A | 27, 30, 34 |
| The addition of laxatives is more effective than behavior modification alone in children with constipation. | B | 30, 31 |
| The addition of enemas to oral laxative regimens does not improve outcomes in children with severe constipation. | B | 32 |
| Most children with functional constipation require prolonged treatment. | C | 19, 35 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Definition
The Rome III criteria are the most accepted criteria for diagnosing childhood constipation (Table 1).5,6 However, the time duration does not need to be fulfilled to start therapy because there is evidence that early treatment favorably affects outcome.2
Table 1. Rome III Diagnostic Criteria for Diagnosing Functional Constipation in Children

| At least two of the following in a child with a developmental age younger than four years* | |
| Two or fewer bowel movements per week | |
| At least one episode of incontinence per week after the acquisition of toileting skills | |
| History of excessive stool retention | |
| History of painful or hard bowel movements | |
| Presence of a large fecal mass in the rectum | |
| History of large diameter stools that may obstruct the toilet | |
| At least two of the following in a child with a developmental age of four years or older with insufficient criteria for irritable bowel syndrome† | |
| Two or fewer bowel movements in the toilet per week | |
| At least one episode of fecal incontinence per week | |
| History of retentive posturing or excessive voluntary stool retention | |
| History of painful or hard bowel movements | |
| Presence of a large fecal mass in the rectum | |
| History of large diameter stools that may obstruct the toilet | |
*—Criteria must be fulfilled for at least one month. Accompanying symptoms may include irritability, decreased appetite, and/or early satiety, and they may disappear immediately following passage of a large stool.
†—Criteria must be fulfilled at least once a week for at least two months.
Adapted with permission from Rasquin A, Di Lorenzo C, Forbes D, et al. Childhood functional gastrointestinal disorders: child/adolescent. Gastroenterology . 2006; 130(5):1533, and Hyman PE, Milla PJ, Benninga MA, Davidson GP, Fleisher DF, Taminiau J. Childhood functional gastrointestinal disorders: neonate/toddler. Gastroenterology . 2006;130(5):1524.
Normal Defecation Patterns
Parents often worry that their child's bowel movements are too infrequent. The number of bowel movements a child has in a day decreases with age and reaches adult frequencies during the preschool years.7,8 An infant averages three to four stools a day in the first week of life, two stools a day later in infancy and the toddler years, and once a day to every other day after the preschool years.9 Many healthy breastfed infants go several days or longer without a bowel movement.2 Thus, less frequent defecation patterns may be normal and must be considered in the context of stool caliber, associated symptoms, and physical examination findings.
Etiology and Pathophysiology
Outside of the neonatal period, childhood constipation is usually functional (i.e., there is no evidence of an organic condition).2,10 Functional constipation is most commonly caused by painful bowel movements that prompt the child to voluntarily withhold stool. To avoid the passage of another painful bowel movement, the child will contract the anal sphincter or gluteal muscles by stiffening his or her body, hiding in a corner, rocking back and forth, or fidgeting with each urge to defecate. Parents often confuse these withholding behaviors as straining to defecate. Withholding of stool can lead to prolonged fecal stasis in the colon with reabsorption of fluid, causing the stool to become harder, larger, and more painful to pass. Over time, as the rectum stretches to accommodate the retained fecal mass, rectal sensation decreases, and fecal incontinence may develop. This cycle commonly coincides with toilet training, changes in routine or diet, stressful events, illness, or lack of accessible toilets, or occurs in a busy child who defers defecation.
Fecal Incontinence
Fecal incontinence is the voluntary or involuntary passage of feces in the underwear or in socially inappropriate places in a child with a developmental age of at least four years. It occurs in 1% to 4% of school-aged children and is almost always associated with underlying constipation.11 Fecal incontinence may also be associated with urinary incontinence.
The pathophysiology of fecal incontinence is poorly understood. An interaction of behavioral and physiologic factors is thought to cause long-standing functional constipation with overflow incontinence.12 Families may incorrectly confuse fecal incontinence for diarrhea or lack of attention. Fecal incontinence often improves when the stool retention is treated.13
Clinical Diagnosis
A history and physical examination are usually sufficient to distinguish functional constipation from constipation caused by an organic condition.2,10 A medical history should include the family's definition of constipation and a careful review of the frequency, consistency, and size of stools; age at onset of symptoms; timing of meconium passage after birth; recent stressors; previous and active therapies; presence of withholding behaviors, pain, or bleeding with bowel movements; abdominal pain; fecal incontinence; and systemic symptoms (Table 2).2 The presence of withholding behaviors supports the diagnosis of functional constipation. Further evaluation may be warranted in children with red flags that might suggest an organic etiology (Table 3).2
Table 2. Components of a Medical History in the Evaluation of Childhood Constipation
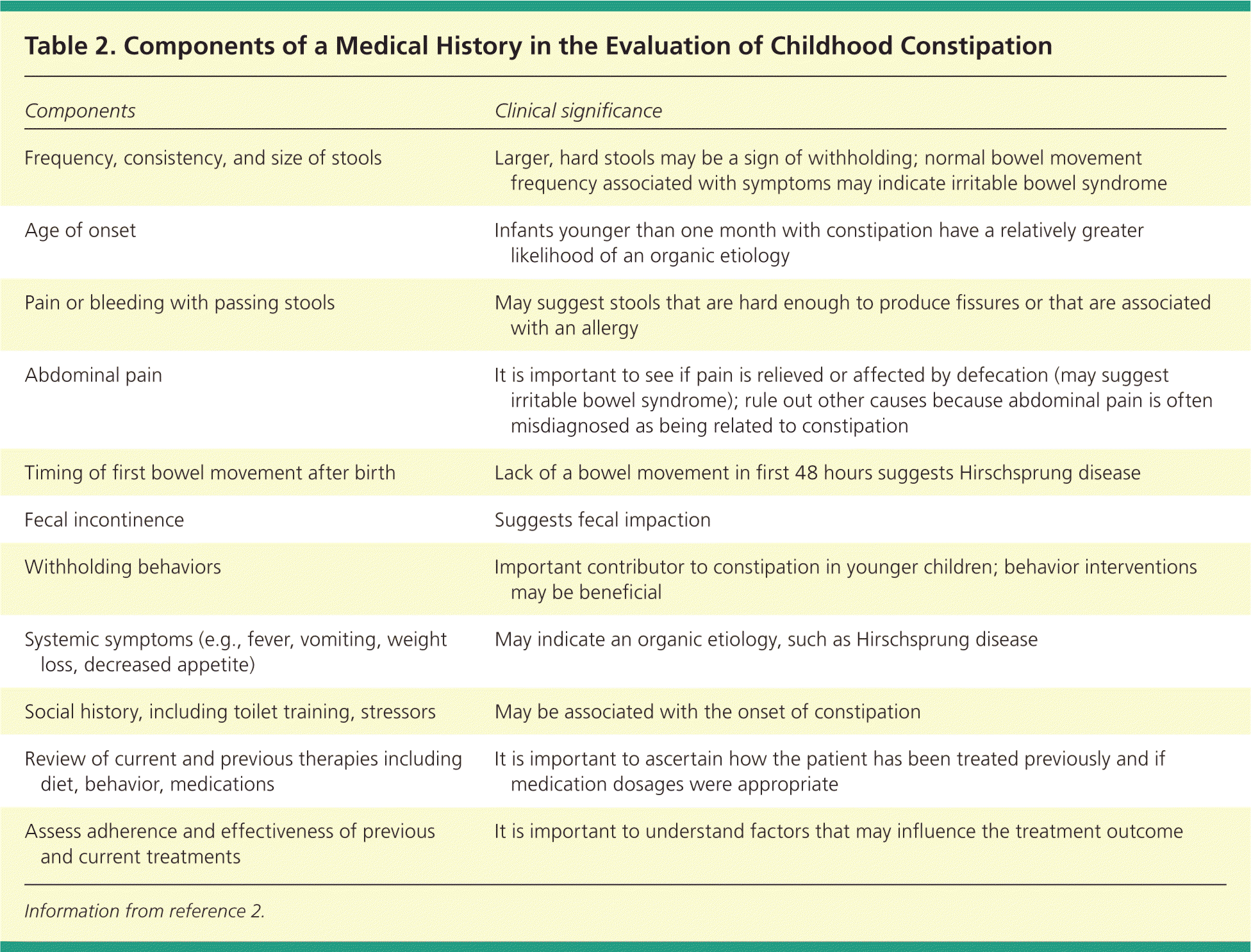
| Components | Clinical significance |
|---|---|
| Frequency, consistency, and size of stools | Larger, hard stools may be a sign of withholding; normal bowel movement frequency associated with symptoms may indicate irritable bowel syndrome |
| Age of onset | Infants younger than one month with constipation have a relatively greater likelihood of an organic etiology |
| Pain or bleeding with passing stools | May suggest stools that are hard enough to produce fissures or that are associated with an allergy |
| Abdominal pain | It is important to see if pain is relieved or affected by defecation (may suggest irritable bowel syndrome); rule out other causes because abdominal pain is often misdiagnosed as being related to constipation |
| Timing of first bowel movement after birth | Lack of a bowel movement in first 48 hours suggests Hirschsprung disease |
| Fecal incontinence | Suggests fecal impaction |
| Withholding behaviors | Important contributor to constipation in younger children; behavior interventions may be beneficial |
| Systemic symptoms (e.g., fever, vomiting, weight loss, decreased appetite) | May indicate an organic etiology, such as Hirschsprung disease |
| Social history, including toilet training, stressors | May be associated with the onset of constipation |
| Review of current and previous therapies including diet, behavior, medications | It is important to ascertain how the patient has been treated previously and if medication dosages were appropriate |
| Assess adherence and effectiveness of previous and current treatments | It is important to understand factors that may influence the treatment outcome |
Information from reference 2.
Table 3. Red Flags Suggesting an Organic Cause of Constipation in Children
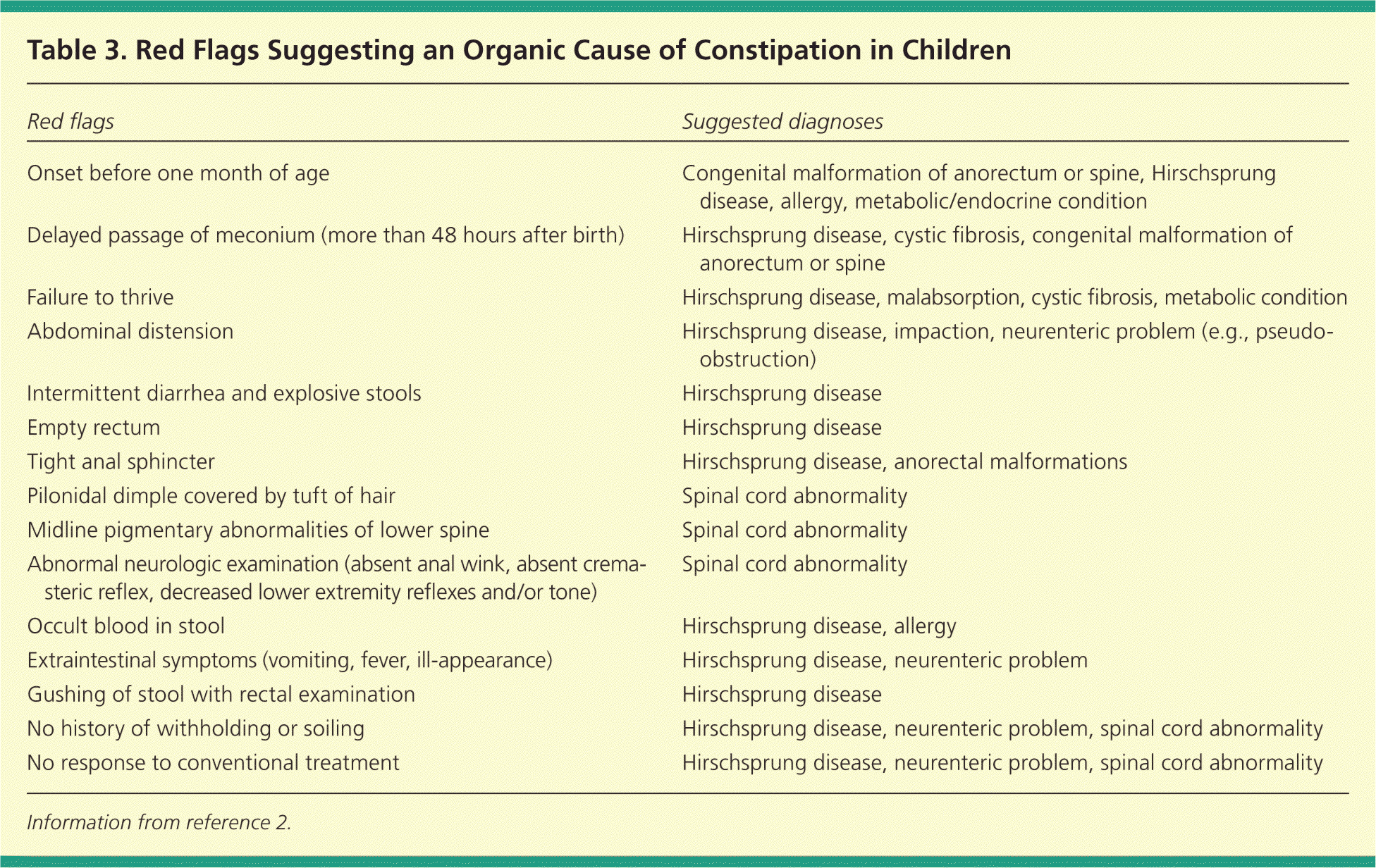
| Red flags | Suggested diagnoses |
|---|---|
| Onset before one month of age | Congenital malformation of anorectum or spine, Hirschsprung disease, allergy, metabolic/endocrine condition |
| Delayed passage of meconium (more than 48 hours after birth) | Hirschsprung disease, cystic fibrosis, congenital malformation of anorectum or spine |
| Failure to thrive | Hirschsprung disease, malabsorption, cystic fibrosis, metabolic condition |
| Abdominal distension | Hirschsprung disease, impaction, neurenteric problem (e.g., pseudo-obstruction) |
| Intermittent diarrhea and explosive stools | Hirschsprung disease |
| Empty rectum | Hirschsprung disease |
| Tight anal sphincter | Hirschsprung disease, anorectal malformations |
| Pilonidal dimple covered by tuft of hair | Spinal cord abnormality |
| Midline pigmentary abnormalities of lower spine | Spinal cord abnormality |
| Abnormal neurologic examination (absent anal wink, absent cremasteric reflex, decreased lower extremity reflexes and/or tone) | Spinal cord abnormality |
| Occult blood in stool | Hirschsprung disease, allergy |
| Extraintestinal symptoms (vomiting, fever, ill-appearance) | Hirschsprung disease, neurenteric problem |
| Gushing of stool with rectal examination | Hirschsprung disease |
| No history of withholding or soiling | Hirschsprung disease, neurenteric problem, spinal cord abnormality |
| No response to conventional treatment | Hirschsprung disease, neurenteric problem, spinal cord abnormality |
Information from reference 2.
Physical examination should include a review of growth parameters, an abdominal examination, an external examination of the perineum and perianal area, an evaluation of the thyroid and spine, and a neurologic evaluation for appropriate reflexes (cremasteric, anal wink, patellar). A digital examination of the anorectum is recommended to assess for perianal sensation, anal tone, rectum size, anal wink, and amount and consistency of stool in the rectum. However, in children with normal neonatal courses or clear withholding behaviors, or in whom trauma is suspected, the rectal examination may be deferred. A test for occult blood in the stool should be performed in all infants with constipation and in any child with constipation who has pain, failure to thrive, diarrhea, or a family history of colon cancer or polyps. The presence of a hard mass in the lower abdomen combined with a dilated rectum filled with hard stool indicates fecal impaction.
Abdominal radiography is of limited value in diagnosing chronic constipation because it lacks interobserver reliability and accuracy.2,14,15 It should be reserved for specific clinical circumstances in which a rectal examination is unreasonable (e.g., in a child with a history of trauma) or the diagnosis is uncertain.
Differential Diagnosis
Table 4 outlines the differential diagnosis of constipation in children and the recommended diagnostic evaluations.2 The age of the patient must be carefully considered.
Table 4. Differential Diagnosis of Constipation in Children

| Conditions | Recommended diagnostic evaluation | ||
|---|---|---|---|
| Functional constipation | History and physical examination; no testing | ||
| Anatomic malformations of the colon and rectum | |||
| Imperforate anus, anal or colonic stenosis, anteriorly displaced anus | Physical examination, barium enema | ||
| Spinal cord abnormalities | |||
| Meningomyelocele, spinal cord tumor or trauma, tethered cord | Spinal magnetic resonance imaging, anorectal manometry, urodynamics | ||
| Metabolic conditions | |||
| Hypothyroidism | Thyroid studies | ||
| Hypercalcemia, hyperkalemia | Serum calcium and potassium levels | ||
| Diabetes mellitus | Fasting glucose level | ||
| Diabetes insipidus | Serum and urine osmolarity | ||
| Neuropathic gastrointestinal disorders | |||
| Hirschsprung disease, internal anal sphincter achalasia | Anorectal manometry, rectal suction biopsy | ||
| Visceral myopathy/neuropathy | Colonic manometry | ||
| Drug use/toxin exposure | |||
| Opiates, phenobarbital, anticholinergics and attention-deficit/hyperactivity disorder drugs, antacids and sucralfate (Carafate), antidepressants, antihypertensives | History, drug level | ||
| Lead toxicity | Lead level | ||
| Other systemic disorders | |||
| Celiac disease | Tissue transglutaminase | ||
| IgA, total IgA, endoscopy | |||
| Cystic fibrosis | Sweat test | ||
| Cow's milk protein intolerance | Cow's milk elimination | ||
| Connective tissue disorder, mitochondrial disorders | Special testing | ||
| Psychiatric disorders | Psychological and psychiatric evaluation | ||
IgA = immunoglobulin A.
Information from reference 2.
YOUNG INFANTS
The likelihood of an organic etiology for constipation is relatively greater in infants younger than six months, and particularly in those younger than three months. Hirschsprung disease must be considered in infants with delayed passage of meconium (more than 48 hours after birth) or other red flags, even in the setting of normal findings on barium enema examination. Hirschsprung disease is the most common cause of lower intestinal obstruction in neonates. A delayed diagnosis can result in enterocolitis, a potentially fatal complication that causes fever; abdominal distension; and explosive, bloody diarrhea.16 Patients with suspected Hirschsprung disease should be referred to a medical center with a pediatric gastroenterologist and surgeon for confirmatory testing with rectal suction biopsy.
If Hirschsprung disease is excluded in an infant with delayed passage of meconium, cystic fibrosis and other anatomic malformations should be considered. The physical examination of a young infant should assess the position and patency of the anus and include a neurologic examination to evaluate for congenital anomalies of the anus and spine (e.g., anteriorly displaced anus, anal stenosis, imperforate anus, spina bifida, tethered cord). Breastfed infants require special consideration because in the absence of red flags or other medical issues, they require no further workup for infrequent bowel movements.
OLDER CHILDREN
Further evaluation is indicated in older children with red flags or with intractable constipation despite strict adherence to therapy. Laboratory studies may be performed to evaluate for systemic diseases, such as thyroid disease, other metabolic diseases, celiac disease, or lead toxicity. Motility studies (e.g., anorectal manometry) can assess for sphincter abnormalities, such as Hirschsprung disease or a nonrelaxing internal anal sphincter. Magnetic resonance imaging of the spine may be necessary to evaluate for a tethered cord, spinal cord tumor, or sacral agenesis.17 A trial of a cow's milk–free diet may also be considered because constipation can be caused by intolerance to cow's milk, especially in young children with anal fissures.2,18
Treatment
The treatment of functional constipation requires parental education, behavior interventions, measures to ensure that bowel movements occur at normal intervals with good evacuation, close follow-up, and adjustment of medication and evaluation as necessary. Algorithms for the evaluation and management of constipation in infants and older children are presented in Figures 1 and 2.2,10,19
Figure 1. Constipation in Infants Younger than Six Months
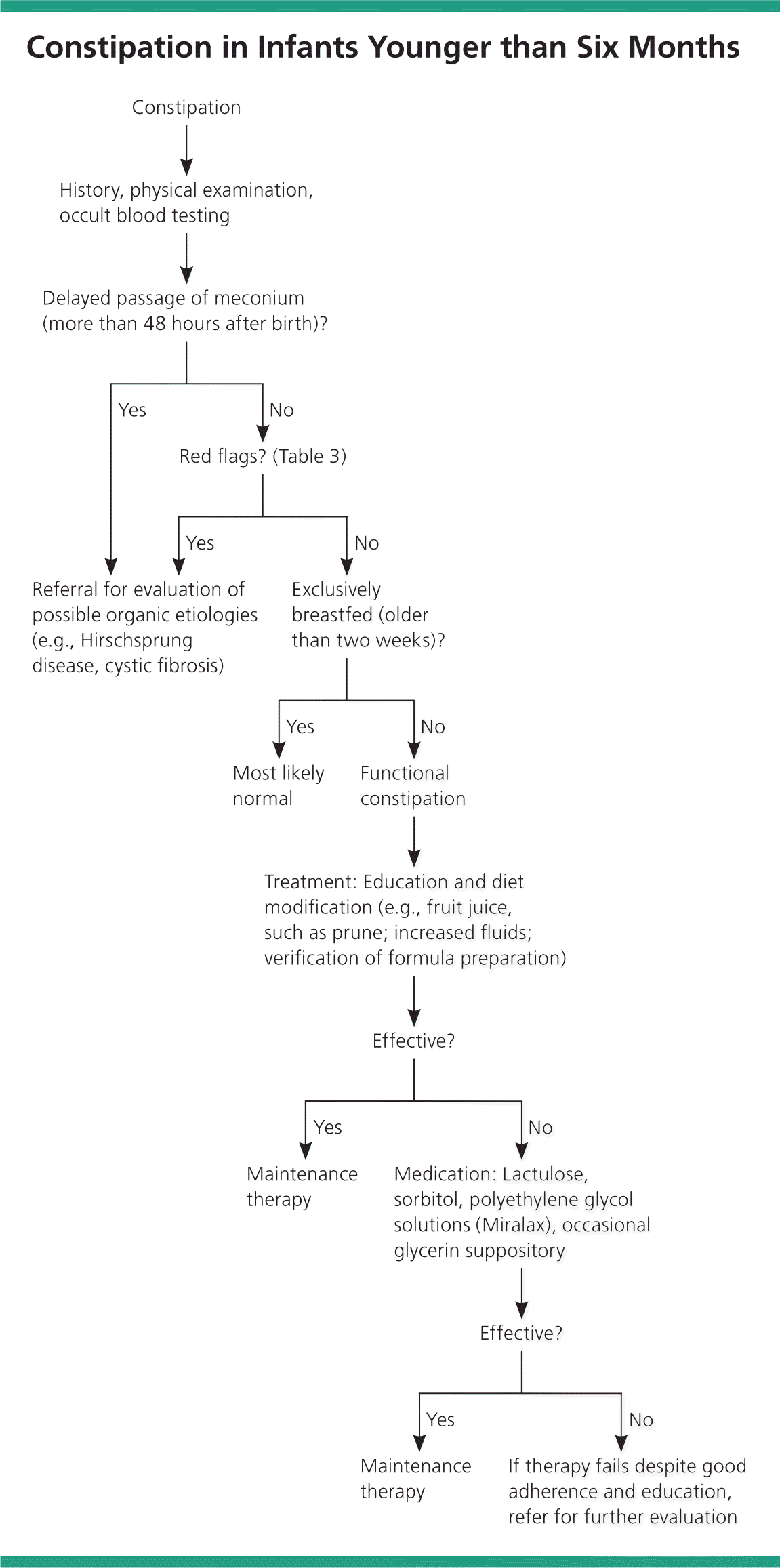
Algorithm for evaluation and management of constipation in infants younger than six months.
Information from references 2, 10, and 19.
Figure 2. Constipation in Children Six Months and Older
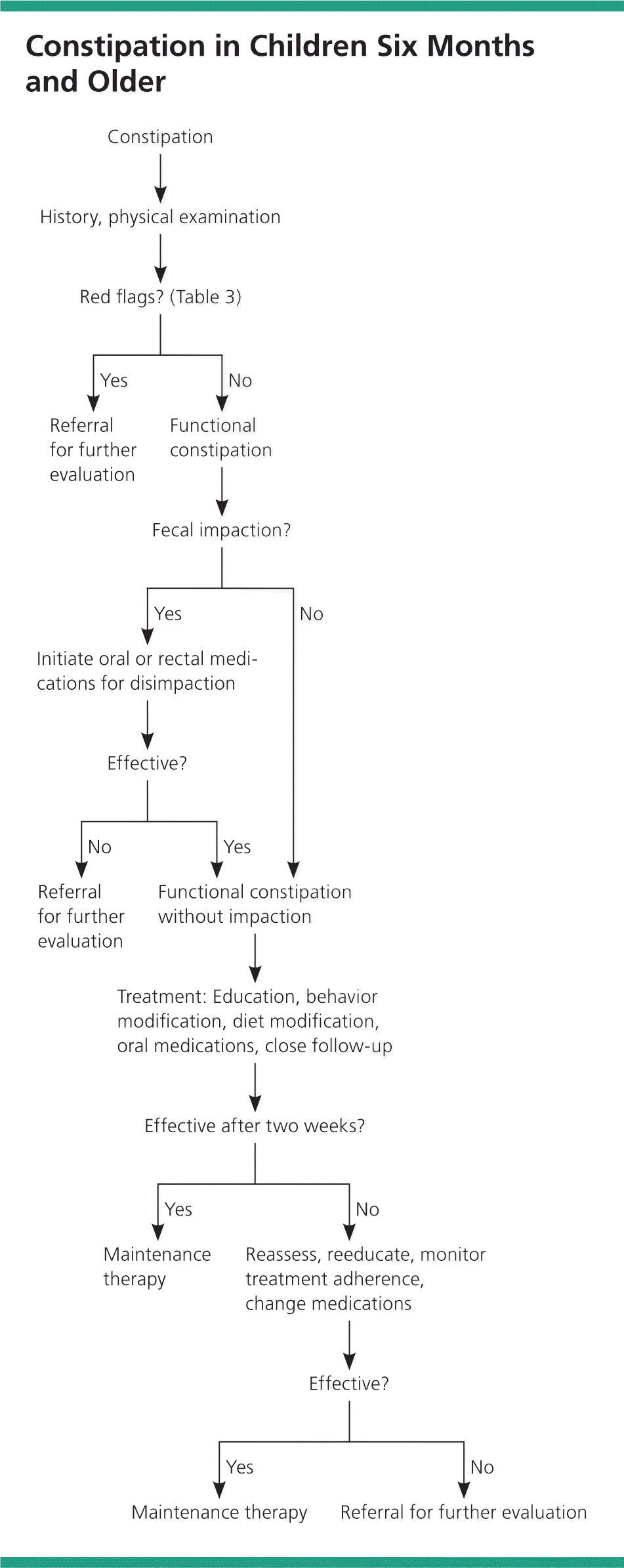
Algorithm for evaluation and management of constipation in children six months and older.
Information from references 2, 10, and 19.
EDUCATION AND BEHAVIOR MODIFICATION
Education is the first step in treatment. Educational materials for parents on constipation and fecal soiling are available at http://www.gikids.org. It is important to explain that fecal incontinence occurs from involuntary overflow of stool and not from voluntary defiance. Behavior modification with regular toileting (for five to 10 minutes) after meals combined with a reward system is often helpful. Parents should be encouraged to maintain a positive and supportive attitude throughout treatment and expect gradual improvement with occasional relapses.
Although behavior modification and education are important, intensive behavior therapy does not seem to add to treatment success, except in rare cases in which the patient has underlying behavior problems.20 Biofeedback has not been shown to be effective in children with functional constipation.2,21
DIETARY CHANGES
Dietary changes are often advised in children with constipation.21 An increased intake of fluids and absorbable and nonabsorbable carbohydrates (e.g., sorbitol in prune, pear, and apple juice) can help soften stools, particularly in infants. The recommended dosage of prune juice for infants is 2 oz per day. It can be diluted with 2 oz of water for palatability. Studies have shown that children with constipation have a lower fiber intake than other children. An increased intake of dietary fiber may improve the likelihood that a child will be able to discontinue laxative therapies.22 The addition of a probiotic (e.g., Lactobacillus GG) may be helpful in some children with functional constipation, although the studies are preliminary.23
DISIMPACTION
When fecal impaction is present, disimpaction with oral or rectal medication is required before initiation of maintenance therapy. Oral medications are less invasive but require more patient cooperation and may be slower to relieve symptoms. A number of therapies are available (Table 5).2,24–26 The advent of polyethylene glycol–based solutions (Miralax) has changed the initial approach to constipation in children because they are effective, easy to administer, noninvasive, and well tolerated.27 Rectal therapies and polyethylene glycol are similarly effective in the treatment of fecal impaction in children.28 Although some evidence supports polyethylene glycol as first-line treatment, the overall data do not clearly demonstrate superiority of one laxative.29
Table 5. Therapies for Disimpaction in Children

| Therapy | Dosage | |
|---|---|---|
| Oral | ||
| Osmotics | ||
| Polyethylene glycol 3350 (Miralax)* | 1.5 g per kg per day | |
| Polyethylene glycol solution (Golytely)* | 25 mL per kg per hour via nasogastric lavage | |
| Magnesium citrate | < 6 years: 2 to 4 mL per kg per day | |
| 6 to 12 years of age: 100 to 150 mL per day | ||
| > 12 years: 150 to 300 mL per day | ||
| Stimulants | ||
| Senna (Senokot) | 2 to 6 years of age: 2.5 to 7.5 mL (8.8 mg per 5 mL); ½ to 1 ½ tablets (8.6 mg per tablet) per day | |
| 6 to 12 years of age: 5 to 15 mL; 1 to 2 tablets per day | ||
| Bisacodyl (Dulcolax) | ≥ 2 years: 5 to 15 mg (1 to 3 tablets) per day in a single dose | |
| Lubricants | ||
| Mineral oil | 15 to 30 mL per year of age per day | |
| Rectal agents | ||
| Enemas (one per day) | ||
| Saline | 5 to 10 mL per kg | |
| Mineral oil | 15 to 30 mL per year of age up to 240 mL | |
| Phosphate soda | 2 to 12 years of age: 66-mL enema (should not to be used in children < 2 years because of the risk of electrolyte abnormality) | |
| > 12 years: 133 mL | ||
| Suppository (one per day) | ||
| Bisacodyl | ≥ 2 years: 5 to 10 mg (½ to 1 suppository) | |
| Glycerin* | ½ to 1 infant suppository; adult suppository for those older than 6 years | |
| Other | ||
| Manual (used rarely; general anesthesia needed) | — | |
*—May be used in infants < 1 year.
MAINTENANCE THERAPY
The goal of maintenance therapy is to avoid reaccumulation of stool by maintaining soft bowel movements, preferably occurring once a day. Given a robust placebo response, there is insufficient evidence to support the effectiveness of laxative therapies over placebo in the treatment of childhood constipation.30 However, most studies show that the addition of laxatives is usually necessary and more effective than behavior modification alone.31 Although the use of enemas has been advocated in the past, recent studies have shown that the addition of enemas to oral laxative regimens does not improve outcomes in children with severe constipation.32
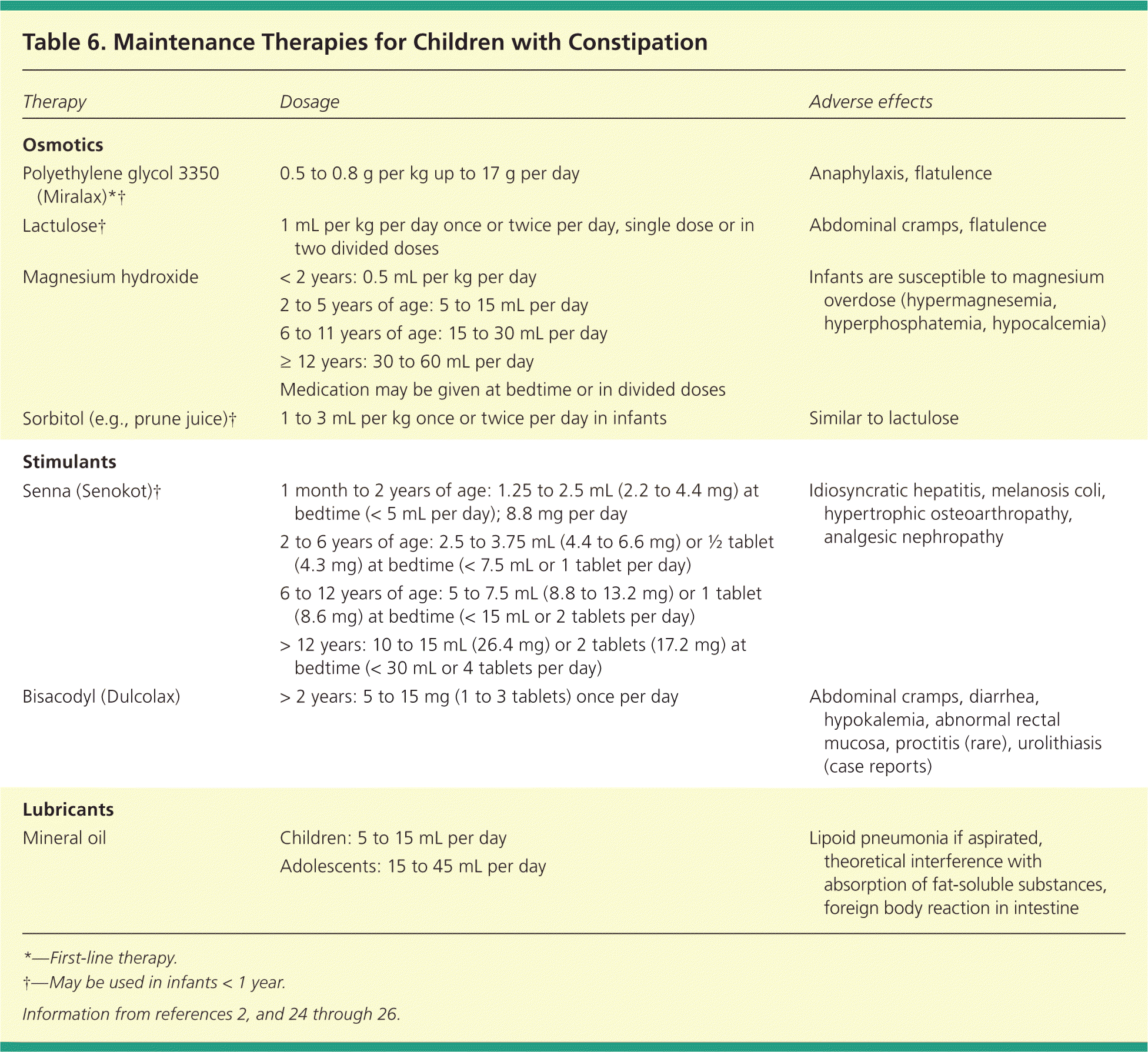
Table 6 summarizes maintenance therapies.2,24–26 Overall, polyethylene glycol achieves equal or better treatment success than other laxatives, such as lactulose or milk of magnesia,30,33,34 although it may be associated with more episodes of fecal incontinence.27 The dose of polyethylene glycol can be adjusted according to treatment response. Maintenance doses of medications need to be continued for several weeks to months after a regular bowel habit is established. Children who are toilet training should remain on laxatives until toilet training is well established.
Table 6. Maintenance Therapies for Children with Constipation
| Therapy | Dosage | Adverse effects |
|---|---|---|
| Osmotics | ||
| Polyethylene glycol 3350 (Miralax)*† | 0.5 to 0.8 g per kg up to 17 g per day | Anaphylaxis, flatulence |
| Lactulose† | 1 mL per kg per day once or twice per day, single dose or in two divided doses | Abdominal cramps, flatulence |
| Magnesium hydroxide | < 2 years: 0.5 mL per kg per day | Infants are susceptible to magnesium overdose (hypermagnesemia, hyperphosphatemia, hypocalcemia) |
| 2 to 5 years of age: 5 to 15 mL per day | ||
| 6 to 11 years of age: 15 to 30 mL per day | ||
| ≥ 12 years: 30 to 60 mL per day | ||
| Medication may be given at bedtime or in divided doses | ||
| Sorbitol (e.g., prune juice)† | 1 to 3 mL per kg once or twice per day in infants | Similar to lactulose |
| Stimulants | ||
| Senna (Senokot)† | 1 month to 2 years of age: 1.25 to 2.5 mL (2.2 to 4.4 mg) at bedtime (< 5 mL per day); 8.8 mg per day | Idiosyncratic hepatitis, melanosis coli, hypertrophic osteoarthropathy, analgesic nephropathy |
| 2 to 6 years of age: 2.5 to 3.75 mL (4.4 to 6.6 mg) or ½ tablet (4.3 mg) at bedtime (< 7.5 mL or 1 tablet per day) | ||
| 6 to 12 years of age: 5 to 7.5 mL (8.8 to 13.2 mg) or 1 tablet (8.6 mg) at bedtime (< 15 mL or 2 tablets per day) | ||
| > 12 years: 10 to 15 mL (26.4 mg) or 2 tablets (17.2 mg) at bedtime (< 30 mL or 4 tablets per day) | ||
| Bisacodyl (Dulcolax) | > 2 years: 5 to 15 mg (1 to 3 tablets) once per day | Abdominal cramps, diarrhea, hypokalemia, abnormal rectal mucosa, proctitis (rare), urolithiasis (case reports) |
| Lubricants | ||
| Mineral oil | Children: 5 to 15 mL per day | Lipoid pneumonia if aspirated, theoretical interference with absorption of fat-soluble substances, foreign body reaction in intestine |
| Adolescents: 15 to 45 mL per day |
*—First-line therapy.
†—May be used in infants < 1 year.
Stimulant laxatives (e.g., bisacodyl [Dulcolax], sennosides) may be required in some children, although data on their use in children are limited. The lack of liquid formulations limits the practical use of stimulant laxatives in younger children. In the primary care setting, stimulant laxatives should be reserved for rescue therapy when an osmotic laxative is ineffective. Patients requiring constant administration of stimulant laxatives should be evaluated further.
Long-Term Prognosis
Most children with functional constipation require prolonged treatment and have frequent relapses.19 Studies have shown that only 60% of children with constipation achieve treatment success after one year of therapy. Children with fecal incontinence or who are younger than four years at onset of constipation are particularly at risk of poor long-term outcomes.35
Referral
Referral to a pediatric gastroenterologist may be needed when a child with constipation has red flags for organic disease or the constipation is unresponsive to adequate therapy. Subspecialists may pursue newer medical therapies, such as lubiprostone (Amitiza), which acts on chloride channels in the intestine,36 or onabotulinumtoxinA (Botox) injected into a nonrelaxing sphincter.37 Surgical therapies, such as antegrade colonic enemas, have also been shown to improve continence in children with intractable constipation.38 Motility testing often helps guide management in children with intractable constipation.19,39 Although most children have functional constipation, it is important to reevaluate those who do not follow the expected course.
Data Sources: A PubMed search was completed using the keywords constipation, child, pediatric, functional constipation, and incontinence. Also searched were the Cochrane database, Essential Evidence Plus, and guidelines from the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition and the National Institute for Health and Care Excellence. Search dates: February 24, 2012, and October 2013.

