Dog bites account for 1% of all injury-related emergency department visits in the United States and more than $50 million in inpatient costs per year. [ corrected] Most animal bites are from a dog, usually one known to the victim. Most dog bite victims are children. Bite wounds should be cleaned, copiously irrigated with normal saline using a 20-mL or larger syringe or a 20-gauge catheter attached to the syringe. The wound should be explored for tendon or bone involvement and possible foreign bodies. Wounds may be closed if cosmetically favorable, such as wounds on the face or gaping wounds. Antibiotic prophylaxis should be considered, especially if there is a high risk of infection, such as with cat bites, with puncture wounds, with wounds to the hand, and in persons who are immunosuppressed. Amoxicillin/clavulanate is the first-line prophylactic antibiotic. The need for rabies prophylaxis should be addressed with any animal bite because even domestic animals are often unvaccinated. Postexposure rabies prophylaxis consists of immune globulin at presentation and vaccination on days 0, 3, 7, and 14. Counseling patients and families about animal safety may help decrease animal bites. In most states, physicians are required by law to report animal bites.
Dog bites account for 1% of injury-related emergency department visits in the United States and an estimated $53.9 million in inpatient costs per year.1 Of the approximately 4.5 million persons who are bitten by dogs each year, approximately 316,000 are treated in the emergency department, and 9,500 are hospitalized.1 [ corrected] There are 10 to 20 animal bite–related deaths, mostly from dogs, annually.1–4
Dog bites account for 85% to 90% of animal bites in the United States at a rate of 103 to 118 per 100,000 population1,5; no one dog breed is most often responsible.6 Pit bull and Rottweiler breeds account for most of the human fatalities related to dog bites over the past two decades.6,7 Most dog bite victims are children, and these bites usually involve the head and neck. Adolescents and adults tend to have more bite wounds to the extremities.2,3,7 More than 70% of bites are from a dog that is known to the victim, and about 50% are self-reported as unprovoked.2
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
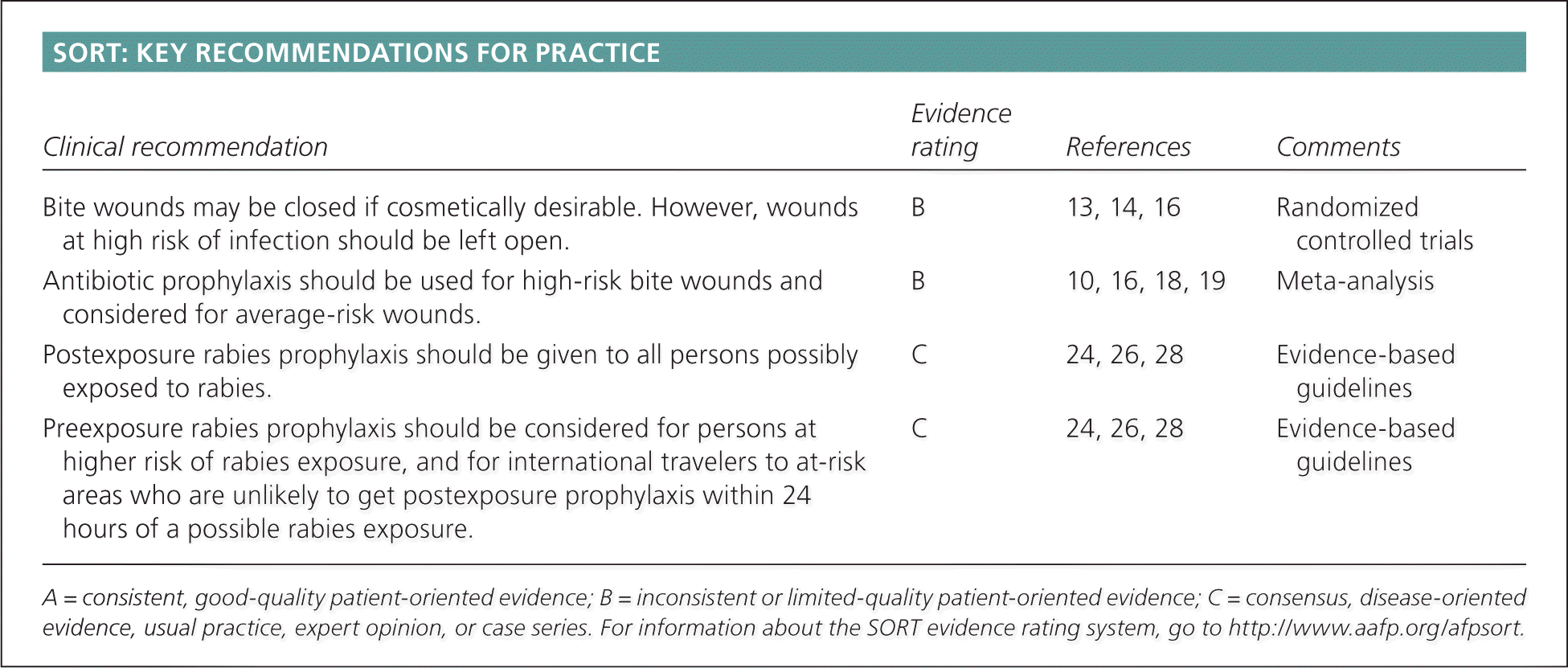
| Bite wounds may be closed if cosmetically desirable. However, wounds at high risk of infection should be left open. | B | 13, 14, 16 | Randomized controlled trials |
| Antibiotic prophylaxis should be used for high-risk bite wounds and considered for average-risk wounds. | B | 10, 16, 18, 19 | Meta-analysis |
| Postexposure rabies prophylaxis should be given to all persons possibly exposed to rabies. | C | 24, 26, 28 | Evidence-based guidelines |
| Preexposure rabies prophylaxis should be considered for persons at higher risk of rabies exposure, and for international travelers to at-risk areas who are unlikely to get postexposure prophylaxis within 24 hours of a possible rabies exposure. | C | 24, 26, 28 | Evidence-based guidelines |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Cat bites account for 5% to 10% of animal bite wounds.1 Cat bites occur most often in adult women, usually on the extremities. Almost all of these bites are self-reported as provoked.2
Wound Treatment
Animal bite wounds are considered grossly contaminated; therefore, proper wound treatment is essential to prevent secondary infection. The affected skin surface should be cleansed, and the wound should be copiously irrigated with water, normal saline, or dilute povidone-iodine solution, especially if the animal may be rabid.8–10 To irrigate the wound, a 20-mL or larger syringe should be used to generate the high pressure required for adequate cleaning.10 If a 20-mL or larger syringe is unavailable, a 20-gauge catheter can be connected to the syringe to increase the pressure.9–11 Cautious debridement of devitalized tissue further decreases the potential for infection.9,10,12
The wound should be carefully explored for tendon or bone involvement and foreign bodies, such as teeth fragments.9,10 Older dogs and cats often have significant periodontal disease, increasing the risk that a tooth will break off during a bite. Radiography is indicated if a foreign body or bone involvement is suspected.9 Tendon ruptures should be evident on examination, but identifying a partial tendon rupture requires careful exploration of the wound. Observing the tendon throughout the joint's full extension and full flexion can reveal small or partially torn tendons, which warrant referral for repair.
Wound Closure
There are few studies addressing whether an animal bite wound should be primarily closed. Traditionally, animal bite wounds were left open to prevent secondary infections. In one study of 169 dog bite wounds in 96 patients, the infection rate was statistically equivalent for wounds that were primarily closed (7.6%) and those that were left to heal by secondary intention (7.8%).13 In a second study of 145 bite wounds that were primarily closed, only 5.5% became infected, including bites from dogs (61%), cats (31%), and humans (8%).14 Both of these studies are small and have design limitations; therefore, wounds may be primarily closed if desired for cosmetic reasons.9,10,13–15 However, allowing a wound to close by secondary intention should be considered if there is a higher risk of infection (Table 110,11,16 ), such as wounds to the hand.9,10 The safety and effectiveness of skin adhesives have not been studied in animal bite wounds.17
Table 1. Factors That Increase the Risk of Infection from an Animal Bite

| Bite in extremities with underlying venous and/or lymphatic compromise | |
| Bite involving the hand | |
| Bite near or in a prosthetic joint | |
| Cat bites | |
| Crush injuries | |
| Delayed presentation | |
| Greater than 6 to 12 hours for bites to the arm or leg | |
| Greater than 12 to 24 hours for bites to the face | |
| Puncture wounds | |
| Victim with diabetes mellitus or immunosuppression | |
Antibiotic Prophylaxis
There are conflicting data regarding antibiotic prophylaxis in the treatment of dog bite wounds and very limited data in other animal bite wounds. A meta-analysis of eight randomized trials showed a benefit with antibiotic prophylaxis in animal bites (relative risk = 0.56; number needed to treat = 14); the infection rate was 16% in untreated patients.18 However, a Cochrane review of nine trials showed no statistical difference in infection rate between prophylaxis and no treatment, except in bite wounds to the hand.19 In hand wounds, antibiotic prophylaxis reduced the rate of infection from 28% to 2% (odds ratio = 0.10; number needed to treat = 4). However, studies were heterogeneous and used different antibiotics. Antibiotic prophylaxis should be used for high-risk bite wounds (Table 110,11,16 ) and considered in average-risk wounds.9,18,19
Cultures of bite wounds are generally not helpful initially, unless the wound is abscessed or already infected.9,10 Common pathogens associated with animal bites include Staphylococcus, Streptococcus, Pasteurella, Capnocytophaga, Moraxella, Corynebacterium, Neisseria, and anaerobic bacteria.20 Pasteurella multocida is a common bacterium in the mouths of cats, but it can also be present in dogs. This bacterium can cause a fast-growing infection in humans and is one of the reasons to consider antibiotic prophylaxis for bite wounds. Wounds that become infected within 24 hours of the bite are often caused by Pasteurella.10–12 Capnocytophaga canimorsus is an emerging human pathogen that has been isolated from the mouths of 24% of dogs and 17% of cats.10,12,21 This fastidious gram-negative bacterium can cause septicemia, meningitis, and endocarditis. Patients who have had splenectomy or who abuse alcohol are at highest risk of C. canimorsus infection. A beta-lactam/beta-lactamase inhibitor combination is the initial treatment of choice for this bacterium.
Antibiotic prophylaxis should be considered for all bites requiring closure and for high-risk bites.9,10 All cat bites are considered high risk for infection because they tend to cause deep puncture wounds.9,10
Amoxicillin/clavulanate (Augmentin) is generally considered the first-line prophylactic treatment for animal bites.10,16 Table 2 summarizes the treatment options.10,16,22 A three-day to seven-day course of prophylactic antibiotics is likely adequate and was typical in most studies.9
Table 2. Prophylactic Antibiotic Dosages for Animal Bites

| Adults | |
| First-line | |
| Amoxicillin/clavulanate (Augmentin), 875/125 mg every 12 hours | |
| Alternatives | |
| Clindamycin, 300 mg 3 times per day plus ciprofloxacin (Cipro), 500 mg twice per day | |
| Doxycycline, 100 mg twice per day | |
| Penicillin VK, 500 mg 4 times per day plus dicloxacillin, 500 mg 4 times per day | |
| A fluoroquinolone; trimethoprim/sulfamethoxazole, 160/800 mg twice per day; or cefuroxime axetil (Ceftin), 500 mg twice per day plus metronidazole (Flagyl), 250 to 500 mg 4 times per day, or clindamycin, 300 mg 3 times per day | |
| Children | |
| First-line | |
| Amoxicillin/clavulanate, 25 to 45 mg per kg divided every 12 hours | |
| Alternative | |
| Clindamycin, 10 to 25 mg per kg divided every 6 to 8 hours plus trimethoprim/sulfamethoxazole, 8 to 10 mg per kg (trimethoprim component) divided every 12 hours | |
| Pregnant women who are allergic to penicillin | |
| Azithromycin (Zithromax), 250 to 500 mg per day | |
| Close monitoring is needed because of high failure rate | |
Tetanus vaccination is recommended after an animal bite if it has been more than five years since the patient has been immunized.11 Table 3 summarizes the indications for tetanus prophylaxis in patients with wounds.23
Table 3. Indications for Tetanus Prophylaxis

| History of tetanus immunization | Clean, minor wounds | All other wounds | ||
|---|---|---|---|---|
| Vaccine | Immune globulin | Vaccine | Immune globulin | |
| Uncertain or < 3 doses | Yes | No | Yes | Yes |
| ≥ 3 doses | No, unless > 10 years since last dose | No | No, unless > 5 years since last dose | No |
Adapted from Kretsinger K, Broder KR, Cortese MM, et al.; Centers for Disease Control and Prevention. Preventing tetanus, diphtheria, and pertussis among adults: use of tetanus toxoid, reduced diphtheria toxoid and acellular pertussis vaccine recommendations of the Advisory Committee on Immunization Practices (ACIP) and recommendation of ACIP, supported by the Healthcare Infection Control Practices Advisory Committee (HICPAC), for use of Tdap among health-care personnel. MMWR Recomm Rep . 2006;55(RR-17):25.
Rabies
Rabies is a virus that can infect any mammal. In the past decade, there have been up to eight human cases in the United States each year.24 Once symptomatic, it is almost universally fatal. Postexposure prophylaxis, which costs about $1,000, is 100% effective if used properly.24 There have been 6,000 to 7,000 documented cases per year of rabies in animals in the United States and Puerto Rico over the past 10 years.25 In the United States, cats are the most commonly infected domesticated animal, whereas raccoons, bats, and skunks are the most commonly infected wild animals. In 2012, there were 257 cases of rabies in cats and 84 cases in dogs.25 In most areas of the United States, it is required by law that dogs and cats be vaccinated. Despite this, data show that only 45% of dogs and 8% of cats that cause bites requiring an emergency department visit are vaccinated for rabies.2
Postexposure prophylaxis is indicated in all persons who were possibly exposed to a rabid animal and is given to about 16,000 to 39,000 persons in the United States each year.26 Prophylaxis consists of immune globulin at presentation and rabies vaccination on days 0, 3, 7, and 14. The immune globulin is infiltrated around the bite wound, and any additional volume is administered at a site distant to the vaccination site, usually the opposite arm as the rabies vaccine. In the past, a fifth dose of the vaccine was given on day 28; however, in 2009, the Advisory Committee on Immunization Practices recommended dropping this step.24,27 If the patient had already received preexposure prophylaxis before the animal bite, no immune globulin is needed, and the rabies vaccine is administered only on days 0 and 3.24
Postexposure prophylaxis is generally not needed in patients with a dog or cat bite as long as the animal is not showing signs of rabies, such as inappetence, dysphagia, abnormal behavior, ataxia, paralysis, altered vocalization, or seizures; however, the animal should be monitored for at least 10 days.8,24,26,27 If the animal shows signs of rabies, becomes sick, or dies, immediate postexposure prophylaxis is recommended. No animal should be euthanized within 10 days of biting someone so that it can be properly observed. If there is a question about whether postexposure prophylaxis should be given, physicians can contact their local health department or go to http://www.cdc.gov/rabies/resources/contacts.html for a list of state and local rabies consultation contacts.
Preexposure prophylaxis should be considered in persons with higher risk of rabies exposure, such as certain laboratory workers, veterinarians, spelunkers, and certain international travelers. The Centers for Disease Control and Prevention recommends that travelers to at-risk areas receive preexposure prophylaxis if they are unlikely to receive treatment within 24 hours of a possible exposure. Preexposure prophylaxis consists of three vaccines given on days 0, 7, and 21 to 28.26,28
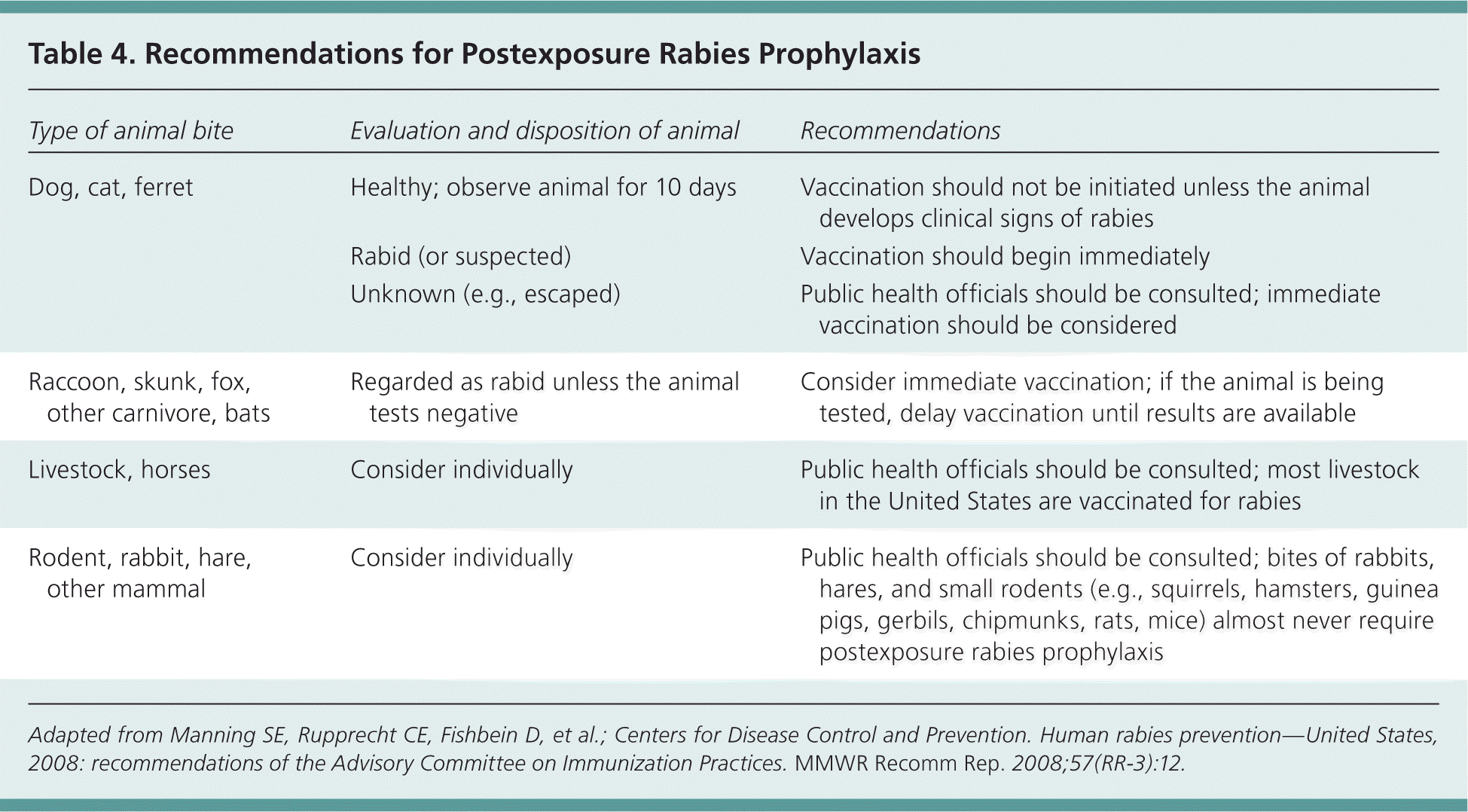
Saliva, brain tissue, and nervous system tissue are considered infective. Blood, urine, and feces are not infective, and contact does not warrant postexposure prophylaxis. Table 4 includes postexposure rabies prophylaxis recommendations for specific animal bites.26 Postexposure prophylaxis should be strongly considered in persons possibly exposed to a bat, such as if awakening from sleep and finding a bat in the room or finding a bat in the room with an unattended child.
Table 4. Recommendations for Postexposure Rabies Prophylaxis
| Type of animal bite | Evaluation and disposition of animal | Recommendations |
|---|---|---|
| Dog, cat, ferret | Healthy; observe animal for 10 days | Vaccination should not be initiated unless the animal develops clinical signs of rabies |
| Rabid (or suspected) | Vaccination should begin immediately | |
| Unknown (e.g., escaped) | Public health officials should be consulted; immediate vaccination should be considered | |
| Raccoon, skunk, fox, other carnivore, bats | Regarded as rabid unless the animal tests negative | Consider immediate vaccination; if the animal is being tested, delay vaccination until results are available |
| Livestock, horses | Consider individually | Public health officials should be consulted; most livestock in the United States are vaccinated for rabies |
| Rodent, rabbit, hare, other mammal | Consider individually | Public health officials should be consulted; bites of rabbits, hares, and small rodents (e.g., squirrels, hamsters, guinea pigs, gerbils, chipmunks, rats, mice) almost never require postexposure rabies prophylaxis |
Adapted from Manning SE, Rupprecht CE, Fishbein D, et al.; Centers for Disease Control and Prevention. Human rabies prevention—United States, 2008: recommendations of the Advisory Committee on Immunization Practices. MMWR Recomm Rep . 2008;57(RR-3):12.
Preventing Animal Bites
Studies have shown that although most primary care physicians agree that counseling patients about pet-related health hazards is important, less than 20% counsel their own patients and family members.29 There are a few studies that demonstrate a benefit of counseling children and families about preventing dog bites.30 Most dogs that bite are known to the victim.2–4,6,7 Dogs should be socialized to children from the time they are puppies. Training makes a dog more confident and less likely to bite out of fear. Pets should have regular veterinary visits to stay updated on vaccines and to improve health. Pets that are in pain or sick are more likely to bite. Neutering dogs has been shown to decrease bites. Young children should never be left alone with pets.31 A brochure on dog bite prevention from the American Veterinary Medical Association is available at https://www.avma.org/public/Pages/Dog-Bite-Prevention.aspx.
Laws and Regulations
Most areas in the United States require health care professionals to report dog bites and many other animal bites, including bites in patients who present to an ambulatory office. Physicians should be familiar with their state and local laws. Because rabies in animals is a national reportable disease, suspected animals should be sent for testing. Local or state health departments can provide information about submitting and storing specimens.
Data Sources: We searched the Cochrane database using the key words animal bite, bite wound, and rabies; the U.S. Preventive Services Task Force and Institute for Clinical Systems Improvement using the key words animal bite, rabies, and bite wound; the Centers for Disease Control and Prevention using the key words animal bite and rabies; and the Agency for Healthcare Research and Quality, National Guideline Clearinghouse, Essential Evidence Plus, and UpToDate using the key word animal bite. Medline was searched when the other sources did not yield answers to our questions. We also searched the Journal of the American Veterinary Medical Association. Search dates: June 2011, January 2012, June 2013, and June 2014.

