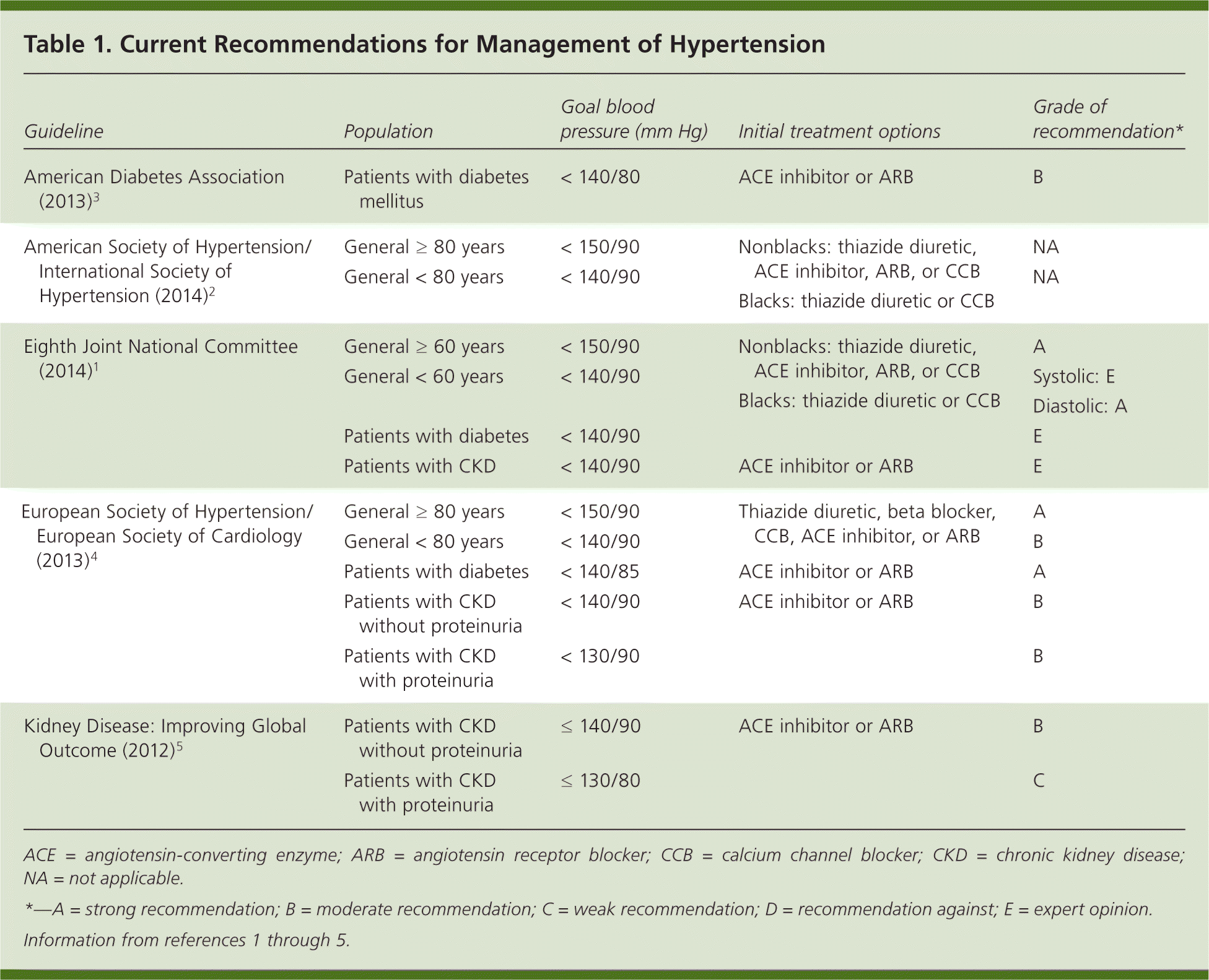
Evidence-based guidelines are indispensable and assist clinicians in providing the most effective care for patients. The Eighth Joint National Committee (JNC 8) recently issued the most anticipated guideline in some time.1 The JNC 8 committee was initially appointed in 2008 by the National Heart, Lung, and Blood Institute. When the National Institutes of Health discontinued sponsorship of clinical recommendations, JNC 8 panel members published their guideline on the management of hypertension in the Journal of the American Medical Association the same week the American Society of Hypertension and the International Society of Hypertension released their guideline.2 The JNC 8 guideline was never endorsed by the American Heart Association or the American College of Cardiology. Current hypertension management recommendations from various organizations are listed in Table 1.1–5
Table 1. Current Recommendations for Management of Hypertension
| Guideline | Population | Goal blood pressure (mm Hg) | Initial treatment options | Grade of recommendation* |
|---|---|---|---|---|
| American Diabetes Association (2013)3 | Patients with diabetes mellitus | < 140/80 | ACE inhibitor or ARB | B |
| American Society of Hypertension/International Society of Hypertension (2014)2 | General ≥ 80 years | < 150/90 | Nonblacks: thiazide diuretic, ACE inhibitor, ARB, or CCB | NA |
| General < 80 years | < 140/90 | Blacks: thiazide diuretic or CCB | NA | |
| Eighth Joint National Committee (2014)1 | General ≥ 60 years | < 150/90 | Nonblacks: thiazide diuretic, ACE inhibitor, ARB, or CCB | A |
| General < 60 years | < 140/90 | Blacks: thiazide diuretic or CCB | Systolic: E Diastolic: A | |
| Patients with diabetes | < 140/90 | E | ||
| Patients with CKD | < 140/90 | ACE inhibitor or ARB | E | |
| European Society of Hypertension/ European Society of Cardiology (2013)4 | General ≥ 80 years | < 150/90 | Thiazide diuretic, beta blocker, CCB, ACE inhibitor, or ARB | A |
| General < 80 years | < 140/90 | B | ||
| Patients with diabetes | < 140/85 | ACE inhibitor or ARB | A | |
| Patients with CKD without proteinuria | < 140/90 | ACE inhibitor or ARB | B | |
| Patients with CKD with proteinuria | < 130/90 | B | ||
| Kidney Disease: Improving Global Outcome (2012)5 | Patients with CKD without proteinuria | ≤ 140/90 | ACE inhibitor or ARB | B |
| Patients with CKD with proteinuria | ≤ 130/80 | C |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker; CCB = calcium channel blocker; CKD = chronic kidney disease; NA = not applicable.
*—A = strong recommendation; B = moderate recommendation; C = weak recommendation; D = recommendation against; E = expert opinion.
Management of hypertension is key for improving health outcomes. However, the new recommendations may frustrate clinicians who want detailed guidance. Hypertension is the most significant cardiac risk factor in older adults.1 Data show that lowering blood pressure by 10 mm Hg in patients with hypertension reduces cardiovascular and stroke mortality by 25% and 40%, respectively.6 The most significant change in the JNC 8 guideline is relaxation of the systolic and diastolic blood pressure goals for adults 60 years and older. This finding was based primarily on six randomized controlled trials (RCTs) comparing intensive vs. conservative blood pressure goals among older patients.7–12
Panel members concluded that the absence of evidence supporting a lower target was grounds to raise blood pressure goals. Although each of the RCTs is scientifically valid, when combined, do they adequately support the current recommendations? Three studies clearly showed reductions in mortality and cardiovascular events when systolic blood pressure was less than 143 mm Hg vs. greater than 150 mm Hg.9,11,12 Three other studies involved extremely healthy participants and were not consistent with the health of the typical U.S. adult of similar age.7,8,11 The weighted mean age of all participants in the six RCTs was 74 years, yet JNC 8 distinguishes 60 years as the transition age for relaxation of blood pressure goals. In three of the six studies, inclusion criteria included age older than 65, 70, or 80 years.7–9 The argument could be made that increasing the transition age to at least 70 years would better reflect the study population. Although the relationship between blood pressure and cardiovascular events seems equivocal with advancing age, younger patients (60 to 70 years) may still benefit from greater reduction of blood pressure. There are no credible RCTs for this age group that compare lower blood pressures (140/90 mm Hg or lower) with JNC 8 recommendations in terms of improved cardiovascular, cerebrovascular, or renal outcomes.1
JNC 8 also represents a paradigm shift in the pharmacologic management of hypertension. Thiazide diuretics had previously been recommended as monotherapy for patients with stage 1 hypertension or in combination with other agents for patients with stage 2 hypertension. Now, thiazides, angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, and calcium channel blockers are indicated for monotherapy. These agents are preferred over beta blockers for initial management because of insufficient evidence that beta blockers provide clinically significant benefits for cardiovascular and cerebrovascular outcomes. The availability of four first-line agents may seem more challenging, but it allows clinicians to incorporate their preferences—and those of their patients—into the accepted practice recommendations. Thiazides and calcium channel blockers are preferred for black patients because of improved cardiovascular and cerebrovascular outcomes, and more effective blood pressure reduction in this population.1 Improved renal outcomes make angiotensin-converting enzyme inhibitors and angiotensin receptor blockers compelling choices for patients with diabetes mellitus or chronic kidney disease.1
As a result of the new guidelines, fewer older adults now meet the diagnostic criteria for hypertension. Rates of hypertension in younger adults (18 to 59 years) are similar under JNC 7 and JNC 8 criteria (20.3% and 19.2%, respectively); however, rates for older adults changed from 68.9% to 61.2%.13 More than 25% of older adults who were receiving antihypertensive therapy under the more stringent JNC 7 targets will be reclassified as at goal under JNC 8, suggesting that millions of Americans are eligible for reduction or elimination of antihypertensive therapy.13,14 However, the panel recommended that therapy not be adjusted for these patients, which creates two distinct standards within the same age group. Do we know which group is receiving better care? Are we fostering a healthier population or merely tolerating higher blood pressure values?
As in JNC 7, physicians have been challenged to stay within the performance measures of blood pressure goals. With more relaxed blood pressure targets for older adults, it is conceivable that clinicians may become less vigilant and be satisfied with near-goal values. Will these slightly higher blood pressure targets improve care for patients or result in higher rates of cardiovascular and cerebrovascular events?
Patients who met the JNC 7 requirements for hypertension should be maintained on their current regimen. For others, achieving a systolic blood pressure closer to 140 mm Hg, compared with 150 mm Hg, is reasonable given the available evidence, assuming that the adverse effects of medication are minimal. Additional well-designed RCTs are needed to address optimal blood pressure goals and the age at which more relaxed targets are acceptable.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army at large.

