A 27-year-old man presented for an occupational physical examination prior to beginning a career as a firefighter. He was healthy with no known chronic medical problems. He was taking no medications and did not smoke or drink alcohol. He exercised regularly. He had no history of cardiovascular symptoms with physical exertion. His family medical history was normal.
He had normal vital signs. On cardiac examination, he had a grade II/VI systolic ejection murmur that was softer during inspiration. The remainder of the examination was normal. He had normal fasting blood glucose and fasting lipid levels. An electrocardiogram was obtained as part of his medical screening requirements (see accompanying figure).
Figure
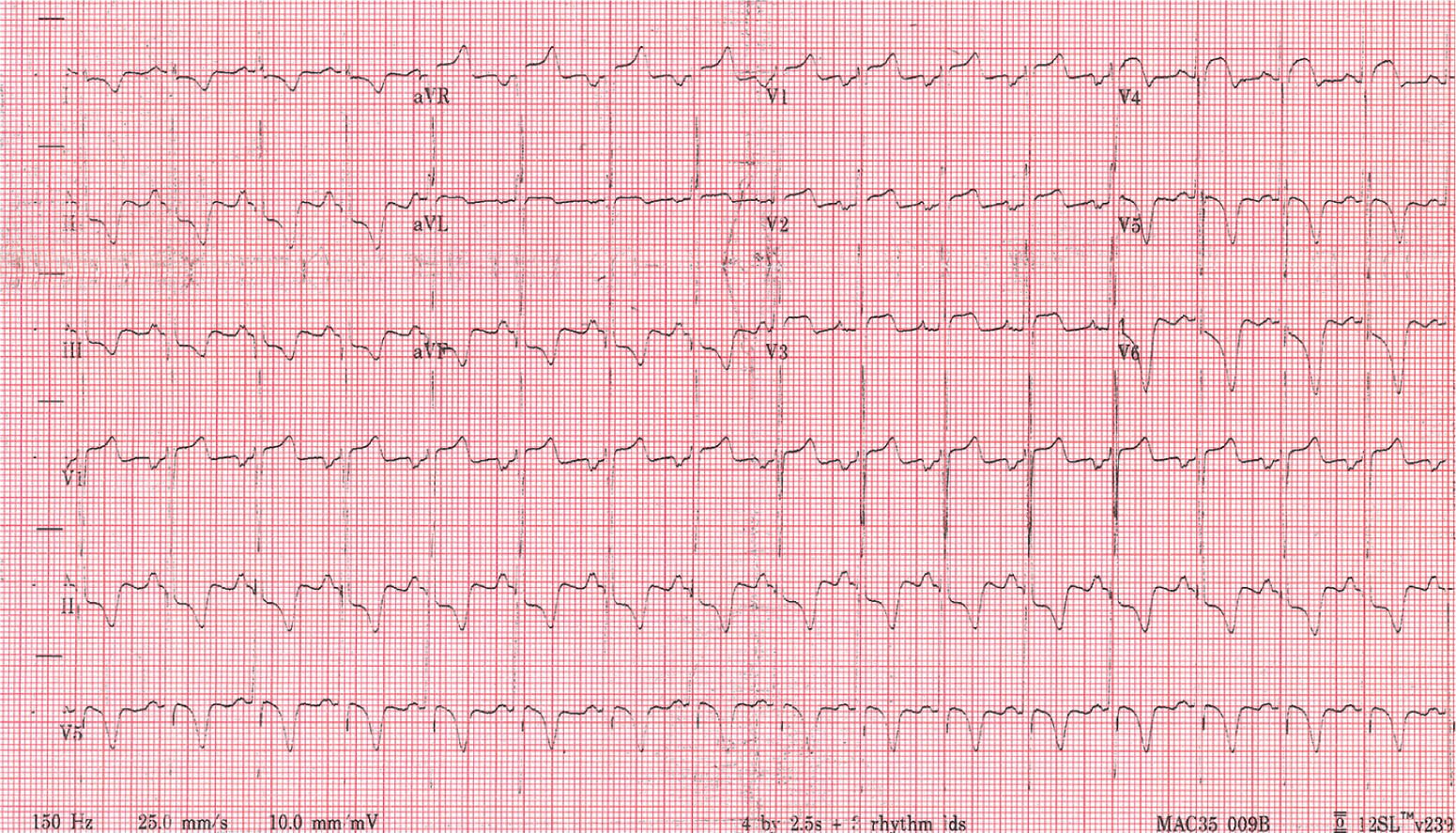
Question
Based on the patient's history, physical examination, and electrocardiogram findings, which one of the following is the most likely diagnosis?
A. Acute myocardial infarction.
B. Athletic heart.
C. Hypertensive heart disease with left ventricular hypertrophy.
D. Hypertrophic cardiomyopathy.
E. Pericarditis.
Discussion
The correct answer is D: hypertrophic cardiomyopathy. The electrocardiogram shows several classic features of hypertrophic cardiomyopathy. There is evidence of left ventricular hypertrophy by voltage criteria in the precordial leads. There are Q waves in the inferior leads (III and aVF) that suggest depolarization through a thick hypertrophied intraventricular septum. Additionally, there is evidence of biatrial abnormality. As the left ventricle thickens, the atrial contraction needed to fill stiff ventricles increases and results in atrial abnormalities. Finally, the deeply symmetric and negative T waves in the inferior leads are typically seen in the apical variant of hypertrophic cardiomyopathy.
An echocardiogram showed a 22-mm septum (upper limit of normal is approximately 11 mm) with an apical thickness of 25 mm. Given the electrocardiogram findings and thickness of the septum and apex, hypertrophic cardiomyopathy was diagnosed. The echocardiogram confirmed that the left ventricular outflow tract was not obstructed, which is consistent with the patient's lack of symptoms. An important part of treating hypertrophic cardiomyopathy is activity restriction to reduce the risk of sudden cardiac death. Risk stratification for sudden death includes six major risk factors: previous cardiac arrest, ventricular tachycardia, extreme left ventricular hypertrophy, unexplained syncope, abnormal blood pressure response, and family history of sudden death. Because of the autosomal-dominant inheritance pattern of some common forms of hypertrophic cardiomyopathy, screening of first-degree relatives is recommended.1,2
Patients presenting with acute myocardial infarction are usually older and have risk factors for coronary artery disease, such as hypertension, hyperlipidemia, and diabetes mellitus. Clinical symptoms, such as chest pain and pressure, are more common with myocardial infarction. The electrocardiogram typically shows localized ST segment elevations or depressions vs. the diffuse ST segment changes on this patient's electrocardiogram. A prior echocardiogram is helpful for comparison.
Patients with athletic heart typically have normal findings on an electrocardiogram or borderline criteria for left ventricular hypertrophy. Atrial abnormalities are rarely noted. The wall thickness is usually less than 15 mm. With deconditioning, the mild left ventricular hypertrophy typically will resolve, as demonstrated on an electrocardiogram and echocardiogram.
Patients with severe hypertensive heart disease can present asymptomatically with left ventricular hypertrophy, but these patients are typically older and have a history of long-standing hypertension. The electrocardiogram does not typically show deep symmetric T wave inversions, as in this patient.
Patients with pericarditis typically have a three-component friction rub on examination that can last throughout the cardiac cycle. The electrocardiogram shows PR segment depression and diffuse ST segment elevation.
Selected Differential Diagnosis of Left Ventricular Hypertrophy

| Condition | Cardiac examination findings | Characteristics |
|---|---|---|
| Aortic regurgitation | High-pitched diastolic murmur that is loudest at the left sternal border | Leads to chronic volume overload resulting in hypertrophy |
| Aortic stenosis | Ejection click; systolic, crescendo-decrescendo murmur that is loudest at the upper right sternal border | Aortic stenosis leads to left ventricular pressure overload |
| Hypertension | Elevated blood pressure; displaced and enlarged apical impulse | Most common cause of left ventricular hypertrophy, long-standing hypertension leads to pressure overload in the left ventricle |
| Mitral regurgitation | High-pitched, blowing, holosystolic murmur that is loudest over the apex; radiates to axilla | Leads to chronic volume overload resulting in hypertrophy |
| Ventricular septal defect | Holosystolic, harsh murmur that is loudest at the lower left sternal border | Usually leads to biventricular hypertrophy |
The views expressed are those of the authors and do not reflect the official policy of the U.S. Department of the Navy, the U.S. Department of Defense, or the U.S. government.

