
Am Fam Physician. 2015;91(1):online
Author disclosure: No relevant financial affiliations.
States currently electing not to expand Medicaid possibly forego the opportunity to expand their primary care workforces by a total of 1,525 physicians. Increased demand from expansion states and a limited primary care physician pool may provide a pull across state lines to the disadvantage of nonexpansion states.
The Affordable Care Act aims to increase health coverage for uninsured Americans, partly through expansion of Medicaid eligibility. To date, 28 states including the District of Columbia have elected to expand this federally funded program, with action pending in two additional states.1 Given that Medicaid expansion has led to increased hiring of primary care physicians (PCPs) in community health centers in expansion states, we aimed to quantify the opportunity cost of not expanding Medicaid by estimating the impact on the primary care workforce in these states.2
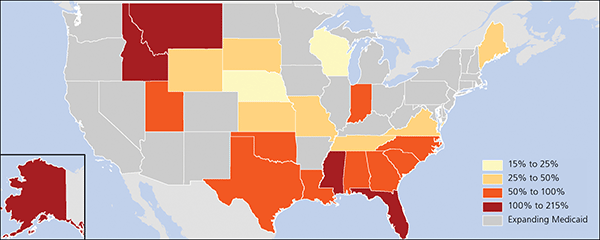
Assuming historical patterns of patient encounter per PCP are stable in each state, we estimated the increased demand for PCPs because of Medicaid expansion using a combination of data from the Kaiser Family Foundation, American Community Survey, American Medical Association Masterfile, Medical Expenditure Panel Survey, and the U.S. Census Bureau.3 If the 23 states currently electing not to expand Medicaid had chosen to expand per Affordable Care Act parameters, we estimate the need for 1,525 additional PCPs by 2030. We included states that have not approved Medicaid expansion or have pending waivers for alternative Medicaid plans as of September 2014. By our estimates, the 28 states expanding Medicaid can expect to increase their primary care workforce by 1,312 physicians. The accompanying figure shows the estimated workforce opportunity cost for each nonexpansion state, in proportion to the annual production of primary care providers.3 For example, Texas foregoes the opportunity to expand its primary care workforce by 316 PCPs through 2030. This is equivalent to 67% of its current annual production of 474 PCPs per year.
With evidence of increased hiring of PCPs in Medicaid expansion states, nonexpansion may mean more than a lost opportunity to strengthen a primary care workforce that is already strained by the challenges of caring for an aging and expanding population.4 Increased primary care demand in neighboring expansion states may attract more PCPs away from nonexpanding states. Less access to primary care may lead to worsening access to health care, less access to preventive care, and poorer overall health outcomes. The economic impact of the primary care workforce is also lost in expansion discussions, despite evidence suggesting PCPs generate up to $1.5 million in annual revenues and 23 new jobs apiece.5
