The term “cancer survivor” refers to anyone living with a diagnosis of cancer. As the U.S. population ages, cancer screening increases, and cancer treatments improve, millions more Americans will be classified as cancer survivors in the future. Although many survivors wish to continue care with their oncologists, patients benefit from care provided by a family physician. Many survivors are older and have comorbidities, which should be addressed to optimize function and longevity. Common late effects of cancer and its treatment include second primary cancers, sexual dysfunction, and psychosocial issues. Cancer recurrence is a significant concern. After treatment for colorectal cancer, intensive surveillance, including colonoscopy, imaging, and serology, confers an overall survival benefit. Breast cancer survivors should receive annual mammography. Prostate cancer survivors should undergo prostate-specific antigen testing every six to 12 months. Melanoma survivors should be counseled on sun protection, including daily sunscreen use, and recognizing characteristics of potentially malignant skin lesions. Female survivors of Hodgkin lymphoma who were treated with chest or axillary radiation between 10 and 30 years of age are at high risk of breast cancer, and should be screened with mammography and magnetic resonance imaging annually starting eight to 10 years after the diagnosis. All cancer survivors treated with chest radiation are at increased risk of cardiovascular disease, and should be screened for other cardiovascular risk factors and treated as indicated.
Before the more hopeful term “cancer survivor” was coined in the 1980s, “cancer victim” was widely employed to identify persons with cancer. Although definitions vary, cancer survivor is most often used to indicate any person who receives a diagnosis of cancer, from the initial diagnosis throughout the phases of illness, including the palliative period.1 The number of Americans living with cancer has increased dramatically, from about 5 million in the mid-1980s to more than 13 million in 2009.2 During the same period, the five-year survival rate for all types of cancer rose from about 50% to more than 65%.2 Many more persons will be classified as cancer survivors in the coming decades because of population aging, improved treatments, and increased screening. The contribution of overdiagnosis is debated, but there is evidence that some cancer survivors would not have been diagnosed without screening. For example, 19% of breast cancers may never have been diagnosed without screening mammography.3
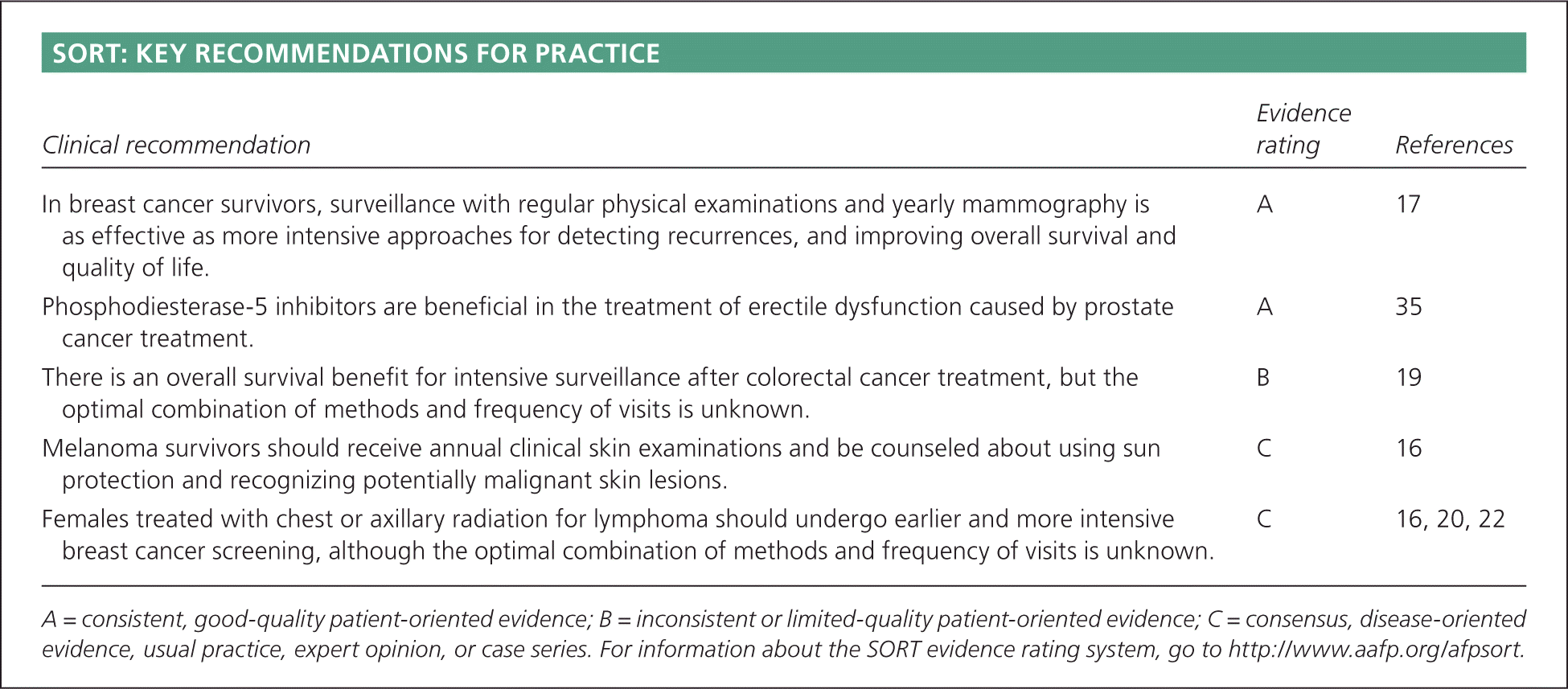
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| In breast cancer survivors, surveillance with regular physical examinations and yearly mammography is as effective as more intensive approaches for detecting recurrences, and improving overall survival and quality of life. | A | 17 |
| Phosphodiesterase-5 inhibitors are beneficial in the treatment of erectile dysfunction caused by prostate cancer treatment. | A | 35 |
| There is an overall survival benefit for intensive surveillance after colorectal cancer treatment, but the optimal combination of methods and frequency of visits is unknown. | B | 19 |
| Melanoma survivors should receive annual clinical skin examinations and be counseled about using sun protection and recognizing potentially malignant skin lesions. | C | 16 |
| Females treated with chest or axillary radiation for lymphoma should undergo earlier and more intensive breast cancer screening, although the optimal combination of methods and frequency of visits is unknown. | C | 16, 20, 22 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Cancer survivors face increased risk of many health problems, including recurrence of the original cancer, development of a second cancer, short- and long-term adverse effects of treatments, and psychosocial challenges. In addition to the cancer itself, these health risks are caused by treatments as well as inherited, lifestyle, and environmental factors.
Although many cancer survivors establish long-term follow-up with their oncologists, family physicians play a vital role in the prevention of illness and the treatment of complications and comorbid conditions. Cancer survivors whose care is shared with a family physician receive more preventive care than those treated primarily by oncologists.3 Additionally, nearly 70% of survivors experience comorbid conditions, with more than 30% having two or more comorbid diseases.4 Although patients express a preference for following up with their oncologists,5 there is no evidence of improved outcomes when care is provided by oncologists vs. family physicians.6
This article focuses on the role of family physicians in caring for survivors of cancers that are commonly diagnosed in adults and often survived for five years or more, including breast, colorectal, and prostate cancers; hematologic malignancies; and melanoma (Table 1).2 Additional information for patients about cancer and cancer survivorship is available from the following organizations: the American Cancer Society (http://www.cancer.org/), the National Cancer Institute (http://www.cancer.gov/), the National Coalition for Cancer Survivor-ship (http://www.canceradvocacy.org/), and the National Comprehensive Cancer Network (http://www.nccn.org/patients/guidelines/default.aspx).
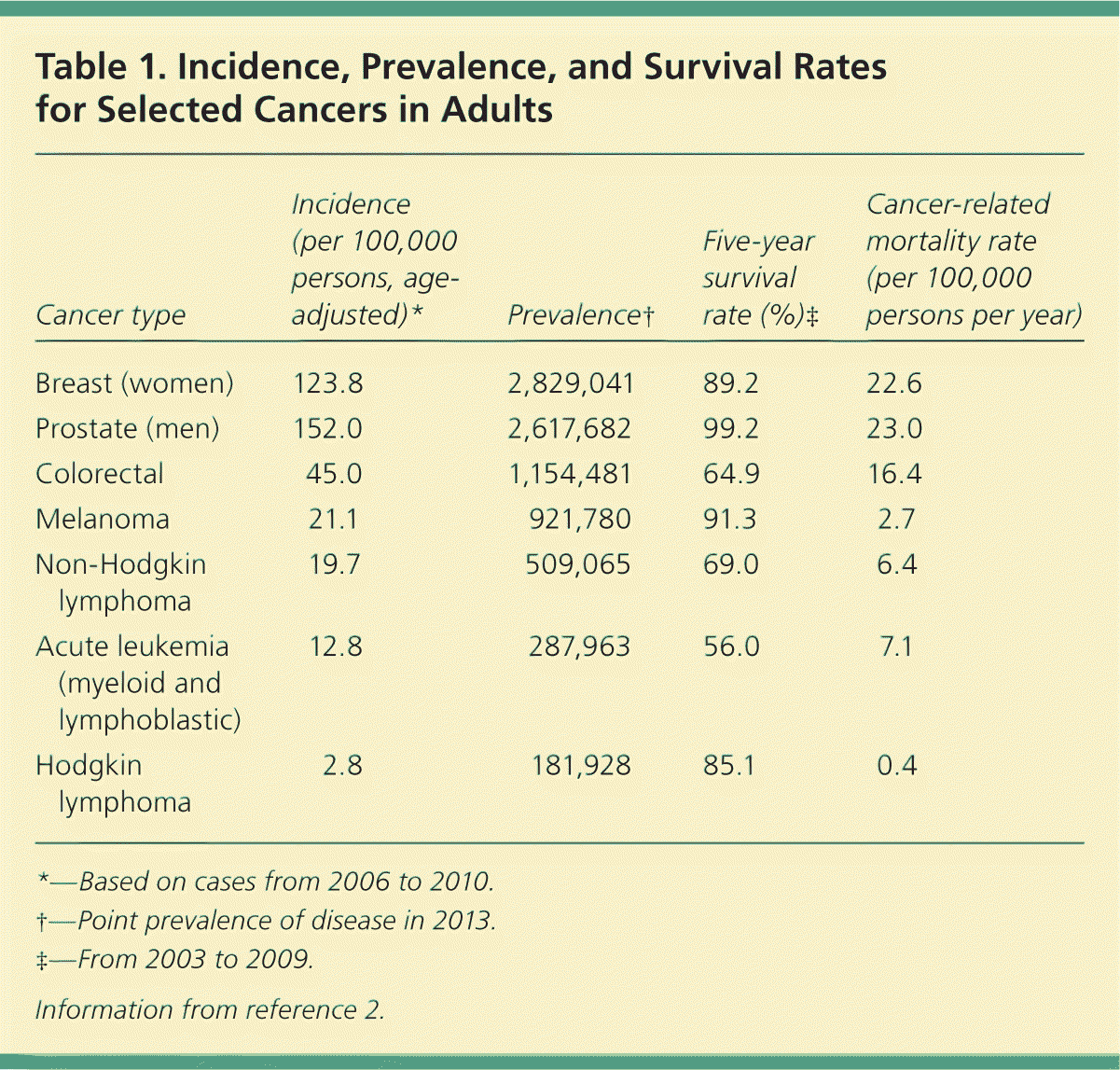
Table 1. Incidence, Prevalence, and Survival Rates for Selected Cancers in Adults
| Cancer type | Incidence (per 100,000 persons, age-adjusted)* | Prevalence† | Five-year survival rate (%)‡ | Cancer-related mortality rate (per 100,000 persons per year) |
|---|---|---|---|---|
| Breast (women) | 123.8 | 2,829,041 | 89.2 | 22.6 |
| Prostate (men) | 152.0 | 2,617,682 | 99.2 | 23.0 |
| Colorectal | 45.0 | 1,154,481 | 64.9 | 16.4 |
| Melanoma | 21.1 | 921,780 | 91.3 | 2.7 |
| Non-Hodgkin lymphoma | 19.7 | 509,065 | 69.0 | 6.4 |
| Acute leukemia (myeloid and lymphoblastic) | 12.8 | 287,963 | 56.0 | 7.1 |
| Hodgkin lymphoma | 2.8 | 181,928 | 85.1 | 0.4 |
*—Based on cases from 2006 to 2010.
†—Point prevalence of disease in 2013.
‡—From 2003 to 2009.
Information from reference 2.
General Care
PREVENTIVE CARE
Long-term cancer survivors require similar preventive care and health maintenance as adults without cancer, yet cancer survivors receive less counseling on diet, exercise, and smoking cessation than patients without cancer.6 Cancer survivors have lower rates of influenza vaccination, cervical cancer screening, and cholesterol screening than comparable persons without a history of cancer.7 These lower preventive service rates may be mitigated when cancer survivors receive care from oncologists and family physicians.7 Cancer survivors and their physicians may not appreciate other health risks in their focus on surviving cancer. For example, patients treated for localized prostate cancer are more likely to die of cardiovascular disease than of cancer.8
COMORBID CONDITIONS
Because cancer disproportionately affects persons older than 65 years, survivors often have comorbid conditions. To optimize the health of these patients, family physicians should address comorbidities. Although the data are mixed, cancer survivors with comorbidities may have higher mortality rates. Compared with patients with cancer who do not have diabetes mellitus, survivors with diabetes have a 40% greater risk of death from any cause.9 Colorectal cancer survivors are less likely than adults without cancer histories to receive recommended care for coronary artery disease, obstructive pulmonary disease, and diabetes.10
GENETICS
The family history plays an important role in overall cancer care. A three-generation family history is traditionally recommended but often not taken, representing a missed opportunity to identify genetic risks related to a cancer diagnosis.11 If a cancer survivor has a personal or family history suggestive of genetic cancer susceptibility (e.g., two or more first- or second-degree relatives with breast or ovarian cancer diagnosed before 50 years of age, indicating consideration for BRCA1 and BRCA2 testing), referral to a medical geneticist may be warranted.12
PSYCHOSOCIAL ISSUES
Compared with persons who do not have cancer, survivors are twice as likely to rate their health-related quality of life as poor.13 Cancer survivors may experience depression, anxiety, sleep disturbance, fatigue, sexual dysfunction, and cognitive impairment. These psychosocial issues may be related to the cancer or its treatment.
COORDINATED CARE
Limited evidence suggests that patients and family physicians prefer shared care with cancer specialists guided by a survivorship care plan.14 The survivorship care plan is a comprehensive discharge document developed by the cancer care team at the end of treatment and includes certain core elements (Table 2).1 Although survivorship care plans are endorsed by the Institute of Medicine, medical specialty organizations, and patient advocacy groups, there is no evidence showing benefit in patient outcomes, though research is ongoing.15
Table 2. Core Elements of the Survivorship Care Plan for Adults Completing Cancer Treatment

| Cancer treatment history |
| Potential long-term and late effects of treatment |
| Recommended surveillance for long-term and late effects |
| Recommended surveillance for recurrence and new cancers |
| Specific information about the timing and content of recommended follow-up |
| Recommendations on preventive practices, and how to maintain health and well-being |
| Information on legal protections regarding employment and access to health insurance |
| Availability of psychosocial services in the community |
Information from reference 1.
Specific Cancers
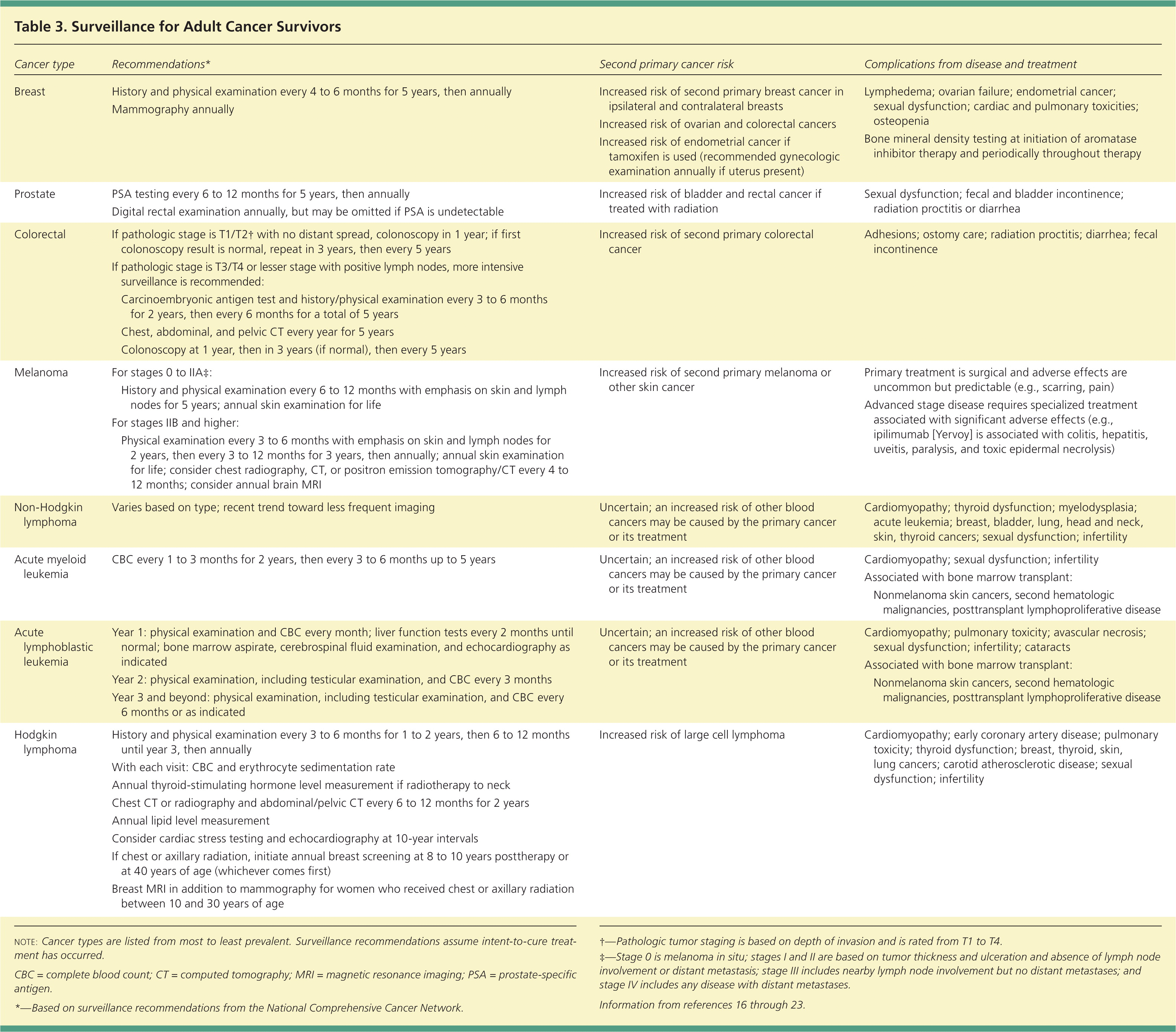
Each type of cancer and its treatments are associated with certain long-term risks. Table 3 lists surveillance recommendations, potential second primary cancers, and possible complications for several types of cancer.16–23 The surveillance recommendations apply to patients who have completed treatment and are assumed to be disease-free. These recommendations do not apply to patients with stage IV or metastatic cancers.
Table 3. Surveillance for Adult Cancer Survivors
| Cancer type | Recommendations* | Second primary cancer risk | Complications from disease and treatment | ||
|---|---|---|---|---|---|
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
|
|
|
| ||
note: Cancer types are listed from most to least prevalent. Surveillance recommendations assume intent-to-cure treatment has occurred.
CBC = complete blood count; CT = computed tomography; MRI = magnetic resonance imaging; PSA = prostate-specific antigen.
*—Based on surveillance recommendations from the National Comprehensive Cancer Network.
†—Pathologic tumor staging is based on depth of invasion and is rated from T1 to T4.
‡—Stage 0 is melanoma in situ; stages I and II are based on tumor thickness and ulceration and absence of lymph node involvement or distant metastasis; stage III includes nearby lymph node involvement but no distant metastases; and stage IV includes any disease with distant metastases.
BREAST CANCER
Breast cancer survivors are at risk of the initial cancer recurring and of a second primary breast cancer developing. Screening with physical examinations every four to six months and annual mammography is recommended.16 Routine breast self-examination is not recommended, but breast self-awareness (a woman's knowledge of her breast tissue so that she can determine if there is a new mass) is recommended.16 Routine surveillance with other imaging modalities and laboratory testing does not improve outcomes, such as detecting recurrences, overall survival, and quality of life.17
Recurrent breast cancer is often diagnosed within five years of treatment.24 Symptoms may be nonspecific (e.g., fatigue, weight loss) or from regional disease (e.g., breast mass, bone pain). Women should be counseled on lifestyle interventions that may decrease the risk of recurrence, including maintaining normal-range body mass index, consuming at least five servings of fruits and vegetables per day, and performing at least 150 minutes of aerobic exercise per week.16 Even during adjuvant treatment, exercise interventions improve cardiorespiratory fitness and the ability to perform daily activities.25
Complications of treatment vary depending on the type of treatment. Upper extremity lymphedema, which affects about 20% of women treated for breast cancer, may occur years after treatment.26 Higher risk of lymph-edema is associated with obesity, more extensive breast and axillary surgery, and axillary radiation.26 Lymph-edema may improve with physical therapy and the use of compressive arm sleeves, but evidence for effective treatments is limited.27
Chemotherapy for breast cancer is associated with a number of late effects, including heart failure, pulmonary toxicity, and leukemia.1 Antiestrogen therapy (e.g., tamoxifen) reduces the risk of recurrent cancer in hormone receptor–positive disease, but it causes hot flashes and sexual dysfunction and is associated with an increased risk of uterine cancer.28 Annual bimanual pelvic examination is recommended for women using tamoxifen.16 Compared with tamoxifen, aromatase inhibitors (e.g., anastrozole [Arimidex]) are more effective for postmenopausal estrogen receptor–positive breast cancers.29 Compared with antiestrogen therapy, aromatase inhibitors cause fewer thromboembolic events and endometrial cancers, but more arthralgia and fractures.29
PROSTATE CANCER
Prostate cancer survivors are at risk of cancer recurrence. Current recommendations include measuring serum prostate-specific antigen (PSA) levels every six to 12 months for the first five years after treatment, followed by annual measurement.16 Digital rectal examination is recommended annually but may be omitted if the PSA level is undetectable.16 PSA levels decline after definitive treatment, and rising levels indicate recurrence. Recurrent prostate cancer is initially treated with androgen deprivation therapy.30 However, all recurrent prostate cancers eventually become resistant to androgen deprivation therapy, at which point chemotherapy or radiotherapy may be appropriate.
Radiotherapy for prostate cancer is associated with an increased risk of bladder and rectal cancers.31 Because the absolute risk of these secondary cancers is small, testing is not recommended.
Localized prostate cancer is treated with prostatectomy or radiotherapy (with androgen deprivation therapy if the cancer is high-grade).16 Complications of both approaches include incontinence and erectile dysfunction. A large 15-year follow-up trial has shown no significant difference in complication rates between prostatectomy and radiotherapy.32 Observation and active surveillance are alternatives for men with low-grade, low-risk cancers or a shorter life expectancy, whose health goals prioritize avoidance of treatment complications.16
Prostate cancer has a 99% five-year survival rate, largely because of increased diagnosis in the era of widespread PSA testing,33 and survivors are more likely to experience morbidity attributable to treatment than directly from the cancer.18 Urinary incontinence is treated with pelvic floor exercises and biofeedback, although evidence of benefit is mixed.34 Erectile dysfunction often responds to treatment with phosphodiesterase-5 inhibitors (e.g., sildenafil [Viagra]).35 Radiation proctitis causes rectal bleeding, tenesmus, diarrhea, and fecal incontinence. Proctitis typically resolves over time after radiation is completed, and is treated with dietary changes (e.g., supplemental fiber) and hydrocortisone enemas.18
Prostate cancer survivors may receive androgen deprivation therapy for two to three years for their initial diagnosis or indefinitely for recurrent disease. In addition to causing erectile dysfunction, androgen deprivation therapy is associated with osteopenia, fatigue, anemia, and gynecomastia. Men receiving androgen deprivation therapy should be monitored for these complications.33
COLORECTAL CANCER
Colorectal cancer survivors are at risk of disease recurrence and second primary colorectal cancers.2 Almost 95% of colorectal cancer recurrences are diagnosed within five years of treatment.36 Surveillance recommendations are based on the stage of the cancer at diagnosis (Table 316–23 ). Although one systematic review found a survival benefit with more intensive surveillance,19 recommendations are based on expert consensus.16 At a minimum, colonoscopy should be performed one year after treatment, assuming that a complete colonoscopy was performed before treatment.
Survivors of colorectal cancer may experience gastrointestinal complications of treatment, including diarrhea, abdominal pain, and fecal incontinence.37 Initial management of diarrhea consists of increased dietary fiber and antidiarrheal medication (e.g., loperamide [Imodium]). Fatigue is the most commonly reported symptom in colorectal cancer survivors.38 Clinicians should ask about sleep quality, stress, and depression, and consider other potential causes (e.g., anemia, thyroid disease) in patients presenting with fatigue. Patients with ostomies are more likely to report symptoms after treatment, and the presence of an ostomy can cause psychological distress and sexual dysfunction.38 Consultation with an ostomy specialist may benefit patients who are having difficulties.
MELANOMA
The number of persons living with melanoma in the United States is rapidly increasing, driven in part by increased numbers of skin biopsies.39 Between 4% and 8% of melanoma survivors develop a second primary melanoma in their lifetime, and recurrence has been documented decades after initial treatment.40 Therefore, indefinite surveillance is recommended by expert consensus guidelines.16 Annual physician skin examinations have limited evidence but are recommended, whereas blood tests and imaging are not recommended.16 Family physicians should educate survivors about recognizing the characteristics of potentially malignant skin lesions and using sun protection. Daily use of sunscreen is recommended to reduce the risk of melanoma.41
LEUKEMIAS AND LYMPHOMAS
There are almost 1 million survivors of leukemia and lymphoma living in the United States.2 Recurrence of disease is a major concern, and surveillance recommendations are specific to the particular cancer16 (Table 316–23 ). Although surveillance by an oncologist is recommended for the first five years after treatment, family physicians provide shared care with oncologists during and after treatment, and care for patients with more distant histories of leukemia and lymphoma.
Most cases of Hodgkin lymphoma are diagnosed in patients younger than 40 years.2 Because Hodgkin lymphoma survivors often live decades after their initial diagnosis, complications may develop over an extended period of time. Young female lymphoma survivors treated with chest or axillary radiation have a risk of breast cancer approaching a cumulative incidence of 20% by 45 years of age.20 Multiple expert-based guidelines recommend that annual breast cancer screening with mammography and magnetic resonance imaging be initiated eight to 10 years after chest or axillary radiation treatment or by 40 years of age, whichever comes first.16,20 Chest radiation is also associated with early coronary artery disease, and patients should be evaluated for other cardiovascular risk factors and counseled to reduce the risk of cardiovascular disease.21
Survivors of leukemia and lymphoma may experience additional complications related to treatment with chemotherapy, corticosteroids, and radiation.22 Family physicians should be alert to late effects of treatment, such as thyroid dysfunction, sexual dysfunction, and treatment-related cancers. Survivors of leukemia treated with bone marrow transplantation are at high risk of developing nonmelanoma skin cancers and secondary blood cancers.23
Data Sources: Sources searched include PubMed, Cochrane database, National Guideline Clearinghouse, Agency for Healthcare Research and Quality, and Essential Evidence Plus. Search terms included: cancer survivor, survivorship, surveillance, follow-up, breast cancer, prostate cancer, colorectal cancer, lymphoma, leukemia, and melanoma. Search dates: January and February 2014, and October 2014.
The author thanks Deborah Wilbur, MD, for her assistance editing this manuscript.

