A 30-year-old man presented to the emergency department with rapidly worsening swelling of the lips (see accompanying figure) that began three hours earlier. He had a history of a developmental disability and hypertension treated with lisinopril (Zestril) for two years. He had no previous episodes of swelling.
Physical examination revealed localized swelling of the upper and lower lips, but no other significant findings. He did not have swelling elsewhere on the body.
Figure
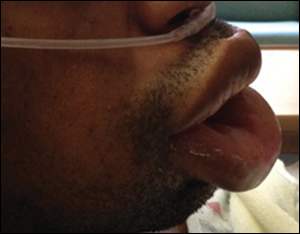
Question
Based on the history and physical examination findings, which one of the following will not aid in the diagnosis and treatment of this patient?
A. C1 inhibitor, C4, C3, and C1q measurements.
B. Serum interleukin-5 and serum eosinophil measurements.
C. Serum tryptase and 24-hour urine histamine measurements.
D. Skin biopsy.
E. Review of medications.
Discussion
The answer is D: skin biopsy. The dermatopathologic findings do not provide clues to the underlying etiology of angioedema. Angioedema is related to increased capillary permeability in the subcutaneous layer.1 Angioedema is usually idiopathic and often occurs when patients are in their 40s or 50s.
Levels of complement C1 inhibitor, C4, C3, and C1q can help distinguish between hereditary, acquired, and other causes of angioedema (see accompanying table).2 The first step in confirming any episode of angioedema is to order a serum C4 level measurement; if the level is depressed, a subsequent C1 inhibitor assay is needed. Hereditary angioedema is differentiated from acquired forms by evaluating levels of C1q. C1q levels are depressed in the acquired form, whereas they are normal in the hereditary form; both forms exhibit low C4 levels.3 The absence of family history, immunologic disorders, or previous malignancy may also suggest acquired angioedema.1 A substantial decrease in C1q inhibitor levels in the acquired form renders C1q available for autoactivation, with initiation of a classical pathway of the complement cascade leading to an inappropriate inflammatory response.1 In idiopathic and allergic angioedema, complement markers remain within the normal range. Patients with idiopathic angioedema may or may not have detectable levels of autoantibodies.3
Suspected angioedemaeosinophilia syndrome warrants a serum interleukin-5 measurement because it specifically controls the differentiation and the recruitment of eosin-ophils to the peripheral circulation from the bone marrow.3 Serum interleukin-5 is elevated in angioedema-eosinophilia syndrome, which can be clinically established with severe bouts of urticaria and pruritus, as well as rapid elevation of serum eosinophils.4
Serum tryptase and 24-hour urine histamine levels are useful markers when evaluating for allergic angioedema. Both are markers of histamine release and will be elevated in someone with an allergic response to a trigger or stressor.5
The medication review is important because nonsteroidal anti-inflammatory drugs (e.g., ibuprofen, naproxen [Naprosyn]) and angiotensin-converting enzyme inhibitors (e.g., lisinopril, captopril) are associated with angioedema.4 Angiotensin-converting enzyme inhibitors are also known to increase flare-ups in those with hereditary angioedema.1 Angioedema in response to a medication most commonly occurs within a week of starting the medication, but can develop months to years after use.
Table. Causes of Angioedema
| Condition | Characteristics | Complement levels |
|---|---|---|
| Hereditary | Begins in childhood; skin, laryngeal, or gastrointestinal attacks possible; does not respond to antihistamines or steroids | C4, C1 inhibitor: Low |
| C1q, C3: Normal | ||
| Acquired | Begins in the 40s and 50s; associated with malignancy and autoimmune disorders; may have trauma or stress triggers | C4, C1 inhibitor, C1q, C3: Low |
| Medication associated | Angiotensin-converting enzyme inhibitors and nonsteroidal anti-inflammatory drugs are common causes | C4, C1 inhibitor, C1q, C3: Normal |
| Allergic | May also have pruritus, urticaria, or anaphylaxis; associated with an exposure | C4, C1 inhibitor, C1q, C3: Normal |
| Idiopathic | Frequent attacks; responds to antihistamines and steroids; associated with urticaria | C4, C1 inhibitor, C1q, C3: Normal |
| Angioedema-eosinophilia syndrome | Periodic attacks associated with urticaria and pruritus; high eosinophil counts; resolves spontaneously | C4, C1 inhibitor, C1q, C3: Normal |
Information from reference 2.

