Hypertension is the most common chronic condition treated by family physicians. Elevated blood pressure is associated with an increased risk of heart failure, myocardial infarction, cerebrovascular disease, and death. Treatment of hypertension reduces the risk of these events. Several lifestyle modifications are associated with improvements in blood pressure, including the Dietary Approaches to Stop Hypertension diet, sodium restriction, regular exercise, and moderate weight loss. There is strong evidence that reducing diastolic blood pressure to less than 90 mm Hg is beneficial in adults older than 30 years. Although there is good evidence to support reducing systolic blood pressure to less than 150 mm Hg in adults older than 60 years, the evidence in younger adults is insufficient to recommend a specific goal. Black patients with chronic kidney disease who are treated with an angiotensin-converting enzyme inhibitor or angiotensin receptor blocker to a blood pressure of less than 140/90 mm Hg experience slower declines in glomerular filtration rates than patients treated with other medications. A blood pressure goal of less than 140/90 mm Hg is recommended in patients with chronic kidney disease and in those with diabetes mellitus. Thiazide diuretics, angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, and calcium channel blockers are the preferred medications in nonblack patients; thiazide diuretics and calcium channel blockers are preferred in black patients.
Hypertension is the most common chronic condition treated by family physicians1 and is associated with an increased risk of coronary artery disease, heart failure, myocardial infarction, chronic kidney disease (CKD), cerebrovascular events, and death.2,3 Treatment of hypertension is associated with reduced incidence of these conditions and reduced mortality.4,5 The U.S. Preventive Services Task Force strongly recommends screening all adults older than 18 years for hypertension.6 In 2013, the Journal of the American Medical Association independently published guidelines for the management of hypertension from the panel members assigned to the Eighth Joint National Committee (JNC 8),7 updating the 10-year-old guidelines on the assessment and management of hypertension in adults (JNC 71). The American Academy of Family Physicians has endorsed the JNC 8 guidelines. This article reviews common questions associated with the new recommendations.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Lifestyle modifications, including the Dietary Approaches to Stop Hypertension diet, sodium restriction, weight loss, and moderate exercise, are associated with reductions in blood pressure, and should be recommended to all patients with hypertension. | B | 8–10, 14 |
| In patients older than 30 years, treatment of diastolic blood pressure to less than 90 mm Hg reduces rates of cardiovascular disease, stroke, and death. | A | 19–22 |
| Treatment of systolic blood pressure to less than 150 mm Hg in patients without comorbid conditions who are older than 60 years reduces rates of cardiovascular disease, stroke, and death. | A | 23–26 |
| Treatment of systolic blood pressure to less than 140 mm Hg is recommended in adults 30 to 60 years of age who do not have comorbid conditions. | C | 7 |
| Treatment of black patients who have chronic kidney disease with an angiotensin-converting enzyme inhibitor reduces the decline in glomerular filtration rate compared with beta blockers or calcium channel blockers. | C | 32 |
| Patients with chronic kidney disease or diabetes mellitus should be treated to a goal blood pressure of less than 140/90 mm Hg. | C | 29, 30, 33–35 |
| First-line pharmacologic treatment of hypertension for nonblack patients includes thiazide diuretics, calcium channel blockers, angiotensin-converting enzyme inhibitors, and angiotensin receptor blockers. | B | 36, 38, 39 |
| First-line pharmacologic treatment of hypertension for black patients includes thiazide diuretics or calcium channel blockers. | B | 40 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
What Questions Did JNC 8 Address?
JNC 8 focused on three questions determined by a 17-member panel originally appointed by the National Heart, Lung, and Blood Institute and used a systematic review of randomized controlled trials (RCTs) that met specific inclusion criteria. The guideline did not address the classification of hypertension, methods for diagnosing hypertension, or initial laboratory evaluation of patients with hypertension (Table 1).1
The questions addressed by JNC 8 included the following:
- In adults with hypertension, does initiating pharmacologic therapy at specific blood pressure thresholds improve health outcomes?
- In adults with hypertension, does treatment with antihypertensive pharmacologic therapy to a specified blood pressure goal lead to improvements in health outcomes?
- In adults with hypertension, do various antihypertensive drugs or drug classes differ in comparative benefits and harms for specific health outcomes?7
Table 1. Initial Laboratory Evaluation of Hypertension from JNC 7
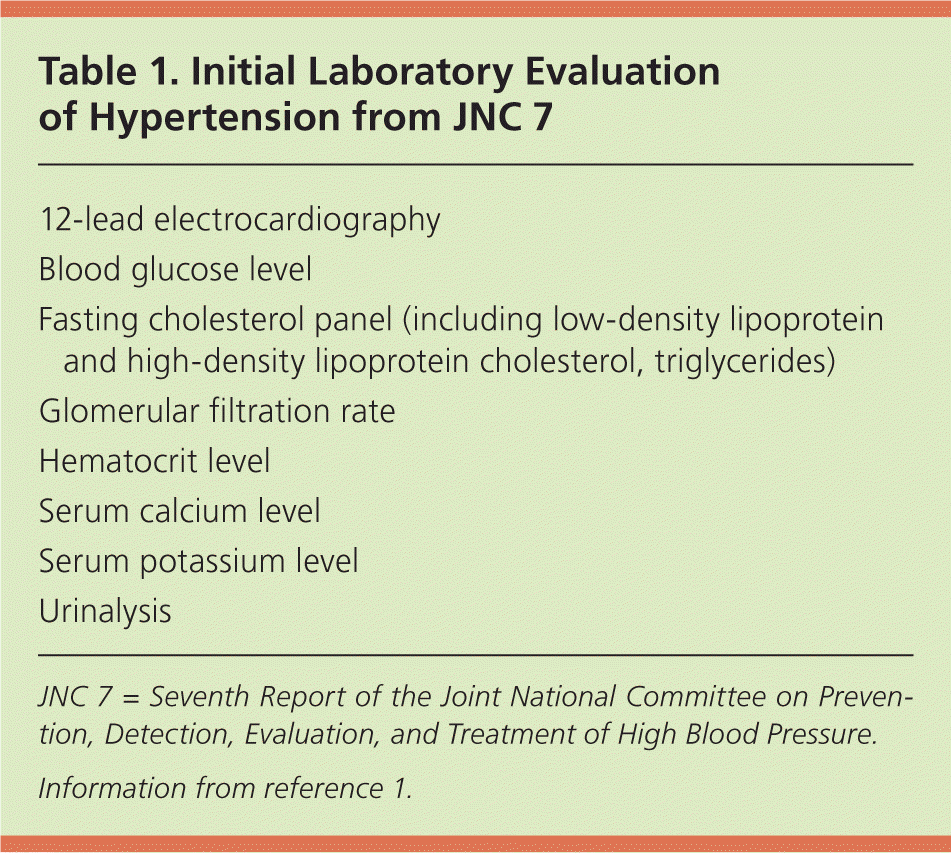
| 12-lead electrocardiography |
| Blood glucose level |
| Fasting cholesterol panel (including low-density lipoprotein and high-density lipoprotein cholesterol, triglycerides) |
| Glomerular filtration rate |
| Hematocrit level |
| Serum calcium level |
| Serum potassium level |
| Urinalysis |
JNC 7 = Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure.
Information from reference 1.
What Are the Effects of Nonpharmacologic Strategies on Blood Pressure?
In the general adult population, patients benefit from following the Dietary Approaches to Stop Hypertension (DASH) dietary pattern and reducing their sodium intake (Table 2).8,9 Combining both strategies lowers blood pressure more than either one alone. Engaging in moderate to vigorous aerobic physical activity for 40 minutes three or four times per week decreases systolic blood pressure (SBP) and diastolic blood pressure (DBP). Weight loss and moderation of alcohol consumption also reduce the risk of hypertension.
Table 2. Components of the Dietary Approaches to Stop Hypertension Diet
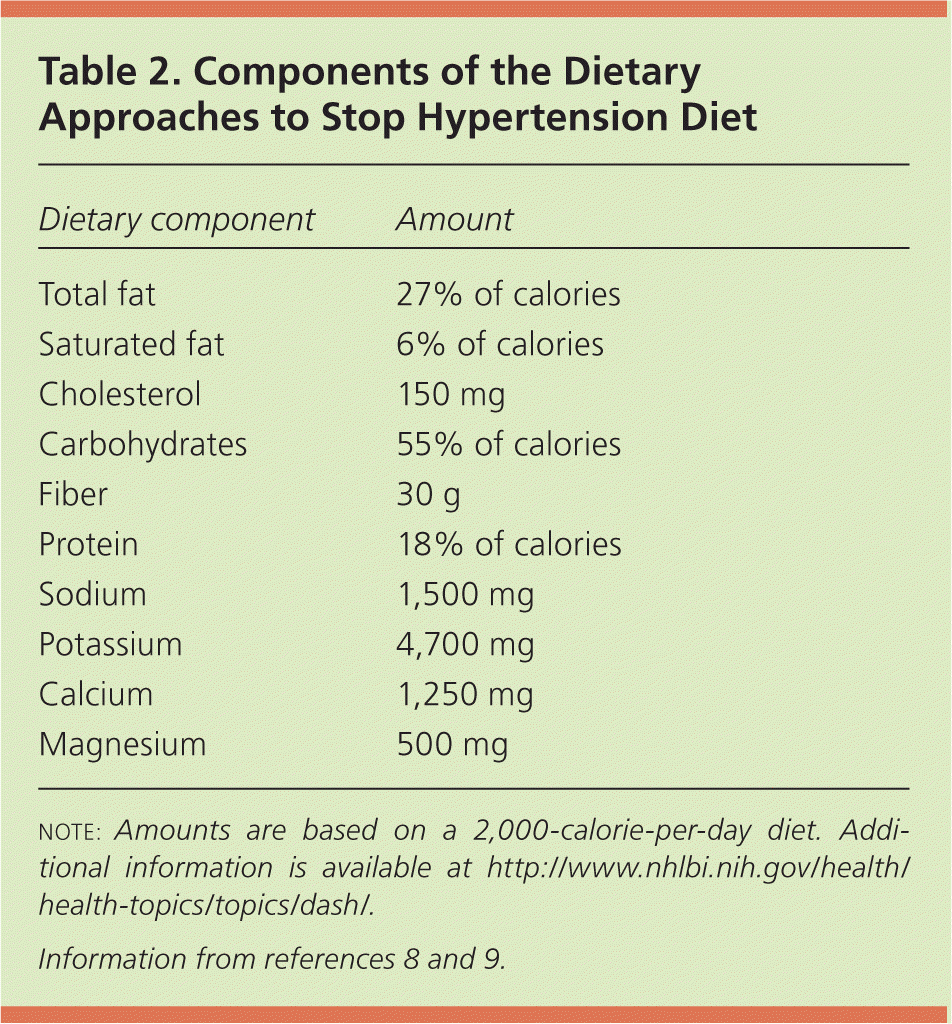
| Dietary component | Amount |
|---|---|
| Total fat | 27% of calories |
| Saturated fat | 6% of calories |
| Cholesterol | 150 mg |
| Carbohydrates | 55% of calories |
| Fiber | 30 g |
| Protein | 18% of calories |
| Sodium | 1,500 mg |
| Potassium | 4,700 mg |
| Calcium | 1,250 mg |
| Magnesium | 500 mg |
note: Amounts are based on a 2,000-calorie-per-day diet. Additional information is available at http://www.nhlbi.nih.gov/health/health-topics/topics/dash/.
SUPPORTING EVIDENCE
The JNC 8 panel endorsed the recommendations from the American Heart Association/American College of Cardiology Lifestyle Work Group summarized in Table 3.10 The original DASH trial in 1997 showed that a diet rich in fruits, vegetables, and low-fat dairy products and limited in saturated and total fats substantially lowered blood pressure in adults.8 Blood pressure was also decreased when dietary sodium intake was restricted to less than 1,500 mg per day; when this restriction was combined with the DASH diet, blood pressure reductions were greater.9 Small observational studies suggest that decreasing sodium intake by approximately 1,000 mg per day is associated with a reduction in rates of cardiovascular events.11–13 There is insufficient evidence to determine if changes in dietary intake of other nutrients (e.g., potassium, calcium) reduce blood pressure.10 Weight loss of approximately 9 lb (4 kg) is associated with a modest reduction in SBP and DBP, but the effects on mortality are unknown.14 Regular aerobic exercise decreases SBP and DBP in patients with hypertension.10
Table 3. Lifestyle Recommendations for Lowering Blood Pressure

| Consume a diet that emphasizes intake of vegetables, fruits, and whole grains; includes low-fat dairy products, poultry, fish, legumes, nontropical vegetable oils, and nuts; and limits intake of sweets, sugar-sweetened beverages, and red meat. Adapt this dietary pattern to appropriate caloric requirements, personal and cultural food preferences, and nutritional therapy for other medical conditions (including diabetes mellitus). Follow plans such as the DASH diet, the U.S. Department of Agriculture Food Patterns, or the American Heart Association diet. |
| Consume no more than 2,400 mg of sodium per day. Further reduction of sodium intake to 1,500 mg per day is associated with even greater reduction in blood pressure. Reducing intake by at least 1,000 mg per day will lower blood pressure even if the desired daily intake is not achieved. |
| Combine the DASH diet with lower sodium intake. |
| In general, advise adults to engage in aerobic physical activity to lower blood pressure (three or four 40-minute sessions of moderate to vigorous activity per week). |
DASH = Dietary Approaches to Stop Hypertension.
Information from reference 10.
Tobacco use is associated with an acute increase in blood pressure,15 and tobacco cessation is associated with reduced rates of stroke and myocardial infarction.16 Regular consumption of alcoholic drinks increases blood pressure in patients with hypertension.17 Reducing alcohol consumption to no more than two drinks per day in men and no more than one drink per day in women improves blood pressure,18 but the effect on cardiovascular end points is unknown. The effects of lifestyle modifications on blood pressure are summarized in Table 4.8–11,14,18
Table 4. Effects of Select Lifestyle Modifications on Blood Pressure

| Intervention | Reduction in blood pressure (mm Hg) | |
|---|---|---|
| Systolic | Diastolic | |
| DASH diet plus sodium restriction | 11.5 | 5.7 |
| Sodium restriction (< 1,500 mg per day) | 7 | 3 |
| DASH diet | 5 to 6 | 3 |
| Weight loss (approximately 9 lb [4 kg]) | 4.5 | 3.2 |
| Exercise | 4 | 3 |
| Restriction of alcohol consumption | 3 | 2 |
note: There is insufficient evidence to state whether a combination of these interventions (other than DASH diet plus sodium restriction) has an additive effect on blood pressure reduction.
DASH = Dietary Approaches to Stop Hypertension.
What Are the Thresholds for Initiating Pharmacotherapy for Hypertension, and What Are the Blood Pressure Goals?
In the general population 60 years and older, pharmacologic treatment should be initiated to achieve a goal blood pressure of less than 150/90 mm Hg. In the general population 30 to 59 years of age, there is good evidence to support pharmacologic treatment to achieve a goal DBP of less than 90 mm Hg. There is insufficient evidence to support an SBP goal, but based on expert opinion, a goal of less than 140 mm Hg is recommended.
SUPPORTING EVIDENCE
The evidence supporting the beneficial effects of lowering DBP is more than 45 years old.19 Since then, numerous RCTs have confirmed that treating DBP to a goal of less than 90 mm Hg improves cardiovascular outcomes and mortality rates. These benefits have been shown in patients older than 30 years.20–22 In trials of adults older than 60 years, treatment to a goal of less than 150/90 mm Hg was associated with reductions in patient-centered outcomes such as overall mortality, cardiovascular mortality, and the incidence of cerebrovascular events.23–25 In a meta-analysis of studies involving patients 60 to 80 years of age, treatment of moderate to severe hypertension was associated with a reduction in cardiovascular and all-cause mortality.26 In these trials, reductions in SBP occurred at the same time as reductions in DBP, making it difficult to discern if the improvements in outcomes were a result of lowering SBP, DBP, or both. The JNC 8 panel concluded that there is insufficient evidence to support a specific SBP goal in adults younger than 60 years.
There is evidence that tight control of blood pressure in adults who do not have other risk factors does not confer benefits and may subject patients to adverse effects of medications. A Cochrane review concluded that treatment of patients with mild hypertension (SBP of 140 to 159 mm Hg and DBP of 90 to 99 mm Hg) did not reduce morbidity or mortality compared with placebo.27 However, a more recent meta-analysis that included data from additional trials found that treatment of mild hypertension reduced strokes, cardiovascular deaths, and total deaths after five years.28 No good-quality RCTs have assessed the benefits of treating elevated DBP in persons younger than 30 years.
The JNC 8 panel concluded that there is strong evidence of benefit for treating DBP greater than 90 mm Hg in adults older than 30 years and for treating SBP greater than 150 mm Hg in adults older than 60 years. Based on expert opinion, they recommend that SBP greater than 140 mm Hg be treated in adults younger than 60 years. The panel also recommends that if an adult undergoing treatment has a blood pressure below these goals and there are no adverse effects from treatment, the antihypertensive regimen should not be changed.7
What Are the Recommended Blood Pressure Goals and Initial Drug Choices for Patients with Diabetes Mellitus or CKD?
In patients with CKD, an angiotensin-converting enzyme (ACE) inhibitor or angiotensin receptor blocker (ARB) should be prescribed, regardless of race. Patients with diabetes or CKD should be treated to a blood pressure goal of less than 140/90 mm Hg.
SUPPORTING EVIDENCE
JNC 8 defines CKD as a measured or estimated glomerular filtration rate (GFR) of less than 60 mL per minute per 1.73 m2 in patients younger than 70 years, or greater than 30 mg of albumin per g of creatinine, regardless of GFR, in patients of any age. A meta-analysis by the National Kidney Disease Education Program concluded that blood pressure goals are unclear in patients with CKD and recommended a goal of less than 130/80 mm Hg based on observational data.29 A systematic review showed no clear benefit for cardiovascular outcomes when blood pressure was lowered to less than 130/80 mm Hg compared with less than 140/90 mm Hg in patients with CKD, although the review had insufficient power to address this question.30 The ongoing Systolic Blood Pressure Intervention Trial is a large, multicenter RCT designed to determine if more intensive SBP control results in better cardiovascular outcomes.31
In the African American Study of Kidney Disease and Hypertension, ACE inhibitors slowed GFR decline more effectively than beta blockers or calcium channel blockers in black patients with CKD, but they did not improve cardiovascular outcomes.32 Based on these results, JNC 8 recommends an ACE inhibitor or ARB for patients with CKD, regardless of their race.
In patients with diabetes, a blood pressure goal of less than 140/90 mm Hg is recommended, and no specific antihypertensive agent is preferred.7 Compared with a goal of less than 180/105 mm Hg, treatment to a goal of less than 150/85 mm Hg is associated with reductions in diabetes-related mortality and complications, and progression of diabetic retinopathy.33 The Action to Control Cardiovascular Risk in Diabetes trial did not show any improvement in fatal and nonfatal major cardiovascular events when SBP was lowered to less than 120 mm Hg compared with less than 140 mm Hg.34 A 2013 Cochrane review concluded that evidence does not support lowering blood pressure in patients with diabetes to a goal lower than that for patients without diabetes.35
Are There Benefits to Using Specific Classes of Antihypertensive Agents in Specific Populations?
In the general nonblack population, initial antihypertensive treatment should include a thiazide diuretic, calcium channel blocker, ACE inhibitor, or ARB. In the general black population, initial treatment should include a thiazide diuretic or calcium channel blocker.
SUPPORTING EVIDENCE
Thiazide diuretics, which were recommended as first-line therapy in the JNC 7 guidelines because of their effectiveness, improvements in patient-centered outcomes, low cost, and favorable adverse effect profile, are recommended by JNC 8 for the same reasons.36 Evidence does not support the use of chlorthalidone over hydrochlorothiazide, or hydrochlorothiazide doses of more than 25 mg.37 Unlike JNC 7, the new guidelines recommend three other classes of antihypertensive medications (ACE inhibitors, ARBs, and calcium channel blockers) as first-line agents in the general nonblack population, and thiazide diuretics or calcium channel blockers as first-line agents in the general black population. This recommendation is based on the results of several RCTs that showed similar improvements in overall mortality, cardiovascular outcomes, cerebrovascular outcomes, and renal outcomes between drug classes.38,39 The JNC 8 panel did not include specific high-risk populations (such as patients with recently diagnosed coronary artery disease or heart failure) in their review of this question. In the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial, thiazide diuretics were superior to calcium channel blockers, and both were superior to ACE inhibitors, in improving cerebrovascular, heart failure, and combined cardiovascular outcomes in black patients.40
Beta blockers are not first-line antihypertensive medications in JNC 8. A Cochrane review concluded that beta blockers (mainly atenolol [Tenormin]) provide modest reductions in cardiovascular outcomes in patients with hypertension, but confer no mortality benefit.41 ACE inhibitors and ARBs should not be prescribed concurrently because this combination increases the risk of renal complications.7 Initiating two medications simultaneously may be considered for patients with markedly elevated blood pressure or multiple comorbidities.1,7,42,43 If more than three medications are needed for blood pressure control, medications from other classes may be required.
How Do Other Hypertension Guidelines Differ from JNC 8?
Recently published guidelines include those by the American Society of Hypertension and the European Society of Hypertension/European Society of Cardiology. Both guidelines make recommendations about antihypertensive medication classes in patients with specific comorbidities. New guidelines from the American Heart Association/American College of Cardiology are expected to be published in 2015.
SUPPORTING EVIDENCE
The American Society of Hypertension clinical practice guideline is intended for use by primary care physicians.42 It recommends a blood pressure goal of less than 140/90 mm Hg for most patients (including those with diabetes and CKD), and less than 150/90 mm Hg for patients 80 years and older. Unlike JNC 8, this guideline makes specific recommendations about medication classes in patients with coronary artery disease, heart failure, and a history of cerebrovascular events.
The European Society of Hypertension/European Society of Cardiology guideline includes classes of recommendations and levels of evidence.43 It recommends a general blood pressure goal of less than 140/90 mm Hg, except in patients older than 80 years, in whom a goal of less than 150/90 mm Hg is suggested, and in patients with diabetes, in whom a DBP of less than 85 mm Hg is recommended. As compared with JNC 8, beta blockers are considered a first-line treatment in young nonblack patients. The guideline also addresses medication use in patients with specific comorbidities. A comparison of disease-specific recommendations is presented in Table 5.42,43
Table 5. Initial Antihypertensive Drug Selection by Patient Population
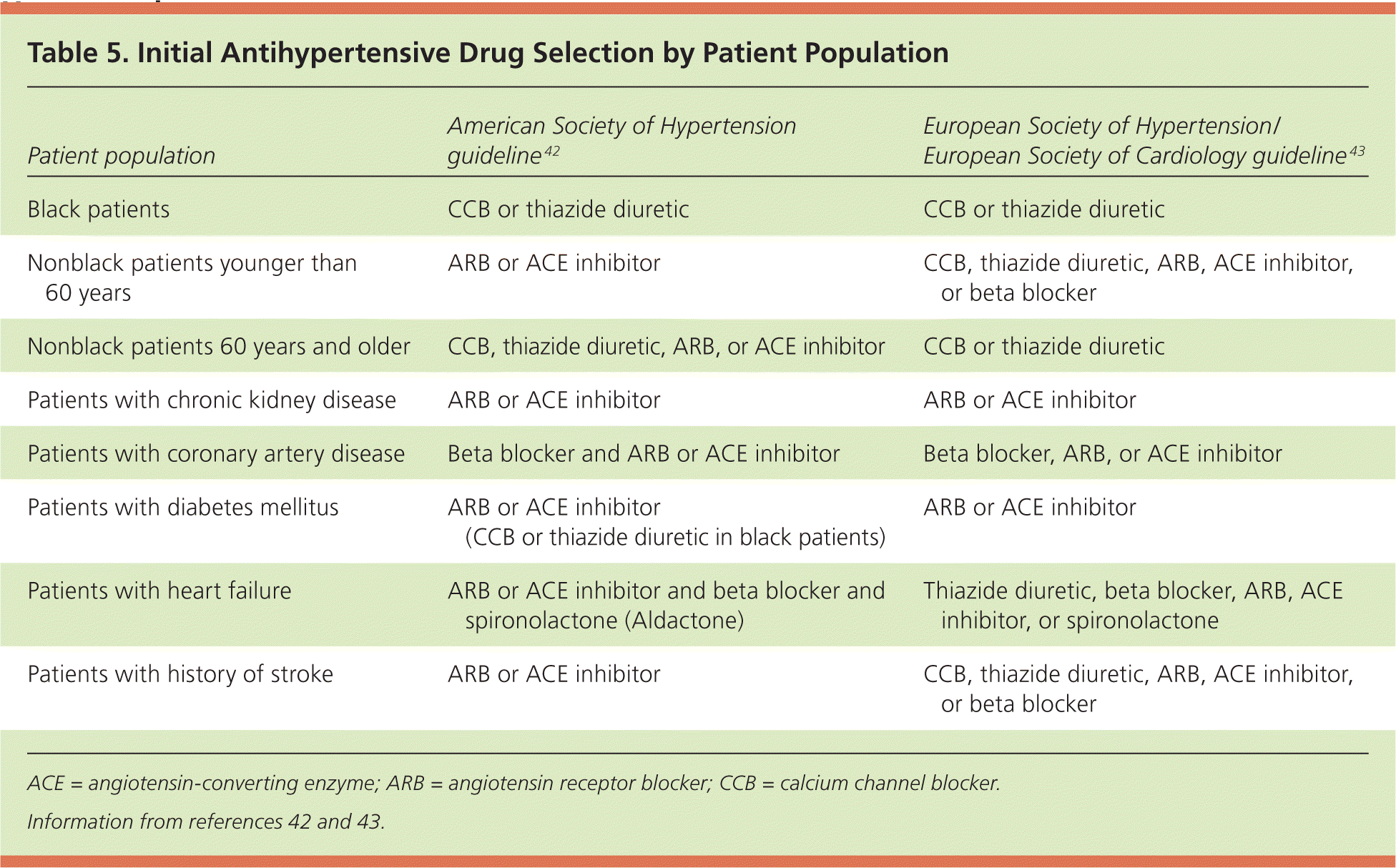
| Patient population | American Society of Hypertension guideline42 | European Society of Hypertension/European Society of Cardiology guideline43 |
|---|---|---|
| Black patients | CCB or thiazide diuretic | CCB or thiazide diuretic |
| Nonblack patients younger than 60 years | ARB or ACE inhibitor | CCB, thiazide diuretic, ARB, ACE inhibitor, or beta blocker |
| Nonblack patients 60 years and older | CCB, thiazide diuretic, ARB, or ACE inhibitor | CCB or thiazide diuretic |
| Patients with chronic kidney disease | ARB or ACE inhibitor | ARB or ACE inhibitor |
| Patients with coronary artery disease | Beta blocker and ARB or ACE inhibitor | Beta blocker, ARB, or ACE inhibitor |
| Patients with diabetes mellitus | ARB or ACE inhibitor (CCB or thiazide diuretic in black patients) | ARB or ACE inhibitor |
| Patients with heart failure | ARB or ACE inhibitor and beta blocker and spironolactone (Aldactone) | Thiazide diuretic, beta blocker, ARB, ACE inhibitor, or spironolactone |
| Patients with history of stroke | ARB or ACE inhibitor | CCB, thiazide diuretic, ARB, ACE inhibitor, or beta blocker |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker; CCB = calcium channel blocker.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms hypertension, high blood pressure, and treatment. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, Essential Evidence Plus, the Institute for Clinical Systems Improvement, the National Guideline Clearinghouse database, and the U.S. Preventive Services Task Force. Search dates: March 1, 2014, and October 10, 2014.

