A 44-year-old man on active duty in the Marines presented with a dry, red patch of skin on his back that had been present for two days. The rash was pruritic and painful to touch. There was no discharge from the lesion. The patient did not have fever or new environmental contacts. He had not been carrying constrictive or heavy gear on his back, and he was not using any new soap or laundry detergent. His medical history was significant for a myocardial infarction several years earlier. Six weeks prior to presenting with the rash, he had coronary stents replaced in a five-hour procedure.
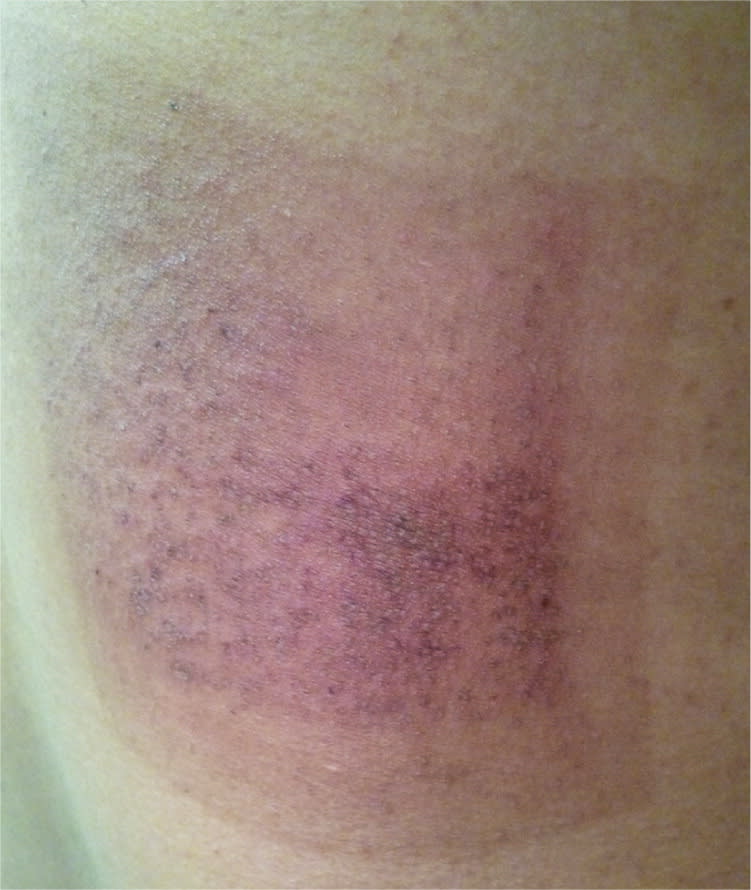
Physical examination revealed a single, nonraised, rhomboid-shaped area inferior to the right scapula (Figure 1). The erythematous lesion was well demarcated. There was a visible capillary break with petechiae 1.5 cm inside of the borders. The central portion of the lesion had a fine scale. There were no other lesions or physical findings.
Figure 1.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Antibiotic-related dermatitis.
B. Irritant contact dermatitis.
C. Pityriasis rosea.
D. Psoriasis.
E. Tinea corporis.
Discussion
The answer is B: irritant contact dermatitis. This patient's lesion was well demarcated and in the shape of the grounding pad used during his recent cardiac stenting procedure. Contact dermatitis can occur from prolonged exposure to the adhesive.
Irritant contact dermatitis may present after exposure to wet conditions, detergents, surfactants, solvents, oxidizing agents, acids, or alkalis.1 The initial treatment for contact dermatitis is to remove the irritant. Topical corticosteroids are generally effective. The steroid potency depends on the severity and location of the lesion. For this patient, the lesion was mild to moderate and treated with a low- to medium-potency topical steroid applied twice daily for one to two weeks.
Dermatitis from antibiotic use commonly presents within one to two weeks of exposure and must be considered with any rash presenting after antibiotic use. Dermatitis from oral antibiotics presents as a diffuse, erythematous, pruritic, maculopapular rash. The rash can occur any time after exposure but resolves with cessation of the antibiotic.2,3
Pityriasis rosea is usually asymptomatic. It often occurs after an upper respiratory tract infection. The lesion classically presents with a single salmon-colored herald patch on the trunk, followed by multiple lesions one to two weeks later. The lesions are plaques with a red collarette of scale. They are usually oval shaped, and the long axis follows skin tension lines. The lesions are classically described as appearing in a Christmas tree distribution on the back. 2,3
Psoriasis is a common skin disorder with a wide range of clinical presentations, including chronic plaques. Plaque psoriasis is the most common presentation and manifests as red and white scaly patches with a silvery-white appearance. Plaques often appear on the elbows and knees, but can occur in any area, including the scalp, genitals, palms, and soles.2,3
Tinea corporis, or ringworm, is a superficial dermatophyte infection that can appear anywhere on the body. It usually presents as annular, flat lesions with a scaly, raised, and well-defined border. They range from 1 to 10 cm in size. The lesions are characterized by a slowly advancing border with central clearing. A potassium hydroxide preparation shows numerous hyphae.2,3
Summary Table
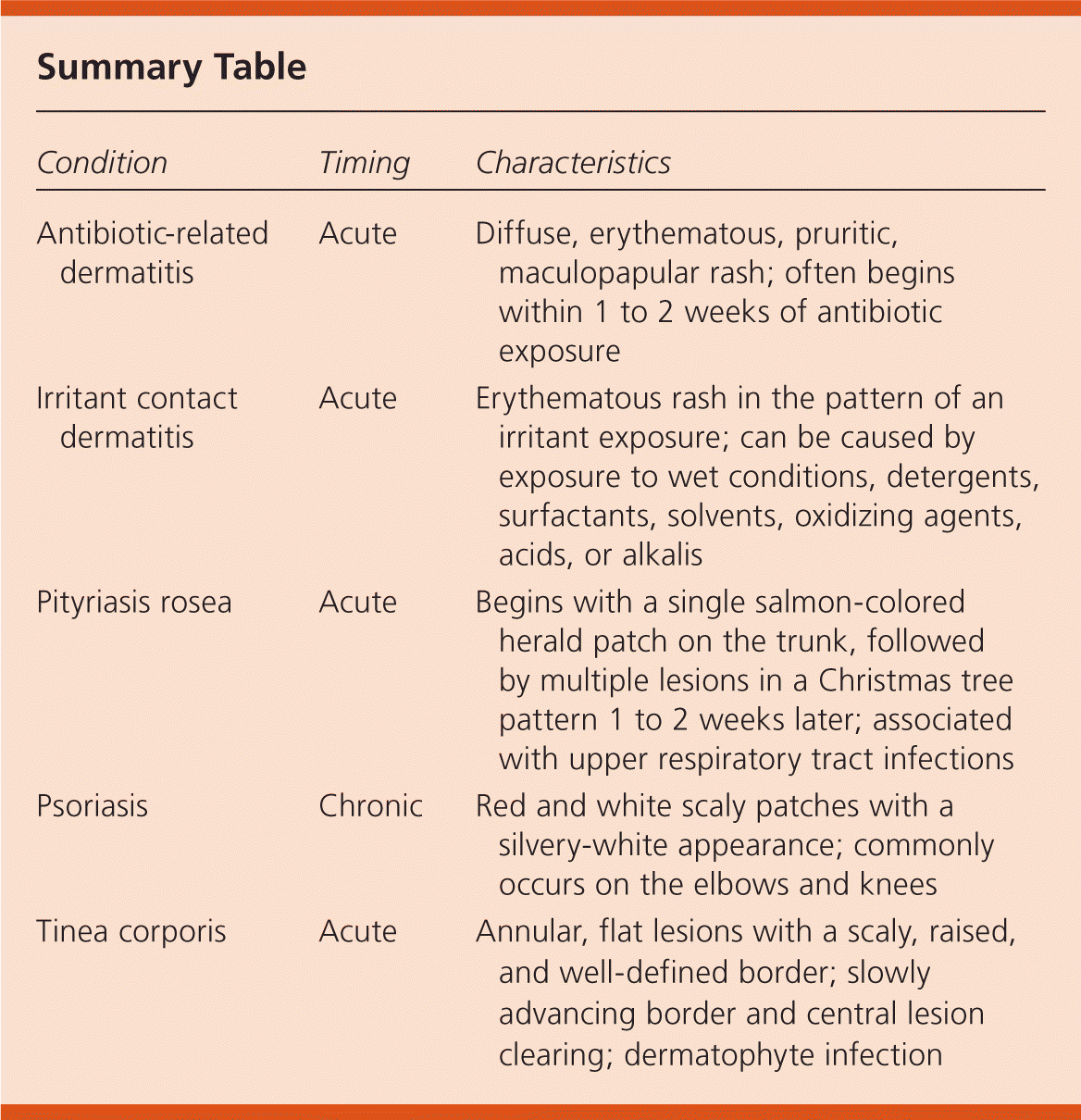
| Condition | Timing | Characteristics |
|---|---|---|
| Antibiotic-related dermatitis | Acute | Diffuse, erythematous, pruritic, maculopapular rash; often begins within 1 to 2 weeks of antibiotic exposure |
| Irritant contact dermatitis | Acute | Erythematous rash in the pattern of an irritant exposure; can be caused by exposure to wet conditions, detergents, surfactants, solvents, oxidizing agents, acids, or alkalis |
| Pityriasis rosea | Acute | Begins with a single salmon-colored herald patch on the trunk, followed by multiple lesions in a Christmas tree pattern 1 to 2 weeks later; associated with upper respiratory tract infections |
| Psoriasis | Chronic | Red and white scaly patches with a silvery-white appearance; commonly occurs on the elbows and knees |
| Tinea corporis | Acute | Annular, flat lesions with a scaly, raised, and well-defined border; slowly advancing border and central lesion clearing; dermatophyte infection |
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Navy Medical Department or the U.S. Navy at large.

