Summary of Recommendation and Evidence
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for vitamin D deficiency in asymptomatic adults (Table 1). I statement.
See the Clinical Considerations section for suggestions for practice regarding the I statement.
Table 1. Screening for Vitamin D Deficiency in Adults: Clinical Summary of the USPSTF Recommendation
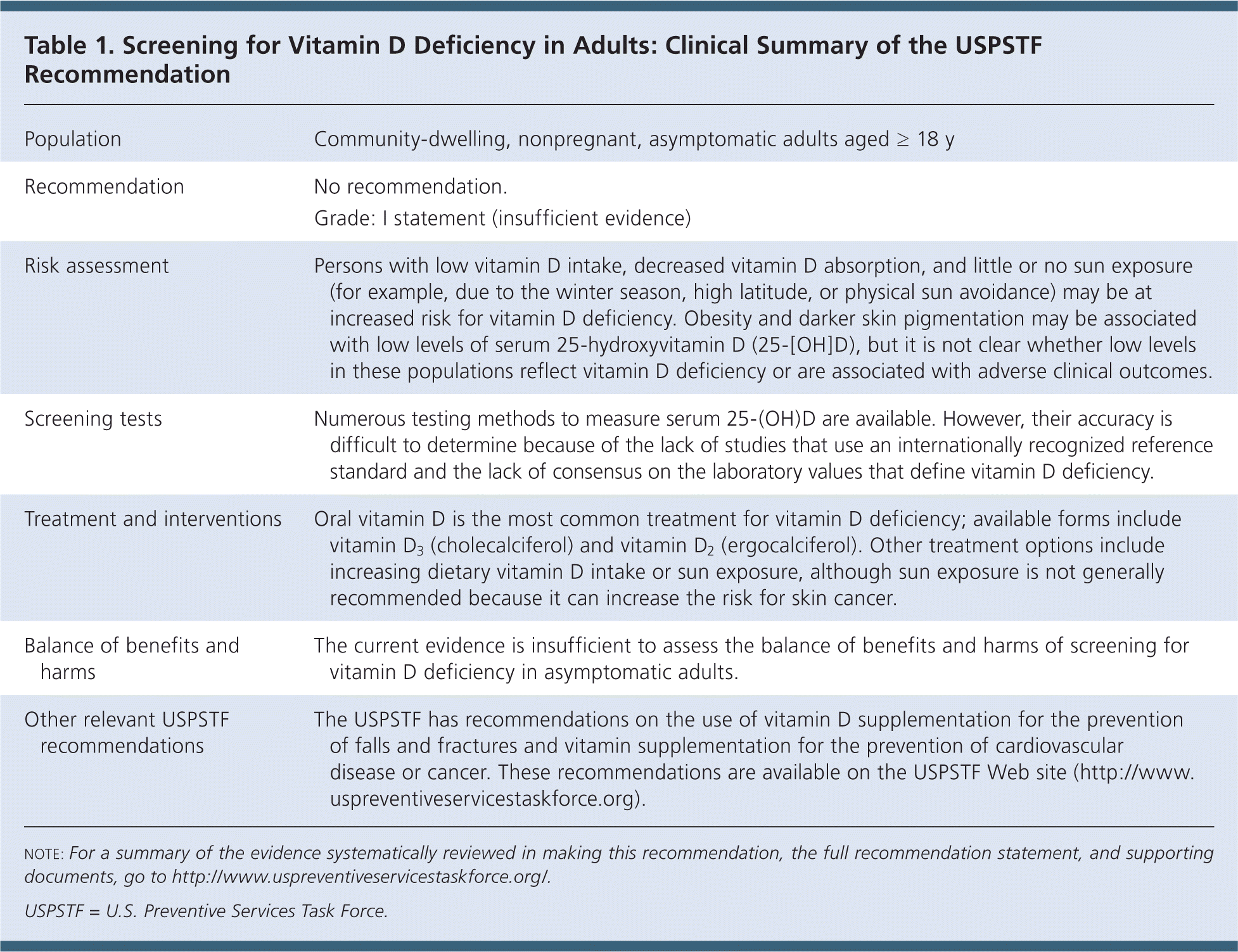
| Population | Community-dwelling, nonpregnant, asymptomatic adults aged ≥ 18 y |
| Recommendation | No recommendation. |
| Grade: I statement (insufficient evidence) | |
| Risk assessment | Persons with low vitamin D intake, decreased vitamin D absorption, and little or no sun exposure (for example, due to the winter season, high latitude, or physical sun avoidance) may be at increased risk for vitamin D deficiency. Obesity and darker skin pigmentation may be associated with low levels of serum 25-hydroxyvitamin D (25-[OH]D), but it is not clear whether low levels in these populations reflect vitamin D deficiency or are associated with adverse clinical outcomes. |
| Screening tests | Numerous testing methods to measure serum 25-(OH)D are available. However, their accuracy is difficult to determine because of the lack of studies that use an internationally recognized reference standard and the lack of consensus on the laboratory values that define vitamin D deficiency. |
| Treatment and interventions | Oral vitamin D is the most common treatment for vitamin D deficiency; available forms include vitamin D3 (cholecalciferol) and vitamin D2 (ergocalciferol). Other treatment options include increasing dietary vitamin D intake or sun exposure, although sun exposure is not generally recommended because it can increase the risk for skin cancer. |
| Balance of benefits and harms | The current evidence is insufficient to assess the balance of benefits and harms of screening for vitamin D deficiency in asymptomatic adults. |
| Other relevant USPSTF recommendations | The USPSTF has recommendations on the use of vitamin D supplementation for the prevention of falls and fractures and vitamin supplementation for the prevention of cardiovascular disease or cancer. These recommendations are available on the USPSTF Web site (http://www.uspreventiveservicestaskforce.org). |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
USPSTF = U.S. Preventive Services Task Force.
Rationale
IMPORTANCE
No consensus exists on the definition of vitamin D deficiency or the optimal level of total serum 25-hydroxyvitamin D (25-[OH]D) (the major form of vitamin D that circulates in the body). Depending on which cut point is used (usually < 50 or < 75 nmol/L [< 20 or < 30 ng/mL]), some studies have shown that low levels of vitamin D are associated with increased risk for fractures, functional limitations, cancer, diabetes, cardiovascular disease, depression, and death.1–3
DETECTION
Many testing methods are available that measure total serum 25-(OH)D levels. However, the accuracy of these tests to detect vitamin D deficiency is difficult to determine because of the lack of studies that use an internationally recognized reference standard and the lack of consensus on the laboratory values that define vitamin D deficiency. The USPSTF found evidence suggesting that results vary by testing method and between laboratories using the same testing methods.
BENEFITS OF DETECTION AND EARLY TREATMENT
The USPSTF found no studies that evaluated the direct benefit of screening for vitamin D deficiency in adults. The USPSTF found adequate evidence that treatment of asymptomatic vitamin D deficiency has no benefit on cancer, type 2 diabetes mellitus, risk for death in community-dwelling adults, and risk for fractures in persons not selected on the basis of being at high risk for fractures. The USPSTF found inadequate evidence on the benefit of treatment of asymptomatic vitamin D deficiency on other outcomes, including psychosocial and physical functioning. Although the evidence is adequate for a few limited outcomes, the overall evidence on the early treatment of asymptomatic, screen-detected vitamin D deficiency in adults to improve overall health outcomes is inadequate.
HARMS OF DETECTION AND EARLY TREATMENT
The USPSTF found no studies that evaluated the direct harms of screening for vitamin D deficiency. The USPSTF found adequate evidence that the harms of treatment of vitamin D deficiency are small to none. No studies reporting on the harms of treatment of vitamin D deficiency identified a significant increase in total adverse events, hypercalcemia, kidney stones, or gastrointestinal symptoms.
USPSTF ASSESSMENT
The USPSTF concludes that the evidence on screening for vitamin D deficiency in asymptomatic adults to improve health outcomes is insufficient and that the balance of benefits and harms of screening and early intervention cannot be determined.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to community-dwelling, nonpregnant adults aged 18 years or older who are seen in primary care settings and are not known to have signs or symptoms of vitamin D deficiency or conditions for which vitamin D treatment is recommended. This recommendation focuses on screening (that is, testing for vitamin D deficiency in asymptomatic adults and treating those who are found to have a deficiency), which is different from other USPSTF recommendation statements on supplementation (that is, recommending preventive medication for patients at increased risk for a specific negative health outcome, such as falls, regardless of whether they have a deficiency).
The USPSTF recognizes that there is no consensus on how to define vitamin D deficiency and does not endorse the use of a specific threshold to identify it. The evidence reviewed by the USPSTF used varying cut points. For the purposes of this recommendation statement, the term “vitamin D deficiency” is used to reflect evidence from study populations generally representing total serum 25-(OH)D levels of 75 nmol/L (30 ng/mL) or less or subpopulations of studies with levels less than 50 nmol/L (< 20 ng/mL).
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
Potential Preventable Burden. Given the lack of consensus on how to define and assess vitamin D deficiency, its precise prevalence estimates are difficult to determine. To collect precise estimates, accurate assay methods, an internationally recognized reference standard, and a specific cut point for defining vitamin D deficiency need to be established. Reported estimates of the prevalence of vitamin D deficiency vary widely depending on the period, cut point, study population, study design, and testing method. Estimates range from as low as 19% using a statistical modeling approach4 to as high as 77% based on NHANES (National Health and Nutrition Examination Survey) data from 2001 to 2004 (using a cut point of < 75 nmol/L [< 30 ng/mL]).5
The effect of vitamin D levels on health outcomes is difficult to evaluate. Lower vitamin D levels have been reported to increase risk for fractures, falls, functional limitations, some types of cancer, diabetes, cardiovascular disease, depression, and death. However, observations of these associations are inconsistent and may vary by the cut point used to define low vitamin D levels and by subpopulation (defined by race or institutionalization). For example, African Americans have paradoxically lower reported rates of fractures despite having increased prevalence of low vitamin D levels than white persons.
If a threshold total serum 25-(OH)D level could be established to define vitamin D deficiency and if testing assays could be standardized, the goal of screening for vitamin D deficiency would be to identify and treat it before associated adverse clinical outcomes occur. However, current evidence is inadequate to determine whether screening for and treatment of asymptomatic low 25-(OH)D levels improve clinical outcomes in community-dwelling adults.
Potential Harms. Screening may misclassify persons with a vitamin D deficiency because of the uncertainty about the cut point for defining deficiency and the variability of available testing assays. Misclassification may result in overdiagnosis (which may lead to nondeficient persons receiving unnecessary treatment) or underdiagnosis (which may lead to deficient persons not receiving treatment).
A rare but potential harm of treatment with oral vitamin D is toxicity, which may lead to hypercalcemia, hyperphosphatemia, suppressed parathyroid hormone, and hypercalciuria. However, the 25-(OH)D level associated with toxicity (often defined as > 500 nmol/L [> 200 ng/mL])6 is well above the level considered to be sufficient. Treatment with vitamin D plus calcium may also be associated with increased risk for kidney stones; vitamin D alone does not seem to increase this risk. In general, treatment with oral vitamin D does not seem to be associated with serious harms. Treatment with increased sun exposure (specifically ultraviolet B [UVB] radiation) may increase risk for skin cancer. Because of this concern, increased sun exposure is generally not recommended as treatment of vitamin D deficiency.
Costs. Several vitamin D testing methods are available; the cost of screening varies.
Current Practice. Testing rates for vitamin D levels seem to be increasing, despite the uncertainty about the definition of deficiency. Although estimates of screening rates in primary care settings are not available, a recent study evaluating data from the National Ambulatory Medical Care Survey and the National Hospital Ambulatory Medical Care Survey found that the annual rate of outpatient visits associated with a diagnosis code for vitamin D deficiency more than tripled between 2008 and 2010 (1,177 visits per 100,000 population in 2010).7 In addition, according to a 2009 survey, total serum 25-(OH)D testing increased by at least 50% compared with the previous year in more than half of the clinical laboratories surveyed.8
ASSESSMENT OF RISK
Although there is not enough evidence to support screening for vitamin D deficiency, some evidence suggests factors that may increase risk for vitamin D deficiency. Persons with low vitamin D intake, decreased vitamin D absorption, and little or no sun exposure (for example, due to the winter season, high latitude, or physical sun avoidance) may be at increased risk for vitamin D deficiency.1,2 Obesity and darker skin pigmentation may also be associated with low levels of total serum 25-(OH)D, but whether these factors reflect vitamin D deficiency or increase the risk for adverse clinical outcomes is unclear. Obesity may allow for greater sequestration of vitamin D into adipose tissue; however, this vitamin D may still be bioavailable.1,2 Increased skin pigmentation reduces the skin's ability to produce vitamin D in response to UVB exposure. Prevalence rates of low total serum 25-(OH)D are 2 to 9 times higher in African Americans and 2 to 3 times higher in Hispanics than in white persons,1 yet the risk for fractures in African Americans is half that in white persons.9 Other factors, such as body composition and calcium economy, have been proposed to explain this paradox10; however, a recent study suggests that although total serum 25-(OH)D levels in African Americans may be low, the concentration of bioavailable 25-(OH)D may not be.1,11 Some evidence suggests that older age and female sex may also be associated with increased risk for vitamin D deficiency; however, these findings are inconsistent.1
SCREENING TESTS
Current vitamin D assays measure total serum 25-(OH)D levels to determine vitamin D status (that is, whether a person is considered to have or not have a deficiency). Many testing methods are available, including competitive protein binding, immunoassay, high-performance liquid chromatography, and combined high-performance liquid chromatography and mass spectrometry. However, the sensitivity and specificity of these tests are unknown because of the lack of studies that use an internationally recognized reference standard. Variability between assay methods and between laboratories using the same methods may range from 10% to 20%, and classification of samples as “deficient” or “nondeficient” may vary by 4% to 32%, depending on which assay is used.1,2 Another factor that may complicate interpretation is that 25-(OH)D may act as a negative acute-phase reactant and its levels may decrease in response to inflammation. Lastly, whether common laboratory reference ranges are appropriate for all ethnic groups is unclear.
TREATMENT AND INTERVENTIONS
Oral vitamin D is most often used to treat vitamin D deficiency; other treatment options include increasing dietary vitamin D intake or UVB exposure. Commonly available forms of oral vitamin D include vitamin D3 (cholecalciferol) and vitamin D2 (ergocalciferol).
ADDITIONAL APPROACHES TO PREVENTION
According to the Institute of Medicine, daily dietary vitamin D intake of 600 IU in adults aged 18 to 70 years and 800 IU in adults older than 70 years should be sufficient to meet the needs of 97.5% of the adult population.12 UVB exposure may also increase vitamin D levels; however, several variables (such as the time of day, season, cloud cover, skin pigmentation, and sunscreen use) can affect the length of exposure needed to attain sufficient vitamin D levels. Sun exposure to prevent vitamin D deficiency is not generally recommended because it increases the risk for skin cancer associated with UVB radiation.
USEFUL RESOURCES
The USPSTF has published recommendations on the use of vitamin D supplementation for the prevention of falls and fractures and vitamin supplementation for the prevention of cardiovascular disease or cancer (available at http://www.uspreventiveservicestaskforce.org). These recommendations differ from the current recommendation statement in that they address vitamin D supplementation in certain populations at high risk for falls, fractures, cardiovascular disease, or cancer without first determining a patient's vitamin D status.

