A 52-year-old Hispanic man presented with two weeks of severe pain and swelling in his knees and wrists that affected his ability to walk. He had a rash on his thighs, knees, hands, and lower back. He did not have fever, dysuria, or eye pain. He had no significant medical history.
His vital signs were normal. He had red-purple, round plaques with scale on his bilateral lower extremities, dorsum of his hands, over the sacral region of his lower back, and in the inguinal region (Figure 1). His palms were normal, but the soles of his feet had a thick, yellow, keratotic scale. There was no fingernail pitting. There was prominent joint swelling and effusion in his wrists and knees (Figure 2), with mild tenderness and limited range of motion. There was diffuse swelling of the right thumb with nail dystrophy.
Laboratory studies revealed an elevated C-reactive protein level of 222 mg per L (2,114.33 nmol per L) and erythrocyte sedimentation rate of 113 mm per hour. Serology tests were positive for Chlamydia trachomatis immunoglobulin M and G.
Figure 1.
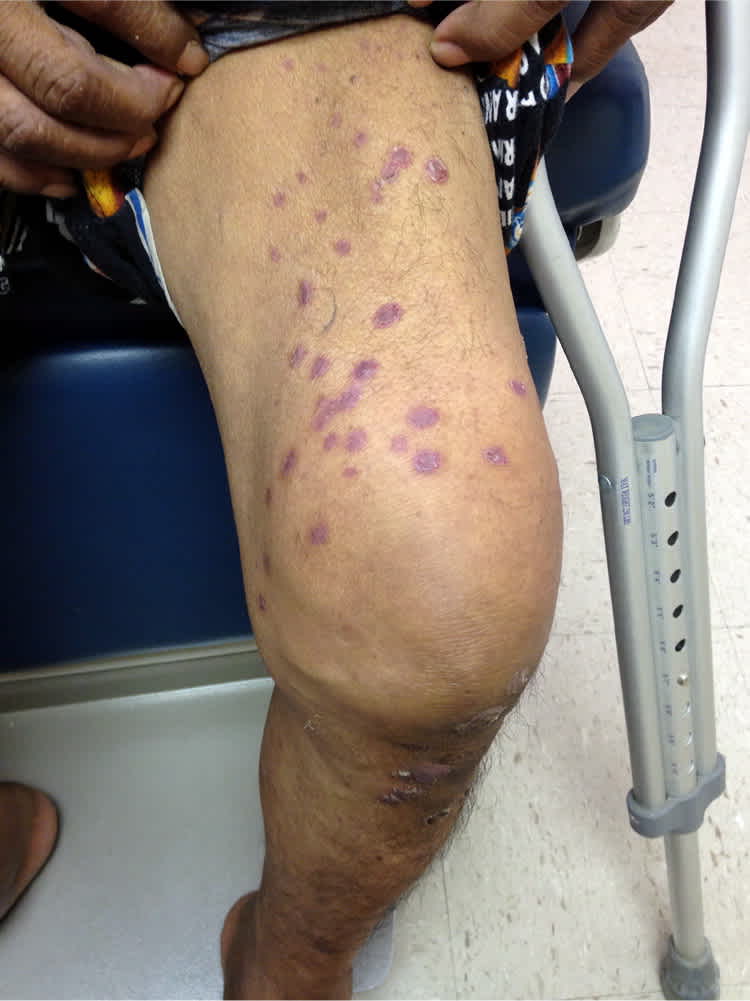
Figure 2.
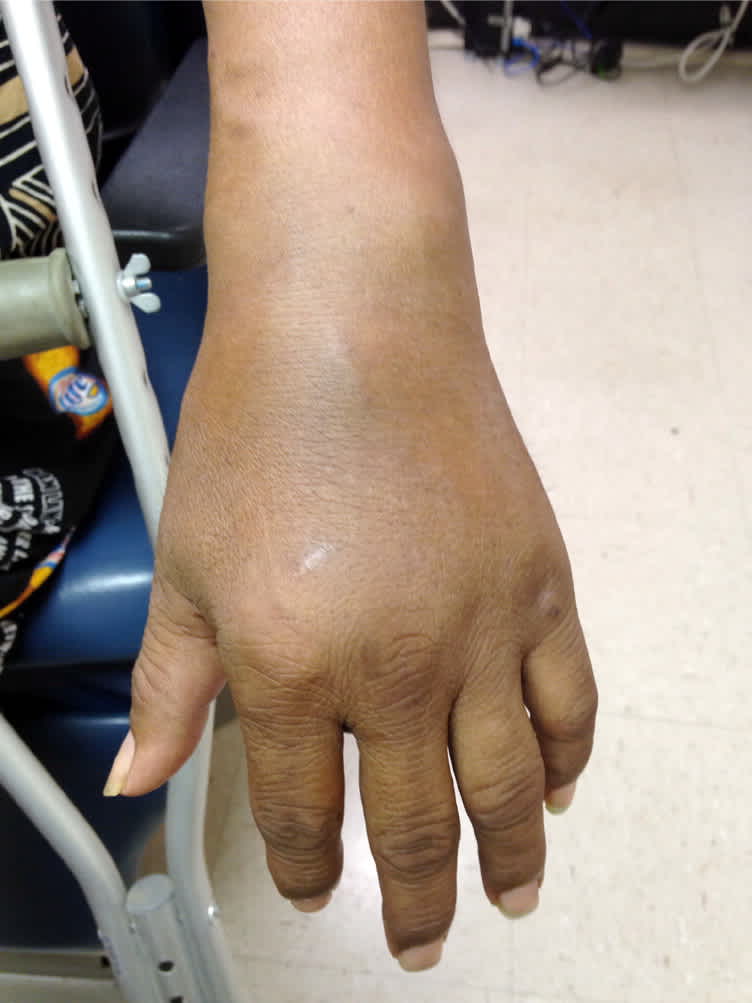
Question
Based on the patient's history, physical examination, and laboratory findings, which one of the following is the most likely diagnosis?
A. Psoriatic arthritis.
B. Reactive arthritis.
C. Rheumatoid arthritis.
D. Systemic lupus erythematosus.
Discussion
The correct answer is B: reactive arthritis. Reactive arthritis is a syndrome that classically involves polyarthritis, urethritis, uveitis, and psoriasiform skin findings in response to a genitourinary or gastrointestinal infection. The acute onset of two of these features, along with testing positive for chlamydia and human leukocyte antigen B27 (HLA-B27) and high inflammatory markers, established the diagnosis in this patient. Only about one-third of patients with the condition present with the classic triad.1 Symptoms typically develop within four weeks of the infection. The most commonly associated pathogens are Chlamydia trachomatis, Shigella, Campylobacter, Salmonella, Yersinia, and Clostridium difficile.1 The mechanism by which these organisms trigger the arthritis and associated symptoms is not well understood.1 The disease is usually self-limited, with most patients symptom-free within 12 months.1
Patients with reactive arthritis may present with a wide variety of symptoms. The skin findings in this patient included plaques of scale, thick keratotic scaling of the plantar feet (keratoderma blennorrhagicum), and nail dystrophy. The arthritis typically presents as an asymmetric polyarthritis, most commonly affecting the knees and ankles. Back and heel pain are also common.1 Conjunctivitis is the most common ophthalmologic finding, affecting approximately 30% to 60% of patients. Uveitis occurs in 12% to 37% of patients and may result in permanent vision loss if untreated.2 The psoriasiform skin findings occur in 5% of patients and present as red plaques with scale on the extensor surfaces of the lower extremities and dorsum of hands and fingers.2
The diagnosis of reactive arthritis is based on history and clinical examination findings. Testing is positive for HLA-B27 in about 70% to 80% of patients with reactive arthritis, and may indicate more serious disease.1 Elevated erythrocyte sedimentation rate and C-reactive protein measurements are common. The patient should be tested for C. trachomatis, and stool cultures should be evaluated for gastrointestinal infection. Joint aspiration can show leukocytes. Radiographs of the affected joints may show soft tissue swelling associated with joint effusions.1
Psoriatic arthritis is a chronic inflammatory, immune-mediated disease that can have clinical findings similar to those of reactive arthritis, especially the skin manifestations. The condition commonly affects the hands, feet, knees, and/or spine, and patients often have a family history of psoriasis. Chlamydia and HLA-B27 are not commonly associated with psoriatic arthritis. Inflammatory markers may be elevated but typically not as high as with a reactive arthritis.
Rheumatoid arthritis is a chronic inflammatory disease that presents with polyarthralgias and polyarthritis, typically affecting the proximal interphalangeal and metacarpophalangeal joints of the hands. Radiographs often show joint deformities and erosive changes. Subcutaneous (rheumatoid) nodules are the typical skin finding.3 Serologic testing is usually positive for rheumatoid factor.
Systemic lupus erythematosus is a chronic inflammatory disease with polyarthralgias of the hands, wrists, and knees. Skin manifestations are usually in photodistributed areas, such as a malar rash across the cheeks, sparing the nasolabial folds.3 Systemic lupus erythematosus is associated with positive antinuclear antibody test results.
Summary Table

| Condition | Characteristics | Test results |
|---|---|---|
| Psoriatic arthritis | Chronic inflammatory polyarthritis affecting the hands, feet, knees, and/or spine; personal or family history of psoriasis is common | No specific serologic testing; erosions with “pencil in cup” deformity on radiography; may be positive for HLA-B27, but this is less common |
| Reactive arthritis | Acute polyarthritis, urethritis, uveitis, psoriasiform skin lesions; develops within four weeks of infection | Positive for genitourinary or gastrointestinal infection; positive for HLA-B27 |
| Rheumatoid arthritis | Chronic inflammatory polyarthritis; typically affects the proximal interphalangeal and metacarpophalangeal joints of the hands; associated with joint deformities and erosive changes; subcutaneous (rheumatoid) nodules | Positive for rheumatoid factor; deformities and erosive changes on radiography |
| Systemic lupus erythematosus | Chronic polyarthritis of hands, wrists, and knees; malar rash across the cheeks, sparing the nasolabial folds | Positive for antinuclear antibody |
HLA-B27 = human leukocyte antigen B27.

