Clinical Question
What are the indications for operative vs. nonoperative management of acute Achilles tendon rupture?
Evidence-Based Answer
Operative and nonoperative management provide similar outcomes. There are no clear evidence-based criteria to decide which patients should undergo operative vs. nonoperative management of acute Achilles tendon rupture. When controlled early mobilization is used in nonoperative management, rerupture rates seem to be the same as in surgical management. There is a higher risk of complications such as scar adhesions and loss of sensation with surgical management, but no difference in return time to work or sporting activity. Patients with an Achilles tendon rupture can be offered either operative or nonoperative treatment with controlled early mobilization. (Strength of Recommendation: A, based on a meta-analysis of randomized controlled trials [RCTs].)
Evidence Summary
A meta-analysis of 10 nonblinded RCTs of 894 adults with unilateral acute Achilles tendon rupture examined operative vs. nonoperative management.1 The overall quality of the trials was high. Follow-up ranged from six months to 2.5 years. Patients in the operative group had approximately 5% fewer reruptures after surgery compared with the nonoperative group (4.3% vs. 9.7%; risk ratio = 0.44; 95% confidence interval, 0.26 to 0.74; P = .002). Overall, there was a higher rate of complications in the operative group, including more scar adhesions, loss of superficial sensation, and superficial infections. There was no difference in rates of deep infections or deep venous thrombosis, or in the number of patients who successfully returned to sports after treatment (Table 1).1,2
Table 1. Outcomes in Patients with Operative vs. Nonoperative Treatment of Achilles Tendon Rupture
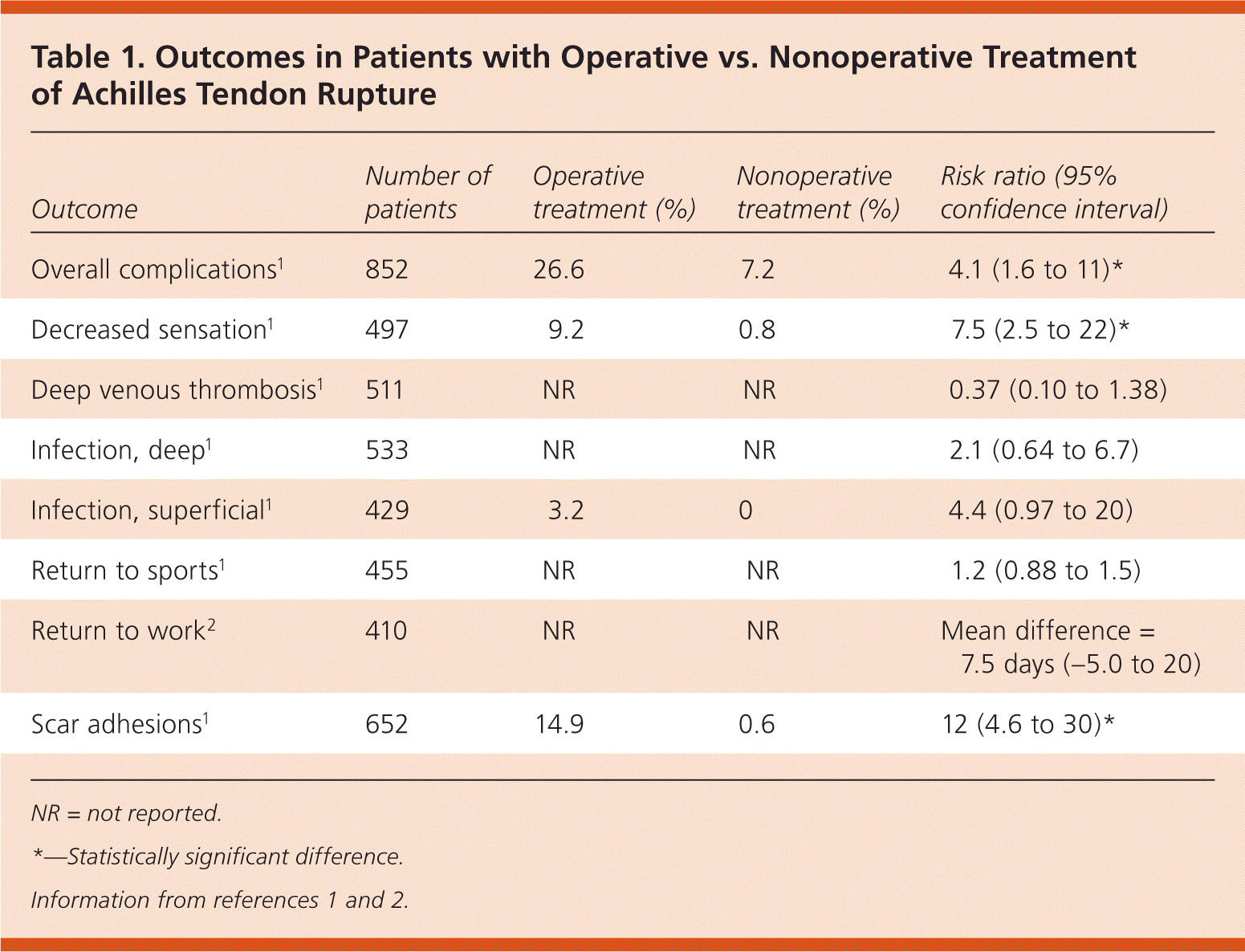
| Outcome | Number of patients | Operative treatment (%) | Nonoperative treatment (%) | Risk ratio (95% confidence interval) |
|---|---|---|---|---|
| Overall complications1 | 852 | 26.6 | 7.2 | 4.1 (1.6 to 11)* |
| Decreased sensation1 | 497 | 9.2 | 0.8 | 7.5 (2.5 to 22)* |
| Deep venous thrombosis1 | 511 | NR | NR | 0.37 (0.10 to 1.38) |
| Infection, deep1 | 533 | NR | NR | 2.1 (0.64 to 6.7) |
| Infection, superficial1 | 429 | 3.2 | 0 | 4.4 (0.97 to 20) |
| Return to sports1 | 455 | NR | NR | 1.2 (0.88 to 1.5) |
| Return to work2 | 410 | NR | NR | Mean difference = 7.5 days (−5.0 to 20) |
| Scar adhesions1 | 652 | 14.9 | 0.6 | 12 (4.6 to 30)* |
NR = not reported.
*—Statistically significant difference.
Another meta-analysis of seven RCTs compared return to work time in patients who underwent operative vs. nonoperative management after one to 2.5 years of follow-up.2 This analysis included 677 adults who sustained an acute Achilles tendon rupture. All seven trials were also included in the previous meta-analysis. Investigators found no significant difference in return to work time between groups.
A meta-analysis of 10 high-quality RCTs (seven of which were included in the above meta-analyses) found that functional rehabilitation with early range of motion exercises reduces rerupture rates in operative and nonoperative treatment groups.3 Investigators in five of the RCTs (N = 185) used early range of motion exercises leading to functional rehabilitation (typically adding active plantarflexion after 10 to 14 days in equinus cast, then progressively reducing restrictions on dorsiflexion), then began formal physical therapy at two to eight weeks. The overall pooled results found lower rerupture risk in the operative group (absolute risk reduction = 5.5%; P = .002), but subgroup analysis of the five RCTs using early mobilization found no significant difference between operative and nonoperative groups (P = .45). There was no significant difference in calf circumference, strength, or functional outcome between groups.
Recommendations from Others
The American Academy of Orthopaedic Surgeons (AAOS) recommends both nonsurgical and surgical approaches as options for treating patients with acute Achilles tendon rupture.4 It supports early (within the first two weeks) protected weight bearing for patients who have been treated surgically (moderate grade of evidence) and the use of a protective device that allows mobilization by two to four weeks postsurgery (moderate grade of evidence). A consensus statement by the AAOS recommends a cautious approach in older adults and in those who smoke or have preexisting medical conditions that may complicate treatment.
Copyright Family Physicians Inquiries Network. Used with permission.

